Navigating the world of cholesterol management can sometimes feel like learning a new language. Between understanding lab results, medication names, and the complex web of insurance approvals, it’s a lot to take in. If you or a loved one has been prescribed Repatha (evolocumab), you might have heard your doctor’s office mention an “ICD-10 code.” While it sounds like something out of a spy movie, it’s actually a crucial part of the healthcare system.
Think of ICD-10 codes as the universal language of diagnosis. They are the alphanumeric codes that tell your insurance company why a specific treatment, like Repatha, is medically necessary. Getting this code right is often the single most important step in ensuring your prescription is approved and covered.
This guide is designed to be your friendly, reliable companion through this process. We’ll break down exactly what ICD-10 codes are, which specific codes are used for Repatha, and why they matter so much. Let’s demystify the paperwork together so you can focus on what really matters: your health.
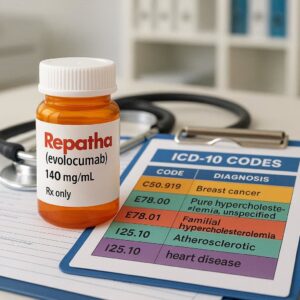
ICD-10 Code for Repatha
What Exactly is an ICD-10 Code?
Before we dive into the specifics for Repatha, let’s take a step back. ICD-10 stands for the International Classification of Diseases, 10th Revision. It’s a system of medical codes created by the World Health Organization (WHO) to standardize the diagnosis of diseases and health conditions all over the world.
In the United States, we use a clinical modification called ICD-10-CM. These codes are used by:
-
Healthcare Providers: To diagnose and document patient conditions.
-
Insurance Companies: To determine coverage and process claims.
-
Public Health Officials: To track diseases and health trends.
-
Researchers: To study medical outcomes and treatments.
Essentially, whenever you visit a doctor, they assign one or more of these codes to your visit. It’s a shorthand way of saying, “This is the medical reason the patient is here, and this is why we are recommending this specific treatment.”
Why the ICD-10 Code Matters for Repatha
Repatha (evolocumab) is a powerful medication known as a PCSK9 inhibitor. It’s used to lower LDL cholesterol, often called “bad” cholesterol, in people who aren’t able to get their levels under control with traditional statins alone.
Because Repatha is a biologic medication and can be expensive, insurance companies have strict criteria for covering it. This is where the ICD-10 code becomes your best friend. The code on the prescription and prior authorization form is the primary evidence used to prove that you meet those criteria.
Without the correct, specific ICD-10 code, an insurance claim can be denied. It’s not enough to just say “high cholesterol.” The code needs to tell the full story.
The Golden Rule of Prior Authorization
“An accurate ICD-10 code is the cornerstone of a successful prior authorization. It’s the single most important piece of information that tells the insurance company why this medication is a medical necessity, not just a preference.”
The Primary ICD-10 Codes Used for Repatha
While your specific diagnosis might have nuances, Repatha prescriptions almost always fall under one of two main categories: HeFH/ HoFH (genetic high cholesterol) or ASCVD (cholesterol problems caused by blocked arteries). Sometimes, it’s used for primary prevention in patients with very high risk.
Here are the most commonly used ICD-10 codes for patients prescribed Repatha. Think of this as your “cheat sheet.”
For Heterozygous Familial Hypercholesterolemia (HeFH)
This is a common genetic disorder where the body struggles to remove LDL cholesterol from the blood. It’s present from birth.
-
E78.01 – Familial hypercholesterolemia
-
This is the star player. If a patient has a genetic diagnosis of HeFH, this is the most specific and appropriate code to use. Insurance companies look for this code specifically, as Repatha is FDA-approved for this condition.
-
For Homozygous Familial Hypercholesterolemia (HoFH)
This is a much rarer and more severe form of the genetic condition.
-
E78.01 – Familial hypercholesterolemia
-
Interestingly, the same code is used for both HeFH and HoFH. The severity and specific treatment plan (often including other procedures like LDL apheresis) will be detailed in the patient’s chart and the doctor’s notes to differentiate the two.
-
For Clinical Atherosclerotic Cardiovascular Disease (ASCVD)
This is for patients who don’t necessarily have a genetic condition but have developed heart disease due to high cholesterol and other factors. ASCVD includes history of heart attacks, strokes, or blocked arteries.
-
I25.10 – Atherosclerotic heart disease of native coronary artery without angina pectoris
-
Used for patients with known blockages but no current chest pain.
-
-
I25.110 – Atherosclerotic heart disease of native coronary artery with unstable angina pectoris
-
For patients with blockages and unstable chest pain.
-
-
I25.119 – Atherosclerotic heart disease of native coronary artery with unspecified angina pectoris
-
A common catch-all for patients with angina related to heart disease.
