Navigating the world of medical coding can feel like deciphering an ancient language. For healthcare professionals, medical coders, billers, and even curious patients, understanding these codes is crucial for accurate documentation, proper billing, and clear communication. Among the thousands of codes, ICD-9-CM code J40 holds a specific and important place, especially when discussing respiratory conditions.
If you’ve found yourself searching for the “ICD 9 code for j40,” you’re likely looking for clarity on what this code represents, how it was used, and what replaced it. This guide is designed to be your definitive resource. We’ll break down everything you need to know about ICD-9 J40, providing not just a definition, but the essential context for its application and its role in the evolution of medical classification systems.
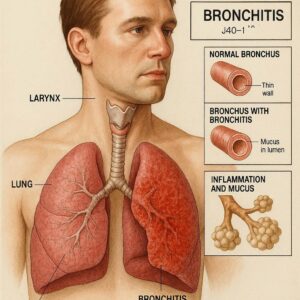
ICD-9-CM Code J40
What is ICD-9-CM Code J40?
Let’s start with the basics. In the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM), J40 is the diagnostic code for “Bronchitis, not specified as acute or chronic.”
Breaking Down the Code’s Meaning
The ICD-9-CM system is organized numerically and alphanumerically. The “J” series covers Diseases of the Respiratory System, specifically codes 460-519. Within that block, J40 falls under the category of “Other diseases of upper respiratory tract” (codes 470-478) and more precisely within “Bronchitis and bronchiolitis” (codes 466, 490-491). However, J40 itself is a standalone code for a very particular scenario.
Here’s what the official descriptor tells us:
-
Bronchitis: This indicates an inflammation of the bronchial tubes, the airways that carry air to your lungs.
-
Not specified as acute or chronic: This is the critical part. It means the diagnosing physician documented “bronchitis” in the patient’s record but did not specify whether it was:
-
Acute Bronchitis: A short-term inflammation often caused by a viral infection, like a cold or flu. Its ICD-9 code was 466.0.
-
Chronic Bronchitis: A long-term, serious condition characterized by a persistent, mucus-producing cough, most commonly associated with smoking or long-term exposure to irritants. Its primary ICD-9 code was 491.xx (with additional digits for specifics).
-
In essence, J40 was a default or unspecified code. It was used when the documentation lacked the clinical detail necessary to assign a more precise code. This often occurred in situations like brief clinic visits, emergency department encounters where the focus was on immediate treatment, or in administrative data sets where detailed clinical information was unavailable.
Why This Specificity Matters
The distinction between acute, chronic, and unspecified bronchitis isn’t just academic. It has real-world implications:
-
Treatment Pathways: Acute bronchitis is typically managed with rest and symptom relief, while chronic bronchitis requires long-term management, pulmonary rehab, and possibly treatment for COPD.
-
Reimbursement: Insurance payers reimburse differently based on diagnosis complexity. An unspecified code like J40 might be reimbursed at a lower rate than a more specific code for chronic bronchitis with complications.
-
Statistical Tracking: Public health agencies track the prevalence of acute versus chronic respiratory conditions to allocate resources. Unspecified codes provide less valuable data for these initiatives.
Clinical Context: When Was ICD-9 J40 Used?
Understanding J40 requires putting yourself in the shoes of a coder or clinician before October 2015. The application of this code followed strict guidelines based on physician documentation.
Typical Clinical Scenarios for J40
-
The Ambiguous Clinic Note: A patient presents with a cough lasting 10 days. The physician examines them, rules out pneumonia, and diagnoses “bronchitis.” The note does not describe the duration in a way that clearly meets the criteria for chronic bronchitis (symptoms most days for at least three months in two consecutive years), nor does it explicitly label it “acute.” J40 would be assigned.
-
Follow-Up or Administrative Visits: A patient is seen for a follow-up on a condition, and bronchitis is listed as a secondary or historical diagnosis without specification from the current encounter.
-
Emergency Department Coding: In a fast-paced ER setting, a provider may document “bronchitis” as the final diagnosis after treating a coughing patient, focusing more on the treatment (e.g., bronchodilator) than the detailed classification.
The Golden Rule of Medical Coding: Documentation is Key
A universal principle in medical coding is: “If it’s not documented, it didn’t happen.” Coders could not assume a bronchitis was acute or chronic based on treatment or medication alone. They were bound by the words in the medical record. If the provider only wrote “bronchitis,” the coder’s only compliant option was J40, even if the coder suspected it was acute.
