Have you ever received a medical bill or glanced at your health record and been mystified by a series of numbers and letters under “diagnosis code”? You’re not alone. For patients and medical coders alike, understanding these codes is crucial for accurate billing, clear communication, and effective healthcare management. If you’re researching the “ICD-9 code for fungal infection,” you’re likely dealing with older records or specific billing questions. This comprehensive guide will not only answer that query but will also provide you with the essential context needed to navigate the world of medical coding for fungal conditions.
First, a critical piece of context: the ICD-9 coding system is no longer in active use for diagnosis reporting in the United States. It was officially replaced by ICD-10-CM on October 1, 2015. However, understanding ICD-9 remains important for historical record analysis, certain research studies, and resolving legacy billing issues. Think of it like an old filing system; you may not add new files to it, but you still need to know how to find something stored there years ago.
This article will serve as your trusted manual. We’ll explore the specific ICD-9 codes for fungal infections, understand their structure, and then bridge the gap to the modern ICD-10 system. Our goal is to empower you with clear, accurate information, whether you’re a patient seeking clarity, a student in the medical field, or a professional brushing up on coding fundamentals.
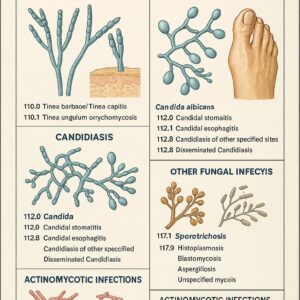
ICD-9 Codes for Fungal Infections
What is ICD-9 and Why is it Relevant?
The International Classification of Diseases, 9th Revision, Clinical Modification (ICD-9-CM) was the standard system used for over three decades to code diagnoses and inpatient procedures in the U.S. healthcare system. It provided a common language, translating medical conditions into alphanumeric codes for billing, statistics, and research.
While ICD-10 has superseded it, knowledge of ICD-9 is not obsolete. Its relevance persists in several key areas:
-
Historical Medical Records: All patient records prior to October 2015 were coded using ICD-9. Understanding these codes is necessary for interpreting past diagnoses and treatment histories accurately.
-
Ongoing Legal and Insurance Cases: Some long-term disability or injury claims that originated before 2015 may still reference ICD-9 codes in their documentation.
-
Academic Research: Studies analyzing long-term health trends often need to reconcile data across both coding systems, requiring fluency in ICD-9.
-
Coding Education: Learning the foundational logic of ICD-9 helps in understanding the more complex structure of ICD-10.
As Dr. Linda Roberts, a health informatics specialist, notes: *”Transitioning from ICD-9 to ICD-10 was like moving from a detailed map of a country’s major highways to a satellite image showing every street and alley. The old map is still valuable for understanding the broad routes, but the new one gives us the precision needed for modern healthcare navigation.”*
The Core Structure of ICD-9 Codes
ICD-9-CM codes are typically 3 to 5 characters long. The structure follows a logical hierarchy:
-
Category (First 3 Digits): This defines the general type of disease or injury. For our focus, the category for most fungal infections is 117.
-
Subcategory (4th Digit): A decimal point follows the first three digits, and the fourth digit provides more specificity about the site or type of condition.
-
Subclassification (5th Digit): This offers the highest level of detail available in ICD-9, often specifying laterality (left, right, bilateral) or a particular clinical detail.
Example: The code 110.1 breaks down as:
-
110: Category for “Dermatophytosis” (fungal skin infections).
-
.1: Subcategory for “Dermatophytosis of nail” (onychomycosis).
Important Note for Readers: The information in this article is intended for educational and reference purposes. It should not be used for self-diagnosis or to determine final medical billing codes. Always consult with a qualified healthcare provider for diagnosis and treatment, and rely on certified medical coders and the current official code sets for all billing and reporting purposes.
The ICD-9 Code for Fungal Infections: A Detailed Breakdown
The umbrella ICD-9 code for systemic and deep fungal infections is found in category 117. This category is titled “Mycoses,” which is the medical term for fungal infections. However, the coding system separates superficial skin infections (like athlete’s foot) into a different chapter. Let’s delve into the specifics.
Major ICD-9 Categories for Fungal Conditions
Fungal infections in ICD-9 are primarily divided into two main groupings:
| ICD-9 Code Range | Category Title | Description & Common Examples |
|---|---|---|
| 110 | Dermatophytosis | Superficial infections of the skin, hair, and nails caused by dermatophyte fungi. |
| 111 | Dermatomycosis, other and unspecified | Other superficial skin mold infections not caused by dermatophytes (e.g., tinea versicolor). |
| 112 | Candidiasis | Infections caused by Candida yeast, affecting sites like the mouth (thrush), vagina, esophagus, or bloodstream. |
| 114 | Coccidioidomycosis | Systemic infection caused by the fungus Coccidioides (Valley fever). |
| 115 | Histoplasmosis | Systemic infection caused by Histoplasma, often affecting the lungs. |
| 116 | Blastomycosis | Systemic infection caused by Blastomyces. |
| 117 | Other Mycoses | A broad category for other fungal infections, including aspergillosis, cryptococcosis, and zygomycosis. |
| 118 | Opportunistic Mycoses | Infections that take advantage of a weakened immune system. |
As you can see, while 117.x is a critical code block, it is part of a larger, organized system.
