Navigating the world of medical coding can often feel like learning a new language. If you are a healthcare provider, a medical coder, or a practice manager, you know that precision is everything. One wrong digit on a claim can mean the difference between a clean reimbursement and a frustrating denial.
Among the many procedures that require meticulous coding, the flexible sigmoidoscopy stands out. It is a common, minimally invasive procedure used to screen for colorectal cancer and diagnose various lower gastrointestinal issues. But because it lives in a “gray area” between a simple anoscopy and a full colonoscopy, getting the CPT code for flexible sigmoidoscopy right is crucial.
In this guide, we will strip away the complexity. We will explore the 45330 series of codes, discuss the critical differences between screening and diagnostic procedures, and look at the modifiers that can make or break your claim. Whether you are a seasoned coder or just starting out, this article aims to be your go-to resource.
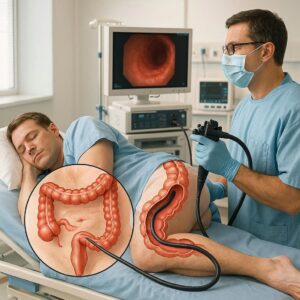
CPT Code for Flexible Sigmoidoscopy
What is a Flexible Sigmoidoscopy?
Before we dive into the numbers, let’s ensure we are all talking about the same procedure. A flexible sigmoidoscopy is an endoscopic procedure that allows a physician to examine the lining of the rectum and the lower part of the colon, specifically the sigmoid colon.
Unlike a colonoscopy, which examines the entire length of the large intestine, a sigmoidoscopy only looks at the distal portion. It is often used as a screening tool for colorectal cancer, or to investigate symptoms like rectal bleeding, chronic diarrhea, or lower abdominal pain.
The procedure typically does not require the same level of sedation as a colonoscopy, making it a quicker and often more accessible option for patients.
The Core Code Family: The 45330 Series
In the world of Current Procedural Terminology (CPT), the flexible sigmoidoscopy lives within the digestive system section. Specifically, all codes for this procedure fall under the 45330 series.
This is the most important thing to remember: The base CPT code for flexible sigmoidoscopy is 45330. However, the story doesn’t end there. The code you choose depends entirely on what the physician does during the procedure.
Here is the breakdown of the 45330 family:
| CPT Code | Procedure Description | What It Means |
|---|---|---|
| 45330 | Sigmoidoscopy, flexible; diagnostic, with or without collection of specimen(s) by brushing or washing (separate procedure) | This is the basic diagnostic scope. The doctor looks around, and maybe does some cleaning or brushing to collect cells, but nothing else. |
| 45331 | …with biopsy, single or multiple | The doctor inserts a biopsy forceps through the scope and takes tissue samples. This code includes the diagnostic scope (45330) plus the biopsy work. |
| 45332 | …with removal of foreign body | The doctor finds and removes something that shouldn’t be there (e.g., a swallowed object). |
| 45333 | …with removal of polyp(s) by snare technique | The doctor uses a wire loop (snare) to cut off polyps. This often involves cauterization to stop bleeding. |
| 45334 | …with control of bleeding (e.g., injection, bipolar cautery, unipolar cautery, laser, heater probe, stapler, plasma coagulator) | The doctor finds a source of bleeding (like an ulcer or a vessel) and stops it using various tools. |
| 45335 | …with submucosal injection | The doctor lifts a lesion or polyp off the muscle wall by injecting fluid under it. This is often a precursor to safe removal. |
| 45338 | …with removal of tumor(s), polyp(s), or other lesion(s) by hot biopsy forceps or bipolar cautery | This is different from the snare technique. The doctor uses forceps that cauterize as they grab, removing small polyps or tissue. |
| 45339 | …with ablation of tumor(s), polyp(s), or other lesion(s) (includes pre- and post-dilation and guide wire passage, when performed) | The doctor destroys the tissue using heat, laser, or other methods rather than physically cutting it out. |
| 45340 | …with dilation by balloon (e.g., balloon dilation) | The doctor inserts and inflates a balloon to open up a narrowed or strictured area in the colon. |
| 45341 | …with endoscopic ultrasound examination | The doctor uses a specialized scope with an ultrasound probe to look at the layers of the colon wall and surrounding structures. |
| 45342 | …with transendoscopic ultrasound-guided intramural or transmural fine needle aspiration/biopsy(s) | This builds on 45341. The doctor uses the ultrasound to guide a needle into a lesion or lymph node to take a sample. |
| 45346 | …with removal of polyp(s) by snare technique (screening) | Medicare-Specific: Used specifically for a screening exam where a polyp is found and removed by snare. |
| 45347 | …with removal of polyp(s) by hot biopsy forceps or bipolar cautery (screening) | Medicare-Specific: Used specifically for a screening exam where a polyp is found and removed by hot biopsy forceps. |
| 45349 | …with ablation (screening) | Medicare-Specific: Used for lesion ablation during a screening exam. |
| 45350 | …with removal of polyp(s) by use of cold forceps (screening) | Medicare-Specific: Used specifically for a screening exam where polyps are removed using cold forceps (without cautery). |
Important Note: The codes 45346, 45347, 45349, and 45350 are relatively new and were introduced to satisfy Medicare’s requirement to distinguish between diagnostic and screening procedures with intervention. Private payers may have different policies regarding their use.
