If you’re navigating medical records, insurance forms, or historical data, you might be searching for a specific diagnostic code: the ICD-9 code for blepharitis. While the ICD-9 system is a legacy coding set, understanding its codes remains crucial for interpreting older documents. This comprehensive guide will not only provide that code but will also bridge the gap to the current medical coding system, offering a deep dive into blepharitis itself—its symptoms, causes, and the most effective treatments available today. Our goal is to transform a simple code lookup into an empowering resource for lasting eye health.
For healthcare professionals, medical coders, and curious patients alike, this article serves as a definitive reference. We’ll move beyond the basics to explore why accurate coding matters, how it impacts patient care, and what you need to know in the modern healthcare landscape. Let’s begin by answering the core question directly.
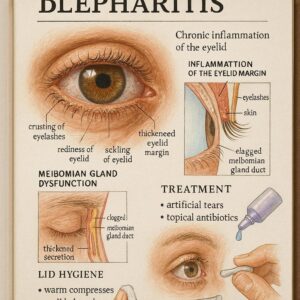
ICD-9 Code for Blepharitis
What Was the ICD-9 Code for Blepharitis?
In the International Classification of Diseases, Ninth Revision (ICD-9), which was used in the United States until October 1, 2015, blepharitis had a specific numerical designation.
The ICD-9 code for blepharitis was 373.00.
This code falls under a broader category within the ICD-9 system:
-
Chapter 7: Diseases of the Eye and Adnexa (360-379)
-
Block 373: Inflammation of the eyelid
It’s important to understand the specificity, or lack thereof, in this code. ICD-9-CM code 373.00 was defined as “Blepharitis, unspecified.” This means it was a general code used for all forms of blepharitis when a more specific type (e.g., ulcerative, squamous) was not documented. The ICD-9 system had limited codes for further specification, which was one of the driving factors for the transition to the more detailed ICD-10.
Why Knowing This Historical Code Still Matters
You might wonder why a code from a retired system is relevant. Here are key reasons:
-
Medical Record Review: Patients and new doctors often review decades of medical history. Encountering an ICD-9 code requires understanding its meaning.
-
Research and Data Analysis: Longitudinal studies spanning years before 2015 rely on ICD-9 data. Accurate interpretation is vital for public health insights.
-
Insurance and Legal Cases: Resolving older insurance claims or understanding historical diagnoses in legal contexts often involves ICD-9 codes.
However, for all current medical, billing, and diagnostic purposes, the ICD-9 system is obsolete. The healthcare world now operates on ICD-10-CM, a system with exponentially greater detail.
The Modern Equivalent: ICD-10-CM Codes for Blepharitis
The transition to ICD-10-CM marked a significant shift from approximately 14,000 codes to over 70,000. For blepharitis, this meant moving from one general code to multiple, highly specific codes. This specificity allows for better tracking of disease types, treatment outcomes, and epidemiological trends.
The foundational ICD-10-CM code for blepharitis is H01.0. But unlike ICD-9, this is just the starting point. The system requires additional digits to specify the type, laterality (which eye), and in some cases, the cause.
Detailed Breakdown of ICD-10-CM Codes for Blepharitis
Here is a comparative table showing how the simple ICD-9 code translates into the granular world of ICD-10.
| Condition | ICD-9 Code (Historical) | ICD-10-CM Code (Current) | Description & Specificity |
|---|---|---|---|
| Unspecified Blepharitis | 373.00 | H01.00 | Unspecified blepharitis, unspecified eyelid |
| H01.001 | Unspecified blepharitis, right upper eyelid | ||
| H01.002 | Unspecified blepharitis, right lower eyelid | ||
| H01.003 | Unspecified blepharitis, right eye, unspecified eyelid | ||
| Squamous Blepharitis | 373.1 (Ulcerative) | H01.11- | Squamous blepharitis of right/left eye, upper/lower lid |
| Ulcerative Blepharitis | 373.1 | H01.12- | Ulcerative blepharitis of right/left eye, upper/lower lid |
| Blepharitis due to Demodicosis | N/A (No specific code) | H01.13- | Blepharitis due to Demodex species mites |
| Other Specified Inflammation | 373.3 (Abscess) | H01.14- | Other specified inflammation of eyelid (e.g., abscess) |
Important Note for Readers: The hyphen (-) in the ICD-10 codes indicates that additional digits are required to complete the code, specifying laterality (right, left, bilateral) and exact eyelid location. This level of detail is mandatory for accurate clinical documentation and billing.
