In the intricate ecosystem of modern healthcare, few elements are as universally pivotal yet as complex as the act of diagnosis coding. It is the linchpin connecting patient care, population health data, clinical research, and healthcare economics. Nowhere is this complexity and need for precision more apparent than in coding for acute conditions that carry significant morbidity, mortality, and financial cost. Acute pancreatitis stands as a paradigm of such a condition—a sudden, inflammatory process of the pancreas that can range from a self-limiting edematous form to a devastating necrotizing disease with multi-organ failure.
For the medical coder, acute pancreatitis is not a single, straightforward code. It is a diagnostic puzzle where clinical etiology, severity, and associated complications dictate a specific alphanumeric pathway within the ICD-10-CM system. The choice between K85.2, K85.1, K85.3, or another subcategory is not an academic exercise; it is a decision with profound implications. Accurate coding ensures appropriate reimbursement through DRG (Diagnosis-Related Group) assignment, facilitates accurate clinical research and epidemiological tracking (e.g., monitoring trends in alcohol vs. biliary causes), and directly impacts quality metrics and hospital performance profiling.
This article embarks on a comprehensive, in-depth exploration of ICD-10-CM coding for acute pancreatitis. Designed to exceed mere code lookup, it delves into the clinical underpinnings that inform code selection, dissects the official coding guidelines, and illuminates the critical dialogue between provider documentation and coder interpretation. With a target audience spanning medical coders, health information management (HIM) professionals, clinical documentation integrity (CDI) specialists, and healthcare administration, this guide aims to be the definitive resource—a detailed, professional, and practical manual that navigates the nuances of K85 and its related codes, empowering accuracy, compliance, and clarity in one of gastroenterology’s most common and serious admissions.
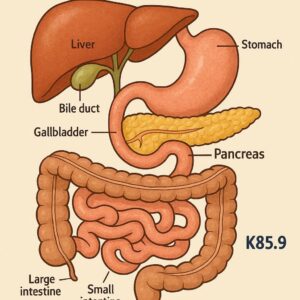
ICD-10-CM Code for Acute Pancreatitis
2. Understanding Acute Pancreatitis: A Clinical Primer for Coders
To code accurately, one must understand the clinical landscape. Acute pancreatitis is an acute inflammatory process of the pancreatic glandular tissue, initiated by the premature activation of pancreatic digestive enzymes within the pancreas itself, leading to autodigestion.
Pathophysiology Simplified: Normally, these enzymes are secreted in an inactive form and become active only in the small intestine. In acute pancreatitis, triggers (like a gallstone blocking the duct or alcohol’s toxic metabolites) cause intracellular activation. These activated enzymes begin to digest pancreatic tissue, causing edema, vascular damage, hemorrhage, and, in severe cases, necrosis (tissue death). This local injury triggers a systemic inflammatory response syndrome (SIRS), which can lead to distant organ failure (lungs, kidneys, cardiovascular system).
Clinical Presentation: Patients typically present with a sudden onset of severe, constant, epigastric (upper abdominal) pain that often radiates to the back. It is frequently accompanied by nausea, vomiting, fever, and tachycardia. On examination, abdominal tenderness is common.
Diagnosis: The diagnosis is established by meeting at least two of the following three criteria (Revised Atlanta Classification):
-
Abdominal pain consistent with the disease.
-
Serum lipase (or amylase) elevation to at least three times the upper limit of normal.
-
Characteristic findings on cross-sectional imaging (contrast-enhanced CT or MRI).
Severity Classification (Crucial for Documentation & Complications):
-
Mild Acute Pancreatitis: No organ failure, no local or systemic complications. Self-limiting.
-
Moderately Severe Acute Pancreatitis: Transient organ failure (resolves within 48 hours) and/or local complications (e.g., peripancreatic fluid collections, necrosis).
-
Severe Acute Pancreatitis: Persistent organ failure (lasting >48 hours) involving one or more organs. This carries high mortality.
