If you’re dealing with medical records, insurance claims, or a personal injury case related to a back injury, you’ve likely encountered the term “ICD-9 code.” Even though this coding system is now historical, its records are still vital for understanding past injuries, ongoing disability cases, and historical medical data. This guide will demystify the ICD-9 coding system for back injuries, providing you with a clear, actionable, and comprehensive resource. We’ll explore the structure of the codes, list the most common ones you’ll encounter, and explain why accurate coding remains crucial.
Let’s start with the basics. ICD-9 stands for the International Classification of Diseases, 9th Revision. It was the standard system used by healthcare providers and insurers in the United States to classify and code all diagnoses, symptoms, and procedures until October 1, 2015. On that date, the U.S. officially transitioned to ICD-10, a much more detailed system. However, understanding ICD-9 codes is still critically important. Why? If your back injury occurred or was treated before 2015, your medical records, insurance settlements, or ongoing workers’ compensation or disability claims are likely documented using ICD-9 codes. For historical research, legal cases involving past injuries, or simply understanding your own old medical bills, this knowledge is indispensable.
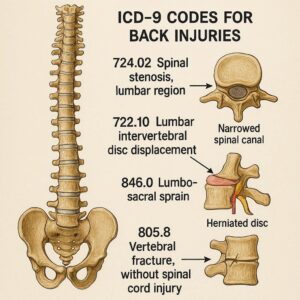
ICD-9 Codes for Back Injury
The Structure of ICD-9 Codes for Musculoskeletal Conditions
ICD-9 codes are alphanumeric, typically 3 to 5 digits long. The first three digits represent the core category of the disease or injury. A decimal point follows the third digit, and then one or two additional digits provide greater specificity regarding the location, type, and laterality (left or right) of the condition.
For back injuries and most musculoskeletal problems, we look within Chapter 13: “Diseases of the Musculoskeletal System and Connective Tissue” (codes 710-739). The specific series for most back injuries and disorders is 720-724.
-
720: Inflammatory spondylopathies (e.g., ankylosing spondylitis)
-
721: Spondylosis and allied disorders (degenerative conditions)
-
722: Intervertebral disc disorders (e.g., herniated discs)
-
723: Other disorders of the cervical region (e.g., cervicalgia, cervicobrachial syndrome)
-
724: Other disorders of the back (a broad category covering lumbago, spinal stenosis, and other unspecified back issues)
It’s crucial to distinguish between an injury (like a fracture or sprain from a specific event) and a disorder (like a degenerative disc disease). True acute “injuries” from trauma are often found in Chapter 17: “Injury and Poisoning” (codes 800-999). For example, a vertebral fracture code would start with 805 or 806, and a sprain/strain of the lumbar spine would be 847.2.
Why Specificity Matters in Coding
The fourth and fifth digits of an ICD-9 code transform a general category into a precise diagnosis. This specificity directly impacts medical care, insurance reimbursement, and legal outcomes. A vague code can lead to claim denials or an incomplete medical narrative.
“In medical coding, specificity is not just a preference—it’s a prerequisite for accurate patient history, appropriate treatment pathways, and fair insurance adjudication.” – Industry Standard Practice
For instance, the code 724.2 means “Lumbago” (low back pain). While this might be used, a more specific code from the 722 or 847 series that identifies a cause (like a herniated disc or a strain) is always preferred if the diagnostic information is available.
Common ICD-9 Codes for Back Injuries and Disorders
Below is a detailed table of the most frequently used ICD-9 codes related to back problems. This will serve as your primary reference.