Why This Coding Specificity is a Game-Changer
The detail in ICD-10-CM is not bureaucratic red tape; it directly benefits patient care.
-
Improved Treatment Plans: Knowing a case is ulcerative (H01.12-) versus squamous (H01.11-) or Demodex-related (H01.13-) guides a doctor’s choice of medication and therapy.
-
Enhanced Research: Public health officials can now track the prevalence of specific blepharitis subtypes, leading to better understanding and resource allocation.
-
Accurate Reimbursement: Specific codes ensure healthcare providers are reimbursed appropriately for the complexity of care provided.
Understanding Blepharitis: More Than Just a Code
Now that we’ve firmly established the coding landscape—both historical and current—let’s focus on the condition itself. Blepharitis is a common and often chronic inflammation of the eyelids, primarily affecting the area where eyelashes grow. It’s a leading cause of ocular discomfort and dry eye symptoms.
Types and Causes of Blepharitis
Blepharitis is typically categorized by its location and cause:
-
Anterior Blepharitis: Affects the outside front of the eyelid, where eyelashes attach.
-
Staphylococcal: Caused by bacteria (Staphylococcus).
-
Seborrheic: Associated with dandruff of the scalp and eyebrows (seborrheic dermatitis).
-
-
Posterior Blepharitis: Affects the inner eyelid, the moist part that touches the eye. This involves the meibomian glands.
-
Meibomian Gland Dysfunction (MGD): The glands become blocked or produce poor-quality oil, a key component of tears.
-
-
Mixed Blepharitis: A combination of anterior and posterior forms, which is very common.
Common Contributing Factors:
-
Demodex mites (microscopic organisms that live in hair follicles)
-
Rosacea (a skin condition causing facial redness)
-
Allergies
-
Dry eyes
-
Certain medications
Recognizing the Symptoms
Blepharitis symptoms can be persistent and frustrating. Patients often report:
-
Red, swollen eyelids
-
A gritty, burning, or stinging sensation in the eyes
-
Crusty debris or “collarettes” at the base of eyelashes (especially upon waking)
-
Watery eyes
-
Itchy eyelids
-
Sensitivity to light
-
Blurred vision that improves with blinking
-
Loss of eyelashes (in severe cases)
A key insight from ophthalmologists: “Blepharitis is often a chronic condition, much like dandruff of the scalp. The goal of treatment is not a one-time cure but effective long-term management to control symptoms and prevent flare-ups.”
A Step-by-Step Guide to Diagnosis and Modern Treatment
How Eye Care Professionals Diagnose Blepharitis
Diagnosis typically involves a comprehensive eye exam, which may include:
-
Patient History: Discussing symptoms, duration, and aggravating factors.
-
Slit-Lamp Examination: Using a special microscope to magnify and illuminate the eyelids, lashes, and tear film.
-
Meibomian Gland Evaluation: Applying gentle pressure to the lids to assess gland function and secretion quality.
-
Tear Film Assessment: Checking tear quantity and quality.
Note: The specific findings from this exam directly inform which precise ICD-10-CM code is assigned. For example, the observation of cylindrical dandruff (sleeves) around lashes might point toward Demodex, leading to code H01.13-.
Effective Treatment Protocols: The Daily Eyelid Hygiene Routine
Management is centered on a consistent daily eyelid hygiene routine. Here is a helpful, actionable list for patients:
-
Apply Warm Compresses: Use a clean, warm washcloth or a commercially available eye mask for 5-10 minutes. This melts hardened oils in the meibomian glands.
-
Lid Massage: Gently massage the eyelids with your eyes closed, moving your finger downward on the upper lid and upward on the lower lid to express the glands.
-
Lid Scrubs: Use a prescribed eyelid cleanser or a dilute solution of baby shampoo on a clean cotton pad or gauze. Gently scrub the base of the lashes to remove crusts and debris.
-
Artificial Tears: Use preservative-free artificial tears to lubricate the eyes and relieve dryness.
