In the intricate ecosystem of modern healthcare, the alphanumeric sequences of the International Classification of Diseases, Tenth Revision, Clinical Modification (ICD-10-CM) are far more than mere administrative placeholders. They are the fundamental language of patient condition, the DNA of epidemiological data, and the bedrock upon which healthcare reimbursement and strategic planning are built. For a condition as common, clinically significant, and potentially severe as pyelonephritis, mastering this language is not just a clerical task—it is a critical component of high-quality patient care and a financially sustainable healthcare system.
Pyelonephritis, an infection of the kidneys and renal pelvis, represents a substantial clinical and economic burden. It accounts for over 250,000 office visits and 100,000 hospitalizations annually in the United States alone. The clinical spectrum is vast, ranging from a simple, community-acquired infection in a healthy young woman to a life-threatening urosepsis in an elderly, diabetic patient with an obstructing stone. This very spectrum is what makes accurate ICD-10 coding for pyelonephritis both challenging and essential.
An imprecise code can distort public health data, misrepresent a hospital’s case-mix index (CMI), and lead to significant financial repercussions through claim denials or underpayments. More importantly, it fails to paint an accurate picture of the patient’s true condition. This article is designed to be the definitive guide for medical coders, health information management (HIM) professionals, physicians, advanced practice providers, and revenue cycle specialists. We will embark on a detailed journey through the anatomy of a pyelonephritis diagnosis, deconstruct the ICD-10 framework that classifies it, and navigate the complex scenarios that test the skills of even the most experienced coders. Our goal is to transform coding from a reactive, data-entry function into a proactive, knowledge-driven process that ensures clinical integrity, financial accuracy, and ultimately, contributes to better patient outcomes.
ICD-10 code for pyelonephritis
2. Understanding the Disease: A Clinical Primer on Pyelonephritis
Before a single code can be assigned, a foundational understanding of the disease itself is paramount. Coding is not an abstract exercise; it is the translation of clinical reality into a standardized format.
What is Pyelonephritis? Pathophysiology and Progression
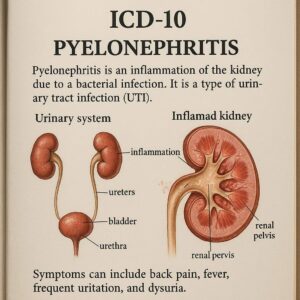
Pyelonephritis is a type of urinary tract infection (UTI) that has ascended from the lower urinary tract (bladder and urethra) to the upper urinary tract, specifically involving the renal parenchyma (the functional tissue of the kidney) and the renal pelvis (the funnel-like structure where urine collects before entering the ureter). The most common pathogenic mechanism is the retrograde ascent of bacteria from the bladder up the ureters into the kidneys.
This ascent is often facilitated by vesicoureteral reflux (VUR), a condition where urine flows backward from the bladder into the ureters. However, it can also occur in the absence of VUR, particularly with virulent organisms or in hosts with compromised defenses. The infection triggers a robust inflammatory response—hence the suffix “-itis”—leading to the infiltration of white blood cells, edema, and potentially, the formation of microabscesses within the kidney. If left untreated or if complicated by obstruction, this can progress to pyonephrosis (pus-filled kidney), renal abscess, emphysematous pyelonephritis (in diabetics), or systemic sepsis.
Clinical Presentation: Signs, Symptoms, and Diagnostic Criteria
The clinical presentation of pyelonephritis can be dramatic, though it may be subtle in the very young, elderly, or immunocompromised. Classic signs and symptoms include:
-
-
-
Fever and Chills: Often high-grade and abrupt in onset.
-
Flank Pain: Unilateral or bilateral, typically costovertebral angle (CVA) tenderness upon physical examination.
-
Nausea and Vomiting: A common systemic response.
-
General Malaise: Profound fatigue and body aches.
-
Lower UTI Symptoms: Although not always present, patients may also report dysuria (painful urination), frequency, and urgency.
-
-
Diagnosis is based on a combination of history, physical exam, and diagnostic testing. Key tests include:
-
-
-
Urinalysis: To look for pyuria (white blood cells in urine), bacteriuria, and sometimes leukocyte casts, which are indicative of renal involvement.
-
Urine Culture and Sensitivity: Crucial for identifying the specific causative organism (most commonly E. coli) and guiding antibiotic therapy.
