In the intricate world of modern healthcare, the clarity of a clinical procedure and the precision of its administrative translation are inextricably linked. Nowhere is this connection more vital than in the realm of procedural coding, where the complex, hands-on work of a gastroenterologist performing an upper gastrointestinal (GI) endoscopy must be accurately captured in a standardized, alphanumeric language. This language is ICD-10-PCS (International Classification of Diseases, Tenth Revision, Procedure Coding System), and mastery of it is not merely an administrative task—it is a critical component of patient care, revenue cycle management, and healthcare data analytics.
An upper GI endoscopy, often referred to as an esophagogastroduodenoscopy (EGD), is a minimally invasive procedure that allows a physician to visually examine the lining of the esophagus, stomach, and duodenum. While the procedure itself is a marvel of medical technology, its financial and operational viability hinges on the accurate assignment of ICD-10-PCS codes. These codes determine reimbursement, inform quality metrics, track disease prevalence, and facilitate crucial research. A single misstep in code selection—confusing an Inspection with an Excision, or missing a device—can lead to claim denials, compliance issues, and a distorted picture of healthcare delivery.
This article is designed to be your definitive guide through the complex landscape of Upper GI Endoscopy ICD-10-PCS coding. We will move beyond simple code look-ups and delve into the underlying logic of the system. You will learn to think like a coder and a clinician simultaneously, deconstructing procedures into their fundamental components to build the correct code with confidence. From the basic diagnostic EGD to advanced procedures like Endoscopic Retrograde Cholangiopancreatography (ERCP) and therapeutic stent placements, we will explore the anatomy, the root operations, the approaches, and the devices that form the building blocks of every code. Prepare to embark on a detailed journey that will transform your understanding and elevate your coding expertise.
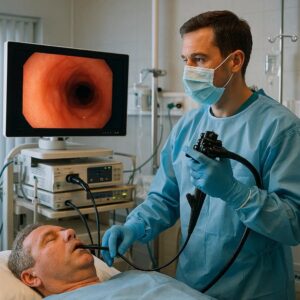
Upper GI Endoscopy ICD-10-PCS Coding
2. Deconstructing the ICD-10-PCS Framework: The Seven-Character Code
Before we apply ICD-10-PCS to upper GI endoscopy, it is imperative to understand its fundamental structure. Unlike its diagnosis counterpart (ICD-10-CM), which is largely based on a decimal system, PCS is composed of seven alphanumeric characters. Each character represents a specific aspect of the procedure, providing a multi-dimensional identifier. This structure allows for immense specificity.
Let’s break down the meaning of each character position:
-
Character 1: Section – This identifies the broad section where the procedure is classified. For the vast majority of upper GI endoscopies, this will be the Medical and Surgical Section, represented by the number 0.
-
Character 2: Body System – This refers to the general physiological system on which the procedure is performed. For upper GI endoscopies, the relevant body systems are:
-
D: Gastrointestinal System – For procedures on the esophagus, stomach, duodenum, and jejunum.
-
F: Hepatobiliary System and Pancreas – For procedures involving the bile ducts, pancreatic ducts, and sphincter of Oddi (crucial for ERCP).
-
-
Character 3: Root Operation – This is the core of the procedure. It defines the objective—what the physician is doing. This is the most critical and often the most challenging character to determine. Root operations like Inspection, Excision, Dilation, and Extraction are the verbs of the PCS language. We will dedicate an entire section to these.
-
Character 4: Body Part – This specifies the exact anatomical site where the root operation was performed. For example, the esophagus is broken down into Upper, Middle, and Lower thirds, each with a unique code.
-
Character 5: Approach – This describes how the physician accessed the site of the procedure. For endoscopy, the most common approaches are:
-
Via Natural or Artificial Opening (0)
-
Via Natural or Artificial Opening Endoscopic (3)
-
Open (0), Percutaneous (3), etc., for non-endoscopic components.
-
-
Character 6: Device – This character identifies any device that remains in the patient after the procedure is completed. Examples include drainage devices, stents, radioactive elements, or monitoring devices. If no device remains, this character is always Z: No Device.
