If you have ever sat at your billing computer wondering which dental code actually fits a diagnostic wax up, you are not alone.
The dental code for wax up lives in a strange gray area. It is not as straightforward as a filling or a crown. Many dental teams struggle to find the right code. Some guess. Others leave money on the table. And a few unknowingly commit billing errors simply because the rules are not clearly explained.
This guide changes that.
We will walk through everything you need to know about coding for a wax up. You will learn which codes work, which ones do not, and how to document your work like a pro. No fluff. No fake codes. Just honest, practical advice you can use today.
Let us start with the most important question.
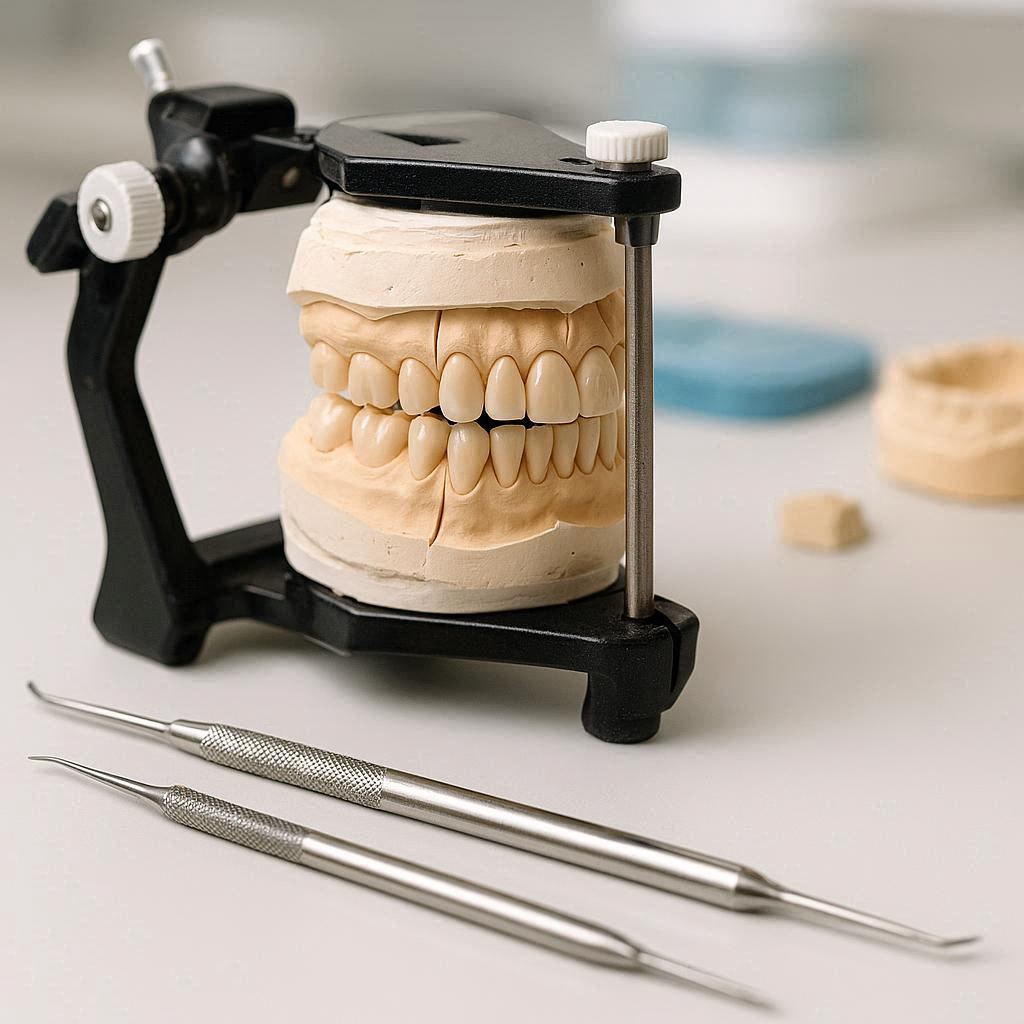
What Is a Diagnostic Wax Up in Dentistry?
