In the intricate theater of abdominal surgery, particularly within the delicate confines of the hepatobiliary system, precision is paramount. Surgeons navigate a complex landscape of ducts, vessels, and organs where millimeters matter and anatomical variations are common. It is within this high-stakes environment that the intraoperative cholangiogram (IOC) emerges not merely as a diagnostic test, but as a crucial navigational tool, a decision-making compass that guides the surgeon’s hands and protects the patient from potential harm. For the medical coder, the IOC represents a similar challenge: a procedure that appears straightforward on the surface but, upon closer inspection, demands a precise understanding of anatomy, surgical technique, and the nuanced structure of the ICD-10-PCS coding system. Accurate coding for an IOC is not a clerical afterthought; it is a critical function that ensures appropriate reimbursement, supports quality data reporting, and reflects the true complexity of the surgical care provided. This article aims to be the definitive resource, transforming the coding of an intraoperative cholangiogram from a task of simple look-up to an exercise in professional mastery.
ICD-10-PCS Code for the Intraoperative Cholangiogram
2. Decoding the Anatomy: The Biliary Tree in Focus
Before a single code can be assigned, a foundational knowledge of the relevant anatomy is non-negotiable. The biliary tree is the system of ducts responsible for transporting bile from the liver, where it is produced, to the duodenum, where it aids in digestion.
-
Liver: The factory. Hepatocytes produce bile.
-
Canaliculi: Tiny ducts within the liver that collect bile.
-
Right and Left Hepatic Ducts: These merge just outside the liver to form the…
-
Common Hepatic Duct: This is the first major conduit.
-
Cystic Duct: The duct that connects the gallbladder to the common hepatic duct.
-
Common Bile Duct (CBD): Formed by the union of the common hepatic duct and the cystic duct. This is the main “superhighway” carrying bile to the intestine.
-
Ampulla of Vater: The point where the common bile duct and pancreatic duct join and empty into the…
-
Duodenum: The first part of the small intestine.
Why this anatomy matters for coding: The entire procedure of an IOC centers on visualizing these ducts. The contrast dye is injected into the cystic duct (most commonly) or sometimes directly into the common bile duct, and it flows through this network. The specific body part values in ICD-10-PCS correspond directly to these anatomical structures. Misidentifying the structure being visualized is a primary source of coding error.
3. The Intraoperative Cholangiogram (IOC) Defined: Purpose, Indications, and Technique
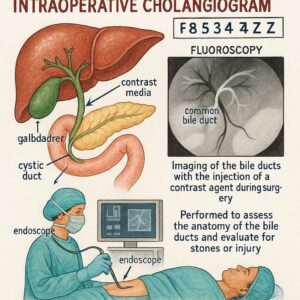
An intraoperative cholangiogram is a radiographic procedure performed during surgery to visualize the biliary ducts. It is most commonly associated with cholecystectomy (gallbladder removal) but can be used in other biliary operations.
Primary Purposes:
-
Anatomical Road Map: To define the anatomy of the biliary tree, identifying the precise location of the cystic duct–common bile duct junction and ruling out anatomical variations that could predispose to injury.
-
Detect Choledocholithiasis: To identify stones within the common bile duct that were not detected preoperatively.
-
Assess for Injury: To confirm the integrity of the biliary tree both before and after dissection, ensuring no iatrogenic damage has occurred.
-
Evaluate for Obstruction: To identify strictures, tumors, or other causes of biliary obstruction.
Standard Technique:
-
Access: The cystic duct is isolated and clamped near the gallbladder.
-
Cannulation: A small incision is made in the cystic duct, and a catheter (e.g., a ureteral catheter or a specialized cholangiocatheter) is inserted and secured.
-
Injection: Water-soluble contrast medium is injected through the catheter under live X-ray (fluoroscopy).
-
Imaging: A series of X-ray images are taken as the contrast fills the ducts, flowing from the cystic duct into the common bile duct and, ideally, freely into the duodenum.
-
Interpretation: The surgeon reviews the real-time fluoroscopic images to assess for filling defects (stones), narrowing (strictures), or leakage (injury).
