If you have ever tried to find the right code for placing a PleurX drain in the abdomen, you know it can feel like a maze. You are not alone.
Many coders, nurses, and even physicians mix this up with chest tube codes. But here is the truth: placing a PleurX catheter in the belly is not the same as placing one in the lung cavity.
This guide walks you through everything you need to know. We will look at the correct CPT codes, when to use them, and how to avoid costly denials. No complex language. No fluff. Just clear, honest help.
Let us start with the most important question.
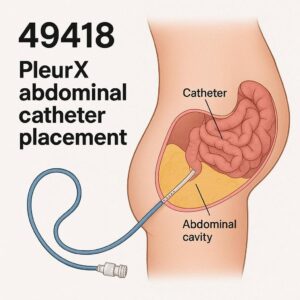
CPT Code PleurX Abdominal Catheter Placement
What Exactly Is a PleurX Abdominal Catheter?
Before we talk about codes, let us understand the procedure itself.
A PleurX catheter is a small, soft drain. Doctors place it inside the peritoneal cavity. That is the space inside your belly that holds fluid. The catheter then tunnels under the skin for a short distance before exiting the body.
Why do patients need this? Two main reasons:
-
Malignant ascites: Fluid builds up because of cancer in the abdomen. Common cancers include ovarian, colon, pancreatic, or liver cancer.
-
Refractory ascites: This happens when diuretics (water pills) stop working. It is often seen in advanced liver disease or cirrhosis.
The beauty of the PleurX system is that patients or caregivers can drain the fluid at home. They do not need to come to the hospital every time. This improves quality of life dramatically.
Important note: The PleurX drain was originally designed for the chest (pleural effusions). Using it in the abdomen is an “off-label” use. However, it is widely accepted and supported by evidence. Insurance still covers it when medical necessity is clear.
The Main Answer: CPT Code for PleurX Abdominal Catheter Placement
Here is the code you came for.
The correct CPT code for placing a PleurX catheter in the abdomen is:
CPT 49407
Descriptor: “Catheter placement, peritoneal, with intraperitoneal injection of contrast for evaluation of catheter function and patency, radiological supervision and interpretation, including placement of a tunneled catheter (e.g., peritoneal dialysis catheter or drain).”
Let us break that down into plain English.
-
49407 covers a tunneled peritoneal catheter. That means the catheter goes through the belly wall and then runs under the skin (the tunnel).
-
It includes radiological guidance. The doctor uses X-ray or fluoroscopy to guide the needle and wire into the correct spot.
-
It also includes checking that the catheter works. The doctor injects contrast dye to make sure fluid can flow in and out.
This is the code for a new placement. Not a removal. Not a revision. A brand new insertion.
Is There Another Code? What About 49406?
Sometimes people ask about CPT 49406. That code is for a non-tunneled peritoneal catheter. A temporary drain. Think of a simple drain that goes straight in and comes straight out. No tunnel. No subcutaneous tract.
A PleurX catheter is always tunneled. So 49406 is incorrect for PleurX placement.
What About Unlisted Codes?
Some coders panic and use CPT 48999 (Unlisted procedure, peritoneum). Do not do that unless you have no other choice. Why? Because unlisted codes invite denials. You have to send a letter with every claim. It slows down payment by weeks or months.
Use 49407. It is the right tool for the job.
When to Use CPT 49407: Clinical Scenarios
Let us make this real. Here are three common situations where you would bill 49407.
Scenario 1: Cancer Patient with Recurrent Ascites
A 62-year-old woman with ovarian cancer. She has been to the hospital four times in two months for large-volume paracentesis (needle drainage). Each time, 5 to 6 liters of fluid come out. She is tired of the trips. Her oncologist suggests a PleurX drain.
Procedure: Interventional radiology places a tunneled PleurX catheter into the peritoneal cavity under fluoroscopy.
Code: 49407
Scenario 2: Cirrhosis Patient with Refractory Ascites
A 55-year-old man with end-stage liver disease. He takes high doses of diuretics. They do not work anymore. His belly is tense and painful. He cannot eat well. His hepatologist refers him for a tunneled peritoneal drain.