Before we talk about codes, we need to be clear on what a wax up actually is.
A diagnostic wax up is a three-dimensional model of a patient’s teeth, made from wax. It is created on a stone model or a digital cast. The goal is to show the patient what their new smile could look like before any permanent work begins.
Think of it as a blueprint. A sculptor does not start carving marble without a clay model. A dentist should not start preparing teeth for multiple crowns or veneers without a wax up.
Wax ups are commonly used for:
- Smile design cases
- Multiple anterior restorations (crowns or veneers)
- Full mouth reconstructions
- Implant treatment planning
- Orthodontic finishing
- Sleep apnea appliances (in some cases)
The wax up helps the dentist, the patient, and the lab technician all see the same vision. It also creates a physical guide for the actual restorations.
But here is the catch.
Insurance companies do not always see a wax up the same way a dentist does. Some view it as part of the diagnostic process. Others see it as a laboratory procedure. And a few do not cover it at all.
That is why choosing the correct dental code for wax up is so important.
The Truth About the Official Dental Code for Wax Up
Let me be direct with you.
There is no single, standalone CDT code that says “wax up.”
The Current Dental Terminology (CDT) code set, published by the American Dental Association (ADA), does not have a code named “wax up.” This surprises many dental professionals when they first look for it.
So what do you do?
You have two honest paths:
- Use D8090 – Comprehensive oral evaluation (in some very specific scenarios)
- Use D0999 – Unspecified diagnostic procedure (with proper documentation)
Neither is perfect. But both can be appropriate when used correctly.
Let me explain each option in detail.
Option 1: D8090 – Comprehensive Oral Evaluation
Some practices bundle the wax up into a comprehensive exam.
Here is the logic. A wax up is part of the diagnostic process. It helps the dentist evaluate the patient’s oral condition and treatment needs. If the wax up is performed as part of a full workup for a major case, some dentists include it under the comprehensive exam code.
But there is a major problem with this approach.
Most payers will not reimburse extra for a wax up under D8090. They see the comprehensive exam as covering the dentist’s time and basic diagnostic tools. A laboratory-fabricated wax model is not considered a basic tool.
Therefore, using D8090 as your dental code for wax up is generally not recommended unless your contract specifically allows it.
Option 2: D0999 – Unspecified Diagnostic Procedure
This is the more honest and flexible code.
D0999 is defined as “unspecified diagnostic procedure, by report.” That last part — “by report” — is critical. It means you must attach a written explanation to your claim. You describe what you did, why you did it, and what materials or lab fees were involved.
Here is a sample narrative for a wax up claim using D0999:
“Diagnostic wax up performed on study models for case D9999. Wax up used for patient education, treatment planning, and fabrication of a silicone index for provisional restorations. Lab fee incurred. Total time: 45 minutes.”
The big advantage of D0999 is that it accurately describes what you did. The big disadvantage is that many medical and dental plans do not cover unspecified codes. They may deny the claim automatically.
But that does not mean you should not bill it. It means you should set proper patient expectations before you start.
Important Note: Some practices choose not to bill insurance for wax ups at all. Instead, they charge the patient directly as a separate diagnostic fee. This is often simpler and avoids claim denials.
A Closer Look at the Table of Common Codes Used for Wax Ups
Sometimes, dental teams mistakenly use other codes for wax ups. Let us look at what works and what does not.
| CDT Code | Official Description | Is It Correct for a Wax Up? | Why or Why Not? |
|---|---|---|---|
| D8090 | Comprehensive oral evaluation | Not recommended | The wax up is a lab procedure, not an exam service. |
| D0999 | Unspecified diagnostic procedure | Yes, with documentation | Requires a written report. Payer coverage varies widely. |
| D0470 | Diagnostic cast (study model) | No | This code is for pouring and trimming models, not waxing on them. |
| D2950 | Core buildup | No | This is a restorative procedure for a single tooth. |
| D9610 | Therapeutic drug injection | No | Not related at all. (Believe it or not, we have seen this error.) |
| D9999 | Unspecified adjunctive procedure | Possibly | Some offices use D9999 for lab work. Check with your payer. |
The safest and most accurate dental code for wax up remains D0999 with a report. But you should always verify with each insurance plan.
