Gastrointestinal (GI) bleeding is not merely a symptom; it is a dramatic clinical event, a crimson flag waved by the body signaling anything from a trivial erosion to a life-threatening malignancy. For clinicians, it’s a diagnostic puzzle demanding swift resolution. For patients, it’s a frightening experience. But in the modern healthcare ecosystem, there is another critical audience for this event: the medical coder. The alphanumeric designations assigned—the ICD-10-CM codes—transform clinical narrative into actionable data that drives reimbursement, influences quality metrics, guides public health initiatives, and fuels critical research.
Coding a GI bleed incorrectly is not a benign clerical error. It can lead to denied claims, skewed hospital performance ratings, misallocation of resources, and flawed epidemiological data. The difference between K25.4 (Chronic or unspecified gastric ulcer with hemorrhage) and K25.0 (Acute gastric ulcer with hemorrhage) hinges on a single documented adjective. The chasm between K92.2 (Gastrointestinal hemorrhage, unspecified) and a more specific code like K62.5 (Hemorrhage of anus and rectum) can mean the difference between adequate and optimal reimbursement, and between vague and valuable health data.
This article is designed to be the definitive guide for medical coders, health information management (HIM) professionals, clinical documentation integrity (CDI) specialists, and even physicians seeking to understand the impact of their documentation. We will embark on a detailed journey through the ICD-10-CM manual, exploring over 9,000 words of in-depth analysis, practical scenarios, and strategic insights. We will dissect the coding pathways for upper and lower GI bleeds, unravel the complexities of combination codes, emphasize the paramount importance of physician documentation, and illuminate the common pitfalls that ensnare even experienced coders. Our goal is to equip you with the knowledge not just to assign a code, but to master the logic and nuance behind coding for gastrointestinal hemorrhage.
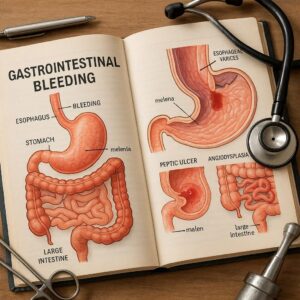
ICD-10-CM Code for Gastrointestinal Bleeding
Table of Contents
ToggleChapter 1: The Anatomy of a GI Bleed – A Coder’s Perspective
Before delving into the code book, a coder must understand the clinical landscape. GI bleeding is categorized by its anatomical origin relative to the ligament of Treitz, which suspends the duodenum.
-
Upper GI Bleed (UGIB): Originates proximal to the ligament of Treitz. This includes the esophagus, stomach, and duodenum. Common causes include peptic ulcers (gastric/duodenal), gastritis, esophageal varices, and Mallory-Weiss tears. Patients may present with hematemesis (vomiting blood, which can be bright red or have a “coffee ground” appearance) and/or melena (black, tarry, foul-smelling stools caused by the digestion of blood).
-
Lower GI Bleed (LGIB): Originates distal to the ligament of Treitz. This encompasses the jejunum, ileum, colon, rectum, and anus. Common causes include diverticulosis, angiodysplasia, colitis (ischemic, infectious, ulcerative), hemorrhoids, and neoplasms. The classic presentation is hematochezia (passage of bright red or maroon blood per rectum), though bleeding from the small bowel can sometimes present as melena.
For the coder, the initial clues are in the diagnosis and the patient’s symptoms documented in the record. However, the final code is determined by the confirmed etiology and site, as identified through procedures like endoscopy, colonoscopy, or capsule endoscopy.
Chapter 2: The ICD-10-CM Framework: Navigating Key Chapters
GI bleed codes are primarily housed in two chapters of the ICD-10-CM manual:
-
Chapter 11: Diseases of the Digestive System (K00-K95): This is the home for most GI bleed codes, particularly those specifying an anatomic site (e.g., gastric ulcer, diverticulosis).
-
Chapter 9: Diseases of the Circulatory System (I00-I99): This chapter contains codes for vascular causes of GI bleeding, most notably esophageal varices (I85) and angiodysplasia of the stomach and duodenum (K31.819 is actually in Ch. 11, but I.D. of intestine I78.8 is in Ch. 9). Hemorrhoids (I84) are also here.