Procedure: Same as above. Image-guided placement of a PleurX catheter.
Code: 49407
Scenario 3: Post-Surgical Chylous Ascites
A 45-year-old woman after a complex abdominal surgery. She develops a chyle leak (milky fluid) in her belly. Draining it once is not enough. The fluid keeps coming back. Her surgical team decides on a long-term tunneled drain.
Procedure: Image-guided PleurX placement.
Code: 49407
Notice a pattern? All three use the same code. The diagnosis changes. The code does not.
Breaking Down the Components of 49407
This code is a “global” code. That means it includes several steps. You do not bill for each step separately.
| Component | Included in 49407? | Can You Bill Extra? |
|---|---|---|
| Fluoroscopic guidance | Yes | No |
| Contrast injection to check flow | Yes | No |
| Catheter insertion (needle, wire, dilator) | Yes | No |
| Creation of subcutaneous tunnel | Yes | No |
| Suture to secure the catheter | Yes | No |
| Dressing application | Yes | No |
| Radiological supervision and interpretation (professional component) | Yes (for the radiologist reading the images) | No |
What is not included? The PleurX catheter itself. That is a supply. You bill supplies separately under HCPCS codes (see below).
HCPCS Supply Code for the PleurX Catheter
The catheter is not free. You need a separate code for the drain.
The correct HCPCS Level II code for a PleurX abdominal catheter is:
C1729
Descriptor: “Catheter, drainage, with or without injection port.”
Alternatively, some payers accept:
-
A4315 (Peritoneal dialysis catheter, permanent, with subcutaneous port/tunnel)
But C1729 is more specific to the PleurX system. Check your local payer policies.
Important: Some payers bundle the catheter into the procedure payment for hospital outpatient departments. Others pay separately. Do not assume. Verify with each carrier.
What About the Drainage Kit and Accessories?
Patients need supplies to drain at home. These are not part of the initial placement code.
The typical home drainage kit includes:
-
Vacuum bottle (500 mL or 1500 mL)
-
Drainage tubing
-
Dressing change supplies
-
Alcohol wipes
-
Gauze
These are billed separately under HCPCS codes like:
-
A7000 (Drainage bottle, each)
-
A7015 (Catheter securement device)
However, many patients get these through a home health or durable medical equipment (DME) supplier. The hospital placing the drain usually does not bill for ongoing supplies.
Modifiers for CPT 49407
Modifiers change the meaning of a code slightly. Here are the ones you need for 49407.
Modifier -50 (Bilateral Procedure)
Can you place two PleurX catheters in one abdomen? Almost never. One drain is usually enough. If a doctor tries two, you would need documentation of why. In practice, you will likely never use -50 with this code.
Modifier -52 (Reduced Services)
Sometimes the procedure does not go as planned. The doctor places the catheter but cannot inject contrast because of adhesions. Or the tunnel is shorter than usual. Modifier -52 tells the payer: “We did less than the full code describes.”
Use this honestly. Do not use it just to save money. Only when documentation supports it.
Modifier -53 (Discontinued Procedure)
The doctor starts the placement. They get the needle into the peritoneum. But then the patient has a vasovagal reaction. The doctor stops. No catheter is placed. Modifier -53 says: “We started but did not finish.”
Modifier -76 (Repeat Procedure by Same Physician)
The first catheter fails. It kinks or gets infected. The doctor removes it and places a new one on a different day. You bill 49407 again with -76.
Modifier -77 (Repeat Procedure by Different Physician)
Same as above, but a different doctor does the second placement.
Modifier -79 (Unrelated Procedure by Same Physician)
The patient had a different surgery yesterday. Today, the same doctor places a PleurX drain for a completely new problem. Modifier -79 tells the payer: “This is not a post-op complication of the first surgery.”