When Should You Use a Wax Up Code?
You should not code for every wax up the same way.
Here are three common scenarios. Each one may call for a different billing approach.
Scenario 1: In-House Wax Up for Patient Education
You take an alginate impression. You pour the model. You or your assistant creates a simple wax up to show the patient the shape of their future crowns.
In this case, you may not bill separately at all. Many dentists consider this part of the treatment planning process. It is wrapped into the overall case fee.
Scenario 2: Lab-Fabricated Wax Up with Significant Lab Fee
You send impressions to a dental laboratory. The lab technician creates a detailed diagnostic wax up and returns it to you. There is a hard lab bill.
Now you have an out-of-pocket expense. You can ethically bill D0999 to the patient’s insurance, attaching the lab invoice. You may also charge the patient directly if insurance denies.
Scenario 3: Wax Up Used for a Surgical Guide or Provisional Index
The wax up is not just for show. You use it to create a silicone matrix. That matrix helps you fabricate provisional restorations chairside.
This adds clinical value. Billing D0999 is reasonable here, especially if the wax up saved you significant chair time later.
Documentation Requirements That Protect Your Claim
If you are going to use D0999, your documentation must be excellent.
Insurance auditors love to deny unspecified codes. They assume you used the code because you did not know the correct one. Prove them wrong with clear, detailed notes.
Your wax up documentation should include:
- A clear reason why the wax up was needed
- Whether it was done in-house or by a lab
- The lab fee amount (if applicable)
- The total clinician time spent (if done in-house)
- How the wax up changed or guided treatment
- A photo of the wax up in the patient’s chart
- A copy of the lab invoice (if applicable)
One more thing. Keep the actual wax model or a high-quality photograph in the patient’s record. If an auditor asks for proof, you must be able to show them.
Pro Tip: Write your D0999 narrative before you submit the claim. Read it as if you were an insurance reviewer. Does it clearly explain why no other code worked? If not, rewrite it.
Why Insurance Often Denies the Dental Code for Wax Up
I want to be honest with you. Even with perfect coding, many insurers will deny a wax up claim.
Why?
Because many dental benefit plans consider wax ups to be part of the diagnostic process that is already covered under the exam. Others call it an educational tool, not a medical necessity. And a few plans specifically exclude “laboratory procedures performed for diagnosis only.”
Do not get frustrated. This is just how the system works.
Your job is not to guarantee payment. Your job is to code accurately and document thoroughly. Then, if the claim denies, you have two choices:
- Write off the cost as a patient education expense.
- Bill the patient directly after explaining the potential denial upfront.
Most successful practices choose the second option. They present a treatment plan that includes a separate line item for the wax up. They explain that insurance may not cover it. The patient decides.
This is ethical. This is transparent. And it protects your relationship with the patient.
A Realistic Billing Workflow for Wax Ups
Let me walk you through a practical step-by-step workflow.
Step 1: Determine Medical or Dental Necessity
Ask yourself: Is this wax up truly necessary for safe, predictable treatment?
For a single crown on a back tooth? Probably not.
For a six-unit anterior smile makeover? Absolutely yes.
Step 2: Estimate the Cost
If you are using an outside lab, get the lab fee first. Add your chair time. Now you have a true cost.
Step 3: Discuss with the Patient
Say this: “I recommend a diagnostic wax up. It is like a blueprint for your new smile. It costs $XXX. Some insurance plans do not cover this service. If your plan denies it, you will be responsible for the fee. Are you comfortable moving forward?”
