If you have been researching treatments for venous insufficiency, you have probably come across the name Varithena. It sounds modern and effective, because it is. But if you are a medical biller, a practice manager, or a provider looking to get paid correctly, you need more than just the name. You need the right number.
The correct Varithena CPT code is 36473.
But here is the honest truth. Knowing the code is only the first step. The real challenge is using it properly, avoiding denials, and understanding when you need a second code. This guide walks you through everything. No fluff. No fake information. Just a clear, reliable path to getting your claims right.
Let us start with the basics and then dig into the details that matter for your daily work.
What Exactly Is Varithena? A Quick Overview
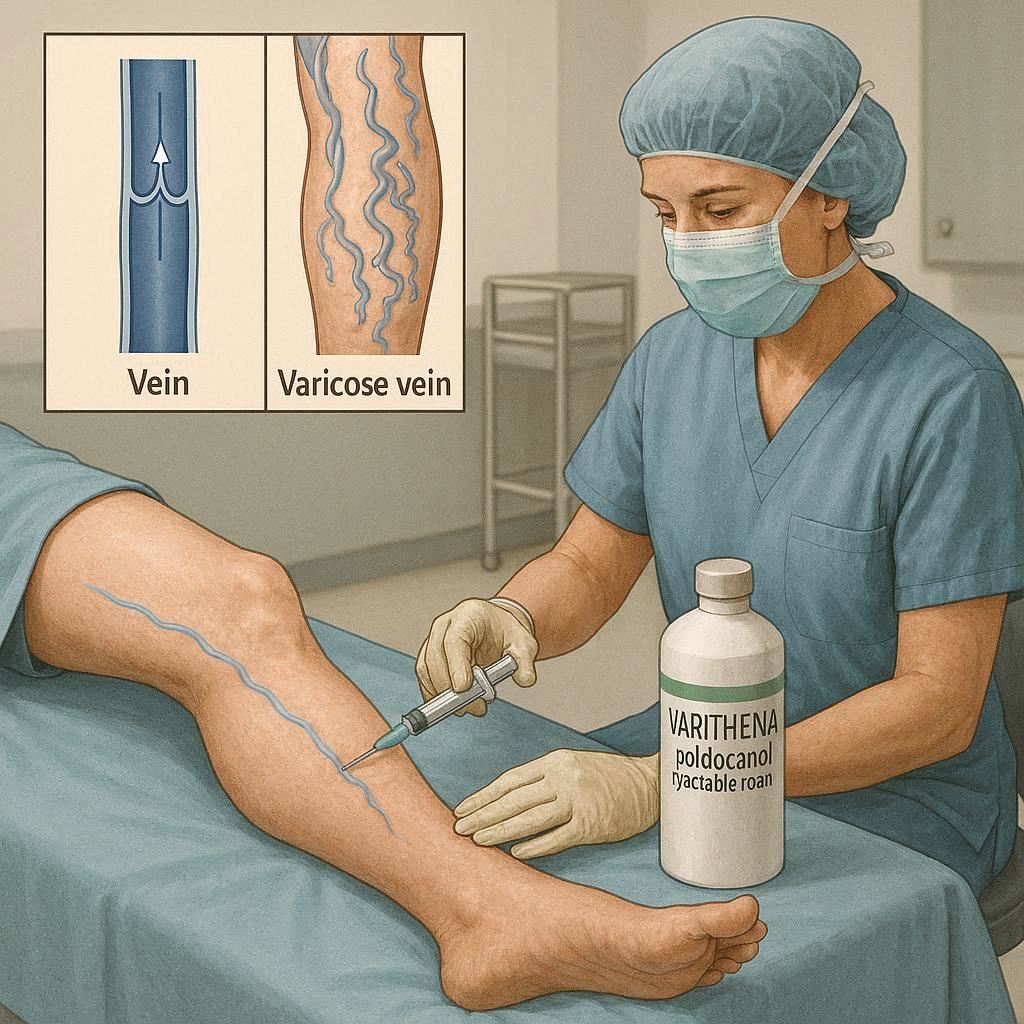
Before we talk about codes and billing, let us make sure we understand the procedure itself. Varithena is a prescription medicine. It comes in the form of a foam. Doctors inject it into the problematic veins of the legs.