Deep Dive: Category 117 – Other Mycoses
This is the category most searchers are looking for when they query “ICD 9 code for fungal infection” in a general sense. It requires a fourth digit for specificity. Below is a table of the most clinically significant codes within this category.
| ICD-9 Code | Full Description | Common Name & Clinical Context |
|---|---|---|
| 117.0 | Rhinosporidiosis | Chronic infection primarily affecting the mucous membranes of the nose and eye. |
| 117.1 | Sporotrichosis | “Rose gardener’s disease.” A subcutaneous infection often entering through a skin puncture from plant matter. |
| 117.2 | Chromoblastomycosis | Chronic skin and subcutaneous tissue infection, often causing cauliflower-like lesions. |
| 117.3 | Aspergillosis | Infection caused by Aspergillus mold. Can range from allergic reactions to invasive lung or systemic disease, especially in immunocompromised patients. |
| 117.4 | Mycotic mycetomas | Deep tissue infections causing swelling and grain-like clusters of fungi, often in the foot (Madura foot). |
| 117.5 | Cryptococcosis | Serious infection caused by Cryptococcus neoformans, commonly affecting the lungs and central nervous system (meningitis). |
| 117.6 | Zygomycosis (Phycomycosis/Mucormycosis) | Aggressive infection by fungi in the Mucorales order. Often involves the sinuses, brain, or lungs and is a medical emergency. |
| 117.7 | Pneumocystosis | Pneumonia caused by Pneumocystis jirovecii, a major opportunistic infection in AIDS and other immunodeficiencies. |
| 117.8 | Other specified mycoses | Includes rare infections like lobomycosis. |
| 117.9 | Unspecified mycosis | Used when a fungal infection is confirmed but the specific type is not identified. |
Coding Common Superficial Infections (Not in 117)
It’s vital to remember that the most common fungal infections people encounter are coded elsewhere. Here’s a quick reference:
-
Athlete’s Foot (Tinea Pedis): 110.4
-
Jock Itch (Tinea Cruris): 110.3
-
Ringworm of the Body (Tinea Corporis): 110.5
-
Fungal Nail Infection (Onychomycosis): 110.1
-
Vaginal Yeast Infection: 112.1
-
Oral Thrush: 112.0
The Critical Transition: From ICD-9 to ICD-10-CM
The shift to ICD-10-CM was not a simple update; it was a fundamental expansion. ICD-9 contained approximately 14,000 codes. ICD-10-CM boasts over 68,000. This increase allows for breathtaking specificity, which improves patient care, public health tracking, and billing accuracy.
Key Differences Between the Systems
-
Format: ICD-9 codes are 3-5 digits, numeric. ICD-10 codes are 3-7 characters, alphanumeric.
-
Specificity: ICD-10 mandates much greater detail. It can laterality, severity, etiology, and encounter type (initial, subsequent, sequelae).
-
Organization: Chapters were reorganized, and new ones were added.
ICD-9 to ICD-10 Conversion for Fungal Infections
There is rarely a direct 1-to-1 match. An ICD-9 code usually maps to a family of more precise ICD-10 codes. Here is a conversion guide for the primary codes we’ve discussed.
| ICD-9 Code | ICD-9 Description | Primary ICD-10-CM Code Range | ICD-10-CM Description & Key Differences |
|---|---|---|---|
| 117.3 | Aspergillosis | B44.* | Aspergillosis. ICD-10 specifies the site (e.g., B44.0 for invasive pulmonary aspergillosis, B44.1 for other pulmonary aspergillosis, B44.2 for tonsillar aspergillosis). |
| 117.5 | Cryptococcosis | B45.* | Cryptococcosis. Specific codes for pulmonary (B45.0), cerebral (B45.1), cutaneous (B45.2), etc. |
| 117.6 | Zygomycosis | B46.* | Zygomycosis. Includes codes for pulmonary mucormycosis (B46.0), rhinocerebral (B46.1), gastrointestinal (B46.2), etc. |
| 117.7 | Pneumocystosis | B59 | Pneumocystosis. |
| 110.1 | Dermatophytosis of nail | B35.1 | Onychomycosis. |
| 112.1 | Candidiasis of vulva and vagina | B37.3 | Candidiasis of vulva and vagina. |
Important Note for Coders: The General Equivalence Mappings (GEMs) provided by the CDC and CMS are the authoritative tools for converting between ICD-9 and ICD-10. The table above is a simplified educational reference. Always consult the current ICD-10-CM code book and official guidelines for accurate coding.