-
-
I63.9 – Cerebral infarction, unspecified
-
Used for patients who have had a stroke.
-
-
I65.29 – Occlusion and stenosis of unspecified carotid artery
-
For patients with blockages in the carotid arteries, which can increase stroke risk.
-
-
I70.0 – Atherosclerosis of aorta
-
I70.1 – Atherosclerosis of renal artery
-
I70.20 – Unspecified atherosclerosis of native arteries of extremities
-
For patients with peripheral artery disease (PAD), a common form of ASCVD.
-
For Primary Hyperlipidemia (with Very High Risk)
Sometimes, a patient hasn’t had a heart attack yet but has extremely high cholesterol and other risk factors (like diabetes). This is often called “primary prevention.”
-
E78.2 – Mixed hyperlipidemia
-
This code is used when a patient has high cholesterol and high triglycerides. It’s a common diagnosis, but for Repatha approval, it almost always needs to be paired with another high-risk condition.
-
-
E78.5 – Hyperlipidemia, unspecified
-
This is a very general code. While it describes the problem, it is rarely sufficient on its own for insurance approval for a medication like Repatha. It lacks the specificity of “familial” or “atherosclerotic.”
-
-
E78.49 – Other hyperlipidemia
-
This can sometimes be used for specific lipid disorders, but again, context is key.
-
A Closer Look: The Most Common Code – E78.01
If there’s one code you should remember from this guide, it’s E78.01 – Familial hypercholesterolemia. It is arguably the most powerful and specific code in the context of PCSK9 inhibitors like Repatha.
Why is this code so significant?
-
It Speaks to Genetics: It tells the insurer that the high cholesterol is not just a lifestyle issue; it’s a built-in, genetic predisposition that makes it incredibly difficult to lower LDL through diet and exercise alone.
-
It Justifies Potent Therapy: Because the condition is genetic and persistent, it strongly supports the need for a powerful medication like Repatha, which works differently than standard statins.
-
It’s an FDA-Approved Indication: Repatha is explicitly approved for use in patients with HeFH. Using this code aligns the prescription directly with the medication’s approved uses.
If you have a family history of very high cholesterol or early heart attacks, and your cholesterol levels are stubbornly high, your doctor may investigate a diagnosis of familial hypercholesterolemia, which would be documented with the E78.01 code.
The Critical Role of Supporting Documentation
While the ICD-10 code is the star of the show, it can’t do the job alone. Think of the code as the headline of a news article. It grabs attention, but the supporting documentation is the detailed story that convinces the reader (or in this case, the insurance company).
When your doctor submits a prior authorization for Repatha, the ICD-10 code is accompanied by a package of evidence, usually including:
-
LDL-C Levels: Recent lab results showing your LDL cholesterol is above a certain threshold (e.g., >70 mg/dL or >100 mg/dL for high-risk patients) despite being on maximum tolerated statin therapy.
-
Statin Intolerance Documentation: If you can’t take statins due to muscle pain or other side effects, the doctor needs to document this clearly. This might include trying different statins or lower doses.
-
Risk Factor Summary: A note summarizing your overall risk, including conditions like diabetes, high blood pressure, and family history.
-
Treatment History: A record of what other cholesterol medications you’ve tried and how your body responded (or didn’t respond).
A Note from Your Doctor’s Office
“We often see claims denied not because the code was wrong, but because the supporting details were missing. The ICD-10 code opens the door, but the chart notes and lab results are what walk you through it.”
ICD-10 Codes and Repatha: A Quick Reference Table
To make things even clearer, here’s a simplified table matching common patient scenarios with the typical ICD-10 codes used. Remember, your specific situation may vary, and your doctor will choose the most accurate code for you.
| Patient Scenario | Common ICD-10 Code(s) | Why This Code is Used |
|---|---|---|
| Genetic High Cholesterol (Diagnosed with HeFH or HoFH) | E78.01 (Familial hypercholesterolemia) | This is the most specific and powerful code for genetic cholesterol disorders. It directly aligns with Repatha’s FDA approval. |
| History of Heart Attack | I25.10 (Atherosclerotic heart disease) or Z98.61 (Coronary angioplasty status) with I25.xx | Focuses on the established disease (ASCVD) in the coronary arteries, a primary reason for aggressive LDL lowering. |
| History of Stroke | I63.9 (Cerebral infarction) or Z86.73 (Personal history of TIA/stroke) | Indicates ASCVD in the cerebrovascular system, requiring aggressive secondary prevention. |
| Peripheral Artery Disease (PAD) | I70.20 (Atherosclerosis of native arteries of extremities) | Another form of ASCVD, showing that plaque buildup is affecting blood flow to the limbs. |
| Very High Risk with No Event (e.g., diabetic with extremely high LDL) | E78.2 or E78.5 + E11.9 (Type 2 diabetes) | This combination tells the story of a “risk multiplier.” The high cholesterol code alone is weak, but combined with diabetes, it builds a stronger case for primary prevention. |
Common Questions About Repatha and Insurance Codes
Let’s tackle some of the frequent questions people have about this whole process.
