In the vast and intricate ecosystem of modern healthcare, a single alphanumeric sequence—J45.909—carries immense weight. To the untrained eye, it is a meaningless jumble of characters. But to clinicians, medical coders, health informaticists, and healthcare administrators, it is a precise, condensed story. It tells a tale of a patient’s encounter, a diagnosed condition, a treatment rendered, and a service billed. This code, which stands for “Asthma, unspecified, uncomplicated,” is one of the most frequently used codes in respiratory medicine, yet it is also one of the most misunderstood and often misapplied.
This article embarks on a comprehensive journey to decode J45.909. We will move beyond the dry definitions of coding manuals to explore the clinical, administrative, and financial realities that orbit this ubiquitous code. Why does “unspecified” exist in an era that demands precision? What are the risks of over-relying on this catch-all category? How can healthcare providers document patient encounters more effectively to ensure accurate coding, leading to better patient outcomes and appropriate reimbursement? By answering these questions, we aim to transform J45.909 from a nebulous administrative tool into a clear, understood, and correctly applied component of high-quality patient care. This is not just about coding; it’s about the language we use to describe human health, and mastering this language is fundamental to the future of medicine.
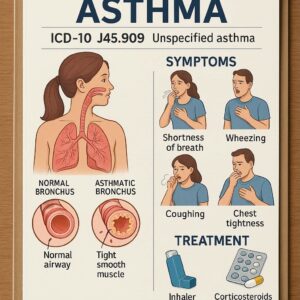
ICD-10 Code for Unspecified Asthma
2. Understanding Asthma: A Brief Pathophysiology Refresher
To truly appreciate the nuances of asthma coding, one must first understand the disease itself. Asthma is not a single, monolithic condition but rather a heterogeneous syndrome characterized by chronic airway inflammation.
The pathophysiology involves a complex interplay of factors:
-
Airway Inflammation: The fundamental characteristic. Allergens, irritants, or viral infections trigger an immune response, leading to swelling of the airway walls, infiltration of inflammatory cells (e.g., eosinophils, mast cells), and production of excess mucus.
-
Airway Hyperresponsiveness (AHR): The airways of an asthmatic become overly sensitive to a wide range of stimuli (e.g., cold air, exercise, smoke). This hyperresponsiveness causes the smooth muscles surrounding the airways to constrict excessively and easily.
-
Variable Airflow Obstruction: The inflammation, mucus, and bronchoconstriction combine to narrow the airways. This obstruction is often reversible, either spontaneously or with bronchodilator medication.
-
Airway Remodeling: In chronic, poorly controlled asthma, long-term inflammation can lead to structural changes in the airway walls, including fibrosis, hypertrophy of smooth muscle, and angiogenesis. This remodeling can lead to a permanent decline in lung function.
This complexity is precisely why asthma manifests in so many different ways—as mild intermittent symptoms, severe persistent attacks, exercise-induced bronchospasm, or allergic asthma. Recognizing these subtypes is the first step toward moving away from “unspecified” and toward precise, meaningful documentation and coding.
3. The ICD-10 Coding System: A Language of Healthcare
The International Classification of Diseases, Tenth Revision (ICD-10) is the foundational system for coding morbidity and mortality statistics, endorsed by the World Health Organization (WHO). In the United States, the Centers for Medicare & Medicaid Services (CMS) and the National Center for Health Statistics (NCHS) maintain a clinically modified version known as ICD-10-CM (Clinical Modification), which is used for diagnostic coding.
Think of ICD-10-CM not as a mere list of codes, but as a sophisticated, hierarchical language. Its purpose is multifold:
-
Standardization: It provides a common language for describing diseases, injuries, and health encounters across the entire healthcare spectrum.
-
Epidemiology and Public Health: It allows for the tracking, analysis, and comparison of morbidity and mortality data across populations and countries. This is crucial for identifying disease outbreaks, allocating resources, and guiding public health policy.
-
Reimbursement: It is the bedrock of the medical billing process. Diagnoses codes are required on claims submitted to insurance companies to justify the medical necessity of services rendered (procedures coded with CPT® or HCPCS codes).