Diagnostic vs. Screening: The Critical Distinction
One of the biggest sources of confusion—and subsequent claim denials—is the difference between a diagnostic and a screening flexible sigmoidoscopy.
Screening
A screening is performed on a patient without any specific symptoms. The goal is purely preventative: to catch cancer or polyps early. For example, an average-risk 55-year-old patient coming in for their routine check-up is receiving a screening.
-
Code to use initially (for the referral/order): G0104 (Medicare) or a screening Z code (e.g., Z12.11) for the diagnosis.
-
CPT for the procedure: If nothing is found, you might still use 45330, but many payers expect the screening-specific HCPCS code (G0104) for Medicare patients. For non-Medicare patients, 45330 with a screening diagnosis code is common, but you must verify the payer’s policy.
Diagnostic
A diagnostic procedure is performed because the patient has symptoms or a known condition. This could be rectal bleeding, a change in bowel habits, abdominal pain, or follow-up on a previous abnormal finding.
-
Code to use: You will use the appropriate 45330-series code based on the work performed (e.g., 45331 for a biopsy), linked to an ICD-10 code describing the symptom (e.g., K62.5 for hemorrhage of rectum).
The “Screening Turns Diagnostic” Scenario
This is where it gets tricky. What happens when a patient comes in for a routine screening, but the doctor finds a polyp or bleeding?
In the past, this was a coding nightmare. However, with the introduction of the “screening with intervention” codes (45346, 45347, 45349, 45350), the process is cleaner for Medicare. You would use these specific codes to indicate that the procedure started as a screening but required an intervention.
For private payers, you often need to append a modifier (like -PT for colorectal cancer screening; test converted to diagnostic) to the standard surgical code (e.g., 45333) to tell the story: “This started as a screening, but we had to do a therapeutic removal.”
Reader Tip: Always, always check with your specific payers. Some commercial insurers still require the diagnostic code (e.g., 45333) with a modifier, while others have adopted the new Medicare-style codes.
Key Modifiers for Flexible Sigmoidoscopy
Modifiers are two-character codes that provide additional information about the service performed. They don’t change the definition of the CPT code, but they tell the payer a crucial part of the story.
Here are the most common modifiers you will use with sigmoidoscopy codes:
-
Modifier -33 (Preventive Service): Used when the primary purpose of the service is the delivery of an evidence-based service in accordance with a US Preventive Services Task Force A or B rating. You might use this with 45330 to indicate a screening on a commercial plan.
-
Modifier -PT (Colorectal cancer screening; test converted to diagnostic): This is a Medicare-specific modifier. Use it when a screening sigmoidoscopy results in a decision to perform a biopsy or polypectomy during the same session. It helps prevent the patient from being billed for a diagnostic procedure they didn’t initially agree to, preserving their screening benefits.
-
Modifier -59 (Distinct Procedural Service): While rarely used for the scope itself, you might see this used in a surgical setting. It indicates that a procedure was distinct or independent from other services performed on the same day. For example, if a patient had a lesion in two different areas that required two different types of removal techniques, you might need this modifier, though this is uncommon in sigmoidoscopy.
-
Modifier -52 (Reduced Services): Used when a service is partially reduced or eliminated at the physician’s discretion. If the physician attempted a sigmoidoscopy but could not advance the scope past a certain point due to a blockage or severe patient discomfort, you might append modifier -52 to the code to indicate the procedure was not completed as planned.