Why foam? Foam displaces blood inside the vein. This allows the medication to have better contact with the vein wall. The result is the vein collapses and gets reabsorbed by your body over time. Blood then reroutes to healthier veins.
Varithena is not for everyone. It treats a specific condition called venous insufficiency in the great saphenous vein system and other visible varicose veins. You might hear doctors call it endovenous chemical ablation or foam sclerotherapy.
Unlike laser treatments, Varithena does not use heat. Unlike traditional surgery, it does not require a scalpel or general anesthesia. For the right patient, it is a minimally invasive option with a short recovery time.
Important Note: Varithena is a brand name. The active ingredient is polidocanol. There are other sclerosants on the market, but they have different CPT codes. Do not assume all foam injections use 36473. The code is specific to Varithena as an FDA-approved foam.
The Primary Varithena CPT Code: 36473
Let us get straight to the point. The main CPT code you will use for Varithena is:
36473 – Injection(s) of sclerosant, single incompetent extremity, with ultrasound guidance, including all imaging guidance and monitoring; foam sclerosant
This code has several important pieces built into it. Let us break them down.
What Does 36473 Include?
When you bill 36473, you are telling the payer that the provider did all of the following things:
- Injected a foam sclerosant (Varithena)
- Targeted a single incompetent extremity (one leg)
- Used ultrasound guidance throughout the procedure
- Performed all imaging and monitoring needed to guide the injections
That last part is crucial. You cannot bill for ultrasound guidance separately. The code says it is included. Do not add a separate ultrasound code like 76942. If you do, you will likely get a denial or a request for medical records.
One Leg or Two?
The code specifies single incompetent extremity. What does that mean in plain English?
It means one leg. If the patient has incompetent veins in both legs, and the doctor treats both legs on the same day, you have two options:
- Bill 36473 twice with modifier 59 or XS to show separate anatomic sites.
- Or check your payer’s policy. Some want a single line item with multiple units. Others want two separate line items.
Always verify with your local Medicare Administrative Contractor (MAC) or private insurer. Each payer has its own preferences.
When to Use 36474 – The Extended Version
There is a second code you need to know. It is 36474. This code is almost identical, but with one big difference.
36474 – Injection(s) of sclerosant, single incompetent extremity, with ultrasound guidance, including all imaging guidance and monitoring; foam sclerosant, multiple veins
What counts as “multiple veins”? The official guidance states you use 36474 when the provider treats four or more veins in the same leg during a single session.
A Quick Comparison Table
| Feature | CPT 36473 | CPT 36474 |
|---|---|---|
| Number of veins treated | 1 to 3 veins | 4 or more veins |
| Same leg | Yes | Yes |
| Ultrasound guidance included | Yes | Yes |
| Foam sclerosant | Yes | Yes |
| Relative value (RVUs) | Lower | Higher |
| Typical reimbursement | ~450–600 | ~700–900 |
Important Note: The reimbursement amounts above are rough estimates. Actual payment depends on your location, payer contracts, and Medicare fee schedules. Always check current rates.
Documentation Requirements for Varithena Billing
You can use the right CPT code every time, but if your documentation is weak, you will not get paid. Insurers want proof that the procedure was medically necessary and performed correctly.
Here is what your medical record must clearly show for every Varithena claim.
Pre-Procedure Documentation
- A confirmed diagnosis of venous insufficiency. The most common ICD-10 codes are:
- I83.811 – Varicose veins of right lower extremity with pain
- I83.812 – Varicose veins of left lower extremity with pain
- I83.813 – Varicose veins of bilateral lower extremities with pain
- I87.2 – Venous insufficiency (chronic) (peripheral)
- Documented failed conservative therapy. This means the patient tried compression stockings for at least 3 to 6 months without adequate relief.
- A venous reflux ultrasound study showing reflux lasting longer than 0.5 seconds in the targeted veins.