Step 4: Perform the Wax Up
Do the work. Take photos. Keep records.
Step 5: Submit the Claim (Optional)
If the patient wants you to submit to insurance, use D0999 with a full narrative and lab invoice.
Step 6: Follow Up
If the claim pays, great. If not, bill the patient according to your signed financial agreement.
This workflow keeps you compliant and your patients happy.
Legal and Ethical Traps to Avoid
I have seen dental offices make some expensive mistakes with wax up coding.
Here are the traps to avoid.
Trap 1: Using a Restorative Code for a Wax Up
Never bill D2950 (core buildup) or D2750 (crown) for a wax up. That is fraud. The service you performed is not the service described by those codes.
Trap 2: Billing D0470 for a Wax Up
D0470 is for diagnostic casts — the stone models themselves. Adding wax to the model creates a different service. Do not use this code unless you truly only poured and trimmed models with no waxing.
Trap 3: Failing to Get a Waiver
If you know insurance will not cover the wax up, have the patient sign a waiver before you start. The waiver should say they understand the service may be denied and they accept financial responsibility.
Trap 4: Inflating Lab Fees
Never add a markup to a lab fee and then bill insurance for the marked-up amount. That is misrepresentation. Bill your actual cost or do not bill the lab portion at all.
Honest Advice: When in doubt, do not bill insurance for wax ups. Charge the patient directly as a diagnostic planning fee. This is simpler, cleaner, and far less likely to trigger an audit.
How to Talk to Patients About Wax Up Costs
Patients often do not understand what a wax up is. They hear “wax” and think of a candle.
You need simple language.
Try this explanation:
“Before I prepare your teeth for your new crowns, I want to build a wax model of exactly how they will look. Think of it like an architect’s drawing for a house. It helps you see the final result before we start. The fee for this model is $XXX. Insurance sometimes covers it, but not always. Would you like me to check your plan first?”
Most patients appreciate the honesty. Many will pay out of pocket just for the peace of mind.
State-by-State and Payer Variations
This is where things get messy.
Different insurance companies treat the dental code for wax up differently. Some examples:
- Delta Dental (various states): Often denies D0999 for wax ups, considering them not medically necessary.
- Cigna: May cover D0999 if a detailed narrative proves the wax up changed the treatment plan.
- Aetna: Typically excludes diagnostic wax ups under most PPO plans.
- Medicaid: Almost never covers wax ups for adults. For children, only in very rare orthodontic cases.
- Blue Cross Blue Shield (dental plans): Varies wildly by state. Always call and ask.
Never assume. Always verify with each individual plan before you promise coverage to a patient.
Alternative Approaches When Insurance Says No
If insurance will not pay, you still have good options.
Option A: Bundle the Wax Up into the Case Fee
Add the wax up cost to your comprehensive treatment fee. Do not itemize it on the insurance claim. Simply absorb the cost into your overhead and price your case accordingly.
Option B: Charge the Patient a Separate Planning Fee
Create an office policy. All smile design cases include a $250–$500 diagnostic planning fee. This covers the wax up, photos, and treatment planning time. The patient pays this fee directly. No insurance involved.
Option C: Use Digital Wax Ups (No Lab Fee)
Many intraoral scanners and design software programs allow you to create a digital wax up. There is no physical wax. There is no lab fee. You show the patient a 3D rendering on a screen.
Digital wax ups are not billable to insurance in most cases. But they cost you almost nothing. You can provide them as a value-added service at no charge.
Resource Link: Learn more about digital smile design and virtual wax ups at the American Academy of Cosmetic Dentistry’s patient education page: aacd.com
Real-Life Examples from Dental Practices
Let me share three real-world scenarios (names changed for privacy).
Example 1: Dr. S. in Texas
Dr. S. performed a diagnostic wax up for a patient needing eight upper veneers. The lab fee was $180. Dr. S. billed D0999 with a narrative and a copy of the lab invoice. The patient had a Delta Dental PPO plan. Delta denied the claim, stating wax ups are “not a covered benefit.” Dr. S. then billed the patient $180. The patient paid without issue.
