In the vast, intricate language of modern healthcare—a lexicon where clinical outcomes, administrative necessity, and financial viability converge—few systems are as simultaneously precise and perplexing as the International Classification of Diseases, Tenth Revision, Procedure Coding System (ICD-10-PCS). For the uninitiated, a code like 0W993ZZ may appear as an inscrutable string of alphanumeric characters, a random sequence devoid of meaning. Yet, for healthcare professionals, medical coders, auditors, and health informaticists, this code represents a complete, vivid narrative. It tells a story of a specific patient, a precise anatomical site, a definitive medical objective, and a carefully executed intervention. This code is the story of a left thoracentesis.
This article embarks on a deep exploration of this single code. We will journey beyond the surface to understand not just what the code is, but why it exists in its particular form, how it is derived from the patient’s story, and what profound implications it carries for clinical data integrity, reimbursement accuracy, and the very understanding of healthcare epidemiology. Our exploration will be detailed, exceeding a mere overview to delve into the clinical anatomy, the procedural nuances, the coding logic, and the real-world applications that make mastery of such codes essential. Prepare to see the left thoracentesis, and the system that classifies it, in an entirely new light.
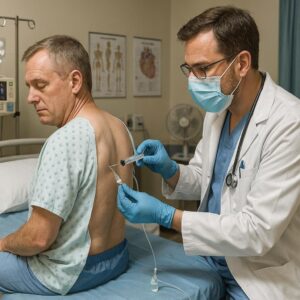
ICD-10-PCS Code for Left Thoracentesis
2. Understanding the Clinical Imperative: What is a Left Thoracentesis?
Before a code can be assigned, the procedure must be understood in its full clinical context. A thoracentesis, also known as a pleural tap, is a fundamental diagnostic and therapeutic procedure in pulmonary and critical care medicine. It involves the percutaneous insertion of a needle or a small catheter through the chest wall into the pleural space—the potential space between the visceral pleura lining the lungs and the parietal pleura lining the inner chest wall.
When this procedure is performed on the left side of the thoracic cavity, it is specifically termed a left thoracentesis.
The “Why”: Indications for the Procedure
The pleural space normally contains a minute amount of lubricating fluid. Pathology arises when this space accumulates excess fluid, a condition known as a pleural effusion. A left thoracentesis is indicated to:
-
Diagnose the Cause: Analysis of pleural fluid (biochemical, cytological, microbiological) is crucial to determine if an effusion is a transudate (e.g., due to heart failure, cirrhosis) or an exudate (e.g., due to infection [empyema], malignancy [lung cancer, mesothelioma], or autoimmune disease).
-
Relieve Symptoms (Therapeutic): Large effusions can cause significant dyspnea (shortness of breath), hypoxia, and chest discomfort. Removing fluid (often 500-1500ml in a therapeutic tap) can provide immediate symptomatic relief.
-
Instill Medication: In cases of malignant effusions or empyemas, medications like talc (for pleurodesis) or antibiotics can be instilled via the thoracentesis catheter.
The “How”: Procedural Execution
The procedure is typically performed with local anesthesia and often under ultrasound guidance, which has become the standard of care to increase safety and efficacy. The patient is positioned sitting upright, leaning forward on a bedside table. After sterile preparation and local anesthetic injection, the physician inserts the needle or catheter along the superior border of a rib (to avoid neurovascular bundles) into the left pleural space. Fluid is then withdrawn via syringe or vacuum bottle.
Risks and Considerations: While generally safe, potential complications include pneumothorax (collapsed lung), bleeding, infection, re-expansion pulmonary edema, and, rarely, splenic or liver injury (on the left and right sides, respectively). This underscores the necessity for precision in the procedure’s documentation and coding.
3. The Architecture of ICD-10-PCS: A System of Precision
ICD-10-PCS is not a mere list of codes; it is a multi-axial, hierarchical system built on a foundation of logic. Each of the seven characters in a valid PCS code has a specific meaning, and each character’s value is selected from a predefined table. This structure allows for the creation of a highly specific code for thousands of procedures.
