Walking into a dental office, the one thing that puts most patients at ease is knowing they won’t feel pain. That assurance comes from local anesthesia. But behind the scenes, there is a complex web of billing and coding that determines how dentists get paid for administering that numbness.
If you are a dental professional, a biller, or a student just getting your feet wet in dental administration, understanding the correct dental code for local anesthesia is vital. Use the wrong code, and a claim gets rejected. Miss a code, and the practice loses revenue. Overuse a code, and you might trigger an audit.
This guide is designed to be your definitive resource. We will strip away the confusion, look at the specific CPT and CDT codes, and explain exactly when and how to use them
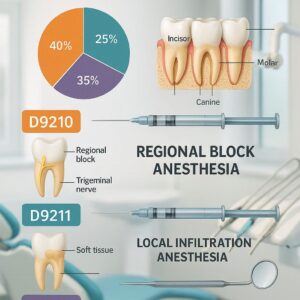
Dental Codes for Local Anesthesia
Table of Contents
ToggleThe Great Debate: Is Local Anesthesia Billable?
Before we dive into the specific numbers, we need to address the most common question in dental billing: Can you actually bill for local anesthesia?
The answer is nuanced. In the vast majority of routine restorative or surgical procedures, the answer is no. The administration of local anesthesia is considered a “bundled” service. This means the cost of the needle, the carpule of anesthetic, and the dentist’s skill in delivering it are included in the fee for the primary procedure (like a filling or an extraction).
However, there are specific exceptions where you can and should bill separately. These exceptions usually involve extraordinary circumstances, specific patient populations, or instances where the anesthesia is the primary service.
Decoding the Language: CDT vs. CPT
When searching for the dental code for local anesthesia, you will encounter two different coding systems. Knowing the difference is the first step to accurate billing.
-
CDT (Current Dental Terminology): Published by the American Dental Association (ADA), this is the code set used exclusively for dental procedures. If you are billing a dental procedure to a dental insurance plan, you use CDT codes. They always begin with the letter “D” (e.g., D9210).
-
CPT (Current Procedural Terminology): Published by the American Medical Association (AMA), these codes are used for medical procedures and services. They are five-digit numeric codes (e.g., 64400). You might use these if you are billing a dental anesthesia procedure to a medical insurance plan, rather than a dental plan.
For the purposes of this article, we will focus primarily on CDT codes, as they are the standard for dental practices.
Important Note for Readers: Always verify the specific coding requirements with the patient’s insurance carrier. Some plans have unique contracts that dictate how and when they will reimburse for anesthesia.
The Core Codes: The D9210 Series
When we talk about the standard dental code for local anesthesia, we are almost always referring to the D9210 series. This family of codes covers local anesthesia not in conjunction with a surgical or restorative procedure. Let’s break them down.
D9210: Local Anesthesia Not in Conjunction with Operative or Surgical Procedures
This is the primary code you will use when the sole purpose of the visit is to administer anesthesia.
-
When to use it: A patient comes in specifically for the management of acute pain. Perhaps they have a toothache so severe they cannot sleep, but the dentist cannot perform the root canal that day due to swelling or schedule constraints. The dentist injects local anesthetic to provide relief. The visit is only for the injection.
-
When NOT to use it: You cannot use D9210 if you are doing a filling, a crown, or an extraction. In those cases, the anesthesia is part of the main procedure.
D9211: Regional Block Anesthesia
While a standard infiltration numbs a small area, a regional block numbs a larger section of the mouth by targeting a main nerve trunk. The most common example is the inferior alveolar nerve block (IANB) to numb half the mandible.
-
When to use it: Similar to D9210, this is used when the block is performed as a distinct service, not in conjunction with another procedure. For example, a patient with trigeminal neuralgia might receive a nerve block for diagnostic or therapeutic pain management.
D9212: Trigeminal Division Block
This is a more specific and profound block. The trigeminal nerve has three divisions (ophthalmic, maxillary, and mandibular). This code is used when blocking a major division of this nerve, often for major surgical procedures or for managing severe, chronic facial pain. Like the others, it is billed separately when it is the primary service.
