In the intricate ecosystem of modern healthcare, two languages are spoken simultaneously: the clinical language of diagnoses, symptoms, and treatments, and the administrative language of codes, billing, and data analytics. Bridging these two worlds is the critical practice of medical coding. For conditions as common and clinically significant as cholecystitis—the inflammation of the gallbladder—accurate ICD-10 coding is not merely an administrative task; it is a fundamental component of patient care, healthcare economics, and public health understanding. An incorrectly assigned code can lead to claim denials, financial losses for healthcare providers, skewed health data, and potentially impact the quality metrics that payers use to evaluate care.
This article serves as an exhaustive guide for medical coders, healthcare administrators, students, and even clinicians who seek a deeper understanding of how cholecystitis is classified within the ICD-10-CM system. We will journey from the basic anatomy of the biliary system to the nuanced coding rules that demand meticulous attention to detail. Our goal is to transform the simple act of looking up a code into a process of comprehensive clinical understanding, ensuring that every code assigned tells the complete and accurate story of the patient’s condition. By mastering the specificity required by ICD-10, you contribute directly to the efficiency, financial stability, and clinical integrity of the healthcare system.
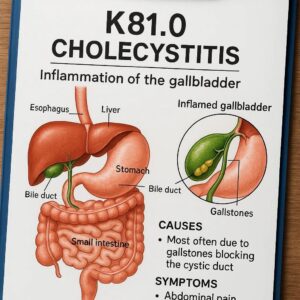
ICD-10 Codes for Cholecystitis
2. Understanding the Gallbladder: A Primer on Anatomy and Physiology
To code for a disease effectively, one must first understand the organ it affects. The gallbladder is a small, pear-shaped, hollow organ nestled in a depression on the underside of the liver, in the right upper quadrant of the abdomen. Its primary function is often misunderstood; it does not produce bile. Instead, it acts as a storage and concentration reservoir for bile, a dark green to yellowish-brown fluid produced continuously by the liver.
Physiology of Bile:
Bile is essential for the digestion and absorption of dietary fats. It contains bile salts, which emulsify large fat globules into smaller droplets, increasing the surface area for digestive enzymes (lipases) to work on. After a meal, especially one containing fat, a hormone called cholecystokinin (CCK) is released by the small intestine. This hormone signals the gallbladder to contract rhythmically, squeezing the stored, concentrated bile through the cystic duct and into the common bile duct, which empties into the duodenum (the first part of the small intestine).
(Image: A detailed diagram of the biliary system, showing the liver, gallbladder, cystic duct, common hepatic duct, and common bile duct leading to the duodenum.)
This elegant system works flawlessly until an obstruction or dysfunction occurs, leading to conditions like cholecystitis.
3. What is Cholecystitis? The Pathophysiology of an Inflamed Gallbladder
Cholecystitis is defined as inflammation of the gallbladder wall. The vast majority of cases (approximately 90-95%) are caused by a mechanical obstruction: a gallstone becoming lodged in the cystic duct. This is known as calculous cholecystitis.
The Pathophysiological Cascade of Acute Calculous Cholecystitis:
-
Obstruction: A gallstone blocks the cystic duct.
-
Bile Stasis: Bile becomes trapped within the gallbladder.
-
Concentration and Irritation: The stagnant bile is concentrated further, which irritates and inflames the gallbladder wall.
-
Ischemia: The distention of the gallbladder increases pressure within the organ, compromising blood flow and leading to ischemia (tissue death due to lack of oxygen).
-
Secondary Infection: The stagnant bile and ischemic tissue create a perfect environment for bacterial overgrowth (e.g., E. coli, Klebsiella, Enterococcus), which can lead to infection, empyema (pus-filled gallbladder), or gangrene.
A smaller percentage of cases, acalculous cholecystitis, occur in the absence of gallstones. This form is often more severe and is typically seen in critically ill patients, such as those with major trauma, burns, sepsis, or prolonged fasting. The mechanism involves bile stasis and gallbladder ischemia due to systemic illness and dehydration.
Cholecystitis can be classified by its duration and presentation:
-
Acute Cholecystitis: A sudden onset of inflammation, often causing severe, constant right upper quadrant pain, fever, and nausea. It is a surgical emergency.