A Fundamental Rule: ICD-10-CM often uses combination codes that specify both the underlying condition AND the manifestation (hemorrhage). This is a critical efficiency of the system. When a combination code exists, you must use it. You do not code hemorrhage separately.
Example: A patient with a bleeding gastric ulcer. The code K25.4 (Chronic gastric ulcer with hemorrhage) is a combination code. You would not additionally code K92.2 (GI hemorrhage, unspecified).
Chapter 3: The Upper GI Bleed Code Set (K25-K28)
This family of codes is for peptic ulcers. Note the 5th digit extension that indicates the complication.
ICD-10-CM Codes for Peptic Ulcer Disease with Hemorrhage
| Code | Description | Clinical Notes for Coders |
|---|---|---|
| K25.0 | Acute gastric ulcer with hemorrhage | Use for a newly diagnosed or acute bleeding gastric ulcer. Documentation of “acute” is key. |
| K25.2 | Acute gastric ulcer with both hemorrhage and perforation | A life-threatening scenario. Requires documentation of both complications. |
| K25.4 | Chronic or unspecified gastric ulcer with hemorrhage | The default for a documented bleeding gastric ulcer when “acute” is not specified. “Unspecified” here relates to the ulcer’s chronicity, not the site. |
| K25.6 | Chronic or unspecified gastric ulcer with both hemorrhage and perforation | |
| K26.0 | Acute duodenal ulcer with hemorrhage | Parallel structure to gastric ulcer codes, but for the duodenum. |
| K26.2 | Acute duodenal ulcer with both hemorrhage and perforation | |
| K26.4 | Chronic or unspecified duodenal ulcer with hemorrhage | Common code for bleeding duodenal ulcers. |
| K26.6 | Chronic or unspecified duodenal ulcer with both hemorrhage and perforation | |
| K27.0 | Acute peptic ulcer, site unspecified, with hemorrhage | Used only when the physician cannot determine if it’s gastric or duodenal (rare with endoscopy). |
| K27.2 | Acute peptic ulcer, site unspecified, with both hemorrhage and perforation | |
| K27.4 | Chronic or unspecified peptic ulcer, site unspecified, with hemorrhage | |
| K27.6 | Chronic or unspecified peptic ulcer, site unspecified, with both hemorrhage and perforation | |
| K28.0 | Acute gastrojejunal ulcer with hemorrhage | For ulcers at a surgical anastomosis (e.g., after a gastrectomy). |
| K28.2 | Acute gastrojejunal ulcer with both hemorrhage and perforation | |
| K28.4 | Chronic or unspecified gastrojejunal ulcer with hemorrhage | |
| K28.6 | Chronic or unspecified gastrojejunal ulcer with both hemorrhage and perforation |
Other Key Upper GI Bleed Codes:
-
K29.01: Acute gastritis with bleeding
-
K29.21: Alcoholic gastritis with bleeding
-
K29.41: Chronic gastritis with bleeding
-
K29.51: Unspecified gastritis with bleeding
-
K22.11: Barrett’s esophagus with bleeding
-
K22.8: Other specified diseases of esophagus (Mallory-Weiss tear is indexed here, K22.8)
-
I85.01: Esophageal varices with bleeding
-
I85.11: Secondary esophageal varices with bleeding
Chapter 4: The Lower GI Bleed Code Set
Lower GI bleeding has a more dispersed set of codes across chapters.
-
Diverticular Disease: K57.41 (Diverticulitis of small intestine with hemorrhage), K57.51 (Diverticulosis of small intestine with hemorrhage), K57.31 (Diverticulitis of large intestine with hemorrhage), K57.41 (Diverticulosis of large intestine with hemorrhage). The 5th digit specifies with or without perforation/abscess.
-
Hemorrhoids: I84.0 – I84.9 (Various types of internal and external hemorrhoids with bleeding). I84.0 is Internal thrombosed hemorrhoids with bleeding.
-
Anal Fissure: K60.3: Anal fissure, unspecified (if bleeding is documented, it may be implied; no specific “with bleeding” code exists. Code the condition).
-
Rectal Bleeding: K62.5: Hemorrhage of anus and rectum. This is a crucial catch-all code for documented rectal bleeding when a more specific cause (hemorrhoids, fissure, ulcer) is not identified.