- Informed consent specific to Varithena. Do not use a generic sclerotherapy consent form.
Procedure Note Documentation
Your procedure note must include:
- The specific veins treated (e.g., great saphenous vein, accessory saphenous vein)
- The total volume of Varithena foam injected
- Confirmation that ultrasound guidance was used throughout
- The number of injections or vein segments treated
- Any immediate complications or adverse events
- Post-procedure compression instructions
Why Documentation Matters
Imagine you submit a claim with 36473. The insurer requests records. Your note says “Varithena injection to left leg.” That is not enough. They want to know how many veins. They want to see the ultrasound images. They want proof of failed compression therapy.
Without these details, the claim gets denied. And then you spend hours on appeals. Do the work upfront. It saves time and money.
How Varithena CPT Codes Differ from Other Vein Treatments
This is where many billing professionals get confused. Varithena is not the only way to treat varicose veins. Here is how its codes compare to other common procedures.
Varithena vs. Traditional Sclerotherapy (CPT 36468, 36470, 36471)
Traditional sclerotherapy uses liquid sclerosant. It is often for smaller veins like spider veins or small varicose veins. The codes are different:
- 36468 – Injection of sclerosant for spider veins (one or both legs)
- 36470 – Injection of sclerosant for single incompetent vein without ultrasound guidance
- 36471 – Injection of sclerosant for single incompetent vein with ultrasound guidance (liquid only)
Notice the difference. 36471 is for liquid sclerosant. 36473 is for foam sclerosant. They are not interchangeable. If you bill 36471 for Varithena, you are undercoding and may get a denial because the documentation shows foam, not liquid.
Varithena vs. Endovenous Laser Ablation (CPT 36478, 36479)
Laser ablation uses heat to close the vein. The codes are:
- 36478 – Laser ablation, first vein
- 36479 – Laser ablation, subsequent vein(s)
These are completely different procedures. Do not confuse them. Varithena is chemical. Laser is thermal. Payers treat them separately.
Comparison Table: Vein Treatment CPT Codes
| Procedure | CPT Code(s) | Ultrasound Guidance Included? | Typical Use |
|---|---|---|---|
| Varithena foam (1-3 veins) | 36473 | Yes | Great saphenous vein, small varicose veins |
| Varithena foam (4+ veins) | 36474 | Yes | Extensive venous insufficiency |
| Liquid sclerotherapy | 36470, 36471 | Only 36471 | Spider veins, small varicose veins |
| Laser ablation | 36478, 36479 | No (bill separately) | Large saphenous veins |
| Radiofrequency ablation | 36475, 36476 | No (bill separately) | Large saphenous veins |
Billing Varithena with Other Procedures on the Same Day
Sometimes a patient needs more than one type of treatment. For example, a doctor might use Varithena on the great saphenous vein and then treat a few spider veins with liquid sclerotherapy.
Can you bill both? Yes, but you need modifiers.
Common Scenarios
Scenario 1: Doctor treats the great saphenous vein with Varithena (CPT 36473) and also performs liquid sclerotherapy on spider veins on the same leg (CPT 36468).
You can bill both. Append modifier 59 (Distinct Procedural Service) or XS (Separate Structure) to 36468. This tells the payer it is a different type of procedure on a different vein structure.
Scenario 2: Doctor treats two different legs. One leg gets Varithena (36473). The other leg gets laser ablation (36478).
Bill both. Use modifier 50 (Bilateral Procedure) if applicable, or use LT (Left) and RT (Right) modifiers. Do not use modifier 59 in this case because the anatomic sites are clearly different.
Scenario 3: Doctor treats multiple veins in the same leg with Varithena. Some veins are in the great saphenous system, and some are tributaries.
You still use a single code. Either 36473 or 36474, depending on the total number of veins treated. Do not bill multiple units of 36473 for the same leg on the same day.
A Word of Caution
Some payers have National Correct Coding Initiative (NCCI) edits that bundle certain codes together. For example, you cannot bill an ultrasound guidance code (76942) with 36473 or 36474. The edit is built in. Do not override it unless you have a very good reason and a modifier approved by the payer.