-
Character 7: Qualifier – This provides additional information about the procedure that is not captured in the other characters. It often specifies a diagnostic or therapeutic context. For example, in the Gastrointestinal system, a common qualifier is X: Diagnostic. This character is frequently Z: No Qualifier.
Visual Aid: Code Building Block
[0] [D] [J] [5] [3] [Z] [X] | | | | | | | | | | | | | Qualifier: Diagnostic | | | | | Device: None | | | | Approach: Via Natural or Artificial Opening Endoscopic | | | Body Part: Duodenum | | Root Operation: Inspection | Body System: Gastrointestinal Section: Medical and Surgical
This code, 0DJ53ZX, represents a diagnostic endoscopic inspection of the duodenum.
3. The Landscape of the Upper GI Tract: Anatomical Essentials for the Coder
Precise anatomical knowledge is the bedrock of accurate PCS coding. The coder must be able to map the physician’s narrative onto the specific body parts defined in the ICD-10-PCS tables.
The Upper Gastrointestinal Tract includes:
-
Esophagus: The muscular tube connecting the pharynx to the stomach. In PCS, it is subdivided into:
-
Upper Esophagus
-
Middle Esophagus
-
Lower Esophagus
-
The Esophagogastric Junction is also a distinct body part.
-
-
Stomach: The J-shaped organ that stores and churns food. Key parts are:
-
Stomach
-
Pylorus (the valve controlling exit from the stomach)
-
-
Duodenum: The first and shortest part of the small intestine, immediately following the stomach. It is a C-shaped structure crucial for digestion.
-
Jejunum: The second part of the small intestine. While a standard EGD typically visualizes only the very first portion of the jejunum, it is a valid body part in PCS.
-
Hepatobiliary and Pancreatic Anatomy (for ERCP):
-
Bile Ducts: Including the Common Bile Duct, Hepatic Duct, and Cystic Duct.
-
Pancreatic Duct
-
Ampulla of Vater / Sphincter of Oddi: The small opening where the bile and pancreatic ducts empty into the duodenum.
-
Illustration:
(Imagine a detailed diagram here showing the mouth, esophagus, stomach, duodenum, jejunum, liver, gallbladder, bile ducts, and pancreas, with labels for each body part as listed in the PCS system.)
*Caption: Anatomical map of the upper GI tract and related structures, highlighting the body parts critical for accurate ICD-10-PCS coding.*
4. The Endoscope as a Tool: Understanding the Medical and Surgical Section (0)
The Medical and Surgical Section (0) encompasses procedures that are performed for a variety of reasons, including diagnosis, treatment, exploration, and/or the alteration of anatomy. The upper GI endoscope is the tool that enables these procedures within this section. It is important to note that the endoscope itself is not the procedure; it is the vehicle for the approach. The root operation defines the action taken through the endoscope.
The key distinction for the coder is to identify when a procedure falls into this section versus others. For example, the introduction of a contrast agent during an ERCP is coded in the Administration section. Taking a biopsy (excision of tissue) through the endoscope is coded in the Medical and Surgical section. This article focuses exclusively on the procedures classified in the Medical and Surgical Section.
5. A Deep Dive into Root Operations: The “Why” Behind the Procedure
The root operation is the cornerstone of ICD-10-PCS. Selecting the correct one requires a careful analysis of the physician’s intent and action. Let’s explore the root operations most relevant to upper GI endoscopy.
5.1. Inspection (J01) – The Diagnostic Cornerstone
-
Definition: Visually and/or manually exploring a body part. The primary goal is to assess its appearance, and no therapeutic intervention is performed. If the procedure is only looking, it is an Inspection.
-
Clinical Example: A diagnostic EGD to investigate dysphagia (difficulty swallowing) or heartburn, where the physician simply visualizes the mucosa and notes its condition.
-
Coding Nuance: The qualifier character is often X: Diagnostic for this root operation. If an abnormality is seen but nothing is done, it remains an Inspection.