-
Medications: In some cases, doctors may prescribe:
-
Topical Antibiotics: Ointments (e.g., erythromycin) applied to the lid margin.
-
Topical or Oral Anti-inflammatories: Steroid eye drops for short-term flare-ups or oral doxycycline/azithromycin for their anti-inflammatory and lipid-modifying properties.
-
Tea Tree Oil Products: For suspected Demodex infestations.
-
Advanced In-Office Treatments
For stubborn cases, several in-office procedures have shown great promise:
-
LipiFlow®: A device that applies heat and gentle pressure to the eyelids to clear meibomian gland blockages.
-
Intense Pulsed Light (IPL) Therapy: Pulses of light applied to the skin around the eyes can reduce inflammation and improve gland function.
-
BlephEx®: A professional micro-blepharoexfoliation procedure to thoroughly clean the lid margin and remove biofilm.
The Critical Link Between Accurate Coding and Patient Care
This journey from the simple ICD-9 code 373.00 to the detailed H01.0- series in ICD-10-CM mirrors the evolution in our understanding of blepharitis. Accurate coding is not just an administrative task; it is a fundamental part of the clinical process.
-
It Starts with Documentation: The eye care provider must carefully document the type, laterality, and any causative factors of the blepharitis.
-
Translation to Code: This documentation is translated into the most specific ICD-10-CM code by a trained coder or the provider.
-
Informing the Care Pathway: This specific code becomes part of the patient’s permanent health record, signaling to any future provider the exact nature of the condition.
-
Supporting Medical Necessity: The code justifies the treatments prescribed, whether it’s a specific medication, a procedure like LipiFlow, or ongoing management visits.
A mismatch between the documented condition and the code used can lead to denied insurance claims, fragmented care, and muddy clinical data. Precision in coding ensures clarity and continuity in the patient’s healthcare journey.
Conclusion
The search for the ICD-9 code for blepharitis (373.00) opens a window into the critical importance of medical coding as the language of healthcare. While this historical code provides a basic label, its modern ICD-10-CM successors (the H01.0- series) offer the specificity needed for personalized, effective treatment of this chronic eye condition. By understanding both the codes and the comprehensive reality of blepharitis—its causes, symptoms, and the essential daily management routine—patients and professionals alike can work towards better ocular health and clearer vision.
Frequently Asked Questions (FAQ)
Q: Can I still use the ICD-9 code for blepharitis on medical forms today?
A: No. As of October 1, 2015, all HIPAA-covered entities (healthcare providers, insurers, etc.) in the United States are required to use ICD-10-CM codes for diagnosis reporting. Using ICD-9 will result in claim denials.
Q: My old medical record says “373.00.” What should I tell my new eye doctor?
A: Simply inform them that you were previously diagnosed with blepharitis. They will conduct a new examination and assign the appropriate, current ICD-10-CM code based on their findings. The old code gives them historical context.
Q: Is blepharitis a serious condition?
A: While it is rarely a threat to sight, it is a chronic and often uncomfortable condition that can significantly impact quality of life. If left unmanaged, it can lead to complications like styes, chalazia, chronic conjunctivitis, corneal inflammation, and worsened dry eye.
Q: Are over-the-counter eyelid wipes effective?
A: Yes, for many people, pre-moistened, sterile eyelid cleansing wipes can be a very convenient and effective part of the daily hygiene routine. Look for ones designed specifically for ophthalmologic use.
Q: If blepharitis is chronic, will I need treatment forever?
A: Management is typically long-term. Think of it like skincare for your eyelids. Even when symptoms improve, most patients need to maintain a basic, reduced-frequency hygiene routine (e.g., 2-3 times per week) to prevent flare-ups.
Additional Resources
For further reading on eye health and blepharitis management from authoritative sources, consider visiting the American Academy of Ophthalmology’s EyeSmart® website at https://www.aao.org/eye-health. They provide patient-friendly, medically reviewed information on a wide range of eye conditions.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. The medical coding information is based on U.S. standards. Always consult with a qualified healthcare professional for diagnosis and treatment of any medical condition, including blepharitis. Coding standards and guidelines are subject to change.
Date: January 09, 2026
Author: The Web Health Writer Team