-
Blood Tests: Complete blood count (CBC) may show leukocytosis (elevated white blood cells). Blood cultures are indicated if systemic sepsis is suspected.
-
Imaging: Renal ultrasound or CT scan is not always necessary for uncomplicated cases but is essential if obstruction (e.g., from a stone), abscess, or emphysematous pyelonephritis is suspected.
-
-
Etiology: The Usual Suspects and Atypical Pathogens
The vast majority (70-95%) of community-acquired acute pyelonephritis cases are caused by uropathogenic Escherichia coli (E. coli). Other common gram-negative organisms include:
-
-
-
Klebsiella pneumoniae
-
Proteus mirabilis (notably associated with struvite stones)
-
Pseudomonas aeruginosa (more common in hospital-acquired infections)
-
Enterobacter species
-
-
Gram-positive pathogens, though less common, include Enterococcus faecalis and Staphylococcus saprophyticus. In hospitalized patients or those with recent instrumentation, the spectrum of pathogens broadens, and antibiotic resistance is a greater concern.
Risk Factors and Potential Complications
Understanding risk factors helps contextualize the coding, especially when documenting associated conditions. Key risk factors include:
-
-
-
Female Gender: Due to a shorter urethra.
-
Sexual Activity: In young women.
-
Pregnancy: Physiological changes increase risk.
-
Urinary Tract Obstructions: Kidney stones, benign prostatic hyperplasia (BPH), tumors.
-
Vesicoureteral Reflux (VUR): Especially in children.
-
Neurological Conditions: Spinal cord injuries, neurogenic bladder.
-
Diabetes Mellitus: Increases risk and severity (e.g., emphysematous pyelonephritis).
-
Immunosuppression: HIV, chemotherapy, transplant patients.
-
Indwelling Urinary Catheters.
-
-
Potential complications, which often require their own specific ICD-10 codes, include:
-
-
-
Sepsis and Septic Shock
-
Renal Abscess (Intrarenal or Perinephric)
-
Pyonephrosis
-
Acute Kidney Injury (AKI)
-
Emphysematous Pyelonephritis
-
Chronic Kidney Disease (from recurrent or chronic pyelonephritis)
-
-
3. The ICD-10 Coding Framework: An Overview of the N10-N16 Block
ICD-10-CM is a highly detailed, hierarchical system. Codes for pyelonephritis and related conditions are found within Chapter 14: Diseases of the Genitourinary System (N00-N99), specifically in the block N10-N16: Renal Tubulo-Interstitial Diseases.
This block encompasses a range of conditions affecting the renal tubules and interstitium, the functional components of the kidney, with inflammation (nephritis) being a common theme. It is crucial to understand that the codes in this block are often “combination codes,” meaning they include both the diagnosis (e.g., pyelonephritis) and its etiology or manifestation (e.g., acute, chronic, obstructive).
4. A Deep Dive into Specific Pyelonephritis Codes
Here, we dissect the primary codes used for pyelonephritis, exploring their definitions, appropriate use cases, and nuances.
N10: Acute Tubulo-Interstitial Nephritis
This is the code for acute pyelonephritis. The term “tubulo-interstitial nephritis” in this context is used synonymously with pyelonephritis in the ICD-10 framework.
-
-
-
Clinical Context: This code is used for a new, active infection of the kidney. The patient presents with the classic acute symptoms described earlier (fever, chills, flank pain). The diagnosis is typically confirmed by urinalysis and culture.
-
Specificity: Code N10 does not specify laterality. Therefore, a 5th digit is required to indicate which kidney is affected.
-
N10.0: Acute tubulo-interstitial nephritis, unspecified kidney
-
N10.1: Acute tubulo-interstitial nephritis, right kidney
-
N10.2: Acute tubulo-interstitial nephritis, left kidney
-
N10.3: Acute tubulo-interstitial nephritis, bilateral
-
-
Key Point: Always strive for the highest level of specificity. If the medical record (e.g., physician’s note, imaging report) clearly states “right-sided” or “left-sided,” you must use N10.1 or N10.2. Using N10.0 (unspecified) when laterality is known is clinically inaccurate and may be flagged by payers.
-
-
N11: Chronic Tubulo-Interstitial Nephritis
This category is for chronic pyelonephritis. Chronicity implies a persistent or recurrent infection/inflammation leading to irreversible scarring and damage to the renal parenchyma. This is a more complex category with several sub-codes.
