If you are an anesthesiologist, a certified registered nurse anesthetist (CRNA), or a medical coder, you know that precision matters. One small mistake on a claim can lead to a denied payment or a compliance headache.
Today, we are focusing on a very common but often confusing procedure: the interscalene block.
You might have a simple question: What is the exact CPT code for interscalene block?
But the real answer is more than just a five-digit number. It involves understanding the difference between single injections and continuous catheters, knowing when to add modifiers, and recognizing what payers expect to see in your documentation.
Let us walk through everything you need to know.
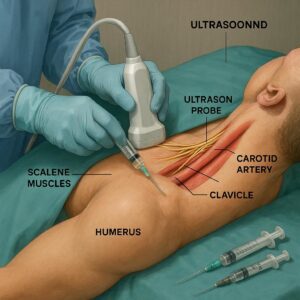
CPT Code for Interscalene Block
The Short Answer: The Primary Code
When you perform a single-injection interscalene brachial plexus block for anesthesia or postoperative pain management, the correct code is:
CPT 64418
To be precise: 64418 – Injection, anesthetic agent; brachial plexus, interscalene.
This code describes the injection of a local anesthetic (like ropivacaine or bupivacaine) into the interscalene groove to block the nerves that supply the shoulder and upper arm.
When To Use 64418
You will use 64418 in several common scenarios:
-
A patient undergoing arthroscopic shoulder surgery receives a preoperative block.
-
A patient with a proximal humerus fracture receives a block for pain control in the emergency department.
-
A patient having a rotator cuff repair gets the block as the primary anesthetic or as a supplement to general anesthesia.
A quick note: Code 64418 is for the procedure of injecting the anesthetic. It is separate from the medical direction time (base units + time units) you bill for anesthesia care. We will cover that integration later.
The Most Common Mistake: Confusing 64418 with Other Nerve Blocks
One reason coders hesitate is that several CPT codes exist for brachial plexus blocks. They are not interchangeable.
Let us clear up the confusion with a simple comparison.
| CPT Code | Procedure Description | Key Distinction |
|---|---|---|
| 64418 | Brachial plexus, interscalene | Needle placement in the interscalene groove (C5-C6 roots). |
| 64415 | Brachial plexus, axillary | Needle placement in the axilla. Used for hand/forearm surgery. |
| 64417 | Brachial plexus, supraclavicular | Needle placement above the clavicle. |
| 64416 | Brachial plexus, continuous infusion | Catheter placement for prolonged infusion (any approach). |
| 64420 | Intercostal nerve, single | For rib fractures or chest wall pain. Different anatomy. |
Why does this matter? If you perform an interscalene block but accidentally bill 64415 (axillary), the payer will likely deny the claim. The anatomical sites are completely different. Always double-check your code before submission.
Continuous Catheters: The Catheter Code (64416)
Sometimes, a single injection is not enough. For major shoulder surgeries (like total shoulder arthroplasty or complex rotator cuff repairs), a surgeon may want pain control for 24 to 72 hours.
In that case, you place a continuous interscalene catheter.
The correct code is CPT 64416.
*64416 – Injection(s), anesthetic agent and/or steroid, brachial plexus, continuous infusion by catheter (including catheter placement), interscalene.*
What 64416 Includes
When you bill 64416, the payment covers:
-
The placement of the catheter using ultrasound or nerve stimulation.
-
The injection of a loading dose.
-
The connection of the catheter to a pump (elastomeric or electronic).
-
Instructions for the patient or nursing staff.
You do not bill 64418 separately on the same day for the same patient. The catheter code is more comprehensive and has a higher relative value unit (RVU).
A Realistic Scenario
Dr. Lee performs an interscalene block with a single injection for a routine arthroscopy. She bills 64418.
Dr. Patel performs an interscalene block with a catheter for a total shoulder replacement. The catheter will infuse local anesthetic for 48 hours. He bills 64416.
Both are correct. The difference is the duration and complexity of the service.
Billing for Ultrasound Guidance
Here is a topic that generates many questions. Do you add a separate code for ultrasound guidance?
The short answer is usually no, you do not bill separately.
In 2019, the American Medical Association (AMA) and the Centers for Medicare & Medicaid Services (CMS) made a significant change. They bundled ultrasound guidance into the primary nerve block code for most peripheral nerve blocks.
For CPT 64418 and 64416, ultrasound guidance is now considered an integral part of the procedure. You cannot bill 76942 (Ultrasonic guidance for needle placement) separately.
When can you bill ultrasound separately?
There are rare exceptions, but they are uncommon in daily practice. For standard interscalene blocks performed in an operating room or procedure suite, you should assume the ultrasound guidance is included.