Common Coding Mistakes and How to Avoid Them
Even experienced coders can stumble. Here are the most frequent pitfalls associated with the CPT code for flexible sigmoidoscopy:
1. Coding Based on the Order, Not the Operative Report
Never code solely from the referral paper. The referral might say “Screening sigmoidoscopy,” but the operative report might state, “Patient reported blood in stool for two weeks. Scope performed. Polyp found and removed by snare.” This is a diagnostic procedure with an intervention (45333). Always code from the physician’s final documentation.
2. Forgetting to Check the Bowel Prep
While the physician is responsible for documentation, a coder should be aware that a poorly prepped colon can impact coding. If the procedure was abandoned because of poor prep, this is not a complete sigmoidoscopy. You may need to append a modifier (like -53 for Discontinued Procedure) or use a different code, depending on what was actually done.
3. Unbundling Services
The 45330-series codes are “bundled.” This means a code like 45331 (with biopsy) includes the diagnostic look (45330) and the biopsy. You cannot bill 45330 and a separate biopsy code. The single code covers the entire encounter.
4. Incorrect Use of Screening Codes
Assuming every 50-year-old patient is getting a screening is dangerous. If a patient has a family history of colorectal cancer, they are considered high-risk. While the intent might be preventative, the presence of a personal risk factor changes the coding strategy for some payers. You must verify if the payer considers a high-risk patient’s exam a “screening” or a “diagnostic” surveillance.
Sample Scenarios and Coding Solutions
Let’s put this knowledge into practice with a few realistic scenarios.
Scenario A: The Routine Screening
-
Patient: 60-year-old, no symptoms, average risk.
-
Procedure: The physician performs a flexible sigmoidoscopy. The mucosa appears normal throughout. No biopsies or interventions are performed.
-
Operative Report Key Phrase: “The patient is asymptomatic and here for routine colorectal cancer screening. The scope was advanced to 60cm. Mucosa was normal. No polyps or masses seen.”
-
Coding:
-
Medicare: HCPCS code G0104 (Colorectal cancer screening; flexible sigmoidoscopy).
-
Commercial Payer: CPT 45330 with diagnosis Z12.11 (Encounter for screening for malignant neoplasm of colon) and modifier -33 if required by the payer.
-
Scenario B: The Symptomatic Patient with a Biopsy
-
Patient: 45-year-old with chronic diarrhea.
-
Procedure: The physician performs a flexible sigmoidoscopy. The mucosa in the rectum appears erythematous and friable. Multiple biopsies are taken.
-
Operative Report Key Phrase: “Indication: chronic diarrhea. Findings: Inflamed mucosa in the rectum. Biopsies were obtained using cold forceps for pathologic evaluation.”
-
Coding: 45331 (Sigmoidoscopy, flexible; with biopsy, single or multiple). Linked to an ICD-10 code for chronic diarrhea (e.g., K52.9).
Scenario C: Screening Finds a Polyp (Medicare Patient)
-
Patient: 66-year-old, Medicare beneficiary, no symptoms.
-
Procedure: Screening sigmoidoscopy. A 5mm polyp is found in the descending colon. The physician removes it using a snare technique.
-
Operative Report Key Phrase: “Screening exam. A single sessile polyp was identified. This was removed in its entirety via snare cautery and retrieved for pathology.”
-
Coding: 45346 (Sigmoidoscopy, flexible; with removal of polyp(s) by snare technique (screening)). This specific code tells Medicare that the screening benefit applies despite the intervention.
Scenario D: Incomplete Procedure Due to Pain
-
Patient: Patient presents for diagnostic evaluation of rectal bleeding.
-
Procedure: The physician attempts the scope, but the patient experiences significant discomfort. The scope is only advanced to 25cm, and the physician is unable to examine the entire sigmoid colon. No pathology is seen in the examined area.
-
Operative Report Key Phrase: “Due to patient discomfort and looping of the scope, we were unable to advance beyond 25cm. The exam was terminated early. The examined mucosa up to 25cm was normal.”
-
Coding: 45330-52 (Reduced services). This indicates a significant portion of the exam was performed, but not the complete evaluation. You would also need to communicate this clearly in the diagnosis.
The Importance of Accurate Documentation
To a coder, the operative report is the Bible. If it isn’t written down, it didn’t happen. For flexible sigmoidoscopy, the physician’s documentation must support the code chosen.