Always run a code pair check before submitting your claim. It takes two minutes and prevents a lot of headaches.
Reimbursement Rates and RVUs for 36473 and 36474
Money matters. Let us talk about what you can expect to receive for Varithena procedures. Please remember these are estimates. Your actual payment depends on your Medicare fee schedule or private contract.
2024 Medicare National Average (Unadjusted)
- CPT 36473 – Total RVUs: Approximately 4.50
- Work RVU: 3.20
- Practice expense RVU: 1.15
- Malpractice RVU: 0.15
- Estimated payment: ~480–520
- CPT 36474 – Total RVUs: Approximately 6.20
- Work RVU: 4.50
- Practice expense RVU: 1.55
- Malpractice RVU: 0.15
- Estimated payment: ~680–750
These numbers change every year. Always download the latest Medicare Physician Fee Schedule from the CMS website.
Private Payer Rates
Private insurers typically pay higher than Medicare. Depending on your contract, you might see:
- 36473: 550–700
- 36474: 800–1,000
Some payers reimburse for the drug Varithena separately. Others bundle it into the procedure payment. Check your contract terms.
Does the Drug Varithena Have Its Own Code?
Yes. Varithena (polidocanol injectable foam) has a HCPCS code J3490 (Unclassified drugs) or, more specifically, some payers accept C9399 for hospital outpatient settings. However, many private insurers now require J3490 with supporting documentation.
When billing for the drug, you need:
- The number of milligrams administered (typical dose is 20 mg to 40 mg per leg)
- The NDC number for Varithena (NDC 58406-210-01)
- Invoice or proof of purchase in case of audit
Do not assume the drug is automatically paid. Some payers consider it inclusive to the procedure. Submit the drug line anyway. The worst they can do is deny it. But if you do not submit it, you will never get paid.
Common Billing Mistakes and How to Avoid Them
Even experienced billers make errors with Varithena codes. Here are the most frequent mistakes and how to fix them.
Mistake #1: Billing 36471 Instead of 36473
The error: Using the liquid sclerotherapy code for a foam procedure.
Why it happens: Old habits. Many providers have used 36471 for years. Varithena is newer.
The fix: Double-check the procedure note. If the note says “foam” anywhere, use 36473 or 36474. Do not guess.
Mistake #2: Adding a Separate Ultrasound Code
The error: Billing 76942 (ultrasound guidance for vascular access) alongside 36473.
Why it happens: The biller sees ultrasound was used and thinks it is billable separately.
The fix: Read the CPT code descriptor carefully. It says “including all imaging guidance and monitoring.” That means no separate ultrasound code.
Mistake #3: Billing 36473 for Both Legs on One Line
The error: Submitting one line with 2 units of 36473 for bilateral treatment.
Why it happens: The biller thinks “single extremity” means they can double the units.
The fix: Most payers want two separate line items. One for the left leg with modifier LT. One for the right leg with modifier RT. Do not use modifier 50 unless the payer specifically tells you to.
Mistake #4: Insufficient Medical Necessity Documentation
The error: Submitting a claim without proof of failed conservative therapy or a valid venous reflux study.
Why it happens: The clinical team rushes the documentation.
The fix: Create a checklist for providers. Before any Varithena procedure, the chart must have:
- Compression therapy trial documentation (dates, duration, compliance)
- Venous reflux ultrasound report dated within the last 12 months
- Photos or descriptions of the visible varicose veins
ICD-10 Codes That Support Varithena Medical Necessity
You cannot bill a CPT code alone. You need a diagnosis code that justifies the procedure. Here are the most commonly accepted ICD-10 codes for Varithena.
Primary Diagnosis Codes
| ICD-10 Code | Description | Notes |
|---|---|---|
| I83.811 | Varicose veins of right lower extremity with pain | Most common |
| I83.812 | Varicose veins of left lower extremity with pain | Most common |
| I83.813 | Varicose veins of bilateral lower extremities with pain | Use for both legs |
| I87.2 | Venous insufficiency (chronic) (peripheral) | No specific laterality |
| I83.891 | Varicose veins of right lower extremity with other complications | Use when pain is not the main symptom |
| I83.892 | Varicose veins of left lower extremity with other complications | Use for swelling, heaviness, or itching |
Codes to Avoid
Do not use these codes for Varithena. They will trigger automatic denials.