Common Etiologies (The “GET SMASHED” Mnemonic):
-
Gallstones (Most common ~40%)
-
Ethanol (Alcohol) (Second most common ~30%)
-
Trauma
-
Steroids, Scorpion sting
-
Mumps, Malignancy
-
Autoimmune, Hypertriglyceridemia (Annotation: hypertriglyceridemia is a key other cause)
-
Surgery, ERCP
-
Hypercalcemia, Hyperparathyroidism
-
Endoscopic Retrograde Cholangiopancreatography (ERCP) (already listed)
-
Drugs
For the coder, this clinical framework is essential. The etiology (gallstone, alcohol, drug, etc.) drives the primary code selection. The severity and development of complications (organ failure, pseudocysts, necrosis) will require additional codes. The following sections will translate this clinical knowledge directly into the ICD-10-CM framework.
3. The ICD-10-CM Framework: Chapter 11 (K85)
Acute pancreatitis is classified within ICD-10-CM’s Chapter 11: Diseases of the Digestive System (K00-K95). The specific category is K85: Acute pancreatitis.
The structure of ICD-10-CM emphasizes specificity. Unlike its predecessor ICD-9-CM, which had a single code for acute pancreatitis (577.0), ICD-10-CM requires the coder to identify, to the greatest degree of specificity documented, the underlying etiology or to indicate when the cause is unspecified.
The parent code K85 includes several important clinical concepts within its “includes” notes: acute (recurrent) pancreatitis, abscess of the pancreas, and necrosis of the pancreas (acute, infected). This is critical: if a provider documents “acute necrotizing pancreatitis,” the coder does not code the necrosis separately unless it is specified as a complication or sequela of a previous episode. The necrosis is inherent to this specific acute episode coded under K85.-.
Excludes1 and Excludes2 Notes (The Coder’s Compass):
-
Excludes1: Chronic pancreatitis (K86.1) and Chronic relapsing pancreatitis (K86.1). This is a vital distinction. An Excludes1 note means “not coded here.” If the provider clearly documents a chronic condition, even if it is flaring, you cannot use K85. You must use a code from the chronic pancreatitis family. The acuity (acute exacerbation) may be captured with an additional code if documented (e.g., acute on chronic).
-
Excludes2: Alcohol-induced chronic pancreatitis (K86.0). This reinforces the distinction. Alcohol-induced acute pancreatitis goes to K85.2. Alcohol-induced chronic pancreatitis goes to K86.0.
4. Deconstructing K85: Acute Pancreatitis and its Essential Modifiers
The category K85 is subdivided based on etiology. The fourth, fifth, and sometimes sixth characters provide the required specificity.
K85.0 – Idiopathic acute pancreatitis
K85.1 – Biliary acute pancreatitis
K85.2 – Alcohol-induced acute pancreatitis
K85.3 – Drug-induced acute pancreatitis
K85.8 – Other acute pancreatitis
K85.9 – Acute pancreatitis, unspecified
The default, unspecified code (K85.9) should be a last resort. Official coding guidelines and quality metrics push for specificity. Using K85.9 when the etiology is known or can be inferred from the medical record is clinically inaccurate and may impact reimbursement and data quality.
The following sections will dissect each of these subcategories in exhaustive detail.
5. The Alcohol Question: The Critical Distinction of K85.2
K85.2: Alcohol-induced acute pancreatitis is one of the most commonly used and critically important codes in this category.
Clinical Context: Alcohol is a direct cellular toxin to the pancreas. The risk correlates with the amount and duration of alcohol consumption, though acute pancreatitis can occur after a single binge episode in susceptible individuals. The diagnosis is often one of exclusion after ruling out gallstones and other causes, but a strong history of heavy alcohol use is typically present.
Coding Logic: Assign K85.2 when the provider’s documentation explicitly states the acute pancreatitis is due to alcohol or when the clinical context overwhelmingly supports it as the cause. This is where the coder’s knowledge and the need for querying intersect.
Documentation Triggers for K85.2:
-
“Acute alcoholic pancreatitis.”
-
“Acute pancreatitis secondary to ethanol abuse.”
-
“Pancreatitis due to heavy alcohol use.”
-
Documentation of significant alcohol history (e.g., “patient admits to 1 pint of whiskey daily”) alongside a diagnosis of acute pancreatitis without mention of another cause (e.g., no gallstones on ultrasound). However, in this scenario, a query to the provider to confirm etiology is the gold-standard, compliant practice.