4. Introduction to ICD-10-PCS: The Framework of Precision
ICD-10-PCS (International Classification of Diseases, Tenth Revision, Procedure Coding System) is a multi-axial, alphanumeric system used to report inpatient procedures. Its structure is built on seven characters, each representing a specific aspect of the procedure. Understanding this structure is the key to building a correct code.
-
Character 1: Section – The broad category (e.g., Medical and Surgical, Imaging, Measurement).
-
Character 2: Body System – The general body system (e.g., Heart, Lower Gastrointestinal).
-
Character 3: Root Operation – The objective of the procedure (e.g., Excision, Inspection, Plain Radiography).
-
Character 4: Body Part – The specific part of the body system on which the procedure was performed.
-
Character 5: Approach – The technique used to reach the site (e.g., Open, Percutaneous).
-
Character 6: Device – Any device that remains after the procedure.
-
Character 7: Qualifier – An additional attribute that specifies the procedure further.
For an IOC, we are working exclusively within the Imaging Section (B).
5. Deconstructing the ICD-10-PCS Code for a Standard Intraoperative Cholangiogram
Let us build the code for a typical IOC step-by-step.
5.1. Section: B – Imaging
This is the foundational character. An IOC is a diagnostic imaging procedure, so it falls squarely into this section.
5.2. Body System: 4 – Hepatobiliary System and Pancreas
The biliary ducts are part of the hepatobiliary system. This character correctly locates the procedure within the body.
5.3. Root Operation: 2 – Plain Radiography
This is the most critical and often misunderstood character. The ICD-10-PCS definition of Plain Radiography is: “Taking a single or multiple static view(s) of a body part using electromagnetic radiation.” While fluoroscopy (real-time, dynamic imaging) is used to perform the procedure, the definitive, billable product of an IOC is the series of static radiographic images (or “spot films”) that are captured and saved to the patient’s record for interpretation. Therefore, the root operation is “Plain Radiography,” not “Fluoroscopy.”
5.4. Body Part: Common Hepatic Duct, Hepatic Ducts, and Common Bile Duct
This character specifies the anatomy being visualized. The contrast dye injected into the cystic duct flows into and opacifies the common hepatic duct, the hepatic ducts, and the common bile duct. ICD-10-PCS groups these structures under a single body part value: Common Hepatic Duct, Hepatic Ducts, and Common Bile Duct. There is no separate, more specific body part for the “cystic duct” or “biliary tree” as a whole.
5.5. Contrast: 0 – High Osmolar vs. 1 – Low Osmolar
This character indicates the use of a contrast agent. The documentation must be reviewed to determine the type of contrast used.
-
0 – High Osmolar: An older type of contrast agent.
-
1 – Low Osmolar: A newer, more commonly used type that has a lower risk of adverse reactions.
If the type of contrast is not specified in the operative report, the coder would default to Y – Other Contrast. The key is that contrast is always used in an IOC, so this character will never be “Z – No Contrast.”
5.6. Qualifier: Z – No Qualifier
For this specific procedure, there is no further specification required, so the qualifier is “Z.”
The Complete Code:
Putting it all together, the standard ICD-10-PCS code for an intraoperative cholangiogram is:
B422ZZZ (if using High Osmolar contrast, unspecified, or if the type is not documented and the facility uses Y for unspecified)
B4221ZZ (if specifically using Low Osmolar contrast)
ICD-10-PCS Character Value Breakdown for Intraoperative Cholangiogram
| Character Position | Character Value | Description | Rationale |
|---|---|---|---|
| 1 – Section | B | Imaging | The IOC is a diagnostic imaging procedure. |
| 2 – Body System | 4 | Hepatobiliary System and Pancreas | The biliary ducts are part of this system. |
| 3 – Root Operation | 2 | Plain Radiography | The procedure results in static radiographic images for interpretation. |
| 4 – Body Part | 2 | Common Hepatic Duct, Hepatic Ducts, and Common Bile Duct | This is the specific anatomical structure being visualized. |
| 5 – Approach | Z | No Approach | The “Approach” axis does not apply to the Imaging section. It is always “Z”. |
| 6 – Device | Z | No Device | No device remains after the imaging is complete. |
| 7 – Qualifier | Z | No Qualifier | No further specification is needed for this procedure. |
6. Common Clinical Scenarios and Coding Nuances
6.1. IOC During Laparoscopic Cholecystectomy
This is the most frequent context for an IOC. The coding remains exactly as described above. The fact that the surgery is laparoscopic does not change the Imaging code. The cholecystectomy itself would be coded separately from the Medical and Surgical section (e.g., 0FT44ZZ for laparoscopic removal of the gallbladder).