-
Angiodysplasia/Arteriovenous Malformation (AVM): K31.819 (Angiodysplasia of stomach and duodenum with bleeding), K55.21 (Angiodysplasia of colon with hemorrhage). For small intestinal AVM, see I78.8 (Other diseases of capillaries).
-
Ischemic Colitis: K55.041 (Acute ischemia of large intestine with hemorrhage).
-
Inflammatory Bowel Disease: K51.011 – K51.919 (Various subtypes of ulcerative colitis with rectal bleeding).
-
Post-Procedural Bleeding: K91.840 – K91.849 (Post-procedural hemorrhage of a digestive system organ).
Chapter 5: The Enigma of Unspecified GI Hemorrhage (K92.2)
K92.2 – Gastrointestinal hemorrhage, unspecified is a necessary but often overused code. It should be a last resort.
-
Appropriate Use: When a patient presents with clear signs of a GI bleed (e.g., melena, hematochezia, dropping Hgb), but diagnostic workup (endoscopy/colonoscopy) is inconclusive, not performed due to patient risk, or pending. The site and cause remain truly unknown.
-
Inappropriate Use: When the medical record provides a more specific site or etiology. If an endoscopy report states “bleeding duodenal ulcer,” you must code K26.4 or K26.0, not K92.2. Using K92.2 in this case is a major audit risk and represents a failure of documentation query processes.
Chapter 6: The Importance of Causality: Linking Bleeds to Underlying Etiology
Coding is about causality. A GI bleed is rarely a standalone disease. The coder must establish the cause-and-effect relationship documented by the physician.
-
Drug-Induced: Anticoagulants (warfarin, DOACs), NSAIDs (ibuprofen, naproxen), antiplatelets (aspirin, clopidogrel). You must code the adverse effect (e.g., K25.4 for the ulcer) AND the causative drug (e.g., T45.515A for adverse effect of warfarin). Use codes from T36-T50 with 5th or 6th character ‘5’.
-
Alcohol-Induced: Alcoholic gastritis (K29.21), alcoholic liver disease with variceal bleeding (I85.11, K70.30). Always link the condition to the substance use.
-
Due to Underlying Disease: Portal hypertension causing varices (I85.11), chronic kidney disease contributing to angiodysplasia, a bleeding colon cancer (C18.9, C78.5).
The coder acts as a detective, piecing together the narrative from the history, physical, progress notes, and procedural reports to build an accurate diagnostic picture.
Chapter 7: Documenting for Specificity: What Coders Need from Physicians
Clear physician documentation is the bedrock of accurate coding. CDI specialists and coders should advocate for documentation that answers:
-
Site: Where is the bleed? Stomach, duodenum, sigmoid colon, rectum?
-
Etiology: What is causing it? Ulcer, diverticulum, varices, tumor, AVM?
-
Acuity/Chronicity: Is the ulcer acute or chronic? Is the gastritis acute or chronic?
-
Manifestation: Is hemorrhage/bleeding explicitly stated? (Avoid “Heme positive” or “guaiac positive” alone; these are test results, not diagnoses).
-
Laterality: For diverticulosis/diverticulitis, is it small or large intestine? If large, which part (e.g., sigmoid)?
Example of Poor Documentation: “GI bleed. Likely from diverticulosis.”
Example of Excellent Documentation: “Acute lower GI hemorrhage secondary to actively bleeding diverticulosis of the sigmoid colon, confirmed on colonoscopy.”
Chapter 8: Common Clinical Scenarios and Coding Solutions
-
Scenario 1: A 70-year-old on aspirin and clopidogrel presents with melena. EGD reveals a chronic, actively bleeding duodenal ulcer.
-
Codes: K26.4 (Chronic duodenal ulcer with hemorrhage), T45.515A (Adverse effect of aspirin), T45.525A (Adverse effect of clopidogrel).
-
-
Scenario 2: A patient with a history of cirrhosis presents with massive hematemesis. Emergent EGD shows bleeding esophageal varices.
-
Codes: I85.01 (Esophageal varices with bleeding), K74.60 (Unspecified cirrhosis of liver).
-
-
Scenario 3: A patient presents with hematochezia. Colonoscopy shows blood throughout the colon but no clear source. No angiodysplasia, diverticula, or mass seen. Diagnosis: “Lower GI bleed, unspecified.”
-
Code: K62.5 (Hemorrhage of anus and rectum) is more specific than K92.2 in this context of known lower GI origin.
