If you have ever been told that your teeth feel loose, or if you have suffered a dental injury, your dentist might have mentioned a procedure called splinting. It sounds a bit technical, and when you look at your treatment plan, you will likely see a specific code listed next to it.
Understanding what that code means can help you understand what the dentist is actually planning to do. It also helps you communicate with your insurance company and get a clear picture of the costs involved.
In this guide, we are going to walk through everything you need to know about the dental code for splinting teeth. We will break down the difference between the two main codes, explain when each one is used, and discuss what you can expect during the procedure. Whether you are a patient trying to decipher a bill or someone in the dental field looking for a refresher, this article is for you.
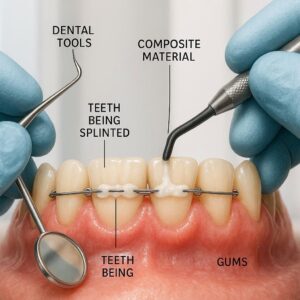
Dental Code for Splinting Teeth
What Is Dental Splinting?
Before we dive into the specific codes, let’s talk about what splinting actually is. In simple terms, dental splinting is a technique used to connect two or more loose teeth together. By joining them, the dentist creates a single, more stable unit. This shared support helps stabilize the teeth, allowing the surrounding tissues—like the gums and bone—to heal.
Think of it like a picket fence. If one post is loose, it wobbles. If you nail that loose post to the sturdy posts next to it, the whole section becomes stable again. Dental splinting works on the same principle.
There are two main reasons why a dentist might recommend this. The first is trauma. If you take a blow to the mouth during sports or an accident, one or more teeth can become loosened. Splinting them gives the supportive ligaments and bone a chance to heal properly. The second reason is periodontal disease. This is a chronic infection of the gums and bone that support your teeth. As the disease progresses, it destroys the bone, leading to increased tooth mobility. Splinting can help manage this mobility and improve comfort.
The Official Dental Codes for Splinting
In the world of dentistry, we use a standardized system called the Current Dental Terminology (CDT) code set. This is maintained by the American Dental Association (ADA). Every procedure a dentist performs has a unique code that is used for billing and record-keeping.
When it comes to splinting teeth, there are two primary codes you will encounter:
-
D4320
-
D4321
These two codes are specifically designated for “provisional splinting.” The keyword here is provisional. This means the splint is intended to be a temporary or semi-permanent solution. It is not a permanent restoration like a crown or a bridge. The goal is to stabilize the teeth for a period of time to allow for healing or as part of a long-term treatment plan.
Let’s explore the difference between these two codes.
D4320: Splinting – Intracoronal
The first code, D4320, is defined as “provisional splinting – intracoronal.” This term describes a splint that is placed inside the structure of the tooth.
To place an intracoronal splint, the dentist must prepare the teeth by creating small channels or grooves within the chewing surface or the back of the teeth. These channels are carefully cut into the enamel and dentin. Then, a strong material—often a fiber-reinforced composite or a metal wire—is laid into these channels and bonded in place with dental composite (white filling material).
Key characteristics of D4320:
-
Invasive: It requires the dentist to cut into the tooth structure. This is irreversible. Once the grooves are made, they must be filled.
-
Aesthetic: Because the material sits within the tooth, it can be very natural-looking, especially if the splint is placed on the back (lingual) side of the teeth.
-
Strong: The mechanical lock of the material within the tooth provides a very strong and rigid connection.
This code is typically used when a patient needs a very rigid, long-term provisional splint. It is common in cases of severe mobility or when the splint is intended to last for several months or even years as a permanent provisional solution.
D4321: Splinting – Extracoronal
The second code, D4321, is defined as “provisional splinting – extracoronal.” As the name suggests, this splint is placed on the outside of the tooth.
With an extracoronal splint, the dentist does not cut into the tooth. Instead, they clean and condition the outer surface of the enamel. Then, they apply a bonding agent and a splinting material—usually a fiber-reinforced ribbon or a wire—directly onto the surface of the teeth. This is then covered with a layer of composite resin to secure it and make it smooth.
