Imagine a fundamental force that governs every heartbeat, every neural impulse, and every cellular contraction. This force is not a mysterious energy but a simple, positively charged atom: the potassium ion. Within the intricate symphony of human physiology, potassium plays a lead role, maintaining the electrical gradient across cell membranes that is essential for life itself. When the concentration of this vital electrolyte falls below a critical threshold, a condition known as hypokalemia emerges. Hypokalemia is often a “silent” imbalance in its early stages, masquerading as generalized fatigue or muscle weakness, but its potential consequences are profound and can be life-threatening, culminating in cardiac arrhythmias, respiratory paralysis, and death.
In the modern healthcare ecosystem, the clinical management of a condition is only one part of the story. The parallel narrative is told through data—specifically, through the alphanumeric codes that capture every diagnosis, procedure, and resource consumed. For medical coders, physicians, and healthcare administrators, navigating the complex world of medical coding is a critical task that impacts patient care, reimbursement, and health data analytics. At the heart of this system for inpatient procedures in the United States is the International Classification of Diseases, Tenth Revision, Procedure Coding System (ICD-10-PCS). This is where a unique challenge arises: Hypokalemia, as a diagnosis, has no direct corresponding procedure code in ICD-10-PCS.
This article aims to be the definitive guide for unraveling this paradox. We will embark on a detailed exploration of why a common and serious condition like hypokalemia does not have a “fix hypokalemia” code. We will dive deep into the structure and philosophy of ICD-10-PCS to illuminate the correct way to code the procedures performed to diagnose, monitor, and treat this electrolyte disturbance. Through comprehensive explanations, detailed tables, and real-world clinical scenarios, this article will equip you with the knowledge to accurately and confidently code the procedural care surrounding hypokalemia, ensuring data integrity, appropriate reimbursement, and a true reflection of the clinical services provided.
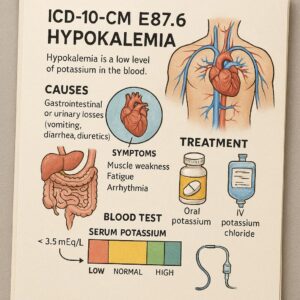
ICD-10-PCS Code of Hypokalemia
2. Understanding the Foundations: ICD-10-CM vs. ICD-10-PCS
To understand the coding of hypokalemia, one must first grasp the fundamental distinction between the two primary coding systems used in the U.S.
ICD-10-CM (International Classification of Diseases, Tenth Revision, Clinical Modification)
-
Purpose: Used to report diagnoses, symptoms, and reasons for encounters in all healthcare settings.
-
Focus: The “what” – What is wrong with the patient?
-
Structure: Alphanumeric codes, usually 3-7 characters long. The codes are based on chapters organized by disease etiology or body system.
-
Example for Hypokalemia: E87.6 – Hypokalemia. This code precisely identifies the diagnosed condition.
ICD-10-PCS (International Classification of Diseases, Tenth Revision, Procedure Coding System)
-
Purpose: Used to report procedures performed during inpatient hospital stays.
-
Focus: The “how” – What did the healthcare provider do to the patient?
-
Structure: Always an alphanumeric code of seven characters. Each character has a specific meaning within a defined table, providing a high level of specificity.
-
Key Philosophy: ICD-10-PCS codes represent objective procedures, not the diagnoses they are intended to treat. There is no code for “treating hypokalemia,” only codes for the specific actions taken, such as “administering intravenous potassium” or “measuring serum potassium levels.”