D9215: Local Anesthesia in Conjunction with Operative or Surgical Procedures
You will notice this code exists, but its use is highly controversial and often considered “unbundling.”
-
What it is: This code is intended to be used when local anesthesia is administered during a procedure, but in a situation that is somehow extraordinary or beyond what is typically provided.
-
The Reality: Most insurance carriers consider the administration of local anesthesia an inherent part of any restorative or surgical procedure. Therefore, they will deny D9215 if it is billed alongside a filling (D2XXX) or an extraction (D7XXX). It is rarely, if ever, reimbursed.
Summary Table: CDT Codes for Local Anesthesia
| Code | Description | Typical Use Case | Reimbursement Status |
|---|---|---|---|
| D9210 | Local anesthesia not in conjunction with operative/surgical procedures | Separate visit for pain management (e.g., toothache relief) | Billable to insurance |
| D9211 | Regional block anesthesia not in conjunction with procedures | Separate visit for a nerve block (e.g., for trigeminal neuralgia) | Billable to insurance |
| D9212 | Trigeminal division block not in conjunction with procedures | Separate visit for blocking a major nerve division for pain | Billable to insurance |
| D9215 | Local anesthesia in conjunction with operative/surgical procedures | Billed alongside a filling or extraction | Almost always denied (bundled) |
Beyond the Basics: Other Relevant Anesthesia Codes
Local anesthesia isn’t the only way to manage pain and anxiety in a dental setting. These related codes are important to know to understand the full picture of anesthesia billing.
Moderate Sedation (Conscious Sedation)
These codes are used when a patient is given medication to relax them but they remain awake and able to respond to verbal commands.
-
D9233: Inhalation of nitrous oxide (laughing gas) – anxiolysis. This is almost always an additional fee separate from the procedure.
-
D9239: Intravenous moderate sedation/analgesia – first 15 minutes.
Deep Sedation and General Anesthesia
These codes are for when the patient is in a state of controlled unconsciousness.
-
D9222: Deep sedation/general anesthesia – first 15 minutes (administered by a dentist).
-
D9223: Deep sedation/general anesthesia – each subsequent 15-minute increment.
These are complex services that require specific training and permits. They are billed separately and are often covered by medical insurance if deemed medically necessary.
Real-World Scenarios: Choosing the Right Code
Let’s put this knowledge into practice. Here are three common scenarios to help you visualize how to apply the correct dental code for local anesthesia.
Scenario 1: The Routine Filling
-
The Visit: A patient comes in for a scheduled appointment to place a composite filling on tooth #19. The dentist administers 1.5 carpules of lidocaine to numb the tooth, prepares the tooth, and places the filling.
-
The Codes: You would bill the appropriate code for the filling, for example, D2391 (posterior composite, one surface). The local anesthesia is included in the fee for D2391.
-
Do you bill a separate anesthesia code? No. D9215 would be inappropriate here.
Scenario 2: The Emergency Root Canal Start
-
The Visit: A patient presents as an emergency with a hot/cold sensitivity that lingers for minutes. The diagnosis is irreversible pulpitis. The dentist decides to start the root canal therapy to relieve the pressure and clean out the infected pulp. They administer 2 carpules of anesthetic and begin the RCT.
-
The Codes: You would bill the root canal code, for example, D3310 (anterior root canal).
-
Do you bill a separate anesthesia code? No. Again, the anesthesia is bundled into the endodontic procedure.
Scenario 3: The Severe Toothache with No Treatment
-
The Visit: A patient arrives late on a Friday afternoon with severe, throbbing pain in tooth #3. The tooth is fractured, and the nerve is exposed. The dentist knows the tooth is non-restorable and needs to be extracted, but the office does not perform surgical extractions and must refer the patient to an oral surgeon. However, the patient is in extreme pain. To provide relief, the dentist administers local anesthesia around tooth #3 to numb the nerve.
-
The Codes: No surgical or restorative procedure was performed. The only service rendered was the injection.
-
Do you bill a separate anesthesia code? Yes. You would bill D9210 – local anesthesia not in conjunction with operative or surgical procedures.