The Seven Characters of ICD-10-PCS:
-
Section: The broadest category (e.g., Medical and Surgical, Obstetrics, Imaging).
-
Body System: The general physiological system involved.
-
Root Operation: The objective of the procedure—the single most important conceptual key to PCS. What is the provider trying to accomplish?
-
Body Part: The specific anatomical site.
-
Approach: The technique used to reach the site (e.g., open, percutaneous, via natural orifice).
-
Device: Whether a device remains after the procedure.
-
Qualifier: Additional information about the procedure (e.g., diagnostic, therapeutic).
This structure is the map we will use to navigate to our specific destination: 0W993ZZ.
4. Deconstructing 0W993ZZ: A Character-by-Character Analysis
Let us now dissect the code for a standard left thoracentesis, where fluid is drained for either diagnostic or therapeutic purposes, and no device remains.
-
0: Section – Medical and Surgical
-
This indicates the procedure involves cutting, separation, or drainage performed for surgical purposes. Thoracentesis qualifies as a surgical procedure in the PCS context.
-
-
W: Body System – Anatomical Regions, General
-
This is a critical character. The pleural space is not considered part of the respiratory system (body system B) in PCS. Instead, it is classified under “Anatomical Regions, General,” which includes body cavities like the pleural cavity, pericardial cavity, and peritoneal cavity.
-
-
9: Root Operation – Drainage
-
This is the core of the code. The PCS definition of Drainage is: “Taking or letting out fluids and/or gases from a body part.” The key phrase is “letting out.” The objective of a thoracentesis is to let out (remove) fluid from the pleural space. It is vital to distinguish this from Extraction (pulling out a foreign body) or Extirpation (taking out solid matter).
-
-
9: Body Part – Pleural Cavity, Left
-
This character pinpoints the exact location. “9” in the “Anatomical Regions, General” table, under the root operation “Drainage,” corresponds specifically to the Left Pleural Cavity. A separate character exists for the Right Pleural Cavity.
-
-
3: Approach – Percutaneous
-
The approach describes how the body part is reached. Percutaneous is defined as “entry by puncture or minor incision of the skin through the skin or mucous membrane and any other body layers necessary to reach the site of the procedure.” A thoracentesis needle or catheter puncture perfectly fits this definition.
-
-
Z: Device – No Device
-
In a standard thoracentesis, after the fluid is removed, the needle or catheter is withdrawn. No device (like a drainage catheter or pacemaker) is left in place. Therefore, the value is Z (None).
-
-
Z: Qualifier – No Qualifier
-
For this specific combination (Drainage of the Pleural Cavity), there is no additional qualifier needed to further specify the procedure. Hence, Z is used.
-
ICD-10-PCS Code Breakdown for 0W993ZZ
| Character Position | Character Value | Meaning | Definition in Context |
|---|---|---|---|
| 1 (Section) | 0 | Medical and Surgical | The procedure involves manual intervention for drainage. |
| 2 (Body System) | W | Anatomical Regions, General | The pleural cavity is classified as a general body cavity, not under the respiratory tract. |
| 3 (Root Operation) | 9 | Drainage | The objective is to “let out” fluid or gas from a body part. |
| 4 (Body Part) | 9 | Pleural Cavity, Left | The specific anatomical site of the procedure. |
| 5 (Approach) | 3 | Percutaneous | Entry via needle puncture through the skin and chest wall. |
| 6 (Device) | Z | No Device | No appliance is left in place post-procedure. |
| 7 (Qualifier) | Z | No Qualifier | No further specification is required. |
| Full Code | 0W993ZZ | Drainage of Left Pleural Cavity, Percutaneous Approach, No Device | The complete procedural description. |
5. The Crucial Link: Medical Documentation and Code Assignment
The code is a reflection of the documentation. Ambiguous documentation leads to inaccurate coding, which impacts data quality, reimbursement, and compliance. The coder is entirely dependent on the physician’s operative report or procedure note.
Key Elements Documentation MUST Include:
-
Procedure Performed: Explicitly states “thoracentesis” or “pleural tap.”