The following table illustrates the core differences:
ICD-10-CM vs. ICD-10-PCS at a Glance
| Feature | ICD-10-CM | ICD-10-PCS |
|---|---|---|
| Full Name | International Classification of Diseases, 10th Revision, Clinical Modification | International Classification of Diseases, 10th Revision, Procedure Coding System |
| Primary Use | Diagnoses, symptoms, reasons for encounter | Inpatient procedures |
| Setting | All healthcare settings (outpatient, inpatient, physician office) | Inpatient hospital admissions only |
| Code Structure | 3-7 characters, mostly decimal-based | Always 7 characters, each with a specific meaning |
| What it Answers | “What is the patient’s condition?” | “What procedure was performed on the patient?” |
| Example for a Patient with Low Potassium | E87.6 – Hypokalemia | 3E033GC – Introduction of Potassium Chloride into Peripheral Vein, Percutaneous Approach |
This distinction is the cornerstone of accurate medical coding. Confusing the two systems is a primary source of error.
3. Hypokalemia Unpacked: Pathophysiology, Causes, and Clinical Presentation
Before delving into coding, a firm clinical understanding is essential. Potassium (K+) is the primary intracellular cation. The steep concentration gradient between the intracellular and extracellular fluid (about 140 mEq/L inside vs. 3.5-5.0 mEq/L outside) is critical for the resting membrane potential of cells, particularly nerve and muscle cells.
Pathophysiology: Hypokalemia is defined as a serum potassium level below 3.5 mEq/L. Its effects are widespread:
-
Neuromuscular: Weakness, cramping, paralysis, and hyporeflexia due to hyperpolarization of cell membranes.
-
Cardiac: Characteristic ECG changes (flattened T waves, prominent U waves, ST depression) and heightened risk of serious arrhythmias like ventricular tachycardia and fibrillation.
-
Renal: Impaired concentrating ability leading to polyuria and polydipsia.
-
Metabolic: Can contribute to glucose intolerance.
Etiology (Causes): The causes of hypokalemia are broadly categorized into three groups:
-
Inadequate Intake: Rarely the sole cause, but can be a contributing factor, especially in malnutrition or eating disorders.
-
Transcellular Shifts: Potassium moves from the extracellular fluid into the cells. This can be caused by alkalosis, insulin administration, beta-adrenergic agonists (e.g., albuterol), or thyrotoxicosis.
-
Increased Losses: This is the most common mechanism.
-
Renal Losses: Diuretics (especially loop and thiazides), hyperaldosteronism, renal tubular acidosis, magnesium deficiency, and high-dose penicillin.
-
Gastrointestinal Losses: Vomiting, diarrhea, laxative abuse, and fistulas.
-
Clinical Presentation: Symptoms often correlate with the severity of the deficiency. Mild hypokalemia (3.0-3.5 mEq/L) may be asymptomatic. Moderate to severe hypokalemia (<3.0 mEq/L) presents with muscle weakness, fatigue, and constipation. Severe cases can lead to paralysis, rhabdomyolysis, and life-threatening cardiac arrhythmias.
4. The Core Principle: Why Hypokalemia Itself Has No ICD-10-PCS Code
This is the central tenet of this article. ICD-10-PCS is not a dictionary of diagnoses or intended outcomes. It is a catalog of actions. You cannot perform a “hypokalemia-ectomy.” Therefore, there is no procedure code that means “treatment of hypokalemia.”
The procedural coding is derived from the specific interventions the clinical team undertakes to correct the imbalance. These interventions fall into several key ICD-10-PCS sections, primarily Administration and Measurement and Monitoring. The coder must look to the physician’s orders, nursing notes, and medication administration records to identify what was done, not what was treated.
5. The Procedural Landscape: Coding the Treatment of Hypokalemia
Let’s explore the primary ICD-10-PCS sections relevant to managing a patient with hypokalemia.
5.1. Section 3: Administration
This section is used for procedures where a substance is introduced into or onto the body. It is the most common section for coding the definitive treatment of hypokalemia: potassium replacement.
The 7 characters in a Section 3 code are:
-
Section: 3 (Administration)
-
Body System: A (Circulatory) for intravenous administration, or 7 (Central Nervous) for intrathecal, etc. For IV potassium, it’s almost always A.
