A tibial plateau fracture is more than a broken bone; it is a devastating injury that strikes at the very core of human mobility—the knee joint. Often resulting from high-energy trauma like motor vehicle accidents or a simple misstep for those with osteoporosis, these fractures demand a sophisticated surgical response. Open Reduction and Internal Fixation (ORIF) is the gold-standard procedure, a complex orchestration of surgical skill aimed at restoring the joint’s anatomy, stability, and function. However, the story does not end in the operating room. The intricate work of the surgeon must be perfectly translated into the language of medical billing and reimbursement through the precise application of Current Procedural Terminology (CPT) codes. This article serves as an exhaustive guide for orthopedic surgeons, coders, billers, and healthcare administrators, delving deep into the clinical nuances of tibial plateau ORIF and demystifying the complex coding landscape that surrounds it. We will explore not just the “what” but the “why,” ensuring that the financial viability of providing this critical care matches the clinical excellence required to perform it.
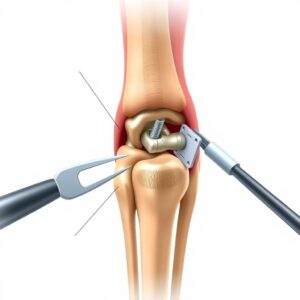
CPT coding for ORIF of Tibial Plateau Fractures
2. Understanding the Injury: Decoding the Tibial Plateau Fracture
Anatomy of the Knee Joint
The tibial plateau is the critical, weight-bearing top surface of the shin bone (tibia) that forms the bottom half of the knee joint. It is composed of two condyles—a larger medial (inside) and a smaller lateral (outside) condyle—which articulate with the femoral condyles to form the knee. These condyles are covered by a layer of articular cartilage, a smooth, slick tissue that allows for frictionless movement. The menisci, two C-shaped wedges of fibrocartilage, sit on top of the plateau, acting as shock absorbers and stabilizers. The integrity of this entire structure is paramount for weight-bearing, walking, and pivoting. A fracture here disrupts this精密 engineered system, often driving bone fragments into the joint space, damaging cartilage, and leading to premature arthritis if not perfectly reduced.
Mechanism of Injury: How Tibial Plateau Fractures Occur
These fractures typically occur through one of two primary mechanisms:
-
High-Energy Trauma: Common in younger patients, these result from events like motor vehicle collisions, falls from significant heights, or pedestrian-versus-vehicle accidents. The force is often a combination of axial load (force driving the femur down into the tibia) and varus or valgus stress (a bending force pushing the knee inward or outward). A bumper striking a pedestrian’s knee is a classic example.
-
Low-Energy Trauma: Seen predominantly in older patients with osteoporotic bone, a simple slip and fall from a standing height can generate enough force to cause a depression fracture of the weaker lateral plateau.
Classification Systems: Schatzker and More
Classification systems are vital for communication, surgical planning, and prognosis. The Schatzker Classification is the most widely used:
-
Type I: Pure split fracture of the lateral plateau.
-
Type II: Split fracture combined with depression of the articular surface.
-
Type III: Pure depression fracture of the lateral articular surface.
-
Type IV: Fracture of the medial plateau (often involving the tibial spines); associated with a high risk of neurovascular injury.
-
Type V: Bicondylar fracture, where both medial and lateral plateaus are separated from the metaphysis.
-
Type VI: A fracture where the articular surface is separated from the tibial shaft, with a transverse or oblique metaphyseal fracture.
Other systems like the AO/OTA classification provide even more granular detail, but Schatzker remains the clinical workhorse.
3. The Surgical Solution: A Deep Dive into Open Reduction and Internal Fixation (ORIF)
The goals of ORIF are unambiguous: to restore the joint surface to within 2 mm of anatomical perfection, achieve absolute stability to allow early range of motion, and correct axial alignment to prevent post-traumatic arthritis.
Preoperative Planning: Imaging and Patient Assessment
Planning begins with advanced imaging. While X-rays provide the initial diagnosis, a CT scan with 2D and 3D reconstructions is non-negotiable. It reveals the exact path of fracture lines, the degree and location of articular depression, and the number and size of fragments. This allows the surgeon to mentally rehearse the reduction sequence and select the appropriate implants. Patient assessment is equally critical, evaluating soft tissue condition (swelling, bruising, blisters), neurovascular status (popliteal artery, peroneal nerve), and overall medical fitness for a major surgery.