Key characteristics of D4321:
-
Non-Invasive: This procedure is reversible. Since no tooth structure is removed, the splint can be removed later, and the teeth are left essentially as they were before.
-
Aesthetic Challenge: Because the material sits on the surface, it can be more visible, especially if placed on the front teeth. However, modern fiber-reinforced composites are very translucent and can be quite aesthetic.
-
Good for Short-Term Use: This is often the preferred method for post-traumatic splinting, where the goal is to stabilize the teeth for a few weeks while the periodontal ligament heals.
D4320 vs. D4321: A Comparison
Choosing between these two codes depends entirely on the clinical situation. Is the splint meant to be a short-term, reversible support? Or is it a longer-term measure to manage chronic mobility?
To help you visualize the differences, here is a comparison table:
| Feature | D4320 (Intracoronal) | D4321 (Extracoronal) |
|---|---|---|
| Definition | Provisional splinting – intracoronal | Provisional splinting – extracoronal |
| Tooth Preparation | Requires cutting grooves or channels into the tooth | No cutting of tooth structure; surface is etched |
| Invasiveness | Irreversible | Reversible |
| Strength | Very high; mechanically locked | High; dependent on adhesive bond to enamel |
| Aesthetics | Excellent; materials are hidden within the tooth structure | Good to excellent; depends on placement (lingual vs. facial) |
| Typical Use | Long-term provisional splinting for periodontal cases | Short-term post-traumatic splinting |
| Removal | Requires drilling to remove splint and fill grooves | Can be polished off with minimal to no damage |
When Is Splinting Necessary?
Dentists do not recommend splinting lightly. It is a procedure that adds maintenance complexity for the patient. You now have multiple teeth connected, which means flossing requires a special technique (using a floss threader). So, why would a dentist recommend it?
Post-Trauma Stabilization
This is the most common scenario for D4321. If you are in a car accident, fall, or sports injury, teeth can become luxated (displaced) or avulsed (knocked out). If a tooth is still in the socket but is extremely loose, splinting it to its neighbors provides the necessary immobility for the tissues to heal.
In these cases, the splint is usually left in place for 2 to 4 weeks. The goal is not permanent stabilization, but rather to act as a cast, similar to what you would put on a broken bone. After the healing period, the dentist will remove the splint, and the teeth should be stable on their own.
Periodontal Disease Management
Periodontitis is a leading cause of tooth loss. As the disease progresses, it destroys the alveolar bone—the bone that holds your teeth in place. When you lose bone support, teeth start to drift and become mobile. This mobility can make chewing difficult and uncomfortable.
In these cases, a dentist or periodontist (a gum specialist) might recommend splinting as part of a comprehensive periodontal treatment plan. This is often where you will see D4320 used.
The splint does not cure the periodontal disease. It simply manages the symptom of mobility. By connecting the teeth, the forces of chewing are distributed across a broader area. This reduces the stress on the individual teeth that have lost bone support.
Important Note for Patients: Splinting is not a standalone treatment for gum disease. It should always be accompanied by active periodontal therapy, such as scaling and root planing (deep cleaning), to control the infection. Without controlling the disease, the bone loss will continue, and eventually, the splinted teeth will fail as a unit.
The Splinting Procedure: What to Expect
Whether your dentist uses code D4320 or D4321, the process is generally straightforward and can usually be completed in one appointment.
Step 1: Anesthesia
Depending on the extent of the splint and whether tooth preparation is required, your dentist may or may not use a local anesthetic. For D4321 (extracoronal), anesthesia is often not needed. For D4320 (intracoronal), it is standard to numb the area to ensure your comfort during the preparation of the grooves.
Step 2: Preparation
For D4320, the dentist uses a high-speed handpiece to create small channels in the teeth. These are usually placed on the back (lingual) side of the teeth so they are not visible when you smile.
For D4321, the dentist will clean the teeth and then “etch” the enamel with a mild acid. This creates a rough surface at a microscopic level, which is essential for the bonding material to adhere strongly.
Step 3: Bonding and Placement
This is where the magic happens. A bonding agent is applied to the prepared teeth or the etched enamel. Then, the splinting material—which is often a flexible ribbon of glass fibers—is placed.
