In the intricate world of medical coding, where complex human experiences are distilled into alphanumeric sequences, few codes carry the weight and transformative promise of CPT code 27130. This five-digit number represents far more than a simple financial transaction; it is the key that unlocks access to one of modern medicine’s most successful and life-altering procedures: the total hip arthroplasty (THA). For thousands of patients each year, the accurate application of this code signifies the end of chronic, debilitating pain and the beginning of a return to mobility, independence, and a higher quality of life. For surgeons, it represents the culmination of years of training and technical skill. For coders, billers, and healthcare administrators, it is a complex puzzle where precision is paramount, and a single misstep can have significant financial and legal repercussions. This article delves deep into the universe of 27130, moving beyond the basic description to explore the anatomical, procedural, coding, financial, and regulatory nuances that define it. Our goal is to provide an exhaustive resource for orthopedic surgeons, coders, billers, practice managers, and healthcare students, transforming this simple code from a abstract identifier into a comprehensive story of clinical success, administrative precision, and patient triumph.
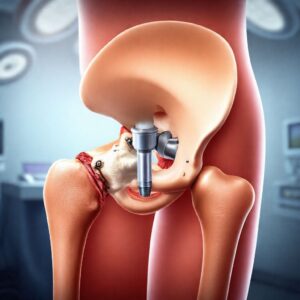
CPT Code for Right Total Hip Arthroplasty
2. Understanding the Procedure: The Art and Science of Total Hip Arthroplasty
Before one can truly grasp the coding of a procedure, one must first understand the procedure itself. Total hip arthroplasty is a masterpiece of orthopedic surgery, a procedure that elegantly addresses the biomechanical failure of the body’s largest weight-bearing joint.
Anatomy of the Hip Joint
The hip is a classic ball-and-socket synovial joint, designed for both remarkable stability and an extensive range of motion. The “socket” (acetabulum) is a concave surface on the lateral aspect of the pelvis. The “ball” is the head of the femur (the thigh bone), which connects to the shaft via the femoral neck. This entire structure is surrounded by a complex network of ligaments, tendons, and muscles—most notably the gluteal muscles—that provide power and stability. The articulating surfaces of the femoral head and acetabulum are covered with a layer of slick, durable hyaline cartilage, which allows for near-frictionless movement and acts as a shock absorber. The joint is lubricated by synovial fluid, contained within a joint capsule. The degeneration of this cartilage is the primary culprit behind the pain and dysfunction that lead to a THA.
Indications for Surgery: When is a THA Necessary?
The decision to perform a total hip arthroplasty is not taken lightly. It is typically a final option after conservative measures—such as physical therapy, weight loss, anti-inflammatory medications, injections, and lifestyle modifications—have failed to provide adequate relief. The primary indications include:
-
Osteoarthritis (Degenerative Joint Disease): The most common reason for THA. It is characterized by the progressive “wear and tear” breakdown of articular cartilage, leading to painful bone-on-bone contact, osteophyte (bone spur) formation, and loss of joint space.
-
Rheumatoid Arthritis: An autoimmune disorder where the body’s immune system attacks the synovial membrane, causing inflammation, pain, and eventual destruction of both cartilage and bone.
-
Post-Traumatic Arthritis: Develops following a significant injury to the hip, such as a fracture or dislocation, which damages the cartilage and leads to premature degeneration.
-
Avascular Necrosis (Osteonecrosis): The death of bone tissue in the femoral head due to a loss of blood supply. This can be caused by trauma, long-term steroid use, excessive alcohol consumption, or other diseases.
-
Congenital Deformities (e.g., Developmental Dysplasia of the Hip – DDH): Abnormal development of the hip joint from birth that predisposes it to early arthritis.
-
Acute Femoral Neck Fractures: In active, elderly patients, a THA (rather than a hemiarthroplasty) may be the preferred treatment for a displaced femoral neck fracture to provide better long-term function and avoid the need for revision surgery.
The Surgical Procedure: A Step-by-Step Overview
While surgical techniques vary by approach and surgeon preference, the core components of a THA remain consistent. The procedure involves replacing both the damaged acetabulum and the femoral head with prosthetic components.