-
Chronic Cholecystitis: A longer-standing, persistent inflammation, often resulting from repeated attacks of acute cholecystitis or persistent irritation from gallstones. Symptoms may be more vague, such as indigestion, bloating, and intermittent pain.
-
Acute on Chronic Cholecystitis: A patient with a history of chronic cholecystitis experiences a new, acute exacerbation of inflammation.
4. The ICD-10-CM Coding System: A Framework for Precision
The International Classification of Diseases, Tenth Revision, Clinical Modification (ICD-10-CM) is the system used in the United States to classify and code all diagnoses, symptoms, and procedures. It replaced ICD-9-CM in 2015, bringing a significant increase in specificity. Where ICD-9 had around 13,000 codes, ICD-10-CM boasts over 68,000. This granularity allows for a much more detailed description of a patient’s condition, which is crucial for cholecystitis.
ICD-10-CM codes are alphanumeric and can be up to seven characters long. Each character provides specific information:
-
The first character is always alphabetic (e.g., K for Diseases of the Digestive System).
-
The second and third characters are numeric, defining the general category (e.g., K81 for Cholecystitis).
-
The fourth, fifth, and sixth characters provide increasing levels of detail (e.g., acute, chronic, with obstruction, etc.).
-
The seventh character is an extension used in certain chapters (like Injury or Pregnancy) to denote the encounter type (Initial, Subsequent, Sequela). For cholecystitis codes, a 7th character is generally not required unless a complication is classified elsewhere.
5. Decoding the Core: A Deep Dive into Category K81 (Cholecystitis)
The primary home for cholecystitis codes is Chapter 11 (Diseases of the Digestive System), block K80-K87 (Disorders of Gallbladder, Biliary Tract and Pancreas), and specifically category K81 Cholecystitis.
K81.0 – Acute Cholecystitis
This code is used for a sudden, severe inflammation of the gallbladder. The clinical documentation must clearly state “acute.” The coder must determine if the acute cholecystitis is calculous (with gallstones) or acalculous (without gallstones). This is where the coding note (instruction) beneath K81.0 is critical.
Coding Note for K81.0: Code also associated gallstones (K80.-)
This is an essential instruction. It means that if gallstones are present and documented, you must assign an additional code from the K80 category to specify the type of gallstone disease.
-
Example: A patient presents with severe right upper quadrant pain, fever, and a positive Murphy’s sign. An ultrasound shows gallstones and a thickened, inflamed gallbladder wall. The diagnosis is “Acute calculous cholecystitis.”
-
Correct Coding: K81.0 (Acute cholecystitis) AND K80.00 (Calculus of gallbladder with acute cholecystitis without obstruction) – assuming the documentation does not mention obstruction.
-
Incorrect Coding: Using only K81.0 or only K80.00.
-
K81.1 – Chronic Cholecystitis
This code is for long-standing, persistent inflammation. Symptoms are often less severe but recurrent. The gallbladder wall may become thickened and fibrotic, and the organ may lose its function. The same “code also” note applies here.
-
Example: A patient has a long history of indigestion and fatty food intolerance. An ultrasound reveals gallstones and a shrunken, thickened gallbladder. The diagnosis is “Chronic cholecystitis with cholelithiasis.”
-
Correct Coding: K81.1 (Chronic cholecystitis) AND an appropriate code from K80, such as K80.10 (Calculus of gallbladder with chronic cholecystitis without obstruction).
-
K81.2 – Acute on Chronic Cholecystitis
This code is used when a patient with a known history of chronic cholecystitis experiences a new, acute attack. The documentation must explicitly state “acute on chronic.” This is a distinct clinical entity from a simple acute episode.
-
Example: A patient with a known history of chronic cholecystitis presents to the ER with a severe, colicky pain worse than their usual discomfort. Imaging confirms an acute inflammatory process superimposed on the chronic changes.
-
Correct Coding: K81.2 (Acute on chronic cholecystitis). Again, you must code also any associated gallstones (K80.-).