-
-
-
N11.0: Nonobstructive Reflux-Associated Chronic Pyelonephritis
This code is used when the chronic kidney damage is directly attributed to vesicoureteral reflux (VUR), without a concurrent obstruction. This is a common scenario in pediatric patients with a history of recurrent UTIs. The code includes the chronic infection and the associated VUR. -
N11.1: Chronic Obstructive Pyelonephritis
This code is used when chronic pyelonephritis occurs secondary to a documented obstruction. This could be due to a kidney stone, ureteral stricture, prostate enlargement, or a congenital anomaly. The code captures the chronic infection and the obstructive component. -
N11.8: Other Chronic Tubulo-Interstitial Nephritis
This is a catch-all code for chronic pyelonephritis that does not fit into the reflux-associated or obstructive categories. It should be used when the chronic condition is documented, but the specific association (reflux or obstruction) is not stated or is due to another cause. -
N11.9: Chronic Tubulo-Interstitial Nephritis, Unspecified
This code is for a general diagnosis of chronic pyelonephritis without any further specification regarding cause. Its use should be minimal if proper clinical documentation is available.
-
-
N12: Tubulo-interstitial Nephritis, Not Specified as Acute or Chronic
This is the “unspecified” code for pyelonephritis. It should be used only when the medical documentation does not specify whether the condition is acute or chronic. For example, if a provider simply writes “pyelonephritis” in a discharge summary without any modifiers, N12 would be appropriate. However, this represents a clinical and coding failure. A coder should ideally query the provider for clarification to assign a more specific code (N10 or N11.x). Like N10, it requires a 5th digit for laterality.
N13.6: Pyonephrosis
Pyonephrosis is a severe, suppurative infection of the kidney where the renal pelvis is filled with pus, typically in the setting of complete obstruction (e.g., from a stone). It is a urological emergency requiring prompt drainage (e.g., via nephrostomy tube). This code is distinct from simple pyelonephritis and indicates a much more critical condition.
N15.1: Renal and Perinephric Abscess
An abscess is a localized collection of pus. A renal abscess is within the kidney tissue, while a perinephric abscess is in the fatty tissue surrounding the kidney. This is a serious complication of pyelonephritis that often requires drainage in addition to intravenous antibiotics. This code should be used in conjunction with a pyelonephritis code (e.g., N10) if both conditions are present.
N16: Renal Tubulo-Interstitial Disorders in Diseases Classified Elsewhere
This category is governed by the “code first” instruction. It is used when the renal tubulo-interstitial disease (including pyelonephritis) is a manifestation of a systemic disease classified in another chapter of ICD-10-CM.
Examples:
-
-
-
Pyelonephritis in Tuberculosis: Code first A18.11 (Tuberculosis of kidney), then use N16.
-
Pyelonephritis in Sarcoidosis: Code first D86.84 (Sarcoidosis of kidney), then use N16.
-
Pyelonephritis in Systemic Lupus Erythematosus: Code first M32.14 (Glomerular disease in systemic lupus erythematosus), then use N16.
-
-
5. The Art of Specificity: Laterality, Causative Organisms, and Associated Conditions
Precision in ICD-10 coding is achieved through the use of additional codes that provide a complete clinical picture.
The Critical Importance of Laterality
As highlighted with codes N10 and N12, laterality is a mandatory component. Bilateral pyelonephritis, while less common, does occur and must be coded as such (e.g., N10.3). Assuming laterality from symptoms alone is not permissible; it must be explicitly documented by the provider.
Coding for the Infectious Agent
While not required for code assignment from the N10-N16 block, it is a best practice and often necessary for accurate reimbursement and infection control to identify the causative organism. Codes from categories B95-B97 are used for this purpose.
-
-
-
B95.-: Streptococcus and Staphylococcus as the cause of diseases classified elsewhere.
-
B96.-: Other specified bacterial agents (e.g., B96.20 for E. coli).
-
B97.-: Viral agents.
-
-
Example: A patient is admitted with acute E. coli pyelonephritis. The codes would be:
-
-
-
N10.1 (if right-sided)
-
B96.20 (Unspecified Escherichia coli [E. coli] as the cause of diseases classified elsewhere)
-
-
Linking to Underlying Conditions
A key strength of ICD-10 is its ability to link complications to their underlying causes. This is vital for risk adjustment and understanding the true patient population.