-
-
Scenario 4: Patient with UC flare presents with 10 bloody bowel movements per day.
-
Code: K51.014 (Ulcerative pancolitis with rectal bleeding) or other specific UC subtype code with final digit ‘4’.
-
Chapter 9: Compliance and Audit Risks: Avoiding Costly Errors
-
Unspecified Code Overuse: Relying on K92.2 when a more specific code is available is a top audit trigger.
-
Missing Combination Codes: Coding both the underlying condition (e.g., K57.30) and a separate hemorrhage code (R58) when a combination code (K57.31) exists.
-
Ignoring Causality: Not linking a bleed to an adverse effect of a medication or an underlying disease.
-
Incomplete Sequencing: In an inpatient setting, the Principal Diagnosis should be the condition chiefly responsible for the admission. For a patient admitted for a bleeding ulcer, the ulcer code (K25.4) should be principal, not the symptom of anemia (D62).
Chapter 10: The Future of GI Bleed Coding: Trends and Predictions
With the advent of artificial intelligence (AI) in clinical documentation and computer-assisted coding (CAC), the role of the human coder will evolve from data entry to data validation and clinical nuance interpretation. Increased specificity in genomics (e.g., coding for bleeding disorders with specific genetic markers) and a continued push for outcome-based reimbursement will place even greater emphasis on perfectly accurate diagnostic coding. The potential for ICD-11-CM on the horizon promises further structural changes, though its U.S. adoption is likely many years away.
Conclusion
Accurate ICD-10-CM coding for gastrointestinal bleeding is a complex but essential skill that requires a synthesis of clinical knowledge, meticulous attention to documentation detail, and a firm grasp of coding guidelines. By moving beyond generic hemorrhage codes to precise etiological and site-specific designations, healthcare professionals ensure proper reimbursement, contribute to high-quality patient data, and support the overall integrity of the healthcare system. Mastery of this topic is not just about compliance—it’s about capturing the true clinical story.
Frequently Asked Questions (FAQs)
Q1: When should I use K92.2 vs. K62.5?
A: Use K92.2 when the origin of the bleed (upper vs. lower) is truly unknown. Use K62.5 when the bleeding is confirmed to be from the rectum/anus (lower GI) but a more specific cause (like hemorrhoids or fissure) is not identified.
Q2: How do I code a GI bleed that is suspected to be from a specific cause, but not yet confirmed?
A: Code what is documented. If the physician documents “suspected diverticular bleed,” you cannot code confirmed diverticulosis with hemorrhage. You may code the symptom (R19.5 Other fecal abnormalities, which includes hematochezia) or K92.2, along with any confirmed conditions. A query may be necessary.
Q3: A patient has both melena and hematochezia. How do I code this?
A: Code the confirmed etiology of the bleed (e.g., K25.4). The symptoms (R11.10 Vomiting of blood, R19.5) are not typically coded separately when the definitive diagnosis is known, as they are integral to the condition.
Q4: What is the most important thing a physician can do to help with accurate GI bleed coding?
A: Provide a clear, concise, and final diagnosis that specifies: 1) Site, 2) Etiology, 3) Presence of hemorrhage, and 4) Acuity (if applicable) in the assessment/plan or procedure report.
Additional Resources
-
Official ICD-10-CM Guidelines: Centers for Disease Control and Prevention (CDC) – The definitive source for coding rules.
-
American Health Information Management Association (AHIMA): ahima.org – Offers publications, webinars, and certification on coding best practices.
-
American Academy of Professional Coders (AAPC): aapc.com – Coding training, certification, and industry news.
-
American College of Gastroenterology (ACG): gi.org – Clinical guidelines and patient education materials on GI bleeding.
Disclaimer
The information contained in this article is for educational and informational purposes only and is not intended as a substitute for professional medical coding advice, consultation, or training. It does not constitute legal or compliance advice. While every effort has been made to ensure the accuracy of the ICD-10-CM codes and guidelines discussed, these are subject to change. Always refer to the most current official ICD-10-CM code set, guidelines, and official coding resources from the CDC and CMS when making coding decisions. The author and publisher disclaim any liability for any loss or damage incurred as a consequence of the use or application of any information presented herein.
Date: December 28, 2025
Author: The Medical Coding Specialist