Primary ICD-9 Code Categories for Back Conditions
| ICD-9 Code | Code Description | Category | Typical Use Case |
|---|---|---|---|
| 722.10 | Displacement of lumbar intervertebral disc without myelopathy | Disc Disorder | A herniated, bulging, or ruptured disc in the low back without spinal cord involvement. |
| 722.52 | Degeneration of lumbar or lumbosacral intervertebral disc | Disc Disorder | Wear-and-tear or degenerative disc disease (DDD) in the low back. |
| 724.2 | Lumbago | Other Back Disorder | General low back pain, often used when a more specific cause isn’t documented. |
| 847.2 | Sprain and strain of lumbar spine | Injury (Sprain/Strain) | An acute injury to the ligaments (sprain) or muscles/tendons (strain) of the low back. |
| 724.02 | Spinal stenosis of lumbar region | Other Back Disorder | Narrowing of the spinal canal in the low back, pressing on nerves. |
| 723.1 | Cervicalgia | Other Back Disorder | Pain in the neck (cervical spine). |
| 722.0 | Displacement of cervical intervertebral disc without myelopathy | Disc Disorder | A herniated disc in the neck. |
| 847.0 | Sprain and strain of neck | Injury (Sprain/Strain) | Whiplash or other acute neck muscle/ligament injury. |
| 805.4 | Fracture of lumbar vertebra without mention of spinal cord injury | Injury (Fracture) | A broken bone in the low back vertebrae. |
| 806.4 | Fracture of lumbar vertebra with spinal cord injury | Injury (Fracture) | A more severe lumbar fracture that involves damage to the spinal cord. |
| 724.4 | Thoracic or lumbosacral neuritis or radiculitis, unspecified | Other Back Disorder | Inflammation of a nerve root, often causing sciatica-like pain. |
| 737.30 | Scoliosis (and kyphoscoliosis), idiopathic | Curvature | A sideways curvature of the spine. |
Detailed Breakdown of Key Codes
Let’s dive deeper into some of the most significant codes you’ll encounter.
1. Lumbar Disc Herniation (722.10)
This is arguably one of the most common specific diagnoses for severe back pain. The code 722.10 sits within the larger family of 722 codes. The fifth digit specifies the spinal region:
-
722.10: Lumbar region
-
722.11: Cervical region
-
722.12: Thoracic region
The term “without myelopathy” is key—it means the disc problem is causing nerve root irritation (radiculopathy, which can lead to sciatica) but is not compressing the actual spinal cord itself.
2. Lumbar Sprain/Strain (847.2)
This code belongs to the Injury chapter (847: “Sprain and strain of other and unspecified parts of back”). It’s the go-to code for acute soft tissue injuries of the low back, such as those from lifting a heavy object, a fall, or a car accident. Proper documentation should link this code to an external cause of injury (an E-code), which we will discuss later.
3. Lumbago (724.2) and the Importance of Specificity
724.2 is a “catch-all” code for lower back pain. While commonly used, it is considered unspecified. From a medical and legal standpoint, relying solely on this code can be problematic. It doesn’t communicate the etiology (cause) of the pain. Was it from an injury? Is it degenerative? A provider should always strive to use a more precise code if the clinical picture supports it. For patients, seeing only this code on a bill might indicate that your provider’s documentation needs to be more detailed.
The Critical Role of E-Codes: Documenting the Cause of Injury
For true injury codes (like 847.2 or 805.4), ICD-9 required the use of Supplementary Classification of External Causes of Injury and Poisoning (E-codes). These codes describe how the injury happened. They are essential for public health tracking and are absolutely critical in workers’ compensation and personal injury litigation.
-
Example: A worker lifts a heavy box at work and feels a tear in his low back.
-
Diagnosis Code: 847.2 (Sprain and strain of lumbar spine)
-
E-Code: E849.0 (Place of occurrence: Industrial place and premises) AND likely E927 (Overexertion and strenuous movements)
-
Common E-Codes for Back Injuries
| E-Code | Description | Typical Scenario |
|---|---|---|
| E849.0 | Industrial place and premises | Injury occurring at a factory, construction site, or office workplace. |
| E849.3 | School, other institution, and public administrative area | Injury at a school or government building. |
| E849.5 | Sports and athletic area | Injury during a football game, gym workout, etc. |
| E819.9 | Motor vehicle traffic accident, unspecified | Back injury from a car crash (more specific E-codes exist for driver, passenger, etc.). |
| E885.9 | Fall on same level from slipping, tripping, or stumbling | A slip-and-fall accident. |
| E927 | Overexertion and strenuous movements | Lifting, pulling, or pushing a heavy object. |
Important Note for Readers: If you are reviewing records for a back injury claim, always check for the presence of both a diagnosis code (from the 800-847 series or 720-724 series) and a corresponding E-code. The absence of an E-code for an acute injury is a significant documentation gap.
Transition from ICD-9 to ICD-10: What Changed?
The transition to ICD-10-CM on October 1, 2015, was a monumental shift. ICD-10 codes are longer (3-7 characters), more detailed, and allow for greater specificity regarding laterality (left/right), episode of care (initial encounter, subsequent encounter, sequela), and precise anatomical location.
Comparative Example: Lumbar Disc Herniation
-
ICD-9: 722.10 – “Displacement of lumbar intervertebral disc without myelopathy.” This one code covers all lumbar disc displacements.