-
-
-
With Vesicoureteral Reflux (VUR): As seen with N11.0, this is a combination code. If a patient has acute pyelonephritis with VUR, you would code N10 and N13.70 (Vesicoureteral reflux, unspecified).
-
With Obstruction: If a patient has acute pyelonephritis due to an obstructing ureteral stone, you would code:
-
N10 (Acute pyelonephritis)
-
N13.6 (Pyonephrosis, if present) OR N13.1 (Hydronephrosis with ureteral stricture)
-
N20.1 (Ureteral calculus)
-
-
With Diabetes: While diabetes is a major risk factor, it is not coded as a direct cause unless the pyelonephritis is a manifestation of the diabetes (e.g., in the case of emphysematous pyelonephritis, which would be coded to E11.69).
-
-
6. Complex Coding Scenarios: From Sepsis to Pregnancy
This is where coding expertise truly shines. Let’s break down some of the most challenging situations.
Coding Pyelonephritis with Sepsis and Urosepsis
This is one of the most critical and error-prone scenarios. The official ICD-10-CM coding guidelines provide a clear sequence.
Scenario: A patient presents with high fever, rigors, hypotension, and CVA tenderness. Blood cultures and urine cultures both grow E. coli. The physician diagnoses “E. coli urosepsis secondary to acute pyelonephritis.”
Step-by-Step Coding:
-
-
-
Identify the Systemic Infection: Sepsis. Code first A41.51 (Sepsis due to Escherichia coli [E. coli]). *Note: The term “urosepsis” is not a codeable term in ICD-10; it is a colloquialism for sepsis originating from a UTI. You must code the sepsis with the identified organism.*
-
Identify the Underlying Local Infection: The source of the sepsis is the pyelonephritis. Code next N10.0 (or the specific laterality code for acute pyelonephritis).
-
Code the Organism (if not included in the sepsis code): In this case, A41.51 already specifies E. coli, so B96.20 is redundant and should not be used.
-
Code any Acute Organ Dysfunction: If the patient has acute kidney injury (AKI) or shock, these would be coded as additional diagnoses (e.g., N17.9 for AKI, R65.21 for severe sepsis with septic shock).
-
-
Final Code Sequence for this scenario:
-
-
-
A41.51 Sepsis due to Escherichia coli
-
N10.1 Acute tubulo-interstitial nephritis, right kidney (if documented)
-
-
Pyelonephritis in Pregnancy (O23.1-)
Pregnancy complicates coding because conditions related to the gestational period are coded from Chapter 15 (Pregnancy, Childbirth, and the Puerperium). The coding guidelines state that if a pregnancy-related condition is specified, you must use a code from Chapter 15.
-
-
-
Code: O23.1- (Infections of kidney in pregnancy)
-
Specificity: This code requires a 5th digit to specify the trimester.
-
O23.11: 1st trimester
-
O23.12: 2nd trimester
-
O23.13: 3rd trimester
-
O23.19: Unspecified trimester
-
-
-
Crucial Note: You do not also code N10 (Acute pyelonephritis). The code O23.1- includes the diagnosis of pyelonephritis in the context of pregnancy. You may, however, use an additional code from B95-B97 to identify the infectious agent if known.
Postprocedural and Iatrogenic Pyelonephritis
If a pyelonephritis develops as a direct result of a procedure (e.g., cystoscopy, catheterization), it is considered a complication.
-
-
-
Code: A code from the T80-T88 block (Complications of surgical and medical care, not elsewhere classified) is used. Specifically, T83.5- (Infection and inflammatory reaction due to prosthetic device, implant and graft in urinary system) might be used for an indwelling catheter, or more generally, T81.4- (Infection following a procedure).
-
Additional Codes: You would also code the specific type of infection (e.g., N10 for acute pyelonephritis) and the organism (B96.-). An external cause code (Y62-Y84) may also be required to identify the specific procedure.
-
-
7. Documentation is Everything: A Guide for Clinicians and Coders
The coder can only code what is documented. Poor documentation is the root cause of most coding errors and denials.
What Physicians Must Document for Optimal Coding:
-
-
-
Specific Diagnosis: “Acute pyelonephritis” is far better than just “pyelonephritis” or “UTI.”
-
Laterality: “Right-sided,” “left-sided,” or “bilateral.”
-
Acuity: “Acute” vs. “Chronic.” If chronic, specify the etiology if known (e.g., “chronic pyelonephritis due to long-standing VUR”).
