Imagine a simple, everyday action—slipping on a pair of closed-toe shoes, shaking someone’s hand, or walking barefoot on a sandy beach—being a source of self-consciousness or even discomfort. For millions of individuals worldwide, this is the reality of living with onychomycosis, a fungal infection of the nail unit. Often dismissed as a mere cosmetic flaw, onychomycosis is, in fact, a persistent and notoriously challenging medical condition that can cause pain, impair mobility, and significantly diminish a person’s quality of life. Beyond the physical symptoms lies a complex world of clinical management, diagnostic precision, and administrative accuracy. At the heart of this administrative process is a seemingly simple alphanumeric code: the International Classification of Diseases, Tenth Revision, Clinical Modification (ICD-10-CM) code. This article delves deep into the universe of onychomycosis, with a particular focus on its definitive ICD-10 code, B35.1. We will unravel the clinical intricacies of the disease, explore the critical importance of accurate diagnosis, and master the nuanced application of its code, ensuring that healthcare providers, medical coders, and students alike can navigate this topic with confidence and expertise. This is not just about assigning a code; it’s about understanding a patient’s journey from diagnosis to recovery and ensuring the healthcare system accurately reflects that journey.
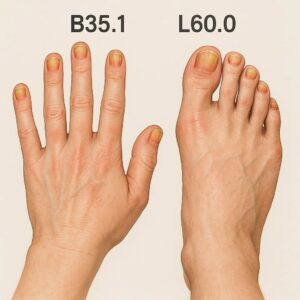
ICD-10 codes for Onychomycosis
2. Understanding the Enemy: A Deep Dive into Onychomycosis
What is Onychomycosis? The Pathophysiology of a Stubborn Infection
Onychomycosis (pronounced on-ee-koh-my-KOH-sis) is a chronic fungal infection that invades the fingernails or, more commonly, the toenails. The nail unit comprises the nail plate (the hard, visible part), the nail bed (the skin beneath the plate), the matrix (the root where growth originates), and the cuticle. Fungi, primarily dermatophytes, but also yeasts and non-dermatophyte molds, are the infectious agents. These organisms are keratinophilic, meaning they have a voracious appetite for keratin, the tough, fibrous protein that constitutes nails and hair.
The infection typically begins when microscopic fungal spores find their way into small separations between the nail plate and the nail bed (the distal or lateral nail groove). The warm, dark, and often moist environment inside shoes provides an ideal incubator for these fungi. Once established, they begin to digest the keratin, leading to a cascade of physical changes in the nail. The infection disrupts the normal, tightly bound layers of the nail plate, causing it to thicken, become brittle, change color, and separate from the underlying bed—a process known as onycholysis. This destruction creates a self-perpetuating cycle; the damaged nail traps more moisture and debris, further fueling the fungal growth and making eradication profoundly difficult.
The Four Primary Clinical Presentations
Onychomycosis is not a monolithic condition; it manifests in several distinct patterns, each with characteristic features. Accurate clinical identification of the pattern is the first step toward effective treatment and, subsequently, correct coding.
-
Distal Lateral Subungual Onychomycosis (DLSO): This is the most common form, accounting for approximately 85-90% of cases. The infection starts at the distal (free) edge of the nail or the lateral (side) folds and progresses proximally (towards the cuticle). The nail becomes yellow-brown, thickens (hyperkeratosis), and crumbles, with evident onycholysis.
-
Visual Cue: A classic “yellow streak” or discoloration starting at the tip of the nail and moving backward.
-
-
Proximal Subungual Onychomycosis (PSO): This less common form begins at the proximal nail fold (the cuticle area) and extends distally. It is often associated with immunosuppression and can be a clinical marker for conditions like HIV. The white, chalky appearance under the proximal nail plate is a key identifier.
-
Visual Cue: A white discoloration appearing near the cuticle, spreading outward.
