In the intricate ecosystem of modern healthcare, two languages constantly interact: the clinical language of diagnosis and treatment, and the administrative language of codes and data. At the heart of this interaction lies the ICD-10-CM (International Classification of Diseases, Tenth Revision, Clinical Modification) system. For a condition as common and clinically significant as acute cholecystitis, accurate coding is not merely a bureaucratic task—it is a vital contributor to patient care quality, epidemiological research, and the financial viability of healthcare institutions. A miscoded case can distort disease prevalence data, trigger a payment denial, or obscure the true severity of a patient’s condition. This article delves deep into the world of ICD-10-CM coding for acute cholecystitis, moving beyond simple code lookup to explore the clinical reasoning, documentation imperatives, and nuanced decision-making that underpin precise code assignment. We will dissect the codes K81.0, K80.00, K80.01, and their companions, transforming you from a code-applier to a knowledgeable coding specialist.
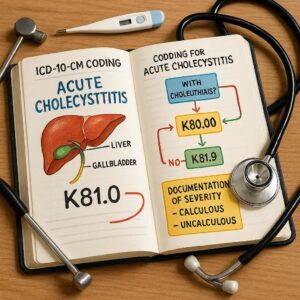
ICD-10-CM Coding for Acute Cholecystitis
2. Understanding Acute Cholecystitis: A Clinical Primer
To code accurately, one must first understand the disease. Acute cholecystitis is the sudden inflammation of the gallbladder wall. In over 90% of cases, this inflammation is triggered by a gallstone (calculus) obstructing the cystic duct, leading to bile stasis, chemical irritation, and often secondary bacterial infection. This is termed acute calculous cholecystitis. The remaining ~5-10% of cases occur in the absence of gallstones, known as acute acalculous cholecystitis, which is often associated with critical illness, major surgery, trauma, burns, or prolonged fasting.
Clinical Presentation: The classic patient presents with:
-
Right Upper Quadrant (RUQ) or Epigastric Abdominal Pain: Often severe, constant, and radiating to the right scapula or shoulder.
-
Fever and Leukocytosis: Signs of systemic inflammation.
-
Palpable Tenderness: Murphy’s sign (arrest of inspiration on RUQ palpation) is a classic physical exam finding.
-
Nausea and Vomiting.
-
Imaging Findings: Ultrasound is the first-line imaging modality, showing gallbladder wall thickening (>3mm), pericholecystic fluid, sonographic Murphy’s sign, and often, visible gallstones.
This clinical understanding is paramount. The coder must recognize that “acute cholecystitis” documented in a post-operative ICU patient likely points to K81.0 (acalculous), while the same phrase in an otherwise healthy middle-aged female immediately raises the question of calculi, steering the coder toward the K80 series.
3. The ICD-10-CM Framework: Chapter 11 (K80-K87)
The ICD-10-CM is logically organized. Acute cholecystitis resides within Chapter 11: Diseases of the Digestive System (K00-K95), specifically in the block K80-K87: Disorders of the gallbladder, biliary tract and pancreas.
A fundamental principle of ICD-10-CM is the “code also” and “code first” instructions. For this block, a crucial note exists: “Use additional code to identify: alcohol abuse and dependence (F10.-), if applicable.” While more relevant for pancreatitis, this highlights the need for thorough review of all conditions.
The two primary subcategories we engage with are:
-
K80: Cholelithiasis (Gallstones)
-
K81: Cholecystitis
The relationship between them is the core of accurate coding for this condition.
4. Decoding K81: Cholecystitis and its Specificity
The K81 category provides options based on chronicity:
-
K81.0: Acute cholecystitis
-
K81.1: Chronic cholecystitis
-
K81.2: Acute cholecystitis with chronic cholecystitis (An acute exacerbation of a chronically inflamed gallbladder)
-
K81.9: Cholecystitis, unspecified
At first glance, K81.0 seems like the straightforward choice for our topic. However, the ICD-10-CM index provides a critical directive. When you look up “Cholecystitis, acute” in the Alphabetic Index, it guides you to “see also Cholelithiasis with cholecystitis.” This is our first clue that K81.0 has a specific application.
5. The Primary Code: K81.0 – Acute Cholecystitis
K81.0 is the code for acute cholecystitis when it is documented as acalculous (without gallstones) OR when the physician’s documentation does not specify the presence or absence of gallstones. It is a “default” code for the acute inflammatory condition when the calculous component is not confirmed.
Clinical Scenarios for K81.0:
-
Post-operative Critical Care Patient: A 65-year-old male, one week after coronary artery bypass grafting, develops fever, RUQ pain, and leukocytosis. Ultrasound confirms acute cholecystitis but shows no gallstones. This is classic acute acalculous cholecystitis. Code: K81.0
-
Vague Documentation: An ER provider documents “Acute cholecystitis” as the final diagnosis without any mention of gallstones on a preliminary read. Until further clarification is obtained, K81.0 is appropriate.