Important Note for Readers: Private commercial payers sometimes have different rules. A few may still accept a separate ultrasound code. However, the majority follow CMS guidelines. To be safe, check your specific payer policies. When in doubt, do not add 76942. You risk an automatic denial.
Modifiers: The Secret to Getting Paid Correctly
A code alone is rarely enough. Modifiers tell the payer important details about the service. For interscalene blocks, two modifiers matter the most.
Modifier 59 – Distinct Procedural Service
Use modifier 59 when the interscalene block is performed on the same day as another nerve block that is not typically performed together.
Example: A patient has both shoulder pain (interscalene block) and knee pain (femoral nerve block). You perform both blocks during the same encounter.
You would bill:
-
64418 – Interscalene block
-
64447 – Femoral nerve block with modifier 59
The modifier tells the payer, “These are separate and distinct procedures on different anatomical sites.”
Modifier 50 – Bilateral Procedure
What if a patient needs an interscalene block on both the left and right sides? This is rare but possible (bilateral shoulder surgery, for example).
You have two options:
-
Bill one line with 64418 50 (bilateral). Medicare will pay 150% of the fee schedule amount.
-
Bill two lines: 64418-LT and 64418-RT. Some commercial payers prefer this method.
Check your local MAC’s guidance. In most cases, using modifier 50 is acceptable.
Time Units and Base Units: How Anesthesia Billing Works
Many readers here work in an anesthesia setting. You need to know how 64418 interacts with anesthesia time.
When you provide regional anesthesia for a surgical procedure, you typically bill two things:
-
The anesthesia service (using CPT codes like 01610 for shoulder surgery).
-
The nerve block (using CPT 64418).
The Most Important Rule
You cannot count the time spent performing the interscalene block as anesthesia time.
Let me repeat that: The 5 to 10 minutes you spend performing the block is not part of the anesthesia start-to-end time.
Why? CMS and other payers consider the block a separate procedure. The anesthesia time begins when you start preparing the patient for the operating room (induction of anesthesia) and ends when you transfer care to the post-anesthesia care unit (PACU).
If you perform the block in a holding area before moving the patient to the OR, that time is excluded from anesthesia time.
A Practical Example
-
8:00 AM – You begin the interscalene block in pre-op.
-
8:10 AM – Block is complete.
-
8:15 AM – Patient enters OR. Anesthesia time begins.
-
9:15 AM – Surgery ends. Anesthesia time ends.
Total anesthesia time: 60 minutes (1 hour).
Separate billable procedure: 64418.
You receive base units for the anesthesia code + time units (60 minutes) + payment for 64418.
Medicare Payment Rates (2026 Estimates)
Money matters. Let us look at realistic payment rates for 64418 and 64416.
Please note: These are estimates. Actual payment varies by geographic location and facility type.
| CPT Code | Total RVUs (2026 approx.) | Estimated Facility Payment |
|---|---|---|
| 64418 | 3.50 | $125 – $150 |
| 64416 | 6.20 | $220 – $260 |
These amounts are for the professional component only. The facility (hospital or ASC) bills separately for supplies and room use.
What About Multiple Blocks?
If you perform an interscalene block and a second, unrelated nerve block (like a sciatic block for the leg), you bill both. Payers generally reimburse both at 100% because they serve different anatomical regions.
If you perform two interscalene blocks on the same patient (left and right side) on the same day, use modifier 50 or LT/RT as discussed. Do not bill two units of 64418 on a single line without a modifier. That will likely be denied as a duplicate.
Documentation Requirements: Protecting Your Claim
Payers deny claims for two main reasons: missing documentation or conflicting documentation. Here is what your procedure note must include for an interscalene block.
A Documentation Checklist
-
Patient identification: Name, date of birth, medical record number.
-
Indication: Why is the block being performed? (e.g., “Postoperative analgesia for right rotator cuff repair.”)
-
Informed consent: A note confirming consent was obtained.
-
Site marking: Verification of the correct side (left or right).
-
Technique: Ultrasound-guided or nerve stimulation? (Ultrasound is standard.)
-
Local anesthetic: Name, concentration, volume, and any additives (epinephrine, dexamethasone).
-
Needle type and size.
-
Any complications or immediate adverse reactions.
-
Block success assessment: Was a sensory or motor response noted?
-
Signature and credentials of the provider.
A Sample Procedure Note Snippet
*”Ultrasound-guided right interscalene brachial plexus block performed. After sterile prep and draping, the interscalene groove was identified using a high-frequency linear probe. A 22-gauge, 50mm Stimuplex needle was advanced in-plane. After negative aspiration, 20mL of 0.5% ropivacaine with 4mg dexamethasone was injected in 5mL aliquots with gentle hydrodissection. No paresthesia or pain reported. Immediate sensory block noted to the deltoid. Patient tolerated well.”*
This level of detail supports medical necessity and justifies the use of 64418.