-
Laterality: Clearly specifies “left”. Phrases like “on the affected side” are insufficient if the laterality is not otherwise clear from the clinical context.
-
Approach: While often implied, mentioning “percutaneous needle” or “under ultrasound guidance” confirms the approach.
-
Intent/Objective: Mention of “for diagnostic analysis” or “for symptomatic relief” supports the root operation of Drainage.
-
No Device Left In Situ: The note should indicate the catheter/needle was removed, or simply not mention placement of an indwelling catheter.
Example of Strong Documentation:
“After informed consent, the patient was placed in an upright position. The left posterior chest wall was prepped and draped sterilely. Under continuous bedside ultrasound guidance, the left pleural effusion was localized. Local anesthesia was administered. A thoracentesis catheter was introduced percutaneously into the left pleural space using the Seldinger technique. Approximately 1100 mL of amber serous fluid was evacuated for therapeutic relief of dyspnea and sent for laboratory analysis. The catheter was removed, and a sterile dressing was applied. The patient tolerated the procedure well.”
This note clearly supports 0W993ZZ.
6. Clinical Scenarios & Coding Examples: From Chart to Code
Scenario 1: Diagnostic Tap for New Effusion
A 68-year-old male with a history of COPD presents with increased shortness of breath. Chest X-ray reveals a new, moderate-sized left pleural effusion. A left thoracentesis is performed under ultrasound guidance, and 400mL of fluid is sent for cell count, protein, LDH, cytology, and culture.
-
Coding Reasoning: The objective is to obtain fluid for analysis (Drainage). It is percutaneous, left-sided, and no catheter remains.
-
ICD-10-PCS Code: 0W993ZZ
Scenario 2: Therapeutic Tap for Malignant Effusion
A 55-year-old female with metastatic breast cancer presents with severe dyspnea. A large left-sided malignant pleural effusion is confirmed. A left thoracentesis is performed, and 1500mL of bloody fluid is removed for symptomatic relief. The catheter is then removed.
-
Coding Reasoning: The primary objective is to relieve symptoms by removing fluid (Drainage). The approach, body part, and device qualifier are identical to Scenario 1. The intent (therapeutic vs. diagnostic) does not change the root operation.
-
ICD-10-PCS Code: 0W993ZZ
Scenario 3: Thoracentesis with Indwelling Catheter Placement (NOT 0W993ZZ)
The same patient as in Scenario 2, but due to rapidly re-accumulating fluid, the physician inserts a tunneled pleural catheter (e.g., PleurX catheter) for ongoing drainage at home.
-
Coding Reasoning: The objective has shifted. The initial drainage is part of the procedure, but the ultimate objective is the insertion of a device that remains. The root operation becomes Insertion, the device character becomes the specific catheter type, and the qualifier may change.
-
Likely ICD-10-PCS Code: 0W9D3JZ (Insertion of Infusion Device into Left Pleural Cavity, Percutaneous Approach) [Note: Exact device character depends on PCS table definitions for the specific catheter]. This is a fundamentally different code.
7. Billing, Reimbursement, and Compliance: The Financial Ecosystem
The accurate assignment of 0W993ZZ is not an academic exercise; it is a critical business function. This code, paired with appropriate diagnosis codes (like J91.8 Pleural effusion in other conditions) and a CPT® code (e.g., 32554 Thoracentesis, needle or catheter, imaging guidance), forms the claim submitted to insurers.
-
DRG Assignment: In the inpatient setting, ICD-10-PCS procedure codes directly influence the assignment of a Diagnosis-Related Group (DRG). A surgical DRG (like one for a major respiratory procedure) often carries a higher reimbursement weight than a medical DRG. The presence of 0W993ZZ can shift a respiratory failure case with effusion into a surgical DRG.
-
Compliance Risks: Miscoding—such as using a code for the right side (0W983ZZ) when the left was performed, or incorrectly coding a diagnostic drainage as an “Inspection”—creates a false claim. This can lead to audits, recoupments, fines, and legal penalties under regulations like the False Claims Act.