-
Unspecified Cause: The physician explicitly states “acute non-calculous cholecystitis” or “acute acalculous cholecystitis.” Code: K81.0
6. When Calculus is King: The K80 Series (Cholelithiasis) and its Connection
This is where precision becomes paramount. If the patient has gallstones and acute cholecystitis, the coding shifts to the K80 category. The ICD-10-CM guidelines prioritize the combined condition.
The relevant codes are found under K80.0: Calculus of gallbladder with acute cholecystitis. This requires a fifth digit to specify obstruction:
ICD-10-CM Codes for Acute Calculous Cholecystitis
| ICD-10-CM Code | Code Description | Clinical Meaning & Documentation Key |
|---|---|---|
| K80.00 | Calculus of gallbladder with acute cholecystitis without obstruction | Gallstones are present, causing acute inflammation, but the common bile duct (CBD) is clear. Documentation may state “acute calculous cholecystitis” or “acute cholecystitis with cholelithiasis.” No mention of CBD stones or obstruction. |
| K80.01 | Calculus of gallbladder with acute cholecystitis with obstruction | Gallstones are present, causing acute inflammation, AND there is obstruction of the cystic duct or common bile duct. Documentation must mention “with obstruction,” “obstructive,” choledocholithiasis,” “CBD stone,” or elevated LFTs (like bilirubin) pointing to blockage. |
| K81.0 | Acute cholecystitis | Acute inflammation without gallstones (acalculous) OR unspecified cause. |
Decoding the Fifth Digit:
-
.0 (Without Obstruction): The stone is causing trouble locally in the gallbladder/cystic duct but isn’t blocking the main common bile duct. Liver function tests (LFTs) are typically normal or mildly elevated.
-
.1 (With Obstruction): This indicates a more complicated scenario. A stone has migrated and is blocking the common bile duct (choledocholithiasis), leading to potential jaundice, cholangitis, or pancreatitis. Documentation of elevated bilirubin, dilated CBD on imaging, or explicit mention of “obstructive” is key.
Clinical Scenario for K80.00: A 45-year-old female presents with RUQ pain, fever, and positive ultrasound showing gallstones and a thickened gallbladder wall. Her labs show normal bilirubin and no dilation of the CBD. Final Diagnosis: Acute calculous cholecystitis. Code: K80.00
Clinical Scenario for K80.01: The same patient presents, but her labs reveal a bilirubin of 3.5 mg/dL, and an MRCP shows a 6mm stone in the distal common bile duct causing dilation. Final Diagnosis: Acute calculous cholecystitis with choledocholithiasis and biliary obstruction. Code: K80.01
7. The Critical Role of the Provider: Documentation is Everything
The coder is bound by the provider’s documentation. Ambiguity leads to coding errors. Ideal documentation is explicit:
-
Poor Documentation: “Acute cholecystitis.”
-
Better Documentation: “Acute calculous cholecystitis.”
-
Best Documentation: “Acute calculous cholecystitis with choledocholithiasis and biliary obstruction.”
The coder’s responsibility when documentation is unclear is to query the provider. A formal query might ask: “Can you clarify if the acute cholecystitis is calculous or acalculous? Additionally, is there evidence of biliary obstruction?” This process ensures accurate code assignment and protects both clinical and coding integrity.
8. Associated Conditions and Complication Codes
Acute cholecystitis does not exist in a vacuum. Coders must be vigilant for associated conditions that require additional codes.
-
Gangrenous or Emphysematous Cholecystitis: These are severe, life-threatening complications. They are not coded separately. The physician’s documentation of “gangrenous cholecystitis” or “emphysematous cholecystitis” is captured under the same codes (K81.0, K80.00, or K80.01). The severity is inherent in the diagnosis.
-
Perforation of the Gallbladder (K82.2): If the gallbladder ruptures, this is a separate, codable condition. You would code both the acute cholecystitis code (e.g., K80.01) and K82.2.
-
Cholangitis (K83.0): Infection of the bile ducts. Often occurs with obstruction (K80.01). Code separately if documented.
-
Biliary Acute Pancreatitis (K85.1): A stone obstructing the ampulla of Vater can cause pancreatitis. Code separately.
-
Sepsis (A41.9): If the infection becomes systemic. Code sepsis first, followed by the acute cholecystitis code.
9. A Step-by-Step Coding Algorithm & Decision Tree
-
Identify the Diagnosis: Confirm “Acute Cholecystitis” is documented.
-
Check for Calculus: Does the documentation mention gallstones, cholelithiasis, or calculi?
-
NO → Proceed to Step 3.
-
YES → Proceed to Step 4.
-
-
Acalculous/Unspecified: Assign K81.0. Stop.
-
Calculous Confirmed: You are in the K80.0 category. Check for Obstruction.