-
Clinical Decision Support: Coded data fuels electronic health record (EHR) systems, enabling clinical decision support tools, population health management, and quality improvement initiatives.
The structure of an ICD-10-CM code is logical. It can be anywhere from 3 to 7 characters long, with each character adding a layer of specificity. The code always begins with a letter, followed by two numbers. This represents the chapter (e.g., “J” for Diseases of the Respiratory System). The characters after the decimal point provide details about etiology, anatomical site, severity, and other clinical specifics.
4. Deep Dive into Chapter X: Diseases of the Respiratory System (J00-J99)
Our code of interest, J45.909, resides in Chapter X of ICD-10-CM. This chapter covers a wide array of conditions, from the common cold (J00) to lung cancer (C34.-, though neoplasms are primarily in Chapter II) and chronic obstructive pulmonary disease (COPD) (J44.-).
Chapter X codes are particularly sensitive to laterality (which lung or lobe is affected) and acuity (acute vs. chronic). The codes are organized into blocks based on anatomical site and disease type (e.g., J00-J06: Acute Upper Respiratory Infections; J40-J47: Chronic Lower Respiratory Diseases).
It is within this chapter that we find the block for Chronic Lower Respiratory Diseases (J40-J47), which includes:
-
J40: Bronchitis, not specified as acute or chronic
-
J41: Simple and mucopurulent chronic bronchitis
-
J42: Unspecified chronic bronchitis
-
J43: Emphysema
-
J44: Other chronic obstructive pulmonary disease (This is a critical code to differentiate from asthma, though they can coexist)
-
J45: Asthma
-
J46: Status asthmaticus
-
J47: Bronchiectasis
This organization highlights the importance of differential diagnosis. Coding a patient with chronic airflow obstruction as asthmatic (J45) versus having COPD (J44) has significant clinical and reimbursement implications.
5. The J45 Category: A Family of Asthma Codes
The J45 category is where specificity begins to take shape. It is subdivided to capture the type and status of a patient’s asthma.
The Fourth Digit: Specifying the Type
The character immediately following “J45” (the fourth character) defines the predominant type of asthma.
-
J45.2-: Mild intermittent asthma Symptoms occur ≤2 days per week and ≤2 nights per month.
-
J45.3-: Mild persistent asthma Symptoms >2 days/week but not daily, and 3-4 nights/month.
-
J45.4-: Moderate persistent asthma Daily symptoms and >1 night/week but not nightly.
-
J45.5-: Severe persistent asthma Symptoms throughout the day and often 7 nights/week.
-
J45.9-: Other and unspecified asthma This is the category that includes our code in focus. It is a catch-all for types that don’t fit the above or when the type is not specified.
The Fifth and Sixth Digits: Specifying the Complication
The fifth (and sometimes sixth) character specifies the current state of the asthma episode.
-
J45.XX0: Uncomplicated The asthma is present but is not currently causing acute symptoms that require intensive intervention.
-
J45.XX1: With exacerbation This indicates an acute or subacute worsening of the patient’s asthma, moving beyond their baseline symptoms and often requiring a change in medication (e.g., a burst of oral corticosteroids). It is not synonymous with status asthmaticus.
-
J45.XX2: With status asthmaticus This is a life-threatening form of asthma exacerbation that is unresponsive to standard initial bronchodilator therapy. It is a medical emergency.
Therefore, a code like J45.21 would mean “Mild intermittent asthma with exacerbation.” This level of detail is powerful.
6. J45.909: Asthma, Unspecified, Uncomplicated – The Code in Focus
Now we arrive at the heart of our discussion: J45.909. Let’s break it down character by character:
-
J: Chapter X, Diseases of the Respiratory System
-
45: The block for Asthma
-
.9: The fourth digit, indicating “Other and unspecified asthma”
-
0: The fifth digit, indicating the specific type is “unspecified”
-
9: The sixth digit, indicating the state is “uncomplicated”
Official Code Description: Asthma, unspecified, uncomplicated.
When is this code applicable? Per the ICD-10-CM Official Guidelines for Coding and Reporting and the Tabular List, this code should be used when:
-
The provider documents a diagnosis of “asthma” without any further specification regarding its type (e.g., mild intermittent, allergic, etc.).