-
Root Operation:
-
Introduction: Putting in or on a therapeutic, diagnostic, nutritional, physiological, or prophylactic substance except blood or blood products. This is used for IV potassium.
-
Transfusion: Putting in blood or blood products.
-
-
Body Region/Type: Specifies the vein type.
-
3 – Peripheral Vein
-
4 – Central Vein
-
0 – Vein (unspecified)
-
-
Approach:
-
3 – Percutaneous
-
E – Via natural or artificial opening (not typical for IV admin)
-
-
Substance: This is the critical character for identifying what was administered.
-
G – Electrolytic (e.g., Potassium Chloride, Sodium Chloride)
-
H – Anti-infective
-
J – Analgesics, etc.
-
-
Qualifier: For “Introduction” of an “Electrolytic” substance, this character specifies the exact electrolyte.
-
C – Potassium
-
D – Sodium
-
F – Magnesium, etc.
-
Building the Code for IV Potassium Chloride:
A patient receives an IV infusion of potassium chloride through a peripheral IV line (percutaneous approach).
-
3 – Section: Administration
-
E – Body System: Circulatory
-
0 – Root Operation: Introduction
-
3 – Body Region: Peripheral Vein
-
3 – Approach: Percutaneous
-
G – Substance: Electrolytic
-
C – Qualifier: Potassium
Final Code: 3E033GC – Introduction of Potassium Chloride into Peripheral Vein, Percutaneous Approach
If the same infusion was given through a central line (e.g., a PICC line), the code would be 3E043GC (Body Region: 4 – Central Vein).
*It is crucial to note that ICD-10-PCS requires a code for each distinct substance. If a patient receives a liter of Normal Saline with 40 mEq of KCl added, two separate administration codes are required: one for the electrolytic substance potassium (3E033GC) and one for the electrolytic substance sodium (3E033GD).*
5.2. Section 4: Measurement and Monitoring
This section covers procedures that determine the level of a physiological or chemical substance or the function of a body system. Coding the diagnostic confirmation and ongoing monitoring of hypokalemia is done here.
The 7 characters for this section are:
-
Section: 4 (Measurement and Monitoring)
-
Body System: A (Physiological systems) or B (Physiological devices). For lab tests, it’s A.
-
Root Operation:
-
Measurement: Determining the level of a physiological or chemical substance. This is used for a serum potassium lab test.
-
Monitoring: Determining the level of a physiological or chemical substance for a prolonged period.
-
-
Body System/Function: Specifies what is being measured.
-
5 – Urinary
-
8 – Circulatory
-
C – Nervous, etc. For a serum potassium, it’s 8 (Circulatory) as the potassium is measured in the blood.
-
-
Approach: 0 – Open, 3 – Percutaneous, X – External. For a blood draw, it’s X (External).
-
Function/Device:
-
For “Measurement” of a “Circulatory” substance, this character identifies the substance.
-
B – Potassium
-
A – Sodium
-
D – Chloride, etc.
-
-
Qualifier: Typically Z – No Qualifier for these measurements.
Building the Code for a Serum Potassium Test:
A phlebotomist draws blood from a patient’s vein to check the potassium level.
-
4 – Section: Measurement and Monitoring
-
A – Body System: Physiological Systems
-
1 – Root Operation: Measurement
-
8 – Body System: Circulatory
-
X – Approach: External
-
B – Function/Device: Potassium
-
Z – Qualifier: No Qualifier
Final Code: 4A018BZ – Measurement of Potassium in Circulatory System, External Approach
5.3. Section 5: Osteopathic and Other Complementary Procedures
While less common, a physician might use osteopathic manipulative treatment (OMT) to address somatic dysfunction related to a patient’s overall condition, which could include issues stemming from or contributing to metabolic stress. This would be coded from this section, but it is not a direct treatment for the low potassium itself.
6. Advanced Scenarios and Complex Cases
Real-world coding is rarely simple. Let’s apply these principles to complex patient scenarios.