-
Data Integrity: At a macro level, accurate coding of procedures like thoracentesis provides vital public health data. It helps track the prevalence of procedures, outcomes, and complications, informing resource allocation and clinical research.
8. Common Pitfalls and Auditor Red Flags
-
Laterality Errors: Confusing left (9) and right (8) is a common and costly mistake.
-
Incorrect Root Operation: Using “Extraction” (for fluid) or “Inspection” (if only visualizing) instead of “Drainage.”
-
Missing Device: Failing to change the code when a drainage catheter is left in place (e.g., for a few days in empyema management).
-
Body System Error: Incorrectly placing the procedure in the Respiratory System (B) instead of Anatomical Regions, General (W).
-
Linking to Diagnosis: The procedure code must be supported by a medical necessity diagnosis. Coding a thoracentesis without a linked diagnosis code for effusion (e.g., J90, J91.8, R09.1) is a red flag.
9. Beyond the Code: Patient Experience and Procedural Nuances
Understanding the code requires appreciating the patient’s journey. The procedure, while common, can be anxiety-provoking. The sensation of pressure relief after a large-volume tap is often dramatic. The shift to ultrasound guidance has minimized the “blind” nature of the procedure, reducing the pneumothorax rate from ~10% to ~3%. Coders who understand this context are better equipped to ask clarifying questions when documentation is vague, such as “Was ultrasound used?” (confirming percutaneous approach) or “Was the catheter removed at the end?” (confirming no device).
10. Conclusion: The Code as a Story
The ICD-10-PCS code 0W993ZZ is far more than a billing token. It is a meticulously constructed clinical shorthand, a data point in healthcare analytics, and a compliance checkpoint. It encapsulates a complete story: a patient in distress from a left pleural effusion, a clinician performing a percutaneous drainage to alleviate that distress, and a healthcare system documenting and accounting for that care with precision. Mastery of this code, and the system it belongs to, is essential for accurate clinical communication, ethical reimbursement, and the generation of reliable data that drives medical progress forward.
11. Frequently Asked Questions (FAQs)
Q1: Why is the pleural cavity under “Anatomical Regions, General” and not the “Respiratory System” in ICD-10-PCS?
A: PCS uses a strict anatomical hierarchy. The Respiratory System (Body System B) includes the trachea, lungs, and bronchi—the organs of respiration. The pleural cavity is a space surrounding a lung, not part of the lung’s tubular structure itself. It is classified as a general body cavity, similar to the pericardial or peritoneal cavity.
Q2: Does the code change if the thoracentesis is done with ultrasound guidance?
A: No. Ultrasound guidance is a technique used to accomplish the percutaneous approach; it does not change the approach character itself. The approach remains “3” for Percutaneous. This is distinct from CPT® coding, where imaging guidance often has a separate code.
Q3: What is the ICD-10-PCS code for a right thoracentesis?
A: It is 0W983ZZ. The only difference is the fourth character (Body Part): ‘8’ for Pleural Cavity, Right.
Q4: How would I code a thoracentesis that yielded a “dry tap” (no fluid obtained)?
A: You would still code the procedure that was performed. The root operation is still Drainage because the objective was to let out fluid. The fact that no fluid was obtained is an outcome, not a change in the procedure’s intent. The code remains 0W993ZZ (or 0W983ZZ for the right). A diagnosis code for the dry tap outcome might also be assigned.
Q5: When does a thoracentesis become a “chest tube insertion” in terms of coding?
A: This is a critical distinction. A chest tube (tube thoracostomy) is typically larger and placed for longer-term drainage, often of air (pneumothorax) or complex fluid. In PCS, this is often coded as Drainage of the pleural cavity with the Device character specifying a Drainage Device (e.g., character J). The root operation may remain Drainage, but the device changes from “Z” to a specific device value. Always refer to the device table for the specific equipment used.
Date: December 1, 2025
Author: Dr. Anya Sharma, MD, CCS-P
Disclaimer: This article is for informational and educational purposes only. It does not constitute medical or coding advice. Always consult the latest official ICD-10-PCS coding manuals, payer-specific guidelines, and clinical documentation for accurate code assignment.