-
The patient is presenting for a routine encounter for asthma (e.g., a follow-up visit, medication refill) and is not experiencing an exacerbation or status asthmaticus.
-
The asthma is not stated to be due to another underlying condition (e.g., allergic asthma would be coded to a more specific code if the allergen is known).
It is, by design, a non-specific code. Its purpose is to serve as a placeholder when more detailed clinical information is not available or has not been documented by the treating provider.
7. Clinical Scenarios: When to Use J45.909 (And When Not To)
Understanding the application of this code is best achieved through real-world examples.
Scenario 1: Appropriate Use of J45.909
A 35-year-old established patient presents for a annual physical. Their problem list includes “Asthma.” They report that their symptoms have been well-controlled on their daily low-dose inhaled corticosteroid. They use their rescue inhaler less than once a week and have had no nighttime awakenings. The physician’s assessment is “Asthma, stable and well-controlled.”
-
Coding Rationale: The type of asthma is not specified in the documentation (e.g., it’s not labeled as mild persistent). The patient is not experiencing an exacerbation. This is a routine, uncomplicated encounter for asthma.
-
Correct Code: J45.909
Scenario 2: Inappropriate Use of J45.909 (A More Specific Code is Available)
A 10-year-old patient is seen by their pediatrician for a new patient visit. The mother states the child has a history of “asthma that acts up during spring and fall allergy season and when he runs around at soccer practice.” The pediatrician’s assessment is “Allergic asthma and exercise-induced bronchospasm, currently stable.”
-
Coding Rationale: The provider has specified the type: it is allergic and related to exercise. Using J45.909 would be incorrect and would result in a loss of clinical data specificity.
-
Correct Codes: J45.990 (Other asthma, uncomplicated) would be more accurate than J45.909, but even better would be to use a combination code if the specific allergen is known (e.g., J45.909 is not the right choice here). The documentation of “allergic” triggers the need for a more specific code from the J45.9- family.
Scenario 3: Inappropriate Use of J45.909 (An Exacerbation is Present)
A 50-year-old patient presents to the urgent care center with increased shortness of breath, wheezing, and chest tightness for the past 24 hours. They have a history of asthma and report their rescue inhaler is not helping. The physician documents “Asthma exacerbation” and presents a course of oral prednisone.
-
Coding Rationale: The patient is clearly experiencing an acute exacerbation. Using the “uncomplicated” fifth digit is factually incorrect.
-
Correct Code: J45.901 (Asthma, unspecified, with exacerbation)
The following table summarizes key coding scenarios and the appropriate code selection.
ICD-10-CM Asthma Code Selection Guide
| Clinical Scenario | Provider Documentation Example | Appropriate ICD-10-CM Code | Rationale |
|---|---|---|---|
| Routine follow-up, stable asthma | “Asthma, stable.” “Asthma, follow-up.” | J45.909 | Type is unspecified and the state is uncomplicated. |
| New diagnosis, type not yet determined | “Patient presents with wheezing, likely new asthma.” | J45.909 | A default code for an initial encounter when more detail is not available. |
| Acute worsening of symptoms | “Asthma exacerbation.” “Acute asthma attack.” | J45.901 | The presence of an exacerbation requires the fifth digit ‘1’. |
| Life-threatening emergency | “Status asthmaticus.” | J45.902 | A medical emergency distinct from a standard exacerbation. |
| Asthma with a stated type | “Mild persistent asthma, stable.” | J45.40 | The specific type (mild persistent) is documented, moving it out of the “unspecified” (J45.9-) category. |
| Allergic asthma | “Allergic asthma triggered by pollen.” | J45.990 | The documentation specifies “allergic,” which falls under the “other asthma” (J45.99-) category. |
8. The Critical Importance of Specificity in Medical Coding
Relying on “unspecified” codes like J45.909 is sometimes necessary, but making a habit of it has significant downsides.
-
Loss of Clinical Data Granularity: Healthcare data is used for research, public health tracking, and quality improvement. If a large percentage of asthma patients are coded as “unspecified,” it becomes impossible to analyze trends in severe persistent asthma versus mild intermittent asthma. This “data noise” hinders our ability to understand the disease on a population level.