6.2. IOC During Open Cholecystectomy
The same principle applies. The IOC code (B4221ZZ) is assigned in addition to the code for the open cholecystectomy (0FT40ZZ).
6.3. The Abnormal IOC: Stones, Strictures, and Spasm
The IOC code itself does not change based on the findings. A normal cholangiogram and an abnormal one showing a stone are both coded as B4221ZZ. The diagnosis codes (from ICD-10-CM) will reflect the findings (e.g., K80.55 for calculus of bile duct without mention of cholecystitis). If the abnormal finding leads to an immediate additional procedure, that procedure must be coded separately.
7. Advanced Coding Challenges: When the Procedure Becomes More Complex
7.1. From Imaging to Intervention: Coding Subsequent Procedures
This is a critical area for coders. If the IOC reveals a stone in the common bile duct, the surgeon will typically proceed with a common bile duct exploration (CBDE).
-
Scenario: Laparoscopic Cholecystectomy with IOC, followed by Laparoscopic Common Bile Duct Exploration with stone removal.
-
Coding:
-
Cholecystectomy: 0FT44ZZ
-
IOC: B4221ZZ
-
CBDE with Stone Removal: This requires a code from the Medical and Surgical section. The root operation would be Extraction (pulling out a foreign body) from the Common Bile Duct. The approach would be laparoscopic. A possible code would be 0FD48ZZ (Extraction from Common Bile Duct, Via Natural or Artificial Opening Endoscopic). It is vital to code all distinct procedures performed.
-
7.2. The Failed or Incomplete Cholangiogram
If the surgeon attempts an IOC but is unable to cannulate the cystic duct or the contrast does not flow properly and no diagnostic images are obtained, the question arises: is it codeable? The general principle is that a procedure is coded only if it is completed. An attempted but aborted procedure, where the objective was not achieved, is typically not coded. However, if the surgeon’s note clearly documents the attempt and the effort involved (e.g., “multiple attempts at cystic duct cannulation were unsuccessful”), some coding professionals, following the AHA Coding Clinic advice on similar scenarios, advise that it may be coded. The coder must rely on the facility’s policy and the specificity of the documentation.
7.3. Biliary Endoscopy (Choledochoscopy) in Conjunction with IOC
A choledochoscopy involves inserting a small flexible endoscope directly into the common bile duct to visualize its interior. This is a different procedure from an IOC.
-
IOC: External, radiographic imaging.
-
Choledochoscopy: Internal, direct visual inspection.
If both are performed, both are coded. -
IOC: B4221ZZ (Imaging)
-
Choledochoscopy: 0WJG4ZZ (Inspection of Biliary Tract, Via Natural or Artificial Opening Endoscopic)
8. The Coder’s Workflow: A Step-by-Step Approach to Accurate Code Assignment
-
Identify the Procedure: Locate the clear statement in the operative report: “Intraoperative cholangiogram was performed.”
-
Review the Technique: Confirm the steps: cystic duct cannulation, injection of contrast, taking of X-ray images.
-
Determine the Anatomy: Verify that the ducts visualized are the common hepatic and common bile ducts.
-
Note the Contrast: Check the “Materials Used” or narrative portion of the report for the type of contrast.
-
Build the ICD-10-PCS Code:
-
Section: B
-
Body System: 4
-
Root Operation: 2
-
Body Part: 2
-
Approach: Z
-
Device: Z
-
Qualifier: Z
-
Add the Contrast character (0, 1, or Y).