When Medical Insurance Comes Into Play: Billing with CPT Codes
There is a significant area where billing for anesthesia becomes more complex: when you are billing a patient’s medical insurance. This often happens with patients who have special needs, severe anxiety (dental phobia diagnosed as a medical condition), or when the dental procedure is being done in a hospital setting.
In these cases, you might step away from the CDT codes and use CPT codes to describe the anesthesia service to the medical payer.
Here are the common CPT code equivalents:
-
64400: Injection of anesthetic agent (local), trigeminal nerve, any division or branch.
-
64402: Injection of anesthetic agent (local), facial nerve.
-
64405: Injection of anesthetic agent (local), greater occipital nerve.
-
00170: Anesthesia for intraoral procedures, including biopsy; not otherwise specified.
Billing medical insurance for dental anesthesia is a specialized field. It often requires a strong medical necessity letter explaining why the anesthesia is required from a medical, not just a dental, perspective.
The Crucial Concept of “Medical Necessity”
Insurance companies, whether dental or medical, pay for services that are “medically necessary.” This concept is the gatekeeper for claims involving dental codes for local anesthesia.
-
For D9210, D9211, D9212: The medical necessity is the diagnosis of pain. The patient’s record must clearly document the level of pain, its origin, and why the injection was the only treatment provided that day. A diagnosis code like “K08.8 (other specified disorders of teeth and supporting structures)” for acute pain would support the claim.
-
For general anesthesia (D9222/D9223): The medical necessity might be a patient’s developmental disability that prevents them from cooperating, or a severe gag reflex that makes a procedure impossible while awake. This requires detailed documentation.
Without a clear “why,” the claim will be denied. The insurance company will simply say, “This service is not a covered benefit,” or “This service is incidental to the primary procedure.”
Common Billing Mistakes and How to Avoid Them
Even experienced billers can slip up. Here are the most frequent errors related to dental code for local anesthesia and how to steer clear of them.
1. Unbundling (The D9215 Trap)
This is mistake #1. A biller thinks they are maximizing revenue by adding D9215 to every crown and filling. Insurance companies have software that automatically flags and denies these “bundled” codes. It can also flag the provider for potential fraudulent upcoding.
2. Forgetting the Place of Service (POS)
When billing medical insurance, the place of service code is critical. A code for anesthesia administered in a dental office (POS 11) is viewed differently than the same code administered in an ambulatory surgical center (POS 24). Make sure your POS matches the actual setting.
3. Poor Documentation
For a stand-alone anesthesia code like D9210, the clinical notes are everything. A note that simply says “Patient in pain. Gave shot.” is insufficient. A better note would be: “Patient presents with complaint of sharp, spontaneous pain in tooth #30. Exam reveals extensive caries with pulpal exposure. Patient reports pain level 9/10. Patient referred to oral surgeon for evaluation. To provide interim relief, 1.8cc 2% lidocaine with 1:100k epinephrine administered via infiltration buccal and lingual to #30. Patient tolerated well, reports pain level 0/10 post-injection.”
4. Using Expired Codes
Both CDT and CPT code sets are updated annually. Using last year’s code is a guaranteed way to get a claim rejected. Always verify you are using the current year’s codes.
A Helpful Checklist for Coding Local Anesthesia
Before you hit “submit” on a claim that includes a specific dental code for local anesthesia, run through this quick checklist:
-
Was a surgical or restorative procedure performed? If YES, go to Question 2. If NO, use the appropriate D9210-D9212 code based on the type of injection.
-
If a procedure was performed, was the anesthesia “extraordinary”? (e.g., the patient required multiple carpules due to acute infection making the area hard to numb). If YES, you may consider D9215, but be prepared for a denial. If NO, the anesthesia is bundled.
-
Is this a medical claim or a dental claim? If MEDICAL, are you using the correct CPT codes? If DENTAL, are you using the correct CDT codes?
-
Is the documentation in the patient’s chart robust enough to support the code? Does it tell the story of why this service was necessary and what was done?