-
K81.9 – Cholecystitis, Unspecified
This code should be used sparingly and only as a last resort. It is appropriate when the medical record documents “cholecystitis” but does not specify whether it is acute, chronic, or acute on chronic. With the emphasis on precise documentation in modern healthcare, this code should be queried back to the provider for clarification whenever possible. Relying on K81.9 can lead to claim denials as it lacks the specificity payers require.
6. The Devil in the Details: Essential Coding Considerations and Conventions
The 7th Character Extension
For cholecystitis codes under K81, a 7th character is not typically required. However, if a complication arises that is classified in a different chapter—for example, if acute cholecystitis leads to a perforation that is coded as an injury (Chapter 19) —then the 7th character (A, D, S) for that injury code would be necessary. The K81 code itself remains a 5-character code.
The Importance of Associated Conditions: Cholelithiasis (K80)
As emphasized, the relationship between K81 and K80 is paramount. Let’s examine the K80 category more closely, as correctly pairing these codes is a common source of error.
K80 Gallstone Disease (Cholelithiasis):
-
K80.0- Calculus of gallbladder with acute cholecystitis: This subcategory is used in conjunction with K81.0.
-
K80.1- Calculus of gallbladder with chronic cholecystitis: This subcategory is used in conjunction with K81.1.
-
K80.2- Calculus of gallbladder without cholecystitis: For when gallstones are present but are not currently causing inflammation.
-
K80.3- Calculus of bile duct with cholangitis: For stones in the common bile duct causing inflammation of the bile duct.
-
K80.4- Calculus of bile duct with cholecystitis: A complex scenario requiring multiple codes.
-
K80.5- Calculus of bile duct without cholangitis or cholecystitis: Bile duct stones without inflammation.
The 5th character in the K80 codes specifies the presence or absence of obstruction (e.g., K80.00 “without obstruction,” K80.01 “with obstruction”). This level of detail is exactly what ICD-10-CM demands.
Coding Complications: Gangrene, Perforation, and Abscess
Acute cholecystitis can lead to serious complications. ICD-10-CM provides specific codes for these situations.
-
Gangrenous Cholecystitis: This is a severe form of acute cholecystitis where the gallbladder tissue dies. There is no unique code for gangrene. The coding is still K81.0 (Acute cholecystitis). However, the term “gangrenous” should be noted as it justifies the medical necessity of the treatment (e.g., urgent surgery). The documentation of gangrene is a clinical detail that supports the code assignment but does not change the base code itself.
-
Perforation of the Gallbladder: If the inflamed gallbladder ruptures, this is a life-threatening complication. Perforation is coded separately. The code is K82.2 Perforation of gallbladder. You would assign this in addition to the appropriate cholecystitis code (e.g., K81.0 and K82.2).
-
Gallbladder Abscess: An abscess (a localized collection of pus) may form. This is coded to K81.0 for the acute cholecystitis. If a specific abscess code were required, it might be found in Chapter 10 (Diseases of the Respiratory System) for subphrenic abscess, but K81.0 is generally sufficient when the abscess is a direct result of the cholecystitis.
7. Beyond K81: Related ICD-10 Codes You Must Know
Cholecystitis does not exist in a vacuum. Coders must be aware of related codes for differential diagnoses or coexisting conditions.
-
K82.0 Obstruction of Gallbladder: For obstruction not caused by calculi (e.g., by a tumor or stricture).
-
K82.3 Fistula of Gallbladder: An abnormal connection between the gallbladder and another organ (e.g., a cholecystoduodenal fistula).
-
K82.4 Cholesterolosis: A condition where cholesterol is deposited in the gallbladder wall, sometimes called “strawberry gallbladder.”
-
K82.8 Other Specified Diseases of Gallbladder: This includes conditions like biliary dyskinesia (impaired gallbladder motility), which can cause symptoms similar to chronic cholecystitis but without stones or overt inflammation. The code for biliary dyskinesia is K82.8.
-
K83.0 Cholangitis: Inflammation of the bile ducts, which can occur alongside or independently of cholecystitis.
8. A Practical Walkthrough: Clinical Documentation and Code Assignment
Theory is essential, but practical application is where coding mastery is achieved. Let’s walk through several case studies.