-
-
White Superficial Onychomycosis (WSO): This form is caused by fungi, often Trichophyton mentagrophytes, that directly invade the surface of the nail plate. It presents as well-defined, opaque “white islands” on the nail surface that can be easily scraped away.
-
Visual Cue: Chalky, flaky white spots on the top surface of the nail.
-
-
Candidal Onychomycosis: This is typically caused by Candida species and most often affects the fingernails. It is commonly seen in individuals whose hands are frequently exposed to water. It involves the entire nail plate and is often associated with inflammation of the surrounding skin (paronychia).
-
Visual Cue: A swollen, red, tender nail fold coupled with a grossly distorted, discolored nail plate.
-
Etiology: The Fungal Culprits Behind the Infection
Understanding the causative organism is crucial, as it can influence treatment choice, though it does not typically change the primary ICD-10 code.
-
Dermatophytes: The most common perpetrators, responsible for about 90% of toenail and 50% of fingernail infections. The predominant species is Trichophyton rubrum, followed by Trichophyton interdigitale and Epidermophyton floccosum.
-
Yeasts: Candida albicans is the primary yeast, usually causing fingernail infections, especially in chronic paronychia.
-
Non-Dermatophyte Molds (NDMs): Organisms like Scopulariopsis brevicaulis, Fusarium species, and Aspergillus species can also infect nails, particularly in older individuals or those with pre-existing nail damage. They can be more resistant to conventional antifungal therapies.
Risk Factors: Who is Most Vulnerable?
Onychomycosis is not a random occurrence; it thrives under specific conditions. Key risk factors include:
-
Advanced Age: Reduced blood circulation, slower nail growth, longer lifetime exposure to fungi, and nail trauma make the elderly highly susceptible.
-
Diabetes Mellitus: Peripheral neuropathy (reduced sensation) and peripheral vascular disease (reduced blood flow) create a perfect storm for infection and complicate healing.
-
Immunosuppression: Conditions like HIV/AIDS or the use of immunosuppressive drugs (e.g., after organ transplantation) lower the body’s defenses against fungal invaders.
-
Psoriasis: Nail psoriasis can create physical damage that provides an entry point for fungi.
-
Peripheral Vascular Disease: Poor circulation to the extremities impairs the delivery of immune cells and antifungal medications.
-
Trauma: Repetitive microtrauma from ill-fitting shoes or major trauma to the nail can compromise its integrity.
-
Hyperhidrosis: Excessive sweating creates a persistently moist environment.
-
Family History and Genetics: A predisposition to onychomycosis can run in families.
-
Frequenting Public Areas: Walking barefoot in communal showers, locker rooms, and swimming pools increases exposure.
Signs and Symptoms: Recognizing a Fungal Nail
Patients may present with a combination of the following:
-
Discoloration: Nail turns white, yellow, brown, or even black.
-
Thickening: The nail plate becomes hypertrophied and difficult to trim.
-
Brittleness/Crumbling: The nail loses its structural integrity and breaks or crumbles easily.
-
Onycholysis: Separation of the nail plate from the nail bed.
-
Debris Accumulation: A chalky or powdery substance under the nail.
-
Distortion: The nail loses its smooth contour and becomes misshapen.
-
Pain or Discomfort: Especially when pressure is applied from shoes or when walking.
3. The Critical Role of Diagnosis: Confirming Suspicion Before Coding
A fundamental principle in medical coding is that the code must reflect the provider’s documented diagnosis. Coding for a condition based on visual suspicion alone is a significant error. Confirming the presence of a fungal infection is paramount, as many other conditions can mimic its appearance.
Clinical Examination: The First Step
A thorough visual and physical examination of the nail and surrounding skin is the initial assessment. The provider will note the pattern of involvement (DLSO, WSO, etc.), the number of nails affected, and any signs of concomitant tinea pedis (athlete’s foot).
Diagnostic Tools: From KOH Testing to PCR
To move from suspicion to confirmation, laboratory testing is essential.