The Future of Dental Anesthesia Coding
The world of dental coding is not static. We are likely to see continued evolution in how anesthesia is coded, especially as technology advances.
-
Electronic Health Records (EHRs): As EHRs become more sophisticated, they will likely do a better job of flagging potential unbundling errors before claims are ever sent.
-
Tele-dentistry Consults: While you cannot administer anesthesia via a screen, pre-operative consultations to determine the need for sedation or specific anesthesia techniques for medically complex patients are becoming more common and may develop their own coding guidelines.
-
Value-Based Care: As the industry shifts towards value-based care (paying for outcomes, not procedures), the focus may shift away from billing for every single injection and more towards bundled payments for an entire episode of care.
Additional Resources for Mastering Dental Coding
You don’t have to memorize every code. Knowing where to find the answers is just as important.
-
The ADA Guide to Reporting D9210: The American Dental Association publishes specific guides and FAQs on their codes. This is the most authoritative source.
-
Your Local Dental Society: Many local and state dental societies offer coding hotlines or workshops for their members. This is an invaluable resource for getting real-time answers to tricky billing questions.
-
Insurance Provider Manuals: Every major insurance company (Delta Dental, MetLife, Cigna, etc.) publishes a provider manual. These manuals contain their specific coding and billing policies. Download them and keep them handy.
-
AAPC (American Academy of Professional Coders): While focused on medical coding, AAPC offers resources and certifications that are highly relevant for those billing complex anesthesia cases to medical carriers.
Conclusion
Mastering the dental code for local anesthesia is less about memorizing four numbers and more about understanding the philosophy of dental billing. It is a story of context. The same injection that is a billable service on a Friday afternoon emergency visit is simply an invisible part of a procedure on a Tuesday morning filling appointment.
By understanding the difference between the D9210 series, recognizing when anesthesia is bundled, and appreciating the role of medical necessity, you can ensure your claims are accurate, compliant, and properly reimbursed. This protects the practice’s revenue and, most importantly, ensures that the focus remains where it should be: on providing comfortable, pain-free care to patients.
Frequently Asked Questions (FAQ)
1. Can I bill D9215 with every filling to get more money from insurance?
No. This is considered “unbundling” and is a form of insurance fraud. Insurance companies have complex software that will deny these claims. Repeatedly doing this can lead to audits and penalties.
2. What is the difference between D9210 and D9211?
The difference lies in the type of injection. D9210 is for standard local infiltration (numbing a small area around a tooth). D9211 is for a regional block, which numbs a larger area, like the entire lower jaw via an inferior alveolar nerve block.
3. My dentist used two full carpules because the patient had “hot” pulpitis and was hard to numb. Can I bill for that extra anesthetic?
Unfortunately, no. The difficulty of achieving anesthesia, even if it requires more medication, is still considered part of the surgical procedure. There is no valid code to bill for “extra” anesthetic used during a procedure.
4. Does medical insurance ever cover local anesthesia for dental treatment?
Yes, but usually only in specific circumstances. If a patient has a qualifying medical condition (like a severe developmental disability or a bleeding disorder) that necessitates treatment in a hospital setting, the anesthesia component might be billed to and covered by their medical plan.
5. What diagnosis code should I use with D9210?
You should use a diagnosis code that reflects the reason for the pain. Common examples include K04.0 (Pulpitis), K04.1 (Necrosis of pulp), K04.7 (Periapical abscess), or K08.8 (Other specified disorders of teeth and supporting structures). The key is that the diagnosis must support the need for the injection.
6. Is nitrous oxide (laughing gas) considered local anesthesia?
No. Nitrous oxide (D9233) is classified as inhalation anxiolysis, a form of minimal sedation. It is coded separately from local anesthesia and is generally a covered benefit if the patient’s plan includes sedation coverage.
Disclaimer: The information provided in this article is for general informational purposes only and does not constitute legal, billing, or professional coding advice. Coding requirements, insurance policies, and regulations are subject to change and vary by payer and jurisdiction. You should always consult with qualified professionals and refer to the current CDT/CPT manuals and specific payer contracts for guidance on billing and coding.