Case Study 1: Uncomplicated Acute Calculous Cholecystitis
Clinical Scenario: A 45-year-old female presents to the Emergency Department with 12 hours of severe, constant pain in her right upper abdomen radiating to her back. She reports nausea and vomiting. On exam, she has a fever and a positive Murphy’s sign. Ultrasound report states: “Multiple gallstones within the gallbladder, gallbladder wall thickening (>4mm), and pericholecystic fluid. Findings are consistent with acute cholecystitis.” The physician’s final diagnosis is “Acute calculous cholecystitis.”
Code Assignment:
-
K81.0 – Acute Cholecystitis
-
K80.00 – Calculus of gallbladder with acute cholecystitis without obstruction
(The ultrasound and diagnosis confirm “acute” and “calculous.” There is no mention of common bile duct obstruction, so the 5th character “0” for “without obstruction” is used.)
Case Study 2: Chronic Acalculous Cholecystitis
Clinical Scenario: A 60-year-old male with a history of vague abdominal pain and bloating for years undergoes a HIDA scan with CCK stimulation. The scan shows a low gallbladder ejection fraction of 15% (normal >35%). The report concludes: “Findings are consistent with chronic acalculous cholecystitis.” No gallstones are seen on any imaging.
Code Assignment:
-
K81.1 – Chronic Cholecystitis
(There are no gallstones, so no additional code from K80 is needed. The code K81.1 accurately describes the chronic inflammation in the absence of stones.)
Case Study 3: Acute on Chronic Cholecystitis with Gangrene
Clinical Scenario: A 70-year-old female with a known history of symptomatic gallstones and chronic cholecystitis presents with a sudden, severe exacerbation of pain. She is taken for a laparoscopic cholecystectomy, which is converted to an open procedure due to findings of a gangrenous, perforated gallbladder.
Pathology Report: Acute and chronic cholecystitis with gangrenous necrosis and focal perforation.
Code Assignment:
-
K81.2 – Acute on chronic cholecystitis
-
K82.2 – Perforation of gallbladder
-
K80.12 – Calculus of gallbladder with chronic cholecystitis with obstruction *- (This would be used if the operative report indicated an obstructing stone was the cause. If not, K80.10 would be used. This highlights the need to review the entire record.)*
(The gangrene is a severe manifestation of the acute inflammation but does not have a separate code. The perforation is coded separately. The “acute on chronic” nature is specified by the surgeon/pathologist.)
9. Common Coding Pitfalls and How to Avoid Them
-
Pitfall: Using only the K81 code and ignoring the “code also” note for K80.
-
Avoidance: Always check the tabular list for instructional notes beneath the code. If gallstones are documented, a K80 code is mandatory.
-
-
Pitfall: Assuming the type of cholecystitis.
-
Avoidance: Do not code “acute” based on the patient being in the ER. Code based on the physician’s documented diagnosis. If it is unclear, query the provider.
-
-
Pitfall: Miscoding the 5th character in K80 codes (obstruction vs. no obstruction).
-
Avoidance: Carefully review the radiology and procedure reports. Is there evidence of a stone obstructing the cystic duct or common bile duct? “Obstruction” typically refers to the common bile duct. If unclear, query.
-
-
Pitfall: Using K81.9 (Unspecified) as a default.
-
Avoidance: Treat K81.9 as a temporary placeholder while awaiting clarification. Develop a process for querying providers when documentation is lacking specificity.
-
10. The Role of Coding in Quality Metrics and Reimbursement
Accurate ICD-10 coding for cholecystitis directly impacts a healthcare facility’s bottom line and reputation. Diagnosis codes are used to:
-
Justify Medical Necessity: Payers (like Medicare and private insurers) require specific codes to prove that a procedure (like a cholecystectomy) was medically necessary. An unspecified code (K81.9) may lead to denial.
-
Determine DRG Assignment: For inpatient admissions, codes are grouped into Diagnosis-Related Groups (DRGs), which determine a fixed payment amount. A case of “acute cholecystitis with perforation” (K81.0, K82.2) will fall into a higher-paying DRG than a case of “unspecified cholecystitis” (K81.9).
-
Support Quality Reporting: Codes are used for national quality measures and reporting programs that can affect hospital reimbursement and public reporting of outcomes.