-
Anesthesia and Positioning: The patient receives general or regional anesthesia (e.g., spinal block). They are then meticulously positioned on the operating table in a lateral decubitus (on their side) or supine (on their back) position, depending on the surgical approach. The operative leg is prepped and draped sterilely.
-
Incision and Approach: The surgeon makes an incision, typically 4 to 10 inches long, in a location determined by the chosen approach (posterior, anterior, lateral, etc.). The underlying muscles and tissues are carefully separated or split to expose the hip joint capsule.
-
Dislocation: The hip joint is dislocated, bringing the femoral head out of the acetabulum.
-
Femoral Preparation: The femoral head is removed using a saw at the femoral neck. The femoral canal is then reamed and broached to create a precise cavity to accept the femoral stem implant.
-
Acetabular Preparation: The damaged cartilage and bone within the acetabular socket are reamed away, creating a hemispherical shape that will perfectly accommodate the new acetabular cup.
-
Implant Placement:
-
The acetabular cup (typically a metal shell) is press-fit into the prepared socket. It is often secured with additional screws for stability. A liner, usually made of highly cross-linked polyethylene, ceramic, or metal, is locked into the cup.
-
The femoral stem (made of titanium, cobalt-chromium, or other alloys) is inserted into the prepared femoral canal. It may be cemented in place with polymethylmethacrylate (PMMA) bone cement or press-fit for biological fixation where bone grows into a porous coating on the implant.
-
A femoral head component (made of ceramic or metal) is then attached to the stem’s trunnion.
-
-
Reduction and Closure: The new prosthetic ball (femoral head) is reduced back into the new socket (acetabular liner). The surgeon tests the hip’s stability, range of motion, and leg length. The deep tissues and muscle layers are repaired with sutures, and the skin is closed with staples or sutures. A sterile dressing is applied.
Surgical Approaches: Anterior, Posterior, Lateral, and More
The “approach” refers to the anatomical path the surgeon takes to access the hip joint. Each has its own advantages, disadvantages, and implications for recovery.
-
Posterior Approach: The most common approach in the United States. The incision is made on the posterior aspect of the hip, and the gluteus maximus muscle is split. The short external rotator muscles are detached to access the joint. Advantage: Excellent visualization of the acetabulum and femur. Disadvantage: Historically associated with a higher risk of posterior dislocation due to the disruption of the posterior soft tissues. However, modern techniques that meticulously repair the capsule and short external rotators have significantly reduced this risk.
-
Direct Anterior Approach (DAA): Gaining immense popularity due to its “muscle-sparing” nature. The incision is made at the front of the hip, utilizing an internervous plane between the sartorius (femoral nerve) and tensor fasciae latae (superior gluteal nerve). Advantage: Potentially less postoperative pain, faster initial recovery, and a lower historical dislocation rate as the posterior structures remain intact. Disadvantage: Steeper learning curve for surgeons, potentially longer operative times, and specific risks like lateral femoral cutaneous nerve injury leading to thigh numbness.
-
Direct Lateral (Hardinge) Approach: The incision is made on the side of the hip. A portion of the abductor muscles (gluteus medius and minimus) is elevated from the greater trochanter. Advantage: Excellent stability and low dislocation risk. Disadvantage: The abductor muscles are critical for normal gait; weakness or limp due to abductor dysfunction is a known potential complication.
-
Anterolateral Approach: A modification of the lateral approach that aims to better preserve the abductor mechanism.
It is critical for coders to understand that CPT 27130 is independent of the surgical approach. The code is used for a total hip arthroplasty regardless of whether the surgeon uses an anterior, posterior, or lateral technique.
3. Deconstructing CPT Code 27130: The Official Description and Context
The American Medical Association’s (AMA) Current Procedural Terminology (CPT®) code set is the universal language for reporting medical procedures and services. Precision in code selection is the foundation of compliant billing.
CPT® Manual Language
The official CPT descriptor for code 27130 is:
“Arthroplasty, acetabular and proximal femoral prosthetic replacement (total hip arthroplasty), with or without autograft or allograft”
This description is dense with meaning:
-
“Arthroplasty”: Literally means “surgical repair of a joint.”
-
“Acetabular and proximal femoral prosthetic replacement”: This explicitly defines the procedure as involving the replacement of both sides of the joint—the socket (acetabulum) and the ball (proximal femur). This is what makes it “total.”