The Query is Key: If a patient with a history of chronic alcohol use is admitted with acute pancreatitis and imaging shows no gallstones, the coder or CDI specialist should query: “Can you clarify the etiology of the acute pancreatitis? Is it related to alcohol use, idiopathic, or another cause?” This query ensures accurate, provider-confirmed coding.
Associated Coding: Always check for and code associated conditions using additional codes:
-
Alcohol abuse (F10.1-) or Alcohol dependence (F10.2-) based on provider documentation.
-
Acute alcohol intoxication (F10.129, F10.229, F10.929) if applicable.
-
Any withdrawal states (F10.23-, F10.93-).
-
Acute respiratory failure (J96.0-) or Acute kidney failure (N17.9) if they develop as complications.
6. Biliary Acute Pancreatitis (K85.1): The Gallstone Connection
K85.1: Biliary acute pancreatitis is the code for the most common etiology—gallstones.
Pathophysiology: A gallstone, typically from the gallbladder, migrates and becomes impacted at the ampulla of Vater (where the common bile duct and pancreatic duct usually meet). This obstruction causes a backup of pancreatic secretions, triggering enzyme activation and inflammation.
Coding Logic: Assign K85.1 when the provider links the acute pancreatitis to gallstones, biliary sludge, or microlithiasis.
Documentation Triggers for K85.1:
-
“Acute biliary pancreatitis.”
-
“Gallstone pancreatitis.”
-
“Acute pancreatitis due to choledocholithiasis.”
-
Imaging reports confirming cholelithiasis or choledocholithiasis in a patient diagnosed with acute pancreatitis, with provider documentation linking the two.
Associated and Combination Coding: This is where coding becomes intricate. Often, the biliary tract disease itself needs to be coded.
-
Cholelithiasis (K80.20, K80.10, etc.): Code the specific type of gallstones if documented.
-
Choledocholithiasis (K80.30-K80.37): Stones in the common bile duct.
-
Acute cholecystitis (K81.0-): If the gallbladder is also inflamed.
-
Biliary obstruction (K83.1): If documented.
Sequencing: The principal diagnosis is typically the condition that occasioned the admission. For a patient admitted for workup and management of severe abdominal pain found to be acute gallstone pancreatitis, K85.1 is the principal diagnosis. The associated cholelithiasis is a secondary diagnosis. If the patient is admitted for elective cholecystectomy due to known stones and develops acute pancreatitis post-operatively, the pancreatitis becomes a complication code.
7. Drug-Induced Acute Pancreatitis (K85.3): Causality and Specificity
K85.3: Drug-induced acute pancreatitis requires careful attention to causality and the use of additional codes from the T36-T50 series.
Clinical Context: Numerous medications are associated with pancreatitis, including certain antibiotics, diuretics (furosemide, thiazides), antivirals, immunosuppressants, and others. Diagnosis is often based on a temporal relationship (symptoms starting after drug initiation) and exclusion of other causes.
Coding Logic: Assign K85.3 only when the provider explicitly states the pancreatitis is drug-induced or related to a specific medication.
Crucial Step: The T Code. You MUST use an additional code from categories T36-T50 (with fifth or sixth character 5) to identify the causative drug.
-
Example: Acute pancreatitis due to azathioprine.
-
K85.3 (Drug-induced acute pancreatitis)
-
T45.1X5A (Adverse effect of antineoplastic and immunosuppressive drugs, initial encounter)
-
Documentation & Queries: Provider documentation is often vague: “Pancreatitis, possibly related to medication.” This is inadequate for K85.3. A query is necessary: “Can you confirm if the acute pancreatitis is definitively attributed to [drug name]? If so, please document ‘drug-induced acute pancreatitis due to [drug name].'”
8. Other and Idiopathic Etiologies: Navigating K85.8 and K85.9
K85.8: Other acute pancreatitis is used for documented etiologies not represented by the previous codes.
-
Examples: Post-ERCP pancreatitis, traumatic pancreatitis, pancreatitis due to hypertriglyceridemia, autoimmune pancreatitis (acute presentation), post-operative pancreatitis.
-
Coding: Use K85.8 and always code the underlying condition first if it is the reason for admission/encounter.
-
Hypertriglyceridemia-induced: E78.1 (Pure hyperglyceridemia) followed by K85.8.