The dentist carefully positions the ribbon to ensure it is passive. This means it does not pull the teeth out of alignment. The teeth must be in their natural, correct position before the splint is cured. Once everything is in place, the dentist uses a special curing light to harden the composite resin that encases the ribbon.
Step 4: Finishing
After the material is hard, the dentist will smooth and polish the splint. They will check your bite (occlusion) to make sure the splint does not interfere with how your teeth come together when you close your mouth. A high spot on a splint can cause discomfort or even fracture the material.
Insurance Coverage and Reimbursement
One of the most confusing aspects for patients is understanding how insurance handles the dental code for splinting teeth. Unfortunately, it is not always straightforward.
Medical vs. Dental Insurance
This is the first question. If the splinting is due to an accident or trauma, the procedure may be covered under your medical insurance, not your dental insurance. Medical insurance often covers emergency procedures and trauma care. If you were in a car accident, for example, the dental splinting should be billed to your auto insurance or medical plan.
If the splinting is due to periodontal disease, it falls under dental insurance.
Dental Insurance Policies
Even under dental insurance, coverage varies widely.
-
Periodontal Splinting: Many dental insurance plans classify splinting as a “periodontal” service. If your plan has a separate deductible or annual maximum for periodontal services, that will apply. Some plans cover 50% of the cost, while others may cover 80%.
-
Frequency Limitations: Some plans limit how often a splint can be placed. For example, they may only cover a splint once every 3 to 5 years.
-
Alternative Benefits: This is a common insurance concept. If your insurance plan covers a partial denture or a bridge to replace missing teeth, they may argue that a splint is a “lesser” procedure and only pay the cost of the alternative. This is a complex area that your dentist’s billing coordinator can help navigate.
Typical Costs
Without insurance, the cost for splinting can range significantly based on the number of teeth involved, the geographic location, and the complexity of the case.
-
D4321 (Extracoronal): For a simple splint of 2-4 teeth, you might expect a fee ranging from $300 to $800.
-
D4320 (Intracoronal): Because this is more technique-sensitive and involves irreversible tooth preparation, the fee is typically higher, often ranging from $500 to $1,200 or more for a segment of teeth.
It is crucial to remember that these codes are billed per tooth or per segment. The CDT code descriptors often allow for the code to be reported for each tooth splinted, or for the entire arch. Your dentist’s office should provide a clear treatment plan with a breakdown of the total fee.
Alternatives to Dental Splinting
Splinting is not the only option for dealing with mobile teeth. Depending on your specific situation, your dentist might discuss one of these alternatives.
Orthodontic Treatment
If the mobility is caused by a traumatic bite (where some teeth are hitting harder than others), orthodontics can redistribute the forces evenly. Braces or clear aligners can move teeth into a more stable position where they are supported by bone and have proper contacts with opposing teeth.
Occlusal Adjustment
Sometimes, a simple solution is to adjust the biting surfaces of the teeth. This is called occlusal equilibration. By selectively reshaping the enamel, the dentist can eliminate “interferences” that cause certain teeth to take too much force when you chew or grind your teeth.
Nightguard (Occlusal Guard)
If the mobility is due to bruxism (teeth grinding and clenching), a nightguard is often the first line of defense. This custom-made appliance creates a barrier between the teeth, absorbs the forces of grinding, and protects the teeth and their supporting structures from excessive trauma.
Extraction and Replacement
In severe cases where the bone loss is extreme and the prognosis (long-term outlook) for the tooth is hopeless, it may be better to extract the tooth. Leaving a hopeless tooth in a splint can put the adjacent healthy teeth at risk. After extraction, the missing tooth can be replaced with a dental implant, bridge, or partial denture.
Long-Term Care and Maintenance
If you have a dental splint, your home care routine will change. It is not difficult, but it requires diligence.
Cleaning Your Splint
The biggest challenge with a splint is cleaning between the teeth. Because the teeth are now connected, dental floss cannot pass through the contact point.
You will need to use a floss threader. This is a small, flexible plastic loop. You thread your floss through the loop, then pass the loop under the splint and between the teeth. You can then floss the area normally.