5.2. Excision (B) & Resection (T) – Tissue Removal for Analysis
-
Excision (B): Cutting out or off, without replacement, a portion of a body part. The physician’s documentation of “biopsy” almost always maps to Excision.
-
Clinical Example: Taking a biopsy of a suspicious gastric ulcer or an esophageal polyp.
-
Key Point: The body part is the anatomical site from which the tissue was taken (e.g., Stomach, Lower Esophagus).
-
-
Resection (T): Cutting out or off, without replacement, all of a body part.
-
Clinical Example: Endoscopic Mucosal Resection (EMR) or Endoscopic Submucosal Dissection (ESD), where a larger area of abnormal tissue (like early-stage cancer) is removed in its entirety.
-
Key Point: This is used for more extensive removals than a simple biopsy.
-
5.3. Dilation (7) – Opening the Pathway
-
Definition: Expanding an orifice or the lumen of a tubular body part. This is typically done using balloon dilators or guided bougie dilators passed through the endoscope.
-
Clinical Example: Dilation of an esophageal stricture (narrowing) caused by chronic acid reflux or a malignant tumor.
-
Coding Nuance: The device character is used if the dilator (the balloon) is left in place, which is rare. It is typically removed, so the device character is Z: No Device.
5.4. Destruction (5) – Ablating Abnormal Tissue
-
Definition: Physical eradication of a body part in such a way that it is not feasible to reattach the destroyed tissue. The tissue is ablated, fulgurated, vaporized, or cauterized.
-
Clinical Example: Argon Plasma Coagulation (APC) of an angiodysplasia (a vascular abnormality) or cauterization of a bleeding vessel.
-
Key Point: The tissue is destroyed in situ; no specimen is sent to pathology (unlike Excision).
5.5. Extraction (D) – Removing Foreign Objects and Obstructions
-
Definition: Pulling out or off a solid matter from a body part. The solid matter is not a device and was not naturally intended to be there.
-
Clinical Example: Removal of a food bolus impaction from the esophagus or extracting gallstones from the common bile duct during an ERCP.
-
Key Point: This is distinct from Removal (P), which is used for taking out a device.
5.6. Insertion (H) & Replacement (R) – Stents and Feeding Tents
-
Insertion (H): Putting in a non-biological device that remains in the body after the procedure.
-
Clinical Example: Initial placement of an esophageal stent to keep a malignant stricture open or placing a percutaneous endoscopic gastrostomy (PEG) tube.
-
-
Replacement (R): Putting in a device that replaces a previously placed device.
-
Clinical Example: Exchanging an old, clogged PEG tube for a new one.
-
5.7. Bypass (1) – Creating a New Route
-
Definition: Altering the route of passage of the contents of a tubular body part. The procedure reroutes the flow, bypassing a diseased or obstructed segment.
-
Clinical Example: Surgical gastrojejunostomy (though often open, it can be done laparoscopically). In a purely endoscopic context, this is less common but is included for completeness.
5.8. Other Root Operations: Division, Repair, and More
-
Division (8): Cutting into a body part without removing tissue. The classic example is a sphincterotomy during ERCP, where the sphincter of Oddi is cut to facilitate stone removal or stent placement.
-
Repair (Q): Restoring, to the extent possible, a body part to its normal anatomical structure. An example would be the endoscopic clipping of a perforation.
-
Restriction (V): Partially closing an orifice or lumen. This could involve placing clips on a bleeding vessel to restrict blood flow.