-
“With or without autograft or allograft”: Signifies that the code is inclusive of any bone grafting that may be necessary during the procedure. An autograft is bone taken from the patient themselves (often from the resected femoral head), and an allograft is donor bone. Because this is included in the main code, it cannot be billed separately.
“Total” and “Right”: The Critical Components of 27130
CPT code 27130 is inherently unilateral. It describes a procedure performed on a single hip. This is why laterality is a critical component of accurate coding.
-
27130-RT: For a total hip arthroplasty performed on the right hip.
-
27130-LT: For a total hip arthroplasty performed on the left hip.
The modifier -RT or -LT must be appended to the code to specify which hip was operated on. Failure to do so will almost certainly result in a claim rejection or denial, as the payer lacks the necessary information to process it.
Distinguishing 27130 from Other Hip Procedures
A clear understanding of what 27130 is not is just as important as knowing what it is.
-
Hemiarthroplasty (Partial Hip Replacement) – CPT 27125: This procedure involves replacing only the femoral head and neck, leaving the natural acetabulum intact. It is most commonly performed for certain types of hip fractures (e.g., femoral neck fractures) in elderly, lower-demand patients. Using 27130 for a hemiarthroplasty would be incorrect and constitute overcoding.
-
Revision Total Hip Arthroplasty – CPT 27134, 27137, 27138: These codes are used when a previously implanted prosthetic hip needs to be partially or completely replaced. Revision surgery is far more complex, as it involves removing existing implants, dealing with bone loss (often requiring significant bone grafting), and placing new revision implants. Codes are selected based on whether the revision involves the acetabular component only (27137), the femoral component only (27136), or both components (27134). A separate code exists for the removal of the implant (27090-27091). Reporting 27130 for a revision procedure is a serious error.
-
Hip Resurfacing – CPT 27100: This is a bone-conserving alternative to a standard THA, where the femoral head is trimmed and capped with a metal prosthesis, and a metal acetabular component is implanted. It is not as common as it once was but is still an option for some younger, active patients.
-
Conversion to Total Hip – (e.g., 27132): This refers to a THA performed in a hip that has had previous surgery, such as an open reduction internal fixation (ORIF) of a fracture. It is distinct from a revision of a previous arthroplasty.
4. Coding and Billing Mechanics: Navigating the Nuances
Translating the surgical event into a reimbursable claim requires meticulous attention to detail beyond just the primary CPT code.
Modifiers: The -50, -RT, -LT, and When to Use Them
Modifiers are two-character suffixes that provide additional information about a procedure without changing its definition. Their correct use is non-negotiable for compliance.
-
Modifiers -RT (Right side) and -LT (Left side): As discussed, these are essential for specifying laterality. Example:
27130-RT. -
Modifier -50 (Bilateral Procedure): If a surgeon performs a total hip arthroplasty on both the right and left hip during the same operative session, modifier -50 is appended to the code on a single line item. Most payers will reimburse for the second hip at 50% of the allowable fee.
-
Incorrect: 27130-RT and 27130-LT on two separate lines.
-
Correct: 27130-50 (with a quantity of 2 units). Always verify specific payer guidelines, as some may prefer a different billing format.
-
-
Other Relevant Modifiers:
-
-78 (Unplanned Return to the Operating Room): Used if the patient must return to the OR during the global period of 27130 for a related procedure, such as an irrigation and debridement for a suspected infection.
-
-79 (Unrelated Procedure by the Same Physician): Used if a procedure unrelated to the hip arthroplasty is performed during the global period.
-
Global Period: Understanding the 90-Day Postoperative Window
CPT 27130 is a major surgical procedure with a 90-day global period. This means the reimbursement for the code is intended to cover not only the surgery itself but also all of the surgeon’s routine postoperative care for the next 90 days. This includes:
-
Follow-up office visits
-
Dressing changes
-
Removal of sutures or staples
-
Management of uncomplicated postoperative pain
-
Routine monitoring of recovery
Critical Note: If the patient has a complication that requires a return to the operating room (e.g., for a manipulation under anesthesia due to stiffness or an I&D for infection), this care is not included in the global package and can be billed separately with the appropriate modifier (-78).
Bundled Services: What’s Included and What Can Be Billed Separately?