When NOT to Use CPT 49407
Honesty matters. Here are procedures that look similar but use different codes.
| Procedure | Correct CPT Code | Why Not 49407? |
|---|---|---|
| Temporary paracentesis (needle drainage, no catheter left behind) | 49080 or 49081 | No tunneled catheter. Just a needle. |
| PleurX placement in the chest (pleural cavity) | 32554, 32555, 32556, 32557 (depending on imaging and complexity) | Different anatomic site. Different code family. |
| Peritoneal dialysis catheter placement (Tenckhoff) | 49407 (yes, same code) | Same code. The descriptor includes “dialysis catheter.” |
| Removal of a tunneled peritoneal catheter | 49418 (if open) or 49419 (if laparoscopic) | Removal is a different code. |
| Replacement of a tunneled peritoneal catheter | 49423 (exchange over a wire) | Replacement without new tunnel. |
Documentation Requirements for 49407
Payers deny claims when documentation is weak. Here is what your provider must include in the procedure note.
Required Elements:
-
Medical necessity statement. Why does this patient need a tunneled drain? Mention failed paracentesis, diuretic resistance, or poor quality of life.
-
Consent form. Signed and dated. Specifically mentioning a tunneled peritoneal catheter.
-
Procedure details. Step by step:
-
Patient positioning
-
Sterile prep
-
Local anesthetic (lidocaine)
-
Needle entry site
-
Guidewire insertion
-
Fluoroscopy confirmation
-
Dilator and peel-away sheath
-
Catheter insertion
-
Tunnel creation
-
Contrast injection (must document this)
-
Catheter securement and dressing
-
-
Fluoroscopy time. Total time in minutes.
-
Contrast type and volume. Example: “10 mL of Omnipaque 300.”
-
Catheter size and type. “15 French PleurX tunneled drain.”
-
Immediate post-procedure assessment. Catheter flushes easily. Fluid returns.
-
Complications. None, or describe them honestly.
-
Signature and credentials. The physician who performed the work signs.
Professional vs. Technical Components
CPT 49407 includes both the doctor’s work (professional component) and the hospital’s equipment and staff (technical component). But sometimes you split them.
When to Split:
-
Modifier -26 (Professional component): The radiologist reads the images and performs the procedure. But the hospital owns the equipment. Bill 49407-26 for the doctor’s service.
-
Modifier -TC (Technical component): The hospital bills for the room, staff, fluoroscopy machine, and supplies. Not for the doctor’s interpretation.
-
Global (no modifier): One entity does everything. Common in private practice interventional radiology groups.
Note for hospital coders: Most hospitals bill the technical component (TC) to Medicare. The radiologist bills the professional component (-26) separately. Check your chargemaster.
Reimbursement Rates for 49407 (2026 Estimates)
I cannot give you exact fees. They vary by region, payer, and contract. But I can give you reasonable benchmarks.
| Payer Type | Professional Component (-26) | Technical Component (TC) | Global (No Modifier) |
|---|---|---|---|
| Medicare (National average) | $180 – $220 | $900 – $1,100 | $1,080 – $1,320 |
| Commercial insurance | $250 – $400 | $1,200 – $2,000 | $1,500 – $2,500 |
| Medicaid | $120 – $160 | $600 – $800 | $720 – $960 |
These are facility rates. If the procedure happens in a doctor’s office (rare for PleurX), the global payment is lower because there is no separate facility fee.
Common Billing Mistakes and How to Avoid Them
Let me save you from denials. Here are the top five errors coders make with 49407.
Mistake 1: Using Chest Tube Codes
Wrong: 32556 (Thoracic tunneled catheter placement)
Why it is wrong: The chest is not the abdomen. Two different body regions. Two different code families.
Fix: Always confirm the anatomic site in the procedure note.
Mistake 2: Forgetting the Contrast Injection
Wrong: Billing 49407 without documenting contrast.
Why it is wrong: The code descriptor explicitly says “with intraperitoneal injection of contrast.” No contrast? No code.
Fix: Ensure the radiologist writes: “Contrast injected under fluoroscopy. Free flow confirmed.”