-
Post-ERCP: First, code the complication (K85.8), then the procedure reason. Sequencing depends on the circumstance of admission.
-
Traumatic: Code the specific injury (e.g., S36.220- Major contusion of pancreas) as principal, followed by K85.8 to indicate the resulting acute pancreatitis.
-
K85.9: Acute pancreatitis, unspecified is the default when the medical record does not specify an etiology despite adequate workup, or the provider documents “acute pancreatitis” without further qualification.
-
Best Practice: This code should be used sparingly. CDI and coding professionals should query for specificity when clinical indicators (alcohol history, gallstones on imaging) are present but unlinked by the provider. Only use K85.9 after all avenues for clarification have been exhausted.
9. Associated Conditions: The Imperative of Combination Coding
Acute pancreatitis rarely exists in a vacuum. The coder must vigilantly look for and capture associated conditions that paint the complete clinical picture.
Hypertriglyceridemia (E78.1): A known cause. If documented as the cause, sequence first with K85.8. If present but not deemed the cause, it is still coded as a comorbidity.
Hypercalcemia (E83.52): Another potential cause.
Diabetes Mellitus (E08-E13): Pancreatitis can cause transient hyperglycemia, but pre-existing diabetes is a significant comorbidity.
Chronic liver disease (K70-K77), Cirrhosis (K74.-): Common in patients with alcohol etiology.
Morbid obesity (E66.01): A significant risk factor and comorbidity.
10. Complications: Coding Beyond the Initial Diagnosis
The severity and cost of an acute pancreatitis admission are largely determined by its complications. These must be coded when present.
Local Complications:
-
Acute Pancreatic Fluid Collection (APFC): Common in early interstitial edematous pancreatitis. Often not coded separately unless specifically addressed.
-
Pancreatic Pseudocyst (K86.3): A mature, walled-off fluid collection that persists >4 weeks. Code K86.3 in addition to the acute pancreatitis code (e.g., K85.2). This is a sequela of acute pancreatitis.
-
Acute Necrotic Collection (ANC) / Walled-Off Necrosis (WON): Collections containing necrotic material. Often managed invasively. Specific documentation is required; they may be captured under the parent K85 code but if described as a chronic sequelae, separate coding may be needed.
-
Infected Pancreatic Necrosis: A life-threatening complication. Coded with additional code B96.89 (Other specified bacterial agents) if the organism is known, and potentially a code for sepsis.
Systemic Complications (Organ Failure):
-
Acute Respiratory Failure (J96.0-): A hallmark of severe pancreatitis. Code when documented.
-
Acute Kidney Injury (N17.9): Common in severe cases.
-
Shock (R57.-, A41.9 with septic shock): Code the specific type.
-
Systemic Inflammatory Response Syndrome (SIRS) of non-infectious origin (R65.10-R65.11): May be applicable before a diagnosis of pancreatitis is confirmed.
Table 1: ICD-10-CM Coding Pathway for Acute Pancreatitis
| Clinical Scenario (Provider Documentation) | Primary ICD-10-CM Code(s) | Rationale & Additional Codes |
|---|---|---|
| “Acute alcoholic pancreatitis” in a patient with dependence. | K85.2, F10.20 (Alcohol dependence) | Etiology is alcohol. Always code the associated mental/behavioral disorder. |
| “Acute gallstone pancreatitis” with confirmed common bile duct stones. | K85.1, K80.35 (Choledocholithiasis with cholangitis) | Etiology is biliary. Code the specific biliary tract disease. |
| “Acute pancreatitis due to hypertriglyceridemia.” | E78.1, K85.8 | Code the underlying cause first, then “other” acute pancreatitis. |
| “Acute pancreatitis, unspecified cause.” (After workup) | K85.9 | Used only when no etiology is documented or identified. |
| “Acute necrotizing pancreatitis, idiopathic.” | K85.0 | Necrosis is included in the K85 category. |
| “Drug-induced acute pancreatitis due to azathioprine.” | K85.3, T45.1X5A | Must use both the drug-induced pancreatitis code and the T code for the specific drug. |
| “Acute on chronic pancreatitis, alcoholic.” | K86.0 (Alcohol-induced chronic pancreatitis) | The “acute” flare is inherent in the exacerbation of the chronic condition. Do not use K85.2. |
| “Acute pancreatitis with associated pseudocyst formation.” | K85.9 (or specific etiology), K86.3 | Code the acute pancreatitis first, then the pseudocyst as an associated condition. |
| “Post-ERCP acute pancreatitis.” | K85.8, Code for reason of ERCP (e.g., K80.34) | The complication (pancreatitis) is coded, along with the condition that prompted the procedure. |
11. The Documentation Imperative: What Coders Need from Providers
Clear, specific, and consistent documentation is the foundation of accurate coding. Providers should be educated to document:
-
Specific Etiology: “Biliary,” “alcoholic,” “hypertriglyceridemia-induced,” “idiopathic.”