Here are the key elements a coder looks for in an operative report:
-
Indication: Why is this procedure being done? (Screening vs. Diagnostic)
-
Extent of Exam: How far did the scope go? (e.g., “to the descending colon,” “to 50cm”). A complete exam is usually to the splenic flexure.
-
Findings: What was seen? (Normal, polyps, bleeding, inflammation)
-
Specimens: Were any specimens taken? If so, how? (Brushing, biopsy forceps, snare)
-
Intervention: What was done? (Biopsy, snare polypectomy, cautery, foreign body removal)
-
Complications: Were there any issues?
-
Impression/Plan: A summary of the findings and next steps.
When documentation is clear, coding is easy. When it is vague, the coder is forced to make assumptions, which leads to compliance risks.
CPT Code for Flexible Sigmoidoscopy: A Glance at Reimbursement
While reimbursement rates vary wildly based on your geographic location (locality) and the payer (Medicare vs. Blue Cross vs. Commercial), it is helpful to understand the relative value of these codes.
Generally, the more work involved, the higher the reimbursement.
-
45330 (Diagnostic): The lowest relative value in the family.
-
45331 (with Biopsy): Slightly higher to account for the pathology handling and additional physician work.
-
45333 (Snare Polypectomy): Significantly higher than the diagnostic code, reflecting the increased skill and risk involved.
-
45346 (Screening with Snare): Typically priced similarly to 45333, as the work is the same, but the classification is different.
Note: Medicare and most insurers publish their fee schedules online. It is a best practice to download the fee schedule for your locality at the beginning of each year to understand exactly what you will be paid for these codes.
Conclusion
Mastering the CPT code for flexible sigmoidoscopy is about more than just memorizing “45330.” It requires a deep understanding of the clinical scenario, the nuances of the operative report, and the specific requirements of different payers. By distinguishing between screening and diagnostic exams, selecting the correct code from the 45330 family based on the intervention, and applying the appropriate modifiers like -PT or -52, you can ensure accurate reimbursement and compliance. Always remember: when in doubt, let the surgeon’s documentation guide your choice, and never hesitate to verify a payer’s specific policy to avoid costly denials.
Frequently Asked Questions (FAQ)
1. What is the difference between CPT 45330 and 45331?
The difference is the biopsy. 45330 is a diagnostic look only (with possible brushing/washing). 45331 includes the diagnostic look plus the taking of tissue samples (biopsies) during the procedure.
2. Can I bill a separate E/M code on the same day as a sigmoidoscopy?
Yes, but only if the patient’s condition required a significant, separately identifiable service. You must append modifier -25 to the E/M code, and the documentation must clearly support that the E/M service was above and beyond the normal pre- and post-operative work associated with the procedure.
3. What ICD-10 code goes with a screening sigmoidoscopy?
The primary diagnosis code for a screening is Z12.11 (Encounter for screening for malignant neoplasm of colon). If the patient has a family history, you may also code Z80.0 (Family history of malignant neoplasm of digestive organs), but Z12.11 remains the primary reason for the encounter.
4. What does modifier -PT mean for sigmoidoscopy coding?
Modifier -PT (Colorectal cancer screening; test converted to diagnostic) is a Medicare modifier. It is used when a screening sigmoidoscopy becomes diagnostic or therapeutic due to the finding of a polyp or other lesion. It protects the patient from paying a deductible or coinsurance for what started as a free screening.
5. Is a flexible sigmoidoscopy the same as a colonoscopy?
No. A colonoscopy (CPT 45378 series) examines the entire colon. A flexible sigmoidoscopy (45330 series) only examines the rectum and the lower (left) part of the colon. The preparation and sedation levels are also usually different.
Additional Resource
For the most up-to-date information on coding guidelines and payer policies, the American Medical Association (AMA) is the definitive source for CPT code definitions.
[Visit the AMA Website for CPT Code Guidelines] (Link to: https://www.ama-assn.org/)
Note: Always consult the current year’s CPT manual and your local payer contracts for the most accurate coding and billing information.
Disclaimer: The information provided in this article is for educational and informational purposes only and does not constitute legal, billing, or coding advice. Medical coding practices, payer policies, and reimbursement rates are subject to change and vary by location and insurer. You should always consult with qualified professionals and refer to the latest official CPT coding manuals and payer guidelines to ensure compliance and accuracy.