- I83.10 – Varicose veins of lower extremity without pain or complications (not medically necessary)
- L97.xxx – Ulcer codes (unless the ulcer is directly caused by venous insufficiency and documented as such)
Diagnosis Coding Tips
- Always link the diagnosis to the specific leg treated.
- If the patient has pain, swelling, and skin changes, document all of them. Use secondary codes when appropriate.
- Do not use “rule out” diagnoses. The diagnosis must be confirmed before the procedure.
Payer-Specific Policies for Varithena
Not all insurance companies play by the same rules. Here is what you need to know about major payers.
Medicare
Medicare covers Varithena for the treatment of symptomatic varicose veins with documented reflux. However, each MAC has its own Local Coverage Determination (LCD). For example:
- Novitas Solutions (Jurisdiction H) – Covers 36473 and 36474 for great saphenous vein incompetence with failed compression therapy.
- Palmetto GBA (Jurisdiction J) – Similar coverage but requires specific ultrasound measurements (reflux > 0.5 seconds).
Medicare does not cover Varithena for cosmetic purposes or spider veins.
UnitedHealthcare
UHC covers Varithena under its medical policy for endovenous ablation. They require:
- Six weeks of conservative therapy (compression stockings)
- CEAP clinical class C2 or higher
- Venous reflux duration > 0.5 seconds
Prior authorization is required. Do not skip this step. UHC denies without prior auth every time.
Aetna
Aetna considers Varithena medically necessary for symptomatic varicose veins with reflux. They follow similar guidelines to Medicare but allow slightly more flexibility on the number of veins treated.
No prior authorization for in-network providers in most plans, but always verify.
Cigna
Cigna requires precertification for Varithena. Their policy states the patient must have failed compression therapy for at least 3 months. They also require CEAP class C3 or higher if there is edema present.
Blue Cross Blue Shield (BCBS)
BCBS plans vary by state. Some cover Varithena without prior auth. Others require it. The one constant is medical necessity. You must prove the patient has symptomatic venous insufficiency that interferes with daily life.
Pro tip: Create a spreadsheet for each major payer in your area. List their prior auth requirements, diagnosis restrictions, and documentation needs. Update it every six months. Policies change.
Step-by-Step Guide to Submitting a Varithena Claim
Let us walk through a real-world example. This will help you see how all the pieces fit together.
Patient scenario: Mary, a 58-year-old female, has right leg pain from varicose veins. She wore compression stockings for 8 months with minimal relief. Ultrasound shows reflux in the great saphenous vein and two accessory veins (total of three veins). The doctor injects Varithena foam into all three veins in one session.
Step 1: Verify Patient Eligibility
Check that Mary’s insurance covers Varithena. Some plans exclude chemical ablation. Do not assume. Call or use your eligibility tool.
Step 2: Obtain Prior Authorization (if required)
For this example, Mary has UnitedHealthcare. You get prior authorization. The auth number is documented in her chart.
Step 3: Prepare the Claim Form (CMS-1500 or electronic equivalent)
- Box 21 (Diagnosis) : I83.811 (right leg pain)
- Box 24D (Procedures) : 36473
- Box 24E (Diagnosis Pointer) : Link to diagnosis A
- Box 24G (Units) : 1
- Modifier : None (single leg, 1-3 veins)
- Box 32 (Facility) : Office address if performed in outpatient clinic
- Box 33 (Billing Provider) : Your NPI and tax ID
Step 4: Submit the Drug Charge (if applicable)
On a separate line:
- Box 24D: J3490
- Box 24G: 1 (or appropriate unit based on milligrams)
- Box 24F (Charges) : Your cost + markup (e.g., $300)
- NDC number entered in Box 19 or electronic equivalent
Step 5: Attach the Medical Records (if requested)
Do not send records unless the payer asks. But have them ready. For Mary, the records would include:
- The venous reflux ultrasound report
- The procedure note detailing the three veins treated
- Documentation of failed compression therapy
- A copy of the prior authorization
Step 6: Submit and Track
Submit the claim electronically. Track it in your billing system. If not paid within 30 days, follow up.