The concept of “bundling” is central to correct coding. The value of 27130 includes all the usual components of the procedure. The following are typically included and not separately billable:
-
Allograft or Autograft: As indicated in the code descriptor.
-
Cement: If used for fixation (e.g., 27130 includes “with or without cement”).
-
Standard Surgical Approach: The work of exposing the joint via any standard approach is included.
-
Intra-operative fluoroscopy: Routine use for component positioning is considered integral.
The following services may be separately billable if documented and medically necessary:
-
Significant and separately identifiable evaluation and management (E/M) service on the day of surgery. For example, if the surgeon sees the patient for a new problem or a comprehensive re-evaluation unrelated to the decision for surgery, this could be billed with modifier -25 appended to the E/M code to indicate it was a distinct service.
-
Diagnostic arthroscopy (CPT 29900 or 29901) performed immediately prior to the arthroplasty to evaluate a diagnostic dilemma is sometimes separately payable with a modifier -59 (distinct procedural service), but this is rare and must be strongly justified in the documentation.
-
Complex closure is not typically applicable to hip arthroplasty, as the closure is considered standard.
-
Treatment of a distinct, unrelated injury or condition during the same session.
5. The Crucial Role of ICD-10-CM: Linking Diagnosis to Procedure
A CPT code tells the payer what was done; an ICD-10-CM code tells them why it was done. The diagnosis code provides the medical necessity for the procedure. An incomplete or incorrect diagnosis link is a primary cause of claim denials.
Common Primary Diagnosis Codes (M16.-)
The ICD-10-CM codes for osteoarthritis of the hip are found in category M16. Specificity is required regarding laterality, cause, and whether it is the primary or secondary joint affected.
| ICD-10-CM Code | Description | Use Case |
|---|---|---|
| M16.11 | Osteoarthritis of hip, right hip | Primary OA, right hip |
| M16.12 | Osteoarthritis of hip, left hip | Primary OA, left hip |
| M16.0 | Bilateral primary osteoarthritis of hip | For a bilateral procedure |
| M16.31 | Unilateral post-traumatic osteoarthritis, right hip | OA following a past fracture |
| M16.51 | Unilateral secondary osteoarthritis, right hip | OA due to another cause (e.g., avascular necrosis, old infection) |
| M16.7 | Secondary osteoarthritis of hip, bilateral |
Supporting Diagnosis Codes
Other common diagnosis codes supporting medical necessity for 27130 include:
-
Avascular Necrosis of Femoral Head: M87.051 (idiopathic, right hip), M87.351 (secondary, right hip), M87.051 (post-traumatic, right hip).
-
Rheumatoid Arthritis: M05.741 (rheumatoid arthritis with involvement of right hip).
-
Congenital Dislocation of Hip (DDH): Q65.81 (right hip).
-
Fracture of Femoral Neck: S72.00XA (unspecified intracapsular fracture of right femur, initial encounter). Note: The use of THA for an acute fracture is specific and requires clear documentation.
The Importance of Medical Necessity
The documentation in the patient’s medical record must paint a clear picture of why this major surgery was required. This includes:
-
History of persistent pain that significantly limits activities of daily living (ADLs)
-
Failure of an adequate trial of conservative management (e.g., PT, NSAIDs, injections)
-
Physical exam findings (limited range of motion, antalgic gait, tenderness)
-
Radiographic evidence (X-ray, MRI) confirming advanced joint destruction
The coder’s role is to ensure the diagnosis codes selected accurately reflect this documented clinical picture.
6. The Financial Ecosystem: Reimbursement, RVUs, and Payer Policies
The reimbursement for 27130 is not an arbitrary number. It is calculated based on a complex formula that aims to quantify the physician’s work.
Understanding RVUs (Relative Value Units)
The Medicare Physician Fee Schedule (MPFS) uses RVUs to assign value to every CPT code. The total RVUs for a code are the sum of three components:
-
Work RVU (wRVU): Reflects the time, skill, effort, and stress required by the physician to perform the service. This is the largest component for surgical procedures like 27130.
-
Practice Expense (PE) RVU: Covers the cost of running the practice (staff, equipment, supplies, office space).
-
Malpractice (MP) RVU: Covers the cost of professional liability insurance.