-
Associated Conditions: Clearly state if there is obstruction, reflux, abscess, or stones.
-
Causative Organism: Document the final culture and sensitivity results.
-
Link to Sepsis: Clearly state “urosepsis due to…” or “sepsis with source being pyelonephritis.”
-
-
Querying the Provider: Best Practices and Examples
A query is a formal communication from a coder or CDI (Clinical Documentation Improvement) specialist to a provider to clarify documentation in the health record.
-
-
-
Example 1 (Acuity):
-
Documentation: “Pyelonephritis, admit for IV antibiotics.”
-
Query: “Dear Dr. Smith, The patient was admitted for treatment of pyelonephritis. Can you please clarify if this is an acute or chronic infection to ensure accurate code assignment?”
-
-
Example 2 (Laterality):
-
Documentation: “Patient with flank pain and fever, diagnosis of acute pyelonephritis.”
-
Query: “The CT scan report indicates right-sided hydronephrosis and inflammatory changes. Can you specify if the acute pyelonephritis is right-sided, left-sided, or bilateral?”
-
-
-
8. Case Studies: Applying Knowledge to Real-World Scenarios
Let’s apply everything we’ve learned to practical examples.
Case Study 1: Uncomplicated Acute Pyelonephritis
-
-
-
Presentation: A 28-year-old female presents to the ER with a 24-hour history of high fever, chills, and right-sided flank pain. Urinalysis shows numerous WBCs and bacteria. CT scan confirms right-sided pyelonephritis without obstruction. Urine culture is pending. She is admitted for IV antibiotics.
-
Codes:
-
N10.1 Acute tubulo-interstitial nephritis, right kidney.
-
Note: No organism code is assigned as the culture is pending.
-
-
-
Case Study 2: Chronic Obstructive Pyelonephritis with Sepsis
-
-
-
Presentation: A 65-year-old male with a known history of left-sided staghorn calculus presents with altered mental status, hypotension, and fever. Blood and urine cultures grow Klebsiella pneumoniae. CT shows a large, obstructing stone in the left renal pelvis with severe hydronephrosis and features of chronic pyelonephritis. Diagnosis: Septic shock due to Klebsiella urosepsis from chronic obstructive pyelonephritis.
-
Codes:
-
A41.59 Sepsis due to other Gram-negative organisms (Klebsiella)
-
R65.21 Severe sepsis with septic shock
-
N11.1 Chronic obstructive pyelonephritis
-
N20.0 Calculus of kidney
-
-
-
Case Study 3: Pyelonephritis in a Pregnant Patient
-
-
-
Presentation: A 32-year-old female at 24 weeks gestation presents with fever, nausea, and left flank pain. Urine culture is positive for >100,000 CFU/ml of E. coli. Diagnosed with pyelonephritis in pregnancy.
-
Codes:
-
O23.12 Infections of kidney in pregnancy, second trimester
-
B96.20 Unspecified Escherichia coli as the cause of diseases classified elsewhere
-
-
-
Case Study 4: Renal Abscess Following a Ureteric Stone
-
-
-
Presentation: A 45-year-old diabetic male with a recent ureteric stone now presents with persistent fever despite antibiotics. CT scan reveals a 3cm renal abscess in the right kidney and a small stone at the right ureterovesical junction (UVJ).