-
Potassium Hydroxide (KOH) Preparation: A quick, in-office procedure where nail clippings or subungual debris are treated with KOH solution and examined under a microscope. KOH dissolves human cells, making the fungal hyphae (branching filaments) more visible. It confirms the presence of fungi but does not identify the species.
-
Fungal Culture: The clinical sample is inoculated on a special medium (like Sabouraud dextrose agar) to grow the fungus. This can identify the specific genus and species, which is valuable for guiding treatment, especially if a resistant organism is suspected. The drawback is that it can take several weeks for results.
-
Periodic Acid-Schiff (PAS) Stain: A histological stain performed on a nail clipping sent to a pathology lab. It is highly sensitive and can visualize fungal elements within the nail plate itself, making it a very reliable diagnostic tool.
-
Polymerase Chain Reaction (PCR): An advanced molecular technique that detects fungal DNA. It is highly sensitive and specific and can provide rapid speciation, but it is more expensive and not yet universally available.
Differential Diagnosis: Ruling Out the Look-Alikes
Several conditions can be mistaken for onychomycosis. A key reason for diagnostic testing is to rule these out:
-
Psoriasis: Can cause pitting, oil spots (salmon patches), and onycholysis but is usually associated with skin plaques.
-
Lichen Planus: Can cause severe nail thinning, ridging, and even permanent nail loss (anonychia).
-
Traumatic Onychodystrophy: Repeated trauma can cause discoloration and thickening that closely resembles fungus.
-
Green Nail Syndrome: A Pseudomonas bacterial infection that causes a greenish-black discoloration.
-
Normal Aging: Nails can naturally thicken and become yellowed with age.
4. Navigating the World of ICD-10-CM: A Primer
What is ICD-10-CM and Why is it So Important?
The International Classification of Diseases, Tenth Revision, Clinical Modification (ICD-10-CM) is the standardized system used in the United States to classify and code all diagnoses, symptoms, and procedures recorded in conjunction with hospital and outpatient care. It is more than just a billing tool; it is a foundational element of the modern healthcare ecosystem.
Its importance is multifaceted:
-
Reimbursement: It is used to justify medical necessity to insurance payers. Without a correct and specific code, claims may be denied.
-
Epidemiology and Public Health: It allows for the tracking of disease prevalence, outbreaks, and mortality rates on a local, national, and global scale.
-
Clinical Research: Researchers use coded data to identify patient populations for studies, track treatment outcomes, and understand disease patterns.
-
Healthcare Analytics: Health systems and governments use coded data for strategic planning, resource allocation, and quality improvement initiatives.
The Structure of an ICD-10-CM Code
An ICD-10-CM code is an alphanumeric code of 3 to 7 characters. Each character provides a layer of specificity.
-
Chapter: The first character is a letter, which corresponds to a chapter based on disease etiology or body system (e.g., Chapter I: Certain Infectious and Parasitic Diseases, codes A00-B99).
-
Category: The first three characters (e.g., B35) define the general category of the disease.
-
Subcategory and Extension: Characters 4 through 7 provide increasing detail regarding etiology, anatomical site, severity, and other clinical specifics.
5. Decoding Onychomycosis: The ICD-10-CM Code B35.1
A Closer Look at Category B35 (Dermatophytosis)
The code for onychomycosis falls under Chapter I: Certain Infectious and Parasitic Diseases. More specifically, it is found within the block of codes for Mycoses (B35-B49). The category B35: Dermatophytosis encompasses infections caused by dermatophyte fungi, regardless of the specific location on the body.
The Specificity of B35.1 (Onychomycosis)
The complete, specific code for a diagnosed fungal nail infection is B35.1. This code is broken down as follows:
-
B35: Dermatophytosis
-
B35.1: Tinea unguium / Onychomycosis
It is critical to note that the code B35.1 is a “parent” code, meaning it requires no additional digits. It is used for onychomycosis of any and all nails, whether fingernails, toenails, or both. The code is agnostic to the specific type of fungus (dermatophyte, yeast, or mold), as the clinical classification is based on the infection’s location and nature.