-
Severity: Mention of organ failure (respiratory, renal, circulatory), necrosis, or local complications.
-
Clear Links: “Due to,” “secondary to,” “attributed to” linking the cause to the pancreatitis.
-
Chronicity: Distinguish clearly between “acute,” “chronic,” and “acute on chronic.”
-
Complications: Explicitly name any complications that develop (pseudocyst, abscess, respiratory failure).
12. Sequencing and Principal Diagnosis Selection
The principal diagnosis is defined as the condition established after study to be chiefly responsible for occasioning the admission of the patient to the hospital. In most straightforward admissions for acute pancreatitis, the specific K85.- code is the principal diagnosis.
Exceptions:
-
If the patient is admitted for management of hypertriglyceridemia (E78.1) and develops pancreatitis, E78.1 may be principal.
-
If acute pancreatitis develops as a post-procedural complication, the complication code (K85.8) may be sequenced first, followed by the codes for the reason for the procedure and the procedure itself.
-
In acute on chronic scenarios, the chronic condition (K86.0, K86.1) is principal.
13. Case Studies: Applying Logic to Real-World Scenarios
Case 1: A 45-year-old male presents to the ED with severe epigastric pain radiating to the back, nausea, and vomiting. He has a history of heavy alcohol use. Lipase is 1200 U/L. CT shows edematous pancreatitis with no evidence of gallstones. The ED physician documents “acute pancreatitis, likely secondary to EtOH use.” The admitting gastroenterologist documents “Acute pancreatitis.”
-
Coding Action: Query the gastroenterologist to link the etiology: “Based on the patient’s history and ED assessment, can you confirm the acute pancreatitis is alcohol-induced?” If confirmed, code K85.2 and F10.10 (Alcohol abuse).
Case 2: A 60-year-old female is admitted with severe abdominal pain. Ultrasound shows multiple gallstones and a dilated common bile duct. MRCP confirms a stone in the distal CBD. Lipase is 2500 U/L. The surgeon documents “Acute biliary pancreatitis with choledocholithiasis.”
-
Coding: K85.1 (principal), K80.35 (Choledocholithiasis with cholangitis), K80.20 (Calculus of gallbladder without cholecystitis).
Case 3: A patient is admitted for an exacerbation of Crohn’s disease. On hospital day 3, they develop severe abdominal pain and a lipase of 1800. The team documents “Acute pancreatitis, likely related to azathioprine therapy; will hold medication.”
-
Coding Action: This is strong but not definitive. A query is ideal: “Can you confirm the acute pancreatitis is definitively attributed to azathioprine?” If confirmed: K85.3, T45.1X5A, plus the codes for Crohn’s disease.
14. Common Coding Pitfalls and How to Avoid Them
-
Assuming Etiology: Never code K85.2 based solely on a social history of alcohol use without provider linkage. Query.
-
Mistaking Acute for Chronic: Do not use K85.- for “acute exacerbation of chronic pancreatitis.” Use K86.0 or K86.1.
-
Omitting T Codes: Always add the T36-T50 code for drug-induced cases (K85.3).
-
Under-coding Complications: Actively look in progress notes, nursing notes, and consult reports for mentions of organ failure, pseudocysts, or infections.
-
Defaulting to K85.9: Use this code only after all efforts to obtain specificity have failed.