6.1. Hypokalemia in the Cardiac Patient
A patient is admitted with an acute myocardial infarction and is found to have a potassium level of 2.9 mEq/L, with ECG showing ventricular ectopy.
-
Clinical Concern: The hypokalemia significantly increases the risk of lethal arrhythmias in this already vulnerable heart.
-
Procedures:
-
Administration: The patient receives a continuous IV infusion of potassium chloride via a central line. Code: 3E043GC
-
Monitoring: The patient is on a continuous cardiac monitor. Code: 4A1204Z – Monitoring of Cardiac Rhythm, External Approach
-
Measurement: Serum potassium levels are checked every 4-6 hours. Code: 4A018BZ (This code is typically reported only once per encounter for the measurement of a specific substance, regardless of the number of times it’s performed, unless a different methodology is used).
-
-
Coding Insight: The coder must capture both the aggressive replacement (administration) and the intense monitoring due to the high-risk clinical context.
6.2. The Post-Operative Patient
A patient develops hypokalemia on post-op day 1 after a major abdominal surgery, likely due to intraoperative blood loss, fluid shifts, and stress-induced hyperaldosteronism.
-
Procedures:
-
Administration: The patient receives IV potassium chloride piggybacked into a peripheral IV line. Code: 3E033GC
-
The underlying cause may also involve other procedures. If the patient is on a patient-controlled analgesia (PCA) pump delivering an opioid, that would be a separate Administration code: 3E013GC – Introduction of Other Therapeutic Substance into Peripheral Vein, Percutaneous Approach (assuming the opioid is not listed by its specific name in the table).
-
-
Coding Insight: The coder must review the entire record to ensure all administered substances are captured, not just the potassium.
7. The Crucial Link: Bridging ICD-10-CM Diagnosis Codes with PCS Procedure Codes
While PCS codes stand alone, their medical necessity is justified by the ICD-10-CM diagnosis codes. The principle is that the procedure code must be linked to a diagnosis code that explains why the procedure was necessary.
In our examples:
-
The procedure code 3E033GC (IV Potassium) is linked to the diagnosis code E87.6 (Hypokalemia).
-
The procedure code 4A018BZ (Serum Potassium Test) is also linked to E87.6.
If the hypokalemia is due to a specific cause, that cause should also be coded. For example:
-
E87.6 – Hypokalemia
-
E86.0 – Dehydration
-
K21.9 – Gastro-esophageal reflux disease with diuretic use (if applicable, with an additional code from T36-T50 with fifth or sixth character 5 to identify the drug).
This linkage is critical for creating a coherent and defensible medical record for clinical, billing, and auditing purposes.
8. A Practical Coding Workflow: From Patient Encounter to Final Code
To ensure accuracy, follow a systematic process:
-
Review the Medical Record: Start with the discharge summary, then physician notes, nursing notes, medication administration record (MAR), and lab reports.
-
Identify the Diagnoses (ICD-10-CM): Confirm the diagnosis of hypokalemia (E87.6) and any underlying causes.
-
Identify the Procedures (ICD-10-PCS):
-
Scan the MAR for “Potassium Chloride” IV infusions.
-
Check the type of access (peripheral vs. central) to determine the 4th character.
-
Review lab reports to confirm the potassium was measured.
-
Look for any continuous monitoring.
-
-
Construct the PCS Codes: Use the official ICD-10-PCS tables to build each code, character by character.
-
Link and Verify: Ensure every PCS code has a supporting diagnosis code that justifies its medical necessity. Perform a final review to check for accuracy and completeness.
9. Common Pitfalls and How to Avoid Them
-
Pitfall 1: Assigning a PCS code to the diagnosis of hypokalemia.
-
Solution: Remember, PCS is for procedures. Code the action (administration, measurement), not the condition.
-
-
Pitfall 2: Confusing the route of administration.
-
Solution: Carefully review the documentation to distinguish between peripheral (3) and central (4) venous access.