Alternatively, you can use superfloss. This type of floss has a stiff end, a spongy middle section, and regular floss. The stiff end is used to thread the floss under the splint.
Other helpful tools include:
-
Water Flossers: A water flosser (like Waterpik) is excellent for flushing out food debris and bacteria from underneath the splint and around the gumline.
-
Interdental Brushes: Small, conical brushes can be used to clean the spaces between the teeth and around the splint material.
Professional Maintenance
You will need to see your dentist or hygienist more frequently for maintenance. A splint creates a “plaque trap”—an area where bacteria can easily accumulate. Professional cleanings every 3 to 4 months are often recommended to prevent decay (cavities) on the splinted teeth and to manage gum inflammation.
A Note on Accuracy and Realistic Expectations
It is important to be honest about the outcomes of splinting. While it can be an excellent procedure for stabilizing teeth, it is not a cure-all.
For post-traumatic cases, the success rate is high. The teeth often return to normal stability after the splint is removed.
For periodontal cases, the success depends entirely on the patient’s ability to control the disease. If you continue to have active gum disease, the bone loss will continue. The splint will hold the teeth together, but if the bone is gone, the splinted unit will eventually loosen as a group.
The codes D4320 and D4321 are specifically for provisional splinting. If the splint is intended to be a permanent, definitive solution, there are other codes for fixed partial dentures (bridges) or other restorations. A provisional splint is considered a treatment aid, not a final restoration.
Frequently Asked Questions (FAQ)
1. Is splinting teeth painful?
The procedure itself is usually not painful, especially if local anesthesia is used. You may experience some soreness in the gums and teeth for a few days after the procedure as the tissues adjust to the new stability. Over-the-counter pain relievers are usually sufficient to manage this.
2. How long does a dental splint last?
This depends on the type of splint and why it was placed. A post-traumatic splint (D4321) is typically removed in 2 to 6 weeks. A long-term periodontal splint (often D4320) can last for several years if maintained properly, but it is still considered provisional and may eventually need to be replaced or converted into a permanent bridge.
3. Can I eat normally with a splint?
You will need to be cautious. Your dentist will likely recommend a soft-food diet for the first few days. Long-term, you should avoid hard, sticky, or crunchy foods that could put excessive stress on the splint. Items like hard candy, ice, and nuts should be eaten with care.
4. Will my insurance cover the dental code for splinting teeth?
It depends. Coverage is often determined by the reason for the splint. If it is for trauma, medical insurance may cover it. If it is for periodontal disease, dental insurance may cover it, often at 50% after the deductible. Always get a pre-treatment estimate from your dentist’s office before proceeding.
5. What is the difference between a splint and a bridge?
A splint connects existing teeth to stabilize them. A bridge replaces missing teeth by using the adjacent teeth as supports (abutments). A bridge is a permanent, definitive restoration. A splint, especially one billed under D4320 or D4321, is considered provisional.
6. Can a splint be removed?
Yes, a provisional splint can be removed. An extracoronal splint (D4321) can be polished off with minimal effect on the teeth. An intracoronal splint (D4320) requires drilling to remove the material, and the grooves that were cut into the teeth will need to be filled with composite resin.
Conclusion
Navigating dental treatment can feel overwhelming, especially when you are dealing with the stress of loose teeth or a dental injury. Understanding the dental code for splinting teeth—whether it is D4320 for an intracoronal splint or D4321 for an extracoronal splint—empowers you to ask the right questions and make informed decisions about your oral health.
Remember, these codes represent more than just a billing number. They describe a clinical approach. D4321 offers a reversible, non-invasive way to stabilize teeth after trauma, acting as a cast to promote healing. D4320 provides a more robust, long-term solution for managing mobility caused by gum disease, though it requires a permanent alteration of the tooth structure.
Both procedures can be highly effective when used in the right context, but they are just one part of a larger treatment plan. Good oral hygiene, regular professional cleanings, and addressing the underlying cause of the mobility are essential for long-term success.
If your dentist has recommended a splint, ask them which code they will be using and why. This simple question can open a conversation that helps you understand your prognosis and the commitment required to maintain the splint. Your smile is an investment, and knowing the details of your care is the first step in protecting it.