Summary of Key Root Operations in Upper GI Endoscopy
| Root Operation | PCS Code | Definition | Common Upper GI Example | Key Documentation Clues |
|---|---|---|---|---|
| Inspection | J | Visually/manually examining a body part | Diagnostic EGD | “EGD performed for evaluation of dysphagia,” “mucosa appeared normal” |
| Excision | B | Cutting out a portion of a body part | Biopsy of ulcer, polyp | “Biopsies were taken,” “cold forceps biopsy,” “polypectomy” |
| Resection | T | Cutting out all of a body part | Endoscopic Mucosal Resection (EMR) | “EMR performed,” “the lesion was resected in toto” |
| Dilation | 7 | Expanding an orifice or lumen | Balloon dilation of esophageal stricture | “Balloon dilation was performed,” “savary dilation” |
| Destruction | 5 | Eradicating tissue without removal | Cauterization of AVM, APC | “Cauterized,” “fulgurated,” “Argon Plasma Coagulation applied” |
| Extraction | D | Pulling out solid matter | Removal of food impaction, ERCP stone extraction | “Food bolus was removed,” “stone basket used to extract stones” |
| Insertion | H | Putting in a device | Placement of esophageal stent, PEG tube | “Stent was deployed,” “PEG tube placed” |
| Division | 8 | Cutting into a body part | Sphincterotomy of Sphincter of Oddi | “Sphincterotomy performed with needle knife” |
| Repair | Q | Restoring normal anatomy | Clipping of a perforation | “Perforation was closed with endoclips” |
| Restriction | V | Partially closing an orifice/lumen | Clipping of a bleeding vessel | “Hemostatic clips applied to the bleeding vessel” |
| Table Border: Solid 1px border around the entire table and between cells. |
6. The Approach Character: From Natural Orifices to Open Surgery
The approach describes the technique used to reach the site of the procedure. For upper GI endoscopy, the two primary approaches are:
-
Via Natural or Artificial Opening Endoscopic (3): This is the most common approach for upper GI endoscopy. The procedure is performed through a natural opening (the mouth) using an endoscope. This code is used whether the scope passes into the esophagus, stomach, or duodenum.
-
Via Natural or Artificial Opening (0): This approach is used when a procedure is performed through a natural opening but without the use of an endoscope. This is rare in the upper GI tract but could theoretically apply to a blind procedure.
It is crucial to understand that if an endoscopic procedure starts as one approach but converts to an open surgical procedure, you would code both the endoscopic root operation and the open root operation.
7. The Device Character: Capturing What is Left Behind
The device character is only used if a device remains in the patient after the procedure is completed. If the device is removed, you do not code it.
-
Drainage Device (0): For example, a plastic stent placed in the bile duct or pancreatic duct to allow drainage.
-
Stent (4): For example, a metal or plastic esophageal stent.
-
Radioactive Element (U): For example, a brachytherapy seed placed endoscopically (less common).
-
No Device (Z): This is used in the vast majority of cases (e.g., after a biopsy, dilation, or inspection).
8. Putting It All Together: Clinical Scenarios and Code Building
Let’s apply our knowledge to real-world documentation.
Scenario 1: The Routine Diagnostic EGD
-
Procedure Note: “EGD was performed for evaluation of chronic heartburn. The scope was passed under direct vision into the esophagus, stomach, and duodenum. The mucosa was normal throughout. No biopsies were taken.”
-
Deconstruction:
-
Root Operation: The goal was to look. This is Inspection (J).
-
Body Part: The entire upper GI tract was inspected. However, PCS requires coding to the furthest extent reached. In this case, the Duodenum (5).
-
Approach: Via mouth with a scope -> Via Natural or Artificial Opening Endoscopic (3).
-
Device: None -> No Device (Z).
-
Qualifier: The procedure was purely diagnostic -> Diagnostic (X).
-
-
ICD-10-PCS Code: 0DJ53ZX (Inspection of Duodenum, Via Natural or Artificial Opening Endoscopic, Diagnostic)
Scenario 2: Biopsy of an Esophageal Lesion
-
Procedure Note: “EGD revealed a suspicious ulcer in the lower esophagus. Multiple biopsy samples were taken from the ulcer margin using cold forceps.”
-
Deconstruction:
-
Root Operation: Taking tissue samples -> Excision (B).
-
Body Part: Lower Esophagus (C).
-
Approach: Via Natural or Artificial Opening Endoscopic (3).
-
Device: None -> No Device (Z).
-
Qualifier: No Qualifier (Z).
-
-
ICD-10-PCS Code: 0DB53ZZ (Excision of Lower Esophagus, Via Natural or Artificial Opening Endoscopic)
Scenario 3: Dilation of an Esophageal Stricture
-
Procedure Note: “A tight benign stricture was identified in the mid-esophagus. Sequential balloon dilation was performed to 15mm with excellent result.”