Important Note for Readers: This reliance on documentation often led to what is called “code creep” or “upcoding,” where providers might be encouraged to add more specific terms to justify higher-complexity codes. The use of unspecified codes like J40 was sometimes audited to ensure documentation supported the billed services.
The Transition from ICD-9-CM to ICD-10-CM
The most critical thing to know about ICD-9 code J40 is that it is obsolete for use in the United States. As of October 1, 2015, the U.S. healthcare system officially transitioned from ICD-9-CM to ICD-10-CM (Clinical Modification) for diagnosis coding. This was a monumental shift that greatly expanded the number and specificity of codes.
Why the Transition Happened
ICD-9, developed in the 1970s, ran out of space for new diseases and procedures. Its structure was limiting and lacked the clinical detail required for modern medicine, value-based care, and precise epidemiological research. ICD-10-CM was adopted to:
-
Improve the accuracy of disease tracking and public health statistics.
-
Support better payment systems for new technologies and treatments.
-
Provide more detailed data for quality measurement and outcomes research.
-
Align the U.S. with much of the rest of the world, which was already using ICD-10.
What Replaced ICD-9 Code J40?
In ICD-10-CM, the concept of an unspecified bronchitis code still exists, but it is organized differently. The respiratory disease chapter in ICD-10-CM begins with the letter J.
The direct equivalent to ICD-9’s J40 is:
-
ICD-10-CM Code: J40.0
-
Description: Bronchitis, not specified as acute or chronic.
Yes, it looks similar! However, in ICD-10-CM, J40 is a category code that requires a fourth digit. J40.0 is the only option under that category, making it the precise replacement.
The ICD-10-CM Bronchitis Coding Structure
ICD-10-CM offers a much richer and more specific set of options for bronchitis. Here’s a comparison to illustrate the increased granularity:
Bronchitis Codes – ICD-9 vs. ICD-10 Comparison
| Condition | ICD-9-CM Code | ICD-10-CM Code | ICD-10-CM Code Description |
|---|---|---|---|
| Unspecified Bronchitis | J40 | J40.0 | Bronchitis, not specified as acute or chronic |
| Acute Bronchitis | 466.0 | J20.9 | Acute bronchitis, unspecified |
| J20.0 – J20.8 | Acute bronchitis due to various specified organisms (e.g., J20.5 for acute bronchitis due to RSV) | ||
| Simple Chronic Bronchitis | 491.0 | J41.0 | Simple chronic bronchitis |
| Mucopurulent Chronic Bronchitis | 491.1 | J41.1 | Mucopurulent chronic bronchitis |
| Mixed Simple & Mucopurulent | 491.2 | J41.8 | Mixed simple and mucopurulent chronic bronchitis |
| Unspecified Chronic Bronchitis | 491.9 | J42 | Unspecified chronic bronchitis |
As you can see, ICD-10-CM provides distinct codes for different types of chronic bronchitis and allows for the specification of the infectious agent in acute cases. This level of detail was simply not possible in the ICD-9 framework.
Practical Implications: Coding, Billing, and Compliance
For Medical Coders and Billers
If you are handling medical records from before October 1, 2015, you would use ICD-9-CM codes. For a diagnosis of unspecified bronchitis in an old record, you would assign J40.
For all records from on or after October 1, 2015, you must use ICD-10-CM. For the same clinical scenario (unspecified bronchitis), you would assign J40.0.
A Critical Compliance Point: Using an outdated ICD-9 code like J40 on a current claim form (CMS-1500 or UB-04) will result in an immediate rejection from any Medicare, Medicaid, or commercial payer. The systems are programmed to accept only ICD-10-CM codes for dates of service after the transition deadline.
For Healthcare Providers and Clinicians
The transition to ICD-10-CM underscored the importance of specific documentation. To ensure accurate coding and optimal patient care, providers should be precise in their notes. Instead of just “bronchitis,” documenting:
-
“Acute bronchitis” (leads to J20.9)
-
“Acute bronchitis, likely viral” (still J20.9, but better clinical detail)
-
“Chronic bronchitis, patient with 40-pack-year history” (leads to J41.0, J41.1, or J42, and also prompts coding for tobacco use)
This specificity leads to better coding, fewer claim denials, and richer patient data.