Common Denials and How to Avoid Them
Even experienced coders make mistakes. Here are the top three denials for CPT 64418 and how to prevent them.
Denial 1: “Procedure not separately payable”
Why it happens: You billed 64418 on the same day as a surgical procedure that has a “global surgical package” that includes postoperative pain management. Some payers argue that the block is part of the surgery.
How to fix it: Append modifier 59 (or XS, XU) to show the block was a distinct service. Also, check the National Correct Coding Initiative (NCCI) edits. As of 2026, 64418 is generally separately payable with most shoulder surgeries.
Denial 2: “Missing or invalid modifier”
Why it happens: You billed 64418 without an LT or RT modifier, and the payer cannot determine which side was treated.
How to fix it: Always append LT (left) or RT (right) to 64418 and 64416. This is a best practice, even if your local payer does not technically require it. It prevents confusion.
Denial 3: “Incorrect code for service billed”
Why it happens: You used 64415 (axillary) instead of 64418 (interscalene).
How to fix it: Review your documentation. If the procedure note says “interscalene,” use 64418. If it says “axillary,” use 64415. Never guess based on the surgery type. Always code from the documentation.
Frequently Asked Questions (FAQ)
Q1: Can a CRNA bill CPT 64418 independently?
Yes, in most states. CRNAs can perform and bill for peripheral nerve blocks if they are practicing within their state scope of practice and under appropriate physician supervision (if required by the facility or payer). Medicare allows CRNAs to bill for these services directly.
Q2: What is the difference between 64418 and 64416 in terms of documentation?
For 64418, you document a single injection. For 64416, you must document catheter placement, confirmation of catheter position (often with ultrasound or contrast), connection to an infusion device, and post-procedure instructions for catheter management.
Q3: Do I need a separate consent form for the interscalene block?
Most facilities include nerve blocks in the general anesthesia consent form. However, best practice is to have a separate line item or a dedicated consent for regional anesthesia that mentions the risks (pneumothorax, phrenic nerve palsy, hoarseness).
Q4: How do I bill for an interscalene block performed in the emergency department?
The same code applies: 64418. The ED physician bills the code with an appropriate E/M service (e.g., 99283) using modifier 25 to show the block was a separately identifiable service.
Q5: Is there a specific ICD-10 code I need to use with 64418?
You need a diagnosis that supports medical necessity. Common codes include:
-
M25.511 – Pain in right shoulder
-
M25.512 – Pain in left shoulder
-
S42.201A – Fracture of upper end of unspecified humerus (initial encounter)
-
Z98.89 – Postprocedural pain (for elective surgery cases)
Never use an unlisted code like M79.10 (Myalgia, unspecified) unless the documentation truly supports it.
Q6: Can I bill 64418 if the block fails?
Yes, if you performed the procedure with the intent to provide a therapeutic nerve block, you bill for the work performed. A failed block is still a procedure. However, you cannot bill a second 64418 for a repeat attempt on the same day on the same nerve. That would be considered a single service.
Q7: Does Medicare cover interscalene blocks for chronic pain?
Sometimes. Medicare covers nerve blocks for diagnostic or therapeutic purposes for chronic pain conditions, but there are strict local coverage determinations (LCDs). You may need to provide documentation of failed conservative treatment (physical therapy, medications) before Medicare will pay for a block for conditions like chronic shoulder pain.
Additional Resources
For the most up-to-date information, always refer to official sources. Coding changes every year.
-
CMS NCCI Policy Manual: This document explains which codes are bundled. Read Chapter 4 on nerve blocks.
-
ASA Relative Value Guide (RVG): Published annually by the American Society of Anesthesiologists. This is the gold standard for anesthesia coding.
-
Your Local MAC’s LCD: Search for “Interscalene nerve block LCD” plus your state. Medicare Administrative Contractors publish local rules.
[Link to CMS NCCI Edits Search Tool (External Resource)]
Conclusion
To summarize clearly: The correct CPT code for a single-injection interscalene block is 64418. For a continuous catheter, use 64416. Always append LT or RT modifiers, never bill ultrasound guidance separately for standard cases, and document thoroughly. Mastering these details will reduce denials and ensure fair reimbursement for your work.
Final Checklist Before You Submit Your Claim:
-
Did I use 64418 (single) or 64416 (catheter)?
-
Did I add LT or RT?
-
Did I avoid adding 76942 for ultrasound?
-
Is my procedure note complete and signed?
-
Does my ICD-10 code match the medical necessity?
Thank you for reading. Code responsibly.