-
-
Pitfall 3: Incorrectly reporting multiple instances of the same measurement.
-
Solution: Generally, a specific measurement code (like 4A018BZ) is reported only once per encounter. However, each unique administration of a substance is coded separately. If potassium is given via three separate IV piggybacks, you would report 3E033GC three times.
-
-
Pitfall 4: Overlooking the need for separate codes for combined substances.
-
Solution: If an IV fluid contains multiple electrolytes (e.g., KCl and NaCl in the same bag), you must assign a separate Administration code for each unique electrolyte substance.
-
10. The Future of Procedural Coding: A Glimpse Beyond ICD-10-PCS
The healthcare industry is continuously evolving, and medical coding is no exception. The transition to ICD-11 is on the horizon, which includes an updated procedure coding system. While the fundamental principle of coding objective actions will remain, the structure and specificity will change. Furthermore, the increasing use of Artificial Intelligence (AI) and Natural Language Processing (NLP) will likely assist coders by automatically suggesting codes from clinical documentation, but the need for human expertise to validate, interpret, and apply clinical knowledge will remain paramount. Understanding the core concepts explained in this article will provide a strong foundation for navigating any future coding system.
11. Conclusion
Accurately coding for hypokalemia in ICD-10-PCS requires a paradigm shift from thinking about the condition to thinking about the concrete actions taken to address it. There is no procedure for hypokalemia itself; instead, coders must meticulously document the introductions of electrolytes, the measurements of serum levels, and the monitoring of physiological functions. By mastering the structure of the ICD-10-PCS tables, particularly in the Administration and Measurement sections, and by diligently linking these procedures to their justifying diagnoses, healthcare professionals can ensure the integrity of the medical record, support appropriate reimbursement, and contribute to valuable data that drives clinical quality and research forward.
12. Frequently Asked Questions (FAQs)
Q1: My patient has hypokalemia and is taking oral potassium supplements. Is there an ICD-10-PCS code for that?
A: No. ICD-10-PCS is used for inpatient hospital procedures. The administration of oral medications is not considered a procedure that is coded in the PCS system. It is considered part of the routine daily care and is captured in the medication record, but it does not get a separate procedure code.
Q2: How many times do I code 3E033GC if a patient receives a continuous IV potassium infusion over 24 hours?
A: You code it once. A continuous infusion is considered a single procedure, regardless of its duration. You would only code it multiple times if there were multiple, distinct infusions (e.g., one bag in the morning and a separate, new bag in the afternoon).
Q3: The lab report shows the potassium was measured from an arterial blood gas (ABG), not a venous sample. Does that change the code?
A: No, the code 4A018BZ is still correct. The “Body System” character “8” represents the Circulatory system as a whole, which includes both arterial and venous blood. The “Approach” is still “X” for External, as the blood is obtained via an external means (a needle stick).
Q4: What if the potassium is administered via a feeding tube (NG tube)?
A: This would be coded in the Administration section, but with a different body system and approach. The code would be 3E0G76Z – Introduction of Nutritional Substance into Gastrointestinal Tract via Natural or Artificial Opening.
Q5: Where can I find the official ICD-10-PCS guidelines and tables?
A: The complete and authoritative source is the CMS website, which publishes the official ICD-10-PCS files and guidelines annually. The AHA Coding Clinic for ICD-10-CM/PCS is the official source for coding advice and updates.
Date: November 25, 2025
Author: Medical Coding Insights Institute
Disclaimer: This article is intended for educational and informational purposes only and is based on the ICD-10-PCS coding system as of the publication date. It does not constitute professional medical coding, billing, or legal advice. Medical coders must use the most current, official ICD-10-PCS code sets and guidelines provided by the Centers for Medicare & Medicaid Services (CMS) and the American Health Information Management Association (AHIMA) for accurate coding. Always consult with a certified professional coder for specific cases.