The Surgical Procedure: Step-by-Step
-
Positioning and Approach: The patient is positioned supine, often with a bump under the hip. The surgical approach is dictated by the fracture pattern. A lateral approach is most common for lateral fractures. A medial or combined medial and lateral approach is necessary for bicondylar (Schatzker V, VI) or medial (Schatzker IV) fractures.
-
Arthrotomy and Visualization: The joint is opened, and the meniscus may be lifted to visualize the articular surface directly.
-
Reduction: This is the most critical step. Depressed fragments are elevated en masse from below using specialized instruments. The resulting metaphyseal void must be filled with a bone graft (autograft from the iliac crest) or, more commonly today, a bone graft substitute (calcium phosphate cement, allograft chips) to provide structural support and prevent re-collapse.
-
Provisional Fixation: Reduced fragments are held with K-wires.
-
Definitive Fixation: A pre-contoured periarticular plate is applied. These plates are designed to fit the anatomy of the proximal tibia, with locking screws that provide angular stability, forming a fixed-angle construct that is exceptionally strong, especially in osteoporotic bone. Non-locking screws provide compression across fracture lines.
-
Closure: The surgical site is irrigated copiously, and the layers are closed meticulously over drains to minimize the risk of infection.
Implant Technology: Plates, Screws, and Bone Grafts
Modern implant systems are marvels of engineering. Locking plate technology has revolutionized the treatment of complex periarticular fractures. These systems allow surgeons to build a stable “scaffold” around the fractured bone. The choice of bone graft substitute is also crucial; calcium phosphate cements are popular as they provide immediate structural support and are osteoconductive.
4. The Core of Medical Billing: Mastering CPT Codes for Tibial Plateau ORIF
This is where clinical work meets financial reality. Selecting the correct CPT code is paramount and is based entirely on the complexity of the fracture pattern and the work performed.
CPT Code 27535: Open treatment of tibial fracture, proximal (plateau); unicondylar, without internal fixation
This code is a common source of confusion. The descriptor “without internal fixation” is a misnomer. It is used for unicondylar fractures (e.g., Schatzker I, II, III) that are treated with internal fixation. The AMA CPT guidelines clarify that this code includes procedures where internal fixation is used. It is the appropriate code for fractures involving a single condyle that are fixed with plates and/or screws.
CPT Code 27536: Open treatment of tibial fracture, proximal (plateau); bicondylar, with or without internal fixation
This code is reserved for more complex bicondylar fractures (Schatzker V, VI) that involve both the medial and lateral plateaus. The work involved in reducing and stabilizing two separate articular surfaces, often requiring a dual incision approach, is significantly greater, which is reflected in the higher relative value units (RVUs) and reimbursement for this code.
Modifier Use: -22, -50, -52, -59, and -LT/-RT
-
-22 (Increased Procedural Services): Used when the procedure required substantially greater effort than typically required. Examples: extreme obesity, a highly comminuted fracture that took extraordinary time to reconstruct, or severe medical comorbidities that complicated the surgery. Documentation must be impeccable to justify this modifier, including detailed operative notes and a separate letter explaining the extra work.
-
-50 (Bilateral Procedure): Appended if the same procedure is performed on both knees during the same operative session. This is extremely rare for traumatic fractures.
-
-52 (Reduced Services): Used if the procedure was reduced or eliminated at the surgeon’s discretion. Rarely applicable in trauma.
-
-59 (Distinct Procedural Service): Used to indicate that a procedure or service was distinct or independent from other services performed on the same day. Crucial for bypassing NCCI edits if, for example, an external fixator is applied at a separate session before definitive ORIF.
-
-LT / -RT (Left Side, Right Side): Essential for specifying laterality. Never bill without a laterality modifier.