Mistake 3: Billing Paracentesis Codes for Catheter Placement
Wrong: 49080 (Paracentesis without imaging)
Why it is wrong: Paracentesis drains fluid once and leaves nothing behind. A PleurX drain stays in for weeks or months.
Fix: Read the op note. If it says “tunneled” or “indwelling,” use 49407.
Mistake 4: No Medical Necessity in Documentation
Wrong: “Patient has ascites. Placed PleurX.”
Why it is wrong: That does not justify a tunneled drain. Many ascites patients do fine with occasional paracentesis.
Fix: Add: “Patient has undergone six large-volume paracenteses in three months. Symptoms return within five days each time. Diuretics failed. Quality of life severely impaired.”
Mistake 5: Billing Removal as 49407
Wrong: Using the same code for removal one month later.
Why it is wrong: Removal is a different service. Different work. Different code.
Fix: Use 49418 (Removal of peritoneal catheter, open) or 49419 (laparoscopic removal). Or for simple traction removal without incision, some payers accept an unlisted code.
Removal and Replacement of PleurX Abdominal Catheters
Patients do not keep these drains forever. When the ascites improves or the patient no longer needs drainage, the catheter comes out.
CPT Code for Removal (Open Method)
49418 – “Removal of peritoneal catheter, open”
This means a small incision. The doctor cuts the skin, breaks up scar tissue around the cuff, and pulls the catheter out.
CPT Code for Removal (Laparoscopic Method)
49419 – “Removal of peritoneal catheter, laparoscopic”
Less common for simple removal. Used if the catheter is stuck or there is suspected infection inside.
Simple Traction Removal (No Incision)
Some doctors just pull the catheter out at the bedside. No scalpel. No suture.
There is no specific CPT code for this. Most coders use:
-
CPT 49418 with modifier -52 (reduced services) – but this is a gray area.
-
Unlisted code 48999 – safer but requires documentation.
Check your local MAC policy. Some payers accept traction removal as included in the global period of the original placement (if within 90 days).
Replacement Codes
The old catheter fails. The patient still needs a drain.
Two options:
-
Exchange over a wire (49423): The doctor places a wire through the old catheter, removes the old one, and slides a new one over the wire. Less trauma. Same tract.
-
New placement (49407 again): The old tract is unusable. The doctor makes a new tunnel in a different spot.
Global Period for 49407
Medicare assigns a 10-day global period to 49407. What does that mean?
For 10 days after the procedure, the following are not billed separately:
-
Post-op visits related to the procedure
-
Catheter flushes or checks (unless a major complication)
-
Simple troubleshooting
After 10 days, you can bill for:
-
Office visits for catheter problems (use appropriate E/M code with modifier -25 if done same day as a procedure)
-
Catheter removal (if done after day 10)
-
Replacement (if needed after day 10)
Private Payer Policies: What You Need to Know
Medicare is straightforward. Commercial payers are not.
UnitedHealthcare
Requires prior authorization for 49407 for non-dialysis indications (like malignant ascites). They often ask for:
-
Number of paracenteses in prior 90 days
-
Trial of diuretics (with documentation of failure)
-
Life expectancy > 30 days
Aetna
Considers PleurX for malignant ascites medically necessary if:
-
Patient has symptomatic ascites
-
Large-volume paracentesis needed more than once every 14 days
-
Patient cannot tolerate repeated paracenteses
Cigna
Often denies 49407 for cirrhosis patients. They prefer transjugular intrahepatic portosystemic shunt (TIPS) or repeat paracentesis. You will need a strong appeal.
Blue Cross Blue Shield (varies by state)
Some BCBS plans cover PleurX for malignant ascites. Few cover it for refractory cirrhotic ascites. Check the local plan.
Pro tip: Before scheduling a PleurX abdominal placement, call the payer’s pre-authorization line. Ask: “Does your policy cover CPT 49407 for this diagnosis code?” Get the reference number.