-
Impaired Patient Care: In an ideal world, a patient’s EHR would instantly flag those with severe persistent asthma for more intensive management programs. Overuse of unspecified codes cripples these advanced clinical decision support tools, potentially leading to gaps in care.
-
Quality Reporting and Value-Based Care: Medicare, Medicaid, and private insurers increasingly tie reimbursement to quality metrics (Value-Based Purchasing, MIPS). Specific coding is essential for accurately reporting on these quality measures. An unspecified code may not satisfy the requirements of a measure designed to track outcomes for patients with moderate-to-severe asthma.
-
Compliance and Audit Risk: While J45.909 is a valid code, its persistent use without clinical justification can be a red flag for auditors. If a medical record review reveals that the provider consistently documents “asthma” without further detail, it may be seen as a pattern of poor documentation, which could lead to claim denials or even allegations of fraud.
9. The Financial and Reimbursement Impact of J45.909
Coding directly influences the financial health of a medical practice. Different codes can lead to vastly different reimbursement outcomes.
-
Hierarchical Condition Categories (HCCs): This is perhaps the most significant financial impact. HCCs are a risk-adjustment model used by CMS to predict future healthcare costs for patients. Patients with more severe chronic conditions are expected to cost more, so Medicare Advantage plans receive higher capitated payments for them.
-
A specific asthma code like J45.40 (Moderate persistent asthma, uncomplicated) is mapped to an HCC and adds risk-adjusted revenue.
-
An unspecified code like J45.909 is typically NOT mapped to a risk-adjusting HCC. It is considered a “trivial” or low-impact condition that does not significantly predict higher costs. Using J45.909 instead of a more specific code for a patient with significant asthma means the practice is leaving risk-adjusted revenue on the table—revenue that is intended to fund the care of that sicker patient.
-
-
Medical Necessity: For certain procedures (e.g., pulmonary function testing, allergy testing, advanced biologic medications), insurers require a specific diagnosis to establish medical necessity. A claim for a expensive biologic drug like omalizumab (Xolair) submitted with J45.909 will almost certainly be denied, as the policy likely requires a diagnosis of “moderate to severe persistent allergic asthma.” The unspecified code fails to justify the need for the service.
10. Documentation is Key: What Providers Need to Note
The burden of moving away from unspecified codes falls squarely on the shoulders of the healthcare provider and their documentation. A coder can only assign a code based on what is documented; they cannot assume or infer clinical details.
Best Practices for Provider Documentation:
-
Be Specific: Instead of “asthma,” document the type if known: “mild persistent allergic asthma,” “exercise-induced bronchospasm,” “severe persistent asthma.”
-
State the Status: Clearly note if the asthma is “stable,” “well-controlled,” “poorly controlled,” “not well-controlled,” experiencing an “exacerbation,” or if the patient is in “status asthmaticus.”
-
Note Triggers: Document known triggers (e.g., “viral URI induced,” “allergic trigger,” “occupational exposure”).
-
Link to Symptoms and Findings: Connect the diagnosis to the patient’s subjective complaints and objective findings (e.g., “wheezing on auscultation consistent with known asthma,” “patient reports increased SOB and cough, indicating an exacerbation”).
-
Update the Problem List: Ensure the patient’s problem list in the EHR is accurate and reflects the current type and severity of their asthma.
With this level of documentation, a coder can confidently assign a precise code like J45.41 (Moderate persistent asthma with exacerbation) or J45.52 (Severe persistent asthma with status asthmaticus), capturing the true clinical picture and ensuring appropriate data use and reimbursement.
11. The Future of Coding: A Glimpse into ICD-11
The World Health Organization released the ICD-11 in 2019, and it represents a significant modernization of the classification system. While the US is not expected to transition to ICD-11-CM for several years, understanding its structure is forward-thinking.
In ICD-11, asthma is found under code CA23. The structure allows for even greater specificity through the use of extension codes and clusters.