-
-
Code Associated Procedures: Check for and code any subsequent procedures like CBD exploration or choledochoscopy.
-
Assign Diagnosis Codes: Code the findings from the IOC (e.g., choledocholithiasis) and the reason for the surgery (e.g., cholelithiasis).
9. Documentation Requirements: Bridging the Gap Between Surgeon and Coder
Clear documentation is the coder’s lifeline. The ideal operative report for an IOC should include:
-
Indication: Why the IOC was performed (e.g., “routine,” “elevated LFTs,” “dilated CBD on ultrasound”).
-
Technique: “The cystic duct was isolated, clipped distally, and a small ductotomy was made. A 5-Fr ureteral catheter was introduced and secured.”
-
Contrast: “Approximately 10cc of Isovue-300 (low osmolar contrast) was injected under fluoroscopic guidance.”
-
Findings: “The cholangiogram showed free flow of contrast into the duodenum. No filling defects were seen. The biliary anatomy appeared normal.” OR “The cholangiogram revealed a 5mm filling defect in the distal CBD consistent with a stone.”
10. Compliance and Reimbursement: Ensuring Accuracy in a High-Stakes Environment
Incorrect coding of an IOC can lead to:
-
Underpayment: Failing to code the IOC separately when it is a distinct and separately identifiable procedure.
-
Overpayment/Compliance Risk: Coding an IOC when it was not performed or was part of a bundled payment arrangement.
-
Data Integrity Issues: Skewing hospital data on the frequency and complexity of procedures performed.
Coders must be vigilant and code to the highest level of specificity based on the documentation provided.
11. Conclusion
The intraoperative cholangiogram is a vital surgical adjunct that demands an equally precise approach from the medical coder. By mastering the underlying anatomy, the technical details of the procedure, and the logical structure of ICD-10-PCS, coders can move beyond simple data entry to become integral partners in the healthcare revenue cycle. Accurate code assignment for the IOC ensures that the full scope of surgical care is captured, supporting both financial integrity and the quality of patient data.
12. Frequently Asked Questions (FAQs)
Q1: If the surgeon only uses fluoroscopy and doesn’t save any static images, can I still code an IOC?
A: This is a complex area. The official definition of “Plain Radiography” requires the taking of static images. If the surgeon documents an interpretation based solely on real-time fluoroscopy without saved images, many experts would argue it is not codeable as B4221ZZ. The facility should establish a clear policy on this scenario, but the safest practice is to require documentation of saved images.
Q2: What is the ICD-10-PCS code for a percutaneous transhepatic cholangiogram (PTC)?
A: A PTC is a different procedure with a different approach. The code would be B4121ZZ (Plain Radiography of Hepatobiliary System, Low Osmolar Contrast). The key difference is the Body System character is “1” for the entire Hepatobiliary System, as the PTC involves a different access point and visualization technique.
Q3: How do I code an IOC if the surgeon injects the contrast directly into the common bile duct instead of the cystic duct?
A: The body part value remains the same: “Common Hepatic Duct, Hepatic Ducts, and Common Bile Duct.” The anatomy being visualized is identical. The code would still be B4221ZZ. The approach for the injection does not affect the Imaging code.
Q4: Is the IOC always separately payable when performed with a cholecystectomy?
A: Not necessarily. Payment is determined by payer policies, including National Correct Coding Initiative (NCCI) edits. While the IOC is a separately codeable procedure, some payers may bundle it with the primary surgery. The coder’s responsibility is to assign the code accurately based on documentation; the billing office then applies payer-specific rules.
Date: November 29, 2025
Author: The Healthcare Coding Insights Team
Disclaimer: The information contained in this article is for educational and informational purposes only and does not constitute medical or professional coding advice. Code assignment must be based on the complete clinical documentation in the patient’s medical record, official ICD-10-PCS guidelines, and payer-specific policies. The authors and publishers are not responsible for any claims, losses, or damages arising from the use of this information.