The total reimbursement is calculated as: (Work RVU + PE RVU + MP RVU) x Geographic Practice Cost Index (GPCI) x Conversion Factor (CF).
The CF is a dollar amount set by Congress and CMS annually. The GPCI adjusts for regional variations in costs.
Medicare and Commercial Payer Considerations
While Medicare sets a national standard, commercial payers (Blue Cross Blue Shield, Aetna, UnitedHealthcare, etc.) often negotiate their own fee schedules with healthcare providers. The allowed amount for 27130 can vary significantly between Medicare and a commercial plan, and even among different commercial plans. It is imperative for practices to understand their contracts with each payer.
The Impact of Site of Service (Hospital Inpatient vs. Ambulatory Surgery Center)
The place where the surgery is performed has a major impact on billing, but primarily for the facility (hospital/ASC), not the surgeon. The surgeon’s professional fee (reported with 27130) is generally the same regardless of location. However, the facility will bill separately for the use of the operating room, nursing staff, implants, medications, and overnight stay.
-
Inpatient Hospital: For patients who require a hospital stay postoperatively (typically 1-3 days for uncomplicated THA).
-
Ambulatory Surgery Center (ASC): For patients who are healthy enough to have surgery and be discharged the same day. The migration of THA to the ASC setting is one of the most significant trends in orthopedics, driven by improved pain protocols, blood management, and patient selection.
7. Compliance and Auditing: Mitigating Risk in THA Coding
Given the high cost of a THA, it is a prime target for audits by Medicare Administrative Contractors (MACs), the Recovery Audit Contractors (RACs), and commercial payers.
Common Coding Errors and How to Avoid Them
-
Incorrect Laterality: Failing to use -RT or -LT, or using the wrong one. Fix: Double-check the operative report against the claim.
-
Upcoding: Using 27130 (total) when a hemiarthroplasty (27125) was performed. Fix: Read the op report carefully. If only the femoral head was replaced and the acetabulum was not prepared or recemented, it is a hemi.
-
Unbundling: Separately billing for services included in the global package of 27130 (e.g., routine post-op visits, simple wound care). Fix: Understand the global surgical package rules.
-
Lack of Medical Necessity: Using an unspecified or ill-fitting diagnosis code that does not justify the procedure. Fix: Ensure the diagnosis is specific and supported by the patient’s clinical record.
Documentation Requirements: The Surgeon’s Operative Note
The operative report is the coder’s bible. A well-documented report must include:
-
Preoperative and Postoperative Diagnoses
-
Title of Procedure: Clearly stating “Right Total Hip Arthroplasty.”
-
Surgeon(s) and Assistant(s)
-
Anesthesia Type
-
Detailed Description:
-
Incision location and length.
-
Surgical approach used (e.g., “posterior approach to the right hip”).
-
Findings upon entry (e.g., “advanced wear of the femoral head and acetabular cartilage”).
-
Step-by-step account of the procedure, including how the acetabulum was reamed and the femoral canal prepared.
-
Implant Details: Manufacturer, model, and sizes of all components (cup, liner, stem, head). This is crucial for product recall tracking and is often required by registries.
-
Description of closure.
-
-
Estimated Blood Loss (EBL)
-
Specimens Removed (e.g., femoral head sent to pathology)
-
Complications, if any
-
Sponge, Needle, and Instrument Counts
Preparing for an Audit: Key Elements to Have in Place
A proactive compliance plan is the best defense.
-
Maintain organized records: Ensure easy access to the operative report, clinical notes, and imaging reports for any billed claim.
-
Conduct internal audits: Regularly review a sample of your own claims to catch errors before an external auditor does.
-
Provide ongoing coder education: Keep coders updated on annual CPT and ICD-10 changes and payer-specific policies.
8. The Future of Hip Arthroplasty Coding: Trends and Innovations
The field of joint replacement is dynamic, and coding must evolve alongside it.
-
Outpatient THA and Changing Status: CMS has removed total hip arthroplasty from the “Inpatient Only” (IPO) list. This means that Medicare will cover the procedure in both the inpatient and outpatient settings, with the determination based on the patient’s individual medical needs. This shift requires careful patient selection and changes in facility billing.