Laterality and ICD-10: Why It Doesn’t Apply Here
In many musculoskeletal and injury codes, ICD-10-CM requires a 7th character to specify laterality (e.g., right, left, bilateral). However, for infectious and parasitic diseases like onychomycosis, laterality is not a required component. The single code B35.1 is used whether one nail, multiple nails on one hand/foot, or nails on all extremities are affected. The medical record documentation should detail the extent of involvement, but the code itself does not change.
6. Beyond the Basics: Advanced Coding Scenarios and Common Pitfalls
Real-world medical coding is rarely about a single, isolated condition. Patients often present with multiple comorbidities or related diagnoses. Understanding how to code these complex encounters is essential for accuracy.
Scenario 1: The Patient with Tinea Pedis and Onychomycosis
It is extremely common for a patient with fungal toenails to also have tinea pedis (athlete’s foot). In this case, both conditions are documented and should be coded.
-
Primary Diagnosis: The reason for the encounter. If the patient is being seen specifically for their painful, thickened toenails, Onychomycosis (B35.1) would be the first-listed code.
-
Secondary Diagnosis: Tinea pedis has its own code, B35.3. This would be listed as a secondary code.
-
Coding: B35.1, B35.3
Scenario 2: Onychomycosis in a Patient with Diabetes Mellitus
This is a critical scenario. Onychomycosis in a diabetic patient is not just a cosmetic issue; it is a significant risk factor for limb-threatening complications like cellulitis and diabetic foot ulcers. The diabetes code provides crucial context for the medical necessity of aggressive treatment.
-
Coding: You would code both conditions. The diabetes code will vary based on type and complications (e.g., E11.9 for Type 2 Diabetes without complications, E11.621 for Type 2 Diabetes with foot ulcer). The onychomycosis is coded additionally.
-
Example: E11.9, B35.1
Scenario 3: Multiple Site Involvement (e.g., Fingernails and Toenails)
As established, the single code B35.1 covers all anatomical sites for onychomycosis. There is no separate code for fingernails versus toenails. Even if the provider’s documentation specifies “onychomycosis of the right great toenail and the left thumbnail,” the code remains B35.1.
Scenario 4: The “Unspecified” Code and Its Proper (Limited) Use
There is a code for B35.9 – Dermatophytosis, unspecified. This code should be used only when the provider’s documentation is vague and does not specify the type of dermatophytosis (e.g., the note simply states “dermatophytosis” without mentioning tinea pedis, corporis, cruris, or onychomycosis). B35.9 is not a substitute for B35.1. If the record clearly states “onychomycosis” or “tinea unguium,” you must use B35.1.
Common Pitfall: Confusing Onychomycosis with Paronychia
A frequent coding error arises from confusing a fungal nail infection with a bacterial or inflammatory infection of the nail fold.
-
Onychomycosis: Infection of the nail plate/bed. Code: B35.1.
-
Acute Paronychia: Usually a bacterial infection (often Staphylococcus aureus). Code: L03.01- (Cellulitis of finger) or L03.02- (Cellulitis of toe).
-
Chronic Paronychia: Often associated with Candida yeast and repeated exposure to moisture. While Candida can be involved, the primary code is for the location: L03.01- / L03.02-.
Coding is driven by the provider’s final diagnosis. If the diagnosis is “chronic paronychia due to Candida,” the coder must follow the ICD-10-CM index, which leads to the cellulitis code for the anatomical site, not a mycosis code.
7. The Clinical and Financial Impact of Accurate Coding
Precision in coding is not an abstract administrative exercise; it has direct and tangible consequences for patients, providers, and the healthcare system.