-
Codes:
-
N15.1 Renal and perinephric abscess
-
N10.1 Acute tubulo-interstitial nephritis, right kidney
-
N20.1 Ureteral calculus
-
E11.9 Type 2 diabetes mellitus (the underlying risk factor)
-
-
-
ICD-10 Pyelonephritis Code Quick-Reference
| Clinical Scenario | Primary ICD-10 Code | Code Title | Key Instructions / Additional Codes |
|---|---|---|---|
| Simple Acute Pyelonephritis | N10.0-, N10.1, N10.2, N10.3 | Acute tubulo-interstitial nephritis | Must specify laterality. Add B95-B97 for organism if known. |
| Chronic Pyelonephritis with Reflux | N11.0 | Nonobstructive reflux-associated chronic pyelonephritis | This is a combination code. No need for a separate VUR code. |
| Chronic Pyelonephritis with Obstruction | N11.1 | Chronic obstructive pyelonephritis | This is a combination code. Also code the cause of obstruction (e.g., N20.-). |
| Unspecified Acuity | N12.0-, N12.1, N12.2, N12.3 | Tubulo-interstitial nephritis, not specified as acute or chronic | Query the provider for clarity. Must specify laterality. |
| With Pyonephrosis | N13.6 | Pyonephrosis | Code in addition to N10 if acute infection is present. Often requires a code for obstruction (N13.2, N20.-). |
| With Renal Abscess | N15.1 | Renal and perinephric abscess | Code in addition to N10 if acute pyelonephritis is present. |
| In Pregnancy | O23.1- | ||
| (Specify trimester) | Infections of kidney in pregnancy | Do NOT use N10. This is a Chapter 15 code. Add B95-B97 for organism. | |
| Causing Sepsis | A41.5- | ||
| (Specify organism) | Sepsis due to other organism | Code first. Then code N10 for the underlying pyelonephritis. Add R65.21 for septic shock if present. | |
| As a Manifestation of another Disease (e.g., TB) | N16 | Renal tubulo-interstitial disorders in diseases classified elsewhere | Code first the underlying disease (e.g., A18.11). |
9. FAQs: Frequently Asked Questions on Pyelonephritis Coding
Q1: What is the difference between cystitis (N30.0) and pyelonephritis (N10)?
A: Cystitis is an infection limited to the bladder (lower UTI), while pyelonephritis is an infection of the kidney (upper UTI). Pyelonephritis is a more severe, systemic illness. The codes are distinct and should not be confused. If both are present, both can be coded.
Q2: Can I use N10 if the diagnosis is just “UTI” but the symptoms suggest pyelonephritis?
A: No. Coding must be based on physician documentation. You cannot assume a diagnosis based on symptoms or lab values. If the physician only documents “UTI,” you must code a bladder infection (N39.0). This is a prime scenario for initiating a physician query.
Q3: How do I code “recurrent” pyelonephritis?
A: “Recurrent” typically refers to repeated episodes of acute pyelonephritis. Each new episode should be coded as acute pyelonephritis (N10). There is no specific ICD-10 code for “recurrent” as a standalone diagnosis. If the recurrences have led to chronic kidney damage, then a code from the N11 category would be appropriate.
Q4: Is the organism code (B96.-) mandatory?
A: It is not mandatory for assigning the N10 code, but it is highly recommended and often required for accurate billing, antibiotic stewardship, and infection control reporting. Always add it if the organism is identified and documented.
Q5: What if the pyelonephritis is due to a multidrug-resistant organism (MDRO)?
A: You would first code the infection (e.g., N10), then the organism (B96.-), and then an additional code Z16.- (Resistance to antimicrobial drugs) to specify the type of resistance (e.g., Z16.11 for extended-spectrum beta-lactamase (ESBL) resistance).
10. Conclusion: The Synergy of Clinical Accuracy and Coding Precision
Accurate ICD-10 coding for pyelonephritis is a multifaceted process that demands a deep understanding of clinical medicine and coding guidelines. It requires moving beyond simple term-matching to a holistic interpretation of the patient record. The synergy between precise clinical documentation and expert coding is what drives accurate reimbursement, valid quality metrics, and reliable health data for research and public health initiatives. By mastering the nuances of laterality, acuity, associated conditions, and complex scenarios like sepsis, healthcare professionals ensure that the story told by the codes is the true story of the patient’s illness.
11. Additional Resources and References
-
-
Official Source: The ICD-10-CM Official Guidelines for Coding and Reporting, maintained by the Centers for Disease Control and Prevention (CDC) and the Centers for Medicare & Medicaid Services (CMS). https://www.cdc.gov/nchs/icd/icd-10-cm.htm
-
Clinical Reference: UpToDate, DynaMed, or other evidence-based clinical decision support tools for the latest clinical guidelines on pyelonephritis management.
-
Professional Organizations:
-
American Health Information Management Association (AHIMA): https://www.ahima.org
-
American Academy of Professional Coders (AAPC): https://www.aapc.com
-
-
Date: October 22, 2025
Author: Dr. Eleanor Vance, MD, MMM, CIC, CPC
Disclaimer: The information contained in this article is intended for educational and informational purposes only. It is not a substitute for professional medical coding, billing, or legal advice. Code assignment should be based on a thorough review of the patient’s medical record and the most current official coding guidelines. The author and publisher disclaim any liability arising directly or indirectly from the use of this information.