-
Does documentation mention obstruction, obstructive, choledocholithiasis, CBD stone, dilated CBD, or significantly elevated bilirubin?
-
NO → Assign K80.00.
-
YES → Assign K80.01.
-
-
-
Check for Complications: Review the record for gangrene, perforation (K82.2), cholangitis (K83.0), etc. Add codes as necessary.
-
Query if Uncertain: If any element is unclear, initiate a physician query.
10. Common Pitfalls, Audits, and Denials
-
Pitfall 1: Automatically coding K81.0 for every case of acute cholecystitis. This ignores the calculous/obstruction specificity and can lead to under-coding (loss of justified reimbursement) or over-coding (if K81.0 is used when K80.01 is correct).
-
Pitfall 2: Assuming “obstruction” is always present with acute cholecystitis. Cystic duct obstruction is implied; the “obstruction” in K80.01 specifically refers to common bile duct obstruction.
-
Pitfall 3: Missing complication codes like perforation, which significantly impact DRG assignment and reimbursement.
-
Audit Risk: K80.01 pays at a higher severity level than K80.00 or K81.0 in many DRG and APRV systems. Using K80.01 without supporting documentation is a major audit trigger.
-
Denial: A claim for K80.01 submitted with only normal LFTs and no mention of obstruction will likely be denied or downcoded.
11. The Impact of Accurate Coding: Beyond Reimbursement
While correct reimbursement is crucial, accurate coding for acute cholecystitis has broader implications:
-
Patient Care & Outcomes: Accurate data helps identify trends (e.g., rise in acalculous cases post-pandemic). It fuels quality improvement projects.
-
Public Health & Research: Epidemiologists rely on coded data to study the incidence, risk factors, and complications of biliary disease.
-
Operational Planning: Hospital administrators use this data to plan surgical volumes, ICU needs, and resource allocation.
-
Clinical Decision Support: Accurate historical coding data can power algorithms that help diagnose future patients.
12. Conclusion
Mastering ICD-10-CM coding for acute cholecystitis requires a bridge between clinical knowledge and coding rules. It hinges on understanding the disease, meticulously reviewing provider documentation for the presence of calculi and obstruction, and applying the precise code from the K80.0 series or K81.0. By embracing this nuanced approach, coders ensure data integrity, support optimal patient care, and safeguard the financial health of their institutions. Remember, in the language of healthcare data, precision is paramount.
13. Frequently Asked Questions (FAQs)
Q1: The surgeon’s note says “acute and chronic cholecystitis.” What code do I use?
A: This is a distinct diagnosis: Acute cholecystitis with chronic cholecystitis (K81.2). You would not use K81.0 or the K80.0x codes in this specific case unless cholelithiasis is also documented, which would require careful review of the hierarchy in the Tabular List.
Q2: The ultrasound report says “cholelithiasis,” but the discharge summary only lists “acute cholecystitis.” Can I code the stones?
A: No. You must code based on the physician’s final diagnostic statement. The ultrasound is a diagnostic finding that informs the physician’s diagnosis. If the physician does not incorporate “calculous” into their final diagnosis, you should query for clarification. Do not code from imaging reports alone.
Q3: What is the code for gangrenous cholecystitis with stones?
A: There is no separate code for gangrenous cholecystitis. You code the underlying acute cholecystitis. If it is calculous and obstructive, you would assign K80.01. The “gangrenous” descriptor indicates severity but is not separately coded.
Q4: How do I code acute cholecystitis that progressed to septic shock?
A: You would sequence the codes based on the reason for the encounter. Typically, the life-threatening condition (sepsis) is coded first:
-
First: Code for Sepsis (e.g., A41.9)
-
Second: Code for the acute cholecystitis (e.g., K80.00, K80.01, or K81.0)
-
Additional: Code for Septic shock (R65.21) if applicable.
14. Additional Resources & References
-
Official Source: The Centers for Medicare & Medicaid Services (CMS) and the National Center for Health Statistics (NCHS) provide the official ICD-10-CM Guidelines and Tabular/Index Files.
-
Coding Authority: The American Health Information Management Association (AHIMA) (ahima.org) and the American Academy of Professional Coders (AAPC) (aapc.com) offer certifications, newsletters, and continuing education on complex coding topics.
-
Clinical Reference: UpToDate (uptodate.com) and clinical textbooks like Sabiston Textbook of Surgery provide in-depth clinical background essential for understanding physician documentation.
Disclaimer: The information provided in this article is for educational and informational purposes only. It is not intended as medical advice, coding advice, or a substitute for professional clinical judgment. Medical coders must always refer to the most current official ICD-10-CM coding guidelines, payer-specific policies, and consult with qualified coding professionals and physicians for accurate code assignment. The author and publisher assume no liability for errors or omissions.
Date: December 23, 2025
Author: Clinical Coding Specialist