15. The Impact on DRG Assignment and Reimbursement
The MS-DRG system groups clinically similar patients with similar resource use. For pancreatitis, the DRG assignment (e.g., DRG 441 – Disorders of the Pancreas except Malignancy w MCC/CC, DRG 442 w/o MCC/CC) is heavily influenced by:
-
The presence of Complications/Comorbidities (CCs) or Major CCs (MCCs): Codes for acute respiratory failure (J96.0-), acute kidney failure (N17.9), sepsis (A41.9), shock (R57.-) are often MCCs. Pseudocyst (K86.3) may be a CC.
-
Etiology: While not directly changing the DRG, specific etiology supports medical necessity and can impact the severity of illness (SOI) and risk of mortality (ROM) scores.
-
Procedure Codes: If complex procedures like necrosectomy or percutaneous drainage are performed, a surgical DRG may apply.
Accurate, specific coding ensures the DRG accurately reflects the patient’s true clinical picture and the hospital’s resource utilization, leading to appropriate and compliant reimbursement.
16. The Future: ICD-11 and Beyond
The World Health Organization’s ICD-11, which some countries are adopting, offers even greater specificity for pancreatitis. While the US continues with ICD-10-CM, understanding the trajectory is helpful. ICD-11 has separate entities for acute pancreatitis (DC31) with detailed extension codes for etiology (alcohol, gallstones, drugs, etc.), morphology (necrotizing, infected), and severity (organ failure). This granularity reinforces the industry’s direction toward highly specific, clinically rich data capture.
17. Conclusion
ICD-10-CM coding for acute pancreatitis exemplifies the modern coder’s role as a crucial translator of clinical narrative into precise data. Moving beyond K85.9 to the specific etiologic codes (K85.1, K85.2, K85.3, etc.) is not merely a technical requirement—it is fundamental to accurate billing, robust clinical research, effective public health surveillance, and ultimately, the understanding and improvement of patient care for this serious condition. Mastery of this topic requires a symbiotic partnership between detailed provider documentation and vigilant, knowledgeable coding practices.
18. Frequently Asked Questions (FAQs)
Q1: The provider documents “acute pancreatitis” and the ultrasound shows gallstones, but the provider doesn’t explicitly say “biliary.” Can I code K85.1?
A: No. You cannot assume causality. You must query the provider to link the gallstones to the pancreatitis. Use K85.9 until clarification is obtained.
Q2: How do I code “acute on chronic alcoholic pancreatitis”?
A: Code K86.0 (Alcohol-induced chronic pancreatitis). The “acute on chronic” or exacerbation is inherent in this code. Do not use an additional acute pancreatitis code (K85.2).
Q3: A patient has acute pancreatitis and develops a pancreatic pseudocyst 6 weeks later in a follow-up visit. How is this coded?
A: For the follow-up visit, the acute pancreatitis has likely resolved. Code K86.3 (Pancreatic pseudocyst) as the primary diagnosis for that encounter. You would not use an acute pancreatitis code.
Q4: When coding drug-induced pancreatitis (K85.3), what character is used in the T code?
A: You typically use the 5th or 6th character 5 (indicating “adverse effect”) in the T code, as the drug was prescribed correctly and taken as intended, but an unintended reaction occurred.
Q5: What is the difference between K85.8 and K85.9?
A: K85.8 is for a known, specified cause not listed in K85.0-K85.3 (e.g., post-ERCP, traumatic, due to hypertriglyceridemia). K85.9 is used when the cause is unknown or simply not specified in the documentation.
19. Additional Resources
-
Official Source: The ICD-10-CM Official Guidelines for Coding and Reporting (FY 2025): https://www.cms.gov/medicare/coding-billing/icd-10-codes/2025-icd-10-cm
-
Clinical Reference: The Revised Atlanta Classification of Acute Pancreatitis (2012) – Published in Gut.
-
Professional Organizations:
-
American Health Information Management Association (AHIMA): https://www.ahima.org/
-
American Academy of Professional Coders (AAPC): https://www.aapc.com/
-
Disclaimer: This article is intended for educational and informational purposes only. It is not a substitute for professional medical coding advice, clinical guidance, or the official ICD-10-CM coding manuals and guidelines. Always consult the most current, official resources and facility-specific policies for definitive coding and billing decisions.
Date: December 24, 2025
Author: The Medical Coding Institute