-
Deconstruction:
-
Root Operation: Expanding the lumen -> Dilation (7).
-
Body Part: Middle Esophagus (D).
-
Approach: Via Natural or Artificial Opening Endoscopic (3).
-
Device: The balloon is removed -> No Device (Z).
-
Qualifier: No Qualifier (Z).
-
-
ICD-10-PCS Code: 0DD53ZZ (Dilation of Middle Esophagus, Via Natural or Artificial Opening Endoscopic)
Scenario 4: Control of Bleeding Gastric Ulcer
-
Procedure Note: “A actively bleeding vessel was seen in a gastric ulcer in the antrum. Hemostasis was achieved with the application of two hemostatic clips.”
-
Deconstruction:
-
Root Operation: The clips are partially closing the lumen of the vessel to stop flow -> Restriction (V).
-
Body Part: Stomach (F).
-
Approach: Via Natural or Artificial Opening Endoscopic (3).
-
Device: The clips remain in place. In PCS, hemostatic clips are classified as Intraluminal Device (7).
-
Qualifier: No Qualifier (Z).
-
-
ICD-10-PCS Code: 0DV53CZ (Restriction of Stomach, Via Natural or Artificial Opening Endoscopic, Intraluminal Device)
Scenario 5: ERCP with Sphincterotomy and Stone Extraction
This is a multi-step procedure requiring multiple codes.
-
Procedure Note: “The duodenoscope was advanced to the second portion of the duodenum. The ampulla was cannulated, and a sphincterotomy was performed. A balloon catheter was then used to extract several small stones from the common bile duct. The duct was cleared.”
-
Deconstruction – Code 1 (Sphincterotomy):
-
Root Operation: Cutting the muscle -> Division (8).
-
Body System: Hepatobiliary System (F).
-
Body Part: Sphincter of Oddi (0).
-
Approach: Via Natural or Artificial Opening Endoscopic (3).
-
Device: None -> No Device (Z).
-
Qualifier: No Qualifier (Z).
-
Code 1: 0F983ZZ
-
-
Deconstruction – Code 2 (Stone Extraction):
-
Root Operation: Pulling out solid matter -> Extraction (D).
-
Body System: Hepatobiliary System (F).
-
Body Part: Common Bile Duct (4).
-
Approach: Via Natural or Artificial Opening Endoscopic (3).
-
Device: None -> No Device (Z).
-
Qualifier: No Qualifier (Z).
-
Code 2: 0FD53ZZ
-
Scenario 6: Placement of an Esophageal Stent
-
Procedure Note: “A malignant stricture in the lower esophagus was identified. A fully covered metal stent was deployed across the stricture under endoscopic and fluoroscopic guidance.”
-
Deconstruction:
-
Root Operation: Putting in a device -> Insertion (H).
-
Body Part: Lower Esophagus (C).
-
Approach: Via Natural or Artificial Opening Endoscopic (3).
-
Device: The stent is a Stent (4).
-
Qualifier: No Qualifier (Z).
-
-
ICD-10-PCS Code: 0DH54CZ (Insertion of Stent into Lower Esophagus, Via Natural or Artificial Opening Endoscopic)
9. Navigating Complex Procedures: ERCP and Endoscopic Ultrasound (EUS)
ERCP is a hybrid procedure combining endoscopy and fluoroscopy. As seen in Scenario 5, it often requires multiple codes. Remember that the injection of contrast material is coded separately in the Administration section (e.g., 3E0G836 for Introduction of other diagnostic substance into GI tract, via natural or artificial opening).
Endoscopic Ultrasound (EUS) involves an endoscope with an ultrasound probe. If the EUS is performed solely for diagnostic imaging (visualizing layers of the gut wall or adjacent structures), the root operation is Inspection. However, if a Fine Needle Aspiration (FNA) is performed under EUS guidance, that is coded as Excision (or Drainage if fluid is aspirated), with the approach being endoscopic. The guidance itself is not separately coded in PCS.