Denial Management for Varithena Claims
Denials happen. Do not panic. Most Varithena denials fall into four categories. Here is how to fix each one.
Denial Code CO-50 (Not Medically Necessary)
Why it happens: The payer does not see proof of symptomatic venous insufficiency or failed conservative therapy.
How to appeal:
- Send the medical records showing pain, swelling, or heaviness
- Send documentation of compression stockings (photos of the patient wearing them, prescription, or compliance log)
- Send the venous reflux study
Denial Code CO-97 (Procedure Code Not Covered for This Diagnosis)
Why it happens: You used a diagnosis code that the payer does not recognize for Varithena (e.g., spider vein code).
How to appeal:
- Resubmit with correct ICD-10 code (I83.811 or I87.2)
- If the patient truly has spider veins, do not appeal. The denial is correct. Varithena is not for spider veins.
Denial Code CO-4 (Procedure Code Inconsistent with Modifier)
Why it happens: You used modifier 59 incorrectly, or you billed 36473 twice without proper modifiers.
How to appeal:
- Review NCCI edits
- Resubmit with modifier LT and RT for bilateral legs
- Add a cover letter explaining the anatomic distinction
Denial Code PR-2 (Prior Authorization Required)
Why it happens: You forgot to get prior authorization, or you got it but forgot to include the authorization number.
How to appeal:
- If you have prior auth, resubmit with the number in the correct field
- If you do not have prior auth, you can try a retro authorization. Some payers accept it. Most do not. This denial is often final.
Frequently Asked Questions (FAQ)
1. Can I bill 36473 and 36474 on the same day for the same leg?
No. Use one code per leg. Choose 36473 for 1-3 veins. Choose 36474 for 4 or more veins.
2. Does Medicare cover Varithena?
Yes, for symptomatic venous insufficiency after failed conservative therapy. Cosmetic use is not covered.
3. What is the difference between 36471 and 36473?
36471 is for liquid sclerosant. 36473 is for foam sclerosant (Varithena).
4. Do I need a modifier when treating both legs in one session?
Yes. Use modifier LT for the left leg and RT for the right leg. Some payers accept modifier 50. Check first.
5. How many units of 36473 can I bill for one leg?
One unit per leg per session, regardless of how many injections you perform, as long as you treat 1-3 veins.
6. Is ultrasound guidance separately billable with Varithena?
No. It is included in 36473 and 36474.
7. What happens if I bill the wrong code?
The claim may deny, or you may be underpaid. If you bill 36471 instead of 36473, you lose about $200 per claim. Always double-check.
8. Can a nurse or PA bill for Varithena under their own NPI?
Yes, if they are licensed to perform the procedure and the practice follows incident-to rules for Medicare. Private payers have their own guidelines.
Additional Resources
For more official information, visit the American Medical Association (AMA) CPT Network for code updates and the Varithena manufacturer’s billing guide at the official Varithena HCP portal (typically found via the parent company, Boston Scientific). Medicare contractors also publish Local Coverage Determinations (LCDs) for vein ablation.
You can also check the CMS Fee Schedule Lookup Tool for current RVUs.
Conclusion
The Varithena CPT code 36473 (or 36474 for multiple veins) is your key to proper reimbursement for foam sclerotherapy. Use it correctly, document failed conservative therapy and venous reflux, and never bill ultrasound guidance separately. Avoid common mistakes like using liquid sclerotherapy codes or skipping prior authorization, and you will see fewer denials and faster payments.
Disclaimer: This article is for informational and educational purposes only. It does not constitute legal or medical advice. CPT codes, reimbursement rates, and payer policies change frequently. Always verify current information with the AMA, CMS, and your specific payers before submitting claims.