A Practical Guide to Accurate Coding: Step-by-Step
For medical coders, accuracy is non-negotiable. Here is a recommended workflow for coding a fungal infection diagnosis:
-
Start with the Physician’s Documentation: The medical record is your source of truth. Look for the specific diagnosis (e.g., “pulmonary histoplasmosis,” “disseminated coccidioidomycosis”).
-
Identify Key Details:
-
Type of Fungus: Aspergillus, Candida, Histoplasma, etc.
-
Site of Infection: Lung, brain, skin, blood, esophagus, etc.
-
Laterality: For paired organs (e.g., fungal infection of the left knee).
-
Manifestations: Are there specific complications (e.g., meningitis, endocarditis)?
-
Encounter Type: Is this the initial diagnosis, a follow-up, or treatment for a sequela (late effect)?
-
-
Navigate the ICD-10-CM Index: Look up the main term in the Alphabetic Index (e.g., “Histoplasmosis”). Follow the indentations for subterms related to the site.
-
Verify in the Tabular List: Never code directly from the Index. Always go to the numeric Tabular List to confirm the code, review includes/excludes notes, and check for mandatory additional characters.
-
Assign the Most Specific Code Available: Use the full 7 characters if required. Do not use unspecified codes (.9) if the documentation supports a more specific code.
Common Coding Pitfalls to Avoid
-
Coding from Lab Results Alone: A positive culture must be interpreted by the treating physician as a current, clinically significant infection to be coded. Colonization is not an infection.
-
Overlooking “Code First” Notes: Some fungal infections are manifestations of an underlying disease (e.g., candidiasis in a patient with neutropenia due to chemotherapy). ICD-10 often instructs you to “code first” the underlying condition.
-
Ignoring Laterality: Using an unspecified laterality code when the record clearly states “right” or “left” is incorrect and can impact reimbursement.
-
Using Outdated Code Books: ICD-10 is updated annually on October 1st. Using last year’s book can lead to errors.
Conclusion
Understanding the legacy ICD-9 code for fungal infection, primarily within category 117.x, provides essential insight into historical medical data and the foundation of modern coding. The transition to ICD-10-CM has brought a necessary level of detail that enhances clinical accuracy and patient care. Whether you’re deciphering an old record or coding a new diagnosis, the principles of specificity, careful documentation review, and using current, official resources remain paramount. By mastering both the historical context and the modern system, you ensure clarity and precision in the vital language of medical diagnosis.
Frequently Asked Questions (FAQ)
Q1: Can I still use ICD-9 codes for billing today?
A: No. As of October 1, 2015, all HIPAA-covered entities in the United States (healthcare providers, payers, clearinghouses) are required to use ICD-10-CM for diagnosis coding. Using ICD-9 will result in claim rejection.
Q2: I have an old bill from 2014 with code 117.9. What does that mean?
A: Code 117.9 meant “Unspecified mycosis.” It indicates that your medical record from that time documented a fungal infection, but the specific type (e.g., aspergillosis, cryptococcosis) was not identified or stated in a way that allowed for a more precise code.
Q3: How do I find the equivalent ICD-10 code for an old ICD-9 code?
A: The Centers for Disease Control and Prevention (CDC) provides public access to the General Equivalence Mappings (GEMs). These are complex crosswalk files. For most individuals, using a reputable online code lookup tool that includes cross-referencing or consulting a current ICD-10 manual with conversion notes is more practical.
Q4: Why are there so many more codes in ICD-10? Is it just for billing?
A: While improved billing accuracy is a benefit, the primary driver is better patient care and public health. The increased specificity allows for more precise tracking of disease patterns, treatment outcomes, and resource utilization. It enables better clinical research and health policy planning.
Q5: Where can I find the official, up-to-date ICD-10 codes?
A: The CMS (Centers for Medicare & Medicaid Services) and the CDC’s National Center for Health Statistics (NCHS) are the official U.S. government agencies responsible for ICD-10-CM. They publish the official guidelines and code sets free of charge on their websites.
Additional Resources
For further, in-depth study and the most current official information, please visit:
-
CDC ICD-10-CM Official Guidelines: https://www.cdc.gov/nchs/icd/icd-10-cm.htm
-
CMS ICD-10 Provider Resources: https://www.cms.gov/medicare/coding-billing/icd-10-codes
Date: January 22, 2026
Author: The Health Coding Guide Team