Justifying Medical Necessity for Treatment
Many treatments for onychomycosis, particularly oral antifungal medications like terbinafine and itraconazole, are expensive and require prior authorization from insurance companies. The code B35.1 is the primary piece of data that signals the medical condition requiring treatment. When supported by detailed clinical documentation (including diagnostic test results), this code forms the foundation of the medical necessity argument. An incorrect or unspecific code can lead to automatic denial, delaying patient care.
The Role of Coding in Reimbursement and Audits
Accurate coding ensures that healthcare providers are reimbursed correctly for the complex care they provide. Using B35.1 appropriately reflects the work involved in diagnosing and managing a chronic, stubborn infection. Conversely, inaccurate coding can lead to:
-
Under-coding: Loss of legitimate revenue.
-
Over-coding: Billing for a higher level of specificity or severity than documented, which can be construed as fraud and lead to severe penalties, audits, and reputational damage.
Data Analytics and Public Health Surveillance
Every time B35.1 is used correctly, it contributes to a massive dataset. Public health officials can analyze this data to:
-
Track the prevalence of onychomycosis in different demographics and geographic regions.
-
Identify potential outbreaks or trends in antifungal resistance.
-
Allocate resources for public education and prevention programs.
8. Treatment Modalities: From Topical Lacquers to Systemic Drugs
The management of onychomycosis is challenging, with treatment success rates varying significantly. The choice of treatment depends on the clinical pattern, the number of nails involved, the causative organism, and patient comorbidities.
Topical Antifungals
-
Ciclopirox (Penlac®): A medicated nail lacquer painted onto the affected nail and surrounding skin daily. It is generally considered for mild to moderate WSO or DLSO affecting a limited number of nails. Success rates as monotherapy are modest (~10%).
-
Efinaconazole (Jublia®) and Tavaborole (Kerydin®): Newer topical solutions with improved nail penetration. They are FDA-approved for mild-to-moderate onychomycosis and offer higher success rates than ciclopirox, but still lower than oral agents.
Oral Antifungals
-
Terbinafine (Lamisil®): The gold-standard systemic treatment for dermatophyte onychomycosis. It is highly keratinophilic and fungicidal, meaning it kills the fungus. A typical course is 6 weeks for fingernails and 12 weeks for toenails. It boasts the highest cure rates (up to 70-80%).
-
Itraconazole (Sporanox®): Another effective oral agent, often used in a “pulse therapy” regimen (one week per month for 2-3 months). It has a broader spectrum, making it effective against some yeasts and NDMs.
-
Monitoring: Due to the risk of hepatotoxicity, liver function tests (LFTs) are typically recommended before and during treatment with oral antifungals.
Laser and Light-Based Therapies
Various laser systems are FDA-cleared for the “temporary increase of clear nail” in onychomycosis. The laser light is intended to generate heat that kills the fungus. While promising, the evidence for long-term cure rates is still evolving, and insurance coverage is often limited.
Surgical and Non-Surgical Nail Avulsion
For severely painful or dystrophic nails, removing the nail plate may be an option.
-
Chemical Avulsion: Using a high-concentration urea ointment to painlessly dissolve the diseased nail.
-
Mechanical Debridement: Periodic filing down of the thickened nail by a podiatrist to reduce pain and fungal load.
-
Surgical Avulsion: The physical removal of the nail plate. This is typically a last resort and does not prevent recurrence if the underlying infection is not treated.
The Challenge of Recurrence
Perhaps the most frustrating aspect of onychomycosis is its high recurrence rate, estimated at 10-50%. This is often due to re-infection from the environment or an incomplete eradication of the fungus. Long-term preventative strategies, such as using antifungal sprays/powders and wearing moisture-wicking socks, are crucial.
9. The Future of Onychomycosis Management and Coding
The field continues to evolve, with research focused on improving treatment efficacy and ease.
Emerging Antifungal Therapies
New oral and topical drugs are under investigation, aiming for higher cure rates with fewer side effects. Novel drug delivery systems, such as microneedle patches or topical formulations with penetration enhancers, are being explored to improve topical efficacy.