-
The Rise of Robotics and Navigational Technology: Many THAs are now performed with robotic-arm assistance or computer navigation. There is no specific CPT code for the use of this technology in hip arthroplasty. The work involved in setting up and using the system is considered bundled into the primary procedure code (27130). The cost of the technology is typically baked into the facility’s cost or the implant cost.
-
Value-Based Care and Bundled Payments (BPCI): The healthcare system is increasingly shifting from fee-for-service (paying for volume) to value-based care (paying for outcomes). In the Bundled Payments for Care Improvement (BPCI) model, a single payment is made to cover all services related to a THA episode of care, from the surgery itself to 90 days of post-acute care (rehab, nursing home, etc.). This places a premium on efficiency, coordination of care, and minimizing complications. While this doesn’t change the CPT code used, it radically changes the financial model surrounding it.
9. Conclusion
CPT code 27130 for right total hip arthroplasty is a powerful testament to medical advancement, representing a procedure that restores function and alleviates pain for countless individuals. Its accurate application, however, hinges on a deep and nuanced understanding that spans clinical knowledge, precise coding protocols, and evolving regulatory landscapes. From the anatomy of the hip joint to the complexities of RVU-based reimbursement and the shift toward outpatient and value-based care, mastering 27130 requires a commitment to continuous learning and meticulous attention to detail. By ensuring precise code selection, robust documentation, and compliant billing practices, healthcare professionals not only safeguard their practice’s financial health but also contribute to the sustainability of a system that delivers this transformative care.
10. Frequently Asked Questions (FAQs)
Q1: Can I bill for a trochanteric osteotomy separately with a 27130?
A: No. If a trochanteric osteotomy (CPT 27120) is performed as a necessary part of the exposure for a complex primary total hip arthroplasty, it is considered an integral component of the procedure and is bundled into 27130. It is not separately reportable.
Q2: What if the surgeon uses “custom” or “patient-specific” implants?
A: The CPT code remains 27130. There is no separate code for the use of custom implants, cutting guides, or instrumentation. The work involved is included in the primary procedure. The facility may bill separately for the higher cost of the custom implant.
Q3: How do I code a total hip arthroplasty that was converted from a previous internal fixation?
A: This is a “conversion” procedure. You would use the standard THA code, 27130. It is critical that the diagnosis code reflects the reason for the conversion (e.g., M16.51 for post-traumatic secondary osteoarthritis). The previous hardware removal is typically included in the work of the conversion and is not separately billable unless it requires a separate, extensive incision and significant additional time, which is rare.
Q4: My patient had a THA and then was readmitted for a dislocation that required a closed reduction in the emergency room. Can I bill for that?
A: If the closed reduction is performed in the ER without the need for a return to the operating room, it is considered a treatment of a complication and is included in the 90-day global surgical package of 27130. It cannot be billed separately. If an open reduction in the OR is required, you would bill for that with the appropriate code (e.g., 27266) with a -78 modifier.
Q5: Are there any specific documentation requirements for medical necessity for Medicare patients?
A: While there is no single mandated form, Medicare expects the medical record to clearly demonstrate that conservative therapy was tried and failed. The documentation should include the type, duration, and response to treatments like physical therapy, NSAIDs, and injections. The patient’s subjective complaints of pain and functional limitation should be detailed alongside objective findings on exam and imaging.
11. Additional Resources
-
American Medical Association (AMA): For the official CPT® code set and guidelines. https://www.ama-assn.org/
-
Centers for Medicare & Medicaid Services (CMS): For the Medicare Physician Fee Schedule, National Coverage Determinations (NCDs), and Local Coverage Determinations (LCDs). https://www.cms.gov/
-
American Academy of Orthopaedic Surgeons (AAOS): Provides clinical guidelines, coding workshops, and resources for orthopedic surgeons and their staff. https://www.aaos.org/
-
American Health Information Management Association (AHIMA): A premier association for health information management and coding professionals. https://www.ahima.org/
-
American Academy of Professional Coders (AAPC): Offers certifications, training, and resources for medical coders. https://www.aapc.com/
-
ICD-10-CM Official Guidelines for Coding and Reporting: Published by the CDC and CMS, these are the definitive rules for using ICD-10 codes. https://www.cdc.gov/nchs/icd/icd-10-cm.htm