A Helpful List: Documentation Tips to Avoid Unspecified Codes
To move away from codes like J40.0, clinicians can:
-
Specify Acuity: Use “acute,” “chronic,” or “acute on chronic.”
-
Describe Symptoms: Note cough characteristics (productive/dry, color of sputum).
-
State Duration: “Cough for 2 weeks” suggests acute; “cough for 4 months” suggests chronic.
-
Identify Etiology: When known, note “viral,” “bacterial,” or “due to irritant exposure.”
-
Link to History: “Bronchitis in patient with established COPD.”
Why Understanding Historical Codes Still Matters
You might wonder, if ICD-9 is obsolete, why spend time learning about J40? The reasons are practical and enduring:
-
Retrospective Research & Data Analysis: Epidemiological studies, longitudinal health outcomes research, and historical comparisons often require working with data coded in ICD-9. Understanding what J40 represented is essential for accurately interpreting that old data.
-
Legal and Disability Cases: Medical records from past injuries or illnesses coded in ICD-9 may be relevant in legal proceedings or long-term disability claims. Understanding the codes is part of understanding the medical history.
-
Educational Foundation: Learning ICD-9 concepts provides the foundational knowledge that makes the complexity of ICD-10 easier to grasp. It’s the history of the language of medicine.
Quotation from a Healthcare Data Analyst: *“In my work linking decades of patient data, codes like ICD-9’s J40 are time capsules. We can’t simply map them one-to-one to ICD-10; we have to understand the clinical context and documentation habits of that era to create accurate trends. Knowing J40 was a ‘default’ code helps us filter and interpret historical bronchitis prevalence rates with the right caveats.”*
Frequently Asked Questions (FAQ)
Q: Can I still use ICD-9 code J40 today?
A: No. For any healthcare service provided in the U.S. on or after October 1, 2015, you must use ICD-10-CM codes. Using J40 on a current claim will cause it to be rejected. The replacement code is ICD-10-CM J40.0.
Q: What is the difference between J40 and J40.0?
A: Conceptually, they represent the same clinical idea: bronchitis not specified as acute or chronic. The difference is systemic: J40 is the complete code in the ICD-9-CM system. J40.0 is the complete code in the ICD-10-CM system, where the “.0” is a required fourth digit for specificity.
Q: My medical bill from 2014 has code J40 on it. Is that wrong?
A: No, that is correct. For services rendered before October 1, 2015, the use of ICD-9-CM codes, including J40, was standard and required.
Q: Why would a coder use an unspecified code like J40 or J40.0? Isn’t more specific always better?
A: While specificity is always the goal, coders are constrained by the provider’s documentation. If the medical record only supports a diagnosis of “bronchitis” without further detail, the coder is ethically and legally obligated to assign the unspecified code. Using a more specific code without supporting documentation is considered fraud.
Q: Are there other ICD-9 codes similar to J40?
A: Yes. ICD-9-CM was filled with unspecified codes. Another common example in the respiratory chapter was 496 for “Chronic airway obstruction, not elsewhere classified,” which was often used as a default for COPD when the type wasn’t specified. These have all been replaced by more detailed ICD-10-CM options.
Conclusion
ICD-9-CM code J40, representing “Bronchitis, not specified as acute or chronic,” serves as a perfect case study in the evolution of medical coding. It highlights the critical link between clinical documentation and administrative data, the financial and statistical impacts of coding specificity, and the ongoing drive in healthcare toward greater precision. While now a historical code, understanding J40 provides invaluable insight into the foundations of modern diagnostic classification and underscores the permanent importance of clear, detailed patient records in the digital age.
Additional Resource Link:
For the official ICD-10-CM code set and guidelines, always refer to the Centers for Medicare & Medicaid Services (CMS) and the National Center for Health Statistics (NCHS) websites. A reliable public tool for browsing current codes is the CDC’s ICD-10-CM Browser: https://www.cdc.gov/nchs/icd/icd10cm.htm
Disclaimer: This article is for informational and educational purposes only. It is not intended as medical coding, billing, or legal advice. Official coding guidance and code assignment should always be based on the most current official code sets, payer policies, and clinical documentation for the individual patient encounter. Consult with a certified professional coder or relevant official resources for specific cases.