-
CA23.0: Allergic asthma
-
CA23.1: Non-allergic asthma
-
CA23.2: Mixed asthma
-
CA23.Z: Asthma, unspecified
The coding system also allows for adding codes for severity (mild, moderate, severe), the presence of an exacerbation, and for specific phenotypes (e.g., eosinophilic asthma, aspirin-exacerbated respiratory disease). This move towards even greater granularity underscores the industry-wide shift away from unspecified codes and toward precision medicine. The habits formed today in using ICD-10-CM specificity will ease the eventual transition to ICD-11.
12. Conclusion: Mastering the Nuances for Better Patient Care
The ICD-10 code J45.909, “Asthma, unspecified, uncomplicated,” is a vital and necessary tool in the healthcare coding arsenal, serving as a default when specific information is unavailable. However, its habitual use represents a missed opportunity on multiple fronts. It diminishes the richness of clinical data, hinders population health initiatives, introduces audit risk, and, crucially, results in significant financial under-reimbursement in value-based care models. The path forward requires a collaborative effort where providers commit to detailed, specific documentation that captures the true complexity of a patient’s asthma, and coders are empowered to translate that documentation into the most precise code possible. By mastering the nuances of this single code, we take a critical step toward more accurate data, more sustainable healthcare economics, and ultimately, better-informed care for every patient living with asthma.
13. Frequently Asked Questions (FAQs)
Q1: Is it ever required to use J45.909?
A: It is required when the provider’s documentation does not specify the type of asthma (e.g., intermittent, persistent) or the current state (e.g., exacerbation). Coders must assign codes based solely on the documentation provided.
Q2: What is the difference between an exacerbation (J45.901) and status asthmaticus (J45.902)?
A: An exacerbation is a worsening of asthma symptoms that requires a change in treatment but responds to standard therapy (e.g., increased use of rescue inhaler, course of oral steroids). Status asthmaticus is a severe, life-threatening exacerbation that does not respond to standard emergency department treatment within 30-60 minutes and requires more intensive, prolonged care, often in an ICU setting.
Q3: Can I code both asthma and COPD for the same patient?
A: Yes. A patient can have both conditions, which is often referred to as Asthma-COPD Overlap (ACO) or syndrome (ACOS). In ICD-10-CM, you would assign both a code from J44.- (COPD) and a code from J45.- (Asthma). There is a specific code, J44.9 (COPD, unspecified), that excludes asthma, so using both is necessary when both are documented.
Q4: Why would my claim get denied if I use J45.909?
A: It’s unlikely to be denied for being an invalid code. However, it could be denied for medical necessity if the service you are billing for (e.g., a complex pulmonary test or a specific biologic drug) requires a more severe or specific diagnosis code to be considered medically necessary under the payer’s policy.
Q5: How can I improve my documentation to avoid unspecified codes?
A: Make it a habit to specify:
-
Type: “mild intermittent,” “moderate persistent,” “allergic,” “exercise-induced.”
-
Control: “well-controlled,” “not well-controlled.”
-
Status: “stable,” “in exacerbation.”
Simply adding one of these descriptors allows for accurate, specific coding.
14. Additional Resources
-
CDC ICD-10-CM Official Guidelines: https://www.cdc.gov/nchs/icd/icd-10-cm.htm (The definitive source for coding rules.)
-
American Academy of Professional Coders (AAPC): https://www.aapc.com/ (Offers certifications, training, and resources for medical coders.)
-
American Health Information Management Association (AHIMA): https://www.ahima.org/ (A leading authority on health information management.)
-
Global Initiative for Asthma (GINA): https://ginasthma.org/ (Provides globally recognized guidelines for asthma management and classification, which inform clinical documentation.)
-
National Heart, Lung, and Blood Institute (NHLBI) – Asthma Guidelines: https://www.nhlbi.nih.gov/health-topics/asthma-management-guidelines-2020-update (Evidence-based clinical guidelines.)
Date: September 20, 2025
Author: The Health Informatics Team
Disclaimer: The information contained in this article is intended for educational and informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition or treatment, and before undertaking a new health care regimen. Never disregard professional medical advice or delay in seeking it because of something you have read in this article. The author and publisher are not responsible for any errors or omissions or for any consequences from the application of the information provided.