Diagnosis Codes That Support 49407
Medical necessity starts with the right ICD-10-CM code.
| Diagnosis | ICD-10 Code | Notes |
|---|---|---|
| Malignant ascites | R18.8 | Use with a cancer code (C00-C96) as primary. |
| Cirrhosis with ascites | K74.69 | Unspecified cirrhosis. Add K70.31 for alcoholic cirrhosis with ascites. |
| Peritoneal carcinomatosis | C78.6 | Secondary cancer of peritoneum. |
| Chylous ascites | R18.8 | Add E79.89 if due to lymphatic abnormality. |
| Pancreatic ascites | K86.8 | Chronic pancreatitis complication. |
Never use a diagnosis alone. Always pair with a code explaining why the ascites exists.
Example of correct coding:
-
Primary: C56.9 (Malignant neoplasm of ovary)
-
Secondary: R18.8 (Ascites)
-
Procedure: 49407
How to Appeal a Denial for 49407
Denials happen. Do not panic. Here is a three-step appeal strategy.
Step 1: Review the Denial Reason
Common denial codes:
-
CO-50: Not medically necessary.
-
CO-97: Benefit for this service is not covered.
-
PR-204: This service or procedure requires prior authorization.
Step 2: Gather Supporting Documentation
Your appeal letter should include:
-
Operative note (clear, with contrast injection documented)
-
Pre-procedure notes (failed paracentesis, diuretic failure)
-
Imaging report (fluoroscopy confirms placement)
-
Peer-reviewed literature (attach one or two articles supporting PleurX for your patient’s condition)
Step 3: Write a Short, Factual Appeal
Example:
“Dear Medical Director,
Patient [Name] underwent CPT 49407 on [date] for placement of a tunneled peritoneal drain. This was medically necessary because the patient had malignant ascites due to ovarian cancer (C56.9) requiring paracentesis every 5 to 7 days for three months. Diuretics failed. Quality of life was poor.
Attached: op note, imaging, and two articles from the Journal of Vascular and Interventional Radiology supporting this intervention.
Please overturn the denial.”
Send it by fax or certified mail. Track it.
Frequently Asked Questions (FAQ)
1. Can a general surgeon bill 49407 for a PleurX placed in the abdomen?
Yes. Any physician with privileges to perform tunneled peritoneal catheter placement can bill 49407. This includes interventional radiologists, general surgeons, and some gastroenterologists.
2. Does 49407 include the ultrasound guidance for initial site marking?
No. Ultrasound to mark the skin before the procedure is not separately billable if you already bill fluoroscopy. Do not add CPT 76942.
3. How do I bill for a PleurX placement that fails (catheter not placed)?
Use CPT 49407 with modifier -53 (discontinued procedure). Document why you stopped.
4. What is the difference between 49407 and 49406?
49407 = tunneled catheter (PleurX).
49406 = non-tunneled catheter (temporary, straight drain).
5. Can I bill an E/M visit on the same day as 49407?
Yes, if the patient has a separately identifiable problem. Append modifier -25 to the E/M code. Example: 99223-25 (hospital admission for pneumonia) and 49407 (for ascites unrelated to pneumonia).
6. Does Medicare cover 49407 for malignant ascites?
Yes, under certain conditions. Local Coverage Determinations (LCDs) vary. Most MACs cover it when paracentesis is needed more than twice per month.
7. How do I bill for a PleurX catheter that is placed at the bedside without fluoroscopy?
You cannot bill 49407. The code requires radiological supervision. Use an unlisted code (48999) and send documentation. Expect a denial.
8. What is the correct code for flushing a PleurX catheter in the office?
If no other procedure is done, use an E/M code (e.g., 99212 or 99213). If the catheter is blocked and the doctor uses a wire to clear it, that is more complex. Some use 49423 (exchange) even if no new catheter is placed. Check payer policy.
9. Is the PleurX drainage bottle billed separately from the placement?
Yes. The bottle is supply A7000. But most patients get bottles from a DME supplier, not the hospital.
10. Can a nurse place a PleurX catheter?
No. In all US states, only physicians (MD/DO), and sometimes advanced practice providers (NP/PA) with supervision, place tunneled catheters. Nurses cannot bill 49407.