Example 2: Dr. L. in Oregon
Dr. L. stopped billing insurance for wax ups entirely. Instead, she added a $350 “Comprehensive Diagnostic Workup” fee to all major aesthetic cases. The fee covered a digital wax up, intraoral photos, and a 30-minute treatment planning session. Patients paid this fee before any tooth preparation. Dr. L. reported higher case acceptance because patients felt more involved.
Example 3: A Large DSO in Florida
A corporate dental group tried to train all its offices to use D0470 for wax ups. An auditor caught the error. The group had to refund over $40,000 to multiple insurance carriers. They also paid a fine.
The lesson is clear. Use the wrong code, and it can cost you dearly.
Frequently Asked Questions (FAQ)
1. Is there a specific CDT code just for a wax up?
No. The ADA does not have a code named “wax up.” The closest honest option is D0999 (unspecified diagnostic procedure) with a written report.
2. Can I bill a wax up under a crown code?
Absolutely not. That would be insurance fraud. Crown codes are for delivering a crown, not for planning one.
3. Will Medicare cover a dental wax up?
Almost never. Medicare does not cover routine dental services, including diagnostic wax ups. Only in very rare, medically necessary jaw reconstruction cases might it apply, but that is extremely uncommon.
4. How much should I charge a patient for a wax up?
Typical fees range from $150 to $500, depending on the complexity and whether you use a lab. Simple single-unit wax ups are less expensive. Full arch diagnostic wax ups cost more.
5. Do I need a wax up for every crown?
No. Most single crowns do not require a wax up. Wax ups are most valuable for multiple anterior restorations, full mouth reconstruction, and complex aesthetic cases.
6. What if my software has a “wax up” billing code?
Some practice management software includes custom codes. That does not mean they are official CDT codes. Always verify with the current CDT manual.
7. Can I bill the patient and insurance for the same wax up?
No. Never double bill. Either bill insurance or bill the patient. Not both.
8. How long does a typical wax up take?
In-house wax ups can take 30 to 90 minutes. Lab-fabricated wax ups take 3 to 10 business days depending on the lab’s workload.
Final Checklist Before You Submit a Wax Up Claim
Use this checklist to protect yourself.
- The wax up was medically or dentally necessary (document why).
- The patient signed a financial agreement explaining possible insurance denial.
- You are using D0999 (not D0470, not D2950, not a crown code).
- Your narrative is clear, detailed, and attached to the claim.
- You have a photo of the wax up in the patient’s chart.
- You have the lab invoice (if applicable) saved in the record.
- You verified coverage with the specific payer before the procedure.
If you can check every box, you are in good shape. If you cannot, reconsider submitting the claim.
A Note on Future Coding Changes
The CDT code set is updated every year. New codes are added. Old codes are revised.
Could there be a specific dental code for wax up in the future? Possibly. The ADA’s Code Maintenance Committee accepts suggestions from dental professionals. If enough dentists request a dedicated wax up code, it could happen.
Until then, we work with what we have.
Stay informed. Read the new CDT manual each year. And always code honestly.
Conclusion: Three Lines to Remember
The dental code for wax up is not a single, simple code. Use D0999 with a detailed report if you bill insurance. Better yet, consider charging patients directly for this valuable diagnostic service to avoid claim denials altogether. Always document thoroughly and set clear patient expectations upfront.
Additional Resource Link
For the most current CDT codes and official coding guidelines, visit the American Dental Association’s CDT page:
https://www.ada.org/en/publications/cdt
Disclaimer: This article is for informational and educational purposes only. Dental coding is complex and subject to change. Always verify codes with your local payer, insurance carrier, or current CDT manual before submitting claims.
Author: Technical Dental Writer
Date: APRIL 18, 2026