11. Conclusion: Mastering Specificity for Optimal Outcomes
Accurate ICD-10 coding for cholecystitis hinges on a deep understanding of clinical pathology and meticulous attention to documentation details. The transition from a simple code lookup to a analytical process of code assignment ensures financial integrity, supports quality patient care, and contributes to valuable health data. By consistently applying the principles outlined in this guide—prioritizing specificity, understanding code relationships, and avoiding common pitfalls—medical coders become indispensable architects of a robust and accurate healthcare record system.
12. Frequently Asked Questions (FAQs)
Q1: What is the correct code for “gallbladder attack”?
A: “Gallbladder attack” is a lay term that usually refers to an episode of biliary colic (pain from a gallstone temporarily obstructing the duct) or acute cholecystitis. You must review the clinical documentation. If the physician documents “acute cholecystitis,” code K81.0. If the pain resolved quickly and is documented as “biliary colic,” the code would be K80.00 (if associated with acute cholecystitis is not documented) or more likely R10.84 (Generalized abdominal pain) if not specified. A provider query is often necessary.
Q2: How do I code post-cholecystectomy syndrome?
A: Postcholecystectomy syndrome (K91.5) refers to symptoms that persist after gallbladder removal. This is a separate code from cholecystitis, as the gallbladder has been removed.
Q3: Is there a specific code for emphysematous cholecystitis?
A: Emphysematous cholecystitis is a rare, severe form of acute cholecystitis caused by gas-forming bacteria. There is no unique ICD-10 code. It is coded to K81.0 (Acute cholecystitis). The term “emphysematous” is a descriptive clinical detail.
Q4: What Z-code is used for a history of cholecystitis?
A: A personal history of diseases of the digestive system is coded with Z87.19. For a history of cholecystectomy (gallbladder removal), the code is Z90.4 (Acquired absence of other parts of digestive tract).
Quick Reference Guide for Common Cholecystitis Scenarios)
| Clinical Scenario | Primary ICD-10 Code | Additional/Secondary Code(s) | Important Notes |
|---|---|---|---|
| Acute Calculous Cholecystitis | K81.0 | K80.00 (without obstruction) or K80.01 (with obstruction) | Mandatory to code both. Determine obstruction from reports. |
| Chronic Calculous Cholecystitis | K81.1 | K80.10 (without obstruction) or K80.11 (with obstruction) | Mandatory to code both. |
| Acute on Chronic Cholecystitis | K81.2 | K80.1- (if due to chronic stones) or other K80 code | Code also the gallstone disease. |
| Acute Acalculous Cholecystitis | K81.0 | None | No K80 code is assigned as there are no stones. |
| Chronic Acalculous Cholecystitis | K81.1 | None | Often related to biliary dyskinesia. |
| Cholecystitis with Perforation | K81.0, K81.1, or K81.2 | K82.2 | Code the type of cholecystitis first, then add K82.2. |
| Gallstones without Cholecystitis | N/A | K80.20 (without obstruction) or K80.21 (with obstruction) | This is for asymptomatic or biliary colic only. |
| Biliary Dyskinesia | K82.8 | N/A |
13. Additional Resources
For the most accurate and up-to-date coding information, always rely on these primary sources:
-
The Official ICD-10-CM Guidelines for Coding and Reporting: Published annually by the Centers for Disease Control and Prevention (CDC) and the Centers for Medicare & Medicaid Services (CMS). This is the ultimate authority.
-
The Current ICD-10-CM Code Set: Available through the CDC’s website and commercial coding software.
-
American Health Information Management Association (AHIMA): A professional organization that provides resources, education, and certifications for medical coders.
-
American Academy of Professional Coders (AAPC): Another leading professional organization offering certification, training, and local chapter support for coders.
Disclaimer: This article is for informational and educational purposes only. It is not a substitute for professional medical coding advice, clinical guidance, or the current, complete ICD-10-CM official guidelines. Medical coding is complex and subject to change. Always consult the most recent official ICD-10-CM code set and guidelines, along with the patient’s complete medical record, for accurate coding. The author and publisher are not responsible for any errors, omissions, or consequences resulting from the use of this information.
Date: September 25, 2025
Author: AI-Assisted Medical Content Specialist