CPT Code Comparison Table
Here is a quick reference for codes related to peritoneal access.
| CPT Code | Description | Use for PleurX? |
|---|---|---|
| 49407 | Tunneled peritoneal catheter placement with contrast | YES (correct code) |
| 49406 | Non-tunneled peritoneal catheter placement | NO (PleurX is tunneled) |
| 49418 | Open removal of peritoneal catheter | YES (for surgical removal) |
| 49419 | Laparoscopic removal of peritoneal catheter | YES (complex removal) |
| 49423 | Exchange of peritoneal catheter over wire | YES (replacement without new tunnel) |
| 49080 | Paracentesis, without imaging | NO (temporary drainage only) |
| 49081 | Paracentesis, with imaging | NO |
| 32556 | Tunneled thoracic catheter placement (chest) | NO (wrong anatomy) |
| 48999 | Unlisted procedure, peritoneum | Only as last resort |
Real-World Billing Examples
Let me show you three complete billing scenarios.
Example 1: Hospital Outpatient, Medicare
Patient: 70-year-old with pancreatic cancer and malignant ascites.
Procedure: IR places PleurX in abdomen under fluoroscopy.
Billing (hospital):
-
CPT 49407-TC (technical component)
-
HCPCS C1729 (catheter supply)
-
ICD-10: C25.9, R18.8
Billing (radiologist):
-
CPT 49407-26 (professional component)
Example 2: Private Practice IR Group, Commercial Payer
Patient: 55-year-old with cirrhosis, refractory ascites, prior auth approved.
Procedure: Same as above. Global billing (no split).
Billing:
-
CPT 49407 (global)
-
HCPCS C1729
-
ICD-10: K74.69, R18.8
-
Prior auth number in Box 23
Example 3: Removal Only, No Replacement
Patient: 3 months after placement. Ascites resolved. Wants catheter out.
Procedure: Physician pulls catheter at bedside with simple traction. No incision.
Billing (controversial):
-
Some use 49418-52 (reduced open removal)
-
Some use 48999 with documentation
-
Best practice: Check payer policy first
Additional Resources for Coders and Clinicians
You do not have to memorize all of this. Bookmark these resources.
-
American College of Radiology (ACR) Coding Source: Quarterly updates on interventional radiology codes.
Link:https://www.acr.org/Clinical-Resources/Coding-Source -
CMS Local Coverage Determinations (LCDs): Search for “Peritoneal Catheter” in your state.
Link:https://www.cms.gov/medicare-coverage-database -
Society of Interventional Radiology (SIR) Coding Manual: Excellent guidance for tunneled drains.
Link:https://www.sirweb.org/practice-resources/coding-and-reimbursement -
AAPC Discussion Forums: Search “49407 PleurX” for real-world coder conversations.
Link:https://www.aapc.com/discuss -
Becton Dickinson (PleurX manufacturer) Reimbursement Hotline: 1-800-426-2444. They have a dedicated team for coding questions.
Final Thoughts and Best Practices
Let me leave you with three golden rules for coding PleurX abdominal catheter placement.
Rule 1: Always confirm the tunnel.
If the op note does not say “tunneled” or “subcutaneous tract,” do not use 49407. Ask for an addendum.
Rule 2: Document the contrast injection every single time.
No contrast = no code. That is not my rule. That is the CPT rule.
Rule 3: Do not guess. Look it up.
Coding changes every year. The 2026 CPT manual is your friend. Keep it on your desk.
Conclusion (Three Lines)
CPT 49407 is the correct code for PleurX abdominal catheter placement when performed with fluoroscopy and contrast injection. The procedure is medically necessary for patients with malignant or refractory ascites who cannot manage with repeated paracentesis alone. Always document the tunnel, the contrast, and the medical necessity to avoid denials.
Thank you for reading. If you found this guide useful, share it with a colleague who still uses chest tube codes for belly drains. Let us code together, honestly and accurately.