-
ICD-10: M51.26 – “Other intervertebral disc displacement, lumbar region.” But it gets more specific. ICD-10 requires a 7th character:
-
M51.262 – … lumbar region, left side.
-
M51.263 – … lumbar region, right side.
-
M51.269 – … lumbar region, unspecified side.
-
Furthermore, ICD-10 has distinct codes for disc disorders with radiculopathy (nerve pain) versus without. This level of detail provides a much clearer clinical picture.
Practical Implications: Why These Codes Matter to You
For Patients:
-
Understanding Your Bills and Records: You can now decipher the codes on your Explanation of Benefits (EOB) or medical records from pre-2015. If you see only “724.2,” consider asking your provider if a more specific diagnosis was determined.
-
Navigating Claims: If you have an old injury with an ongoing claim, knowing the correct ICD-9 code helps you ensure your medical records accurately support your case.
For Medical Coders and Billers:
-
Historical Research: You may need to reference ICD-9 for audits, appeals, or processing of old claims that were submitted under the old system.
-
Understanding Progression: Seeing a patient’s history coded in ICD-9 provides context for their current ICD-10 coded conditions.
For Legal and Insurance Professionals:
-
Building or Assessing a Case: The specificity (or lack thereof) in an ICD-9 code can strengthen or weaken a personal injury or workers’ compensation case. A code with a corresponding E-code (e.g., 847.2 + E849.0 + E927) creates a clear narrative of a work-related injury. Vague codes like 724.2 do not.
-
Causation Analysis: Accurate coding is the bedrock of establishing medical causation—linking a specific accident or exposure to a specific diagnosed injury.
Conclusion
Navigating the world of ICD-9 codes for back injury is essential for interpreting historical medical events, whether for personal understanding, insurance purposes, or legal proceedings. While the system has been replaced by ICD-10, its legacy lives on in millions of records. By understanding the structure—particularly the distinction between injury codes (800-847) and disorder codes (720-724), the necessity of specific fifth digits, and the crucial role of E-codes—you empower yourself to accurately interpret the story these codes tell. Always seek the most specific code available, as precision in diagnosis coding leads to clarity in treatment, reimbursement, and legal resolution.
Frequently Asked Questions (FAQ)
Q: My medical bill from 2014 only shows the code 724.2. What does this mean for my injury claim?
A: Code 724.2 (Lumbago) is an unspecified code for low back pain. While it confirms you had back pain, it doesn’t specify a cause (like a herniated disc or a sprain). For a strong injury claim, it’s beneficial to have your medical provider amend the records (if appropriate) to reflect a more specific diagnosis code linked to an injury, preferably with an accompanying E-code describing the accident. Consult with your attorney or insurance adjuster.
Q: Can I still submit a claim using ICD-9 codes today?
A: No. For any healthcare services provided on or after October 1, 2015, the U.S. healthcare system requires the use of ICD-10-CM codes for diagnosis. ICD-9 codes are only relevant for services provided before that date or for historical record analysis.
Q: Where can I find the official, complete list of ICD-9 codes?
A: The U.S. Centers for Medicare & Medicaid Services (CMS) maintains the official code sets. You can find comprehensive files and manuals on the CMS ICD-9-CM website. However, for most practical purposes, reputable medical coding websites and books offer more user-friendly indexes.
Q: What’s the biggest practical difference between ICD-9 and ICD-10 for back injuries?
A: Specificity and Laterality. ICD-10 almost always indicates whether the condition affects the left side, right side, or is unspecified. It also has many more codes to describe the exact type of disorder (e.g., 7 different codes for lumbar disc disorders with radiculopathy depending on the specific vertebra). ICD-9 had one-fifth as many codes for all musculoskeletal conditions.
Additional Resources
-
For Official Code Sets: Visit the Centers for Disease Control and Prevention (CDC) ICD-9-CM Archive: https://www.cdc.gov/nchs/icd/icd9cm.htm (This link is provided as an example of the type of resource. Please verify the current URL as archival sites may change.)
-
For Understanding Medical Coding: The American Academy of Professional Coders (AAPC) offers articles and glossaries that explain coding concepts in clear language.
-
For Patient Advocacy: The Patient Advocate Foundation provides resources for understanding medical bills and insurance claims.
Disclaimer: This article is for informational and educational purposes only. It does not constitute medical, legal, or coding advice. Always consult with a qualified healthcare provider for medical diagnoses and treatments, a certified professional coder for billing questions, and an attorney for legal matters pertaining to injuries and claims.
Date: January 09, 2026
Author: The Editorial Team at HealthCode Reference