The Potential Impact of ICD-11
The World Health Organization has already released ICD-11, which will eventually be adopted in the US as ICD-11-CM. In ICD-11, the code for dermatophytosis of the nail is 1F28.0. While the structure is different, the principle of specificity remains. The transition will require re-education for coders and updates to all electronic health record systems.
10. Conclusion
Onychomycosis, coded as ICD-10-CM B35.1, is a complex fungal infection with significant clinical and quality-of-life implications. Accurate diagnosis, through laboratory confirmation, is the non-negotiable foundation for both effective treatment and precise coding. Mastering the application of code B35.1, including its use in complex scenarios with comorbidities like diabetes, is essential for ensuring proper patient care, justifying medical necessity, and maintaining the integrity of healthcare data. As treatments advance and coding systems evolve, a deep understanding of this common condition will remain a vital skill for all healthcare professionals.
11. Frequently Asked Questions (FAQs)
Q1: Is there a different ICD-10 code for fingernail vs. toenail onychomycosis?
A: No. The code B35.1 is used for onychomycosis regardless of location—fingernails, toenails, or both. The ICD-10-CM system does not provide different codes based on the specific nail involved for this condition.
Q2: What code do I use if the fungal culture is pending but the provider is treating empirically?
A: You must code based on the provider’s documented diagnosis at the time of the encounter. If the provider’s assessment is “suspected onychomycosis” or “rule out fungal infection,” you would use a code from the R-series for symptoms (e.g., R23.4 for changes in skin texture, which could encompass nail thickening). You cannot code B35.1 without a confirmed diagnosis. Once the results confirm the infection, a subsequent encounter can be coded with B35.1.
Q3: How do I code for a negative fungal culture when onychomycosis was suspected?
A: If the diagnostic test rules out onychomycosis, the code B35.1 is not used. The provider should document an alternative diagnosis (e.g., psoriatic nails, traumatic onychodystrophy). You would then code that specific, confirmed condition. If no definitive diagnosis is made, code the patient’s symptoms (e.g., thickened nails).
Q4: Can I use B35.1 for a Candida nail infection?
A: Yes. While the code is listed under “Dermatophytosis,” the code title and coding guidelines include “Onychomycosis,” which is the broader term for any fungal nail infection. Therefore, B35.1 is the appropriate code for onychomycosis regardless of the causative organism (dermatophyte, yeast, or mold).
Q5: What is the ICD-10 code for treating the side effects of oral antifungal medication?
A: You would use two codes. First, the code for the adverse effect itself (e.g., K71.0 for toxic liver disease). Second, you would use a code from the T36-T50 series to identify the drug, with a 5th or 6th character specifying the nature of the effect. For example, T36.8X5A – Adverse effect of other systemic antifungals, initial encounter. The onychomycosis code (B35.1) would also be listed as the underlying reason for the treatment.
12. Additional Resources
For the most accurate and up-to-date coding information, always consult these primary sources:
-
The Official ICD-10-CM Guidelines: Published annually by the Centers for Medicare & Medicaid Services (CMS) and the National Center for Health Statistics (NCHS).
-
The ICD-10-CM Code Set: Available directly from the CMS website or through commercial coding books and software.
-
American Academy of Dermatology (AAD): Provides clinical guidelines and resources on the diagnosis and management of onychomycosis.
-
American Podiatric Medical Association (APMA): Offers patient and professional resources focused on foot and nail health.
-
American Health Information Management Association (AHIMA): The premier association for medical coding professionals, offering education, certifications, and updates on coding standards.
Date: October 19, 2025
Author: The Medical Coding Specialist Team
Disclaimer: The information contained in this article is for educational and informational purposes only and is not intended as medical or coding advice. Always consult with a qualified healthcare provider for any health concerns and with a certified medical coder or the latest official coding resources for accurate billing and reimbursement.