Global Period and Postoperative Management
Tibial plateau ORIF is a major procedure with a 90-day global surgical period. This means the surgeon’s fee encompasses all related preoperative, intraoperative, and postoperative care for the following 90 days. This includes follow-up visits, wound checks, cast/splint application, and routine postoperative management. Only unrelated services or complications requiring a return to the OR (e.g., irrigation and debridement for infection) can be billed separately within this period.
5. ICD-10-CM Coding: Precisely Documenting the Medical Necessity
The CPT code tells the what, the ICD-10 code tells the why. Specificity is non-negotiable. The correct code comes from category S82.1- (Fracture of upper end of tibia).
| Fracture Type | ICD-10-CM Code Example | Description |
|---|---|---|
| Lateral, Non-Displaced | S82.121- | Fracture of lateral tibial plateau, closed |
| Lateral, Displaced | S82.122- | Fracture of lateral tibial plateau, open |
| Medial, Displaced | S82.124- | Fracture of medial tibial plateau, closed |
| Bicondylar | S82.112- | Fracture of unspecified tibial spine, closed |
| Open Fracture | S82.122B | Open fracture of lateral tibial plateau, initial encounter for open fracture type I or II |
-
7th Character Required: The 7th character defines the encounter (A – initial, D – subsequent, S – sequela).
-
Open Fracture Gustilo Classification: For open fractures, an additional 7th character extension (B, C, D) specifies the Gustilo type, which is critical for reflecting the severity and increased work involved.
6. Navigating Payer Policies and Avoiding Denials
Bundling and NCCI Edits
The National Correct Coding Initiative (NCCI) contains edits that pair certain codes that should not be billed together. A common issue is the application of an external fixator (CPT 20690-20692) prior to definitive ORIF. If applied during a separate encounter, it can be billed with modifier -59. If applied during the same encounter as the ORIF, it is generally bundled and not separately payable unless it is for a different fracture.
Documentation Requirements for Medical Necessity
The operative report is the foundation of the claim. It must clearly support the code chosen:
-
For 27535, the report should document a unicondylar fracture (e.g., “lateral split-depression fracture”).
-
For 27536, it must explicitly state a bicondylar fracture or describe the involvement of both the medial and lateral plateaus.
-
It should detail the approach(es), the reduction technique, the use of bone graft, and the specific implants used (e.g., “a lateral proximal tibial locking plate was applied”).
-
For modifier -22, the report must detail the extra time, difficulty, and complexity.
7. Case Studies: Applying Knowledge to Real-World Scenarios
Case Study 1: Unicondylar Fracture (Schatzker III)
-
Presentation: A 70-year-old female with osteoporosis slips on ice, sustaining an isolated injury to her right knee. X-ray and CT show a depressed lateral tibial plateau fracture without a split component.
-
Procedure: ORIF via a lateral approach. The articular surface was elevated, the defect was filled with calcium phosphate cement, and a lateral locking plate was applied.
-
Coding: CPT 27535-RT. ICD-10-CM: S82.121D (if closed, subsequent care for healing fracture).
Case Study 2: Bicondylar Fracture (Schatzker V)
-
Presentation: A 45-year-old male is in a motorcycle accident. CT scan reveals a complex fracture with separate fracture lines involving both the medial and lateral plateaus.
-
Procedure: ORIF via separate medial and lateral incisions. Both condyles were reduced and fixed with a medial and a lateral plating system.
-
Coding: CPT 27536-LT (assuming left knee). ICD-10-CM: S82.112A (initial encounter for closed bicondylar fracture).
Case Study 3: Staged Procedure with External Fixation
-
Presentation: A patient presents with a high-energy Schatzker VI fracture with significant soft tissue swelling and fracture blisters.
-
Procedure Day 1: Application of a knee-spanning external fixator for stabilization and to allow soft tissue recovery.
-
Procedure Day 10: Once swelling subsides, the external fixator is removed, and definitive ORIF with dual plates is performed.
-
Coding: Day 1: CPT 20692 (application of multi-pin external fixator) with appropriate modifiers. Day 10: CPT 27536. The use of modifier -59 on the external fixator code (if billed on the same claim) may be necessary to bypass NCCI edits, as it was a distinct procedural service during the global period of the fixator application.