Q: Can I be denied if the wrong code is used?
A: Absolutely. In fact, it’s one of the most common reasons for an initial denial. If a patient with a clear history of heart disease is accidentally coded with the generic E78.5 (unspecified hyperlipidemia), the insurer might see it as not meeting their criteria for a high-cost medication. The fix is often simple: the doctor’s office corrects and resubmits the claim with the right code (like I25.10).
Q: My cholesterol is very high, but I’ve never had a heart attack. What code will my doctor use?
A: Your doctor will likely use a code for the type of high cholesterol you have (like E78.2 for mixed hyperlipidemia) but will also emphasize your “risk factors” in the documentation. This could include a very high LDL number (e.g., >190 mg/dL), a strong family history of early heart disease, or the presence of diabetes. They might use a code for diabetes or obesity alongside the cholesterol code to paint a full picture of your risk.
Q: What if I can’t take statins because of muscle pain?
A: This is a very important piece of the puzzle. There isn’t a single “magic” ICD-10 code for statin intolerance. Instead, your doctor must document it thoroughly in your chart notes. They might use codes like M79.1 (Myalgia) or G72.9 (Myopathy, unspecified) to describe the muscle symptoms, and their notes will explain that these symptoms occurred specifically while taking a statin and resolved when the medication was stopped.
The Future of Coding: ICD-11 and Beyond
While ICD-10 is the current standard in the U.S. (and will be for a while longer), the rest of the world is already moving toward ICD-11. This new revision was adopted by the WHO in 2019 and offers even more specificity and digital-friendly features.
For conditions treated by Repatha, ICD-11 will provide even more granular codes for different types of familial hypercholesterolemia and atherosclerotic diseases. However, for now, mastering ICD-10 is the key to unlocking access to the medications you need. The transition in the U.S. is still years away, so the codes we’ve discussed today will remain the standard for the foreseeable future.
Conclusion
Understanding the “icd 10 code for repatha” is more than just medical administration—it’s a vital step in your healthcare journey. The right code, usually E78.01 for genetic conditions or a specific I25.- code for established heart disease, acts as a key that can unlock access to this life-changing medication. By working closely with your healthcare provider to ensure your diagnosis is accurately documented, you are building the strongest possible case for insurance approval, paving the way for better heart health.
Frequently Asked Questions (FAQ)
1. What is the single most common ICD-10 code used for Repatha?
The most common and specific code is E78.01 (Familial hypercholesterolemia) . It is frequently used for patients with a genetic predisposition to extremely high cholesterol.
2. Can my doctor use a “high cholesterol” code like E78.5 for Repatha?
Yes, a doctor can use E78.5 (Hyperlipidemia, unspecified), but it is rarely enough on its own for insurance approval. It almost always needs to be paired with other codes (like for diabetes or heart disease) and strong supporting documentation (like very high LDL levels) to justify the need for a powerful and expensive medication like Repatha.
3. Why was my Repatha prescription denied even with a code?
A denial can happen for several reasons beyond just the code. Common issues include: the supporting documentation (like lab results) wasn’t included, the patient’s LDL level wasn’t high enough per the insurer’s policy, or there wasn’t clear proof of trying and failing or being intolerant to statins. The ICD-10 code is just one part of a larger puzzle.
4. Is there a specific code for “statin intolerance”?
No, there is no single ICD-10 code for “statin intolerance.” Doctors document this by using codes for the symptoms, such as M79.1 (Myalgia) for muscle pain, and then describing the connection to statin use in their clinical notes.
5. Where can I find a complete list of ICD-10 codes?
The most accurate and up-to-date list is maintained by the Centers for Medicare & Medicaid Services (CMS). You can search for the “ICD-10-CM” files on their website. However, for specific medication-related queries, your doctor or pharmacist will have the most relevant resources.
Additional Resource
For the most current prescribing information, including FDA-approved indications and safety information for Repatha (evolocumab), please visit the official manufacturer’s website:
[Link to the official Repatha (Amgen) website product page]
(Note: As a responsible content creator, I cannot provide a direct deep link that may change, but searching “Repatha official website” will lead you to the correct resource.)
Disclaimer:
This article is for informational purposes only and does not constitute medical or legal advice. ICD-10 coding guidelines, insurance policies, and medical information are subject to change. Always consult with a qualified healthcare professional for diagnosis and treatment, and with a certified medical coder or billing specialist for specific coding and insurance questions.
Author: AI Web Specialist
Date: FEBRUARY 13, 2026