10. Common Pitfalls and How to Avoid Them
-
Coding an Inspection when a Biopsy is Taken: If a biopsy is performed, the root operation is Excision, not Inspection. The Inspection is inherent in the Excision and is not coded separately.
-
Incorrect Body Part: Confusing the lower esophagus with the upper stomach, or not coding to the furthest extent reached. Always cross-reference the physician’s anatomical description with the PCS body part definitions.
-
Misidentifying the Root Operation: Using “Control of Bleeding” as a root operation. You must determine how the bleeding was controlled (e.g., Destruction via cautery, Restriction via clips).
-
Over-coding the Device: Coding a device that was used but removed (e.g., a biopsy forceps, a dilation balloon). Only code devices that remain.
-
Ignoring the Qualifier: Forgetting to use the X: Diagnostic qualifier for a purely diagnostic Inspection.
11. The Importance of Physician Documentation
The coder is entirely dependent on the quality of the physician’s procedure report. Incomplete or vague documentation is the primary source of coding errors. Encourage physicians to be specific:
-
State the indication (diagnostic vs. therapeutic).
-
Describe what was seen (anatomy).
-
Detail what was done (biopsied, dilated, stented, cauterized).
-
Specify the instruments used (cold forceps, hot snare, balloon size, type of stent).
-
Note the final diagnosis.
12. Conclusion: The Path to Coding Mastery
Mastering Upper GI Endoscopy ICD-10-PCS coding is a journey of continuous learning that demands a synthesis of anatomical knowledge, procedural understanding, and meticulous attention to the system’s logical structure. By deconstructing each procedure into its fundamental components—Section, Body System, Root Operation, Body Part, Approach, Device, and Qualifier—you can move beyond memorization to genuine comprehension. This expertise ensures accurate reimbursement, supports quality patient care, and contributes to the integrity of vital health data. Remember, the codebook is your map, but clinical documentation is your terrain; navigate both with care and precision.
13. Frequently Asked Questions (FAQs)
Q1: If an EGD is performed and a polyp is found and biopsied, do I code both the Inspection and the Excision?
A1: No. When a diagnostic procedure (Inspection) leads to a biopsy (Excision), you code only the Excision. The Inspection is considered an integral part of the procedure and is not coded separately.
Q2: How do I code a screening EGD?
A2: A screening EGD, where the patient is asymptomatic, is still coded with the root operation Inspection. The intent is to inspect for potential disease. The ICD-10-CM diagnosis code (e.g., Z12.81) would indicate the screening nature, but the PCS code would be the same as a diagnostic inspection (e.g., 0DJ53ZX).
Q3: What is the difference between Excision and Resection in the context of a polypectomy?
A3: This depends on the physician’s documentation. A simple polypectomy where the polyp is snipped off is typically coded as Excision. However, if the physician documents Endoscopic Mucosal Resection (EMR) or states that the lesion was “resected in its entirety,” implying a more substantial tissue removal, then the root operation Resection is used.
Q4: How do I code a procedure that involves both the stomach and duodenum?
A4: You code the procedure that is performed at the furthest anatomical extent. If you inspect and biopsy the stomach and then advance to inspect the duodenum, the Inspection code would be for the Duodenum. However, if you perform distinct procedures in different locations (e.g., biopsy the stomach and also biopsy the duodenum), you would code two separate Excision procedures.
Q5: Where can I find the official ICD-10-PCS guidelines and code tables?
A5: The Centers for Medicare & Medicaid Services (CMS) and the National Center for Health Statistics (NCHS) are the official publishers of the ICD-10-PCS system. These resources are available on the CMS website. Commercial coding vendors also provide licensed, searchable versions of the code set.
Date: November 24, 2025
Author: Gastrointestinal Coding Specialist
Disclaimer: This article is intended for educational purposes and to provide a foundational understanding of ICD-10-PCS coding principles. It is not a substitute for the official ICD-10-PCS code set, guidelines, or professional coding advice. Coders must always consult the most current year’s official codebooks and payer-specific policies for accurate code assignment.