8. The Financial and Operational Impact of Accurate Coding
The difference between 27535 and 27536 is not trivial; it can represent a difference of thousands of dollars in reimbursement. Miscoding a bicondylar fracture as a unicondylar one (using 27535 instead of 27536) constitutes under-coding, leaving significant revenue on the table and failing to compensate the practice for the immense additional work and resources used. Conversely, using 27536 for a true unicondylar fracture is over-coding and fraud, which can lead to audits, hefty fines, and reputational damage. Accurate coding is therefore not just an administrative task; it is a fundamental component of ethical and sustainable surgical practice. It ensures that the resources needed to maintain a state-of-the-art trauma service—including staff, implants, and imaging equipment—are adequately funded.
9. Conclusion: Synthesizing Clinical Excellence with Coding Expertise
Mastering the CPT coding for tibial plateau ORIF requires a deep understanding of the fracture’s anatomy and surgical repair. The critical distinction lies between unicondylar (27535) and bicondylar (27536) patterns. Flawless documentation in the operative report is the non-negotiable foundation that justifies the code selection and ensures appropriate reimbursement. Ultimately, precise coding is the essential bridge that connects surgical artistry to financial sustainability, ensuring these life-restoring procedures can continue to be offered to patients in need.
10. Frequently Asked Questions (FAQs)
Q1: Can I bill for bone graft separately when performing a tibial plateau ORIF?
A: Generally, no. The work of harvesting autograft (e.g., from the iliac crest) and the material cost of allograft or bone graft substitute are considered integral to the fracture repair and are bundled into the primary procedure code (27535 or 27536). You cannot separately report codes like 20910 (bone graft, local) or 20912 (bone graft, structural) for the same surgical field.
Q2: What if I use a arthroscopically assisted technique to help with the reduction?
A: Arthroscopic assistance is a fantastic tool for visualizing the articular reduction without a large open arthrotomy. However, CPT code 29855 (Arthroscopically aided treatment of tibial fracture, proximal) is specifically for purely arthroscopic procedures. If you perform an open procedure (with an incision for plate placement) and use the scope for assistance, you bill only the open treatment code (27535 or 27536). The arthroscopic portion is not separately reportable.
Q3: How do I code for a revision ORIF procedure for a failed fixation or nonunion?
A: Revision surgery is complex. You would typically use the same primary code (27535 or 27536) but append modifier -78 (Unplanned Return to the Operating Room). The diagnosis code would change to reflect the complication (e.g., T84.1- for mechanical complication of internal fixation, M84.1- for nonunion). The work is often more difficult, so thorough documentation to support modifier -22 may also be warranted.
Q4: A patient has both a tibial plateau fracture and a tibial shaft fracture. How is this coded?
A: This is a complex scenario. If the fractures are distinct and treated with separate implants (e.g., a plate for the plateau and an intramedullary nail for the shaft), you may report both codes (e.g., 27536 for the plateau and 27758/27759 for the shaft) with modifier -59 on the second code. However, NCCI edits often bundle these, and payer policies vary widely. The operative report must clearly document the separate nature of the injuries and the independent procedures performed.
11. Additional Resources
-
American Medical Association (AMA): For the definitive CPT codebook and official guidelines.
-
American Academy of Orthopaedic Surgeons (AAOS): Provides clinical resources, coding workshops, and position statements on orthopedic billing.
-
Centers for Medicare & Medicaid Services (CMS): For National Correct Coding Initiative (NCCI) edits and Medicare-specific policies.
-
Orthopedic Trauma Association (OTA): Offers advanced courses and publications focused on the treatment and coding of complex fractures.
12. Disclaimer
This article is intended for informational and educational purposes only. It does not constitute medical, legal, or coding advice. The information provided is based on current guidelines and practices but is subject to change. CPT is a registered trademark of the American Medical Association. Medical coding is complex and highly dependent on the specific details of each patient encounter and the contents of the medical documentation. The ultimate responsibility for accurate coding and billing lies with the healthcare provider. It is imperative to consult the most current, official CPT and ICD-10-CM code sets, payer-specific policies, and a certified professional coder for definitive guidance on individual cases. The author and publisher disclaim any liability for any loss or damage resulting from reliance on the information contained